Arginine in the Treatment of Patients with Sickle Cell Disease: A Systematic Review
Eleuterio RMN1*, Nogueira NAP1, Eleutério J2, Araújo TG1 and Lemes RPG1
1Technological Innovation in Medicine Department, Federal University of Ceara, Brazil
2Pathology Department, Federal University of Ceara, Brazil
Submission: October 04, 2016; Published: October 24, 2016
*Corresponding author: Renata Mirian Nunes Eleutério, Technological Innovation in Medicine Department, Federal University of Ceara, Fortaleza, CE, Padre Antônio Tomás Avenue, number 3885, apartment 202, CEP: 60192-120, Brazil, Tel:+55 (85) 99637 6879; Email: renatameleuterio@gmail.com
How to cite this article: Eleuterio R, Nogueira N, Eleutério J, Araújo T, Lemes R. Arginine in the Treatment of Patients with Sickle Cell Disease: A Systematic Review. Adv Biotech & Micro. 2016; 1(4): 555566. DOI: 10.19080/AIBM.2016.01.555566
Abstract
Introduction: Sickle cell anemia (SCA), a monogenic disease prevalent in Brazil, is characterized by a point mutation, generating abnormal hemoglobin, hemoglobin S (HbS). Hydroxyurea, the drug used to treat SCA, increases fetal hemoglobin and nitric oxide levels; however, it is both cytotoxic and genotoxic. Arginine has been studied as one option for managing the disease. Material and methods: A systematic review was performed on scientific literature located by searching databases using the keywords “arginine” and “sickle cell anemia.” Articles published within the last 10 years were included if written in Portuguese, English, or Spanish, and describing studies that used humans. The articles were evaluated and classifieds according to the recommendations of the Brazilian Medical Association. Results and discussion: The search resulted in 139 articles, of which 65 were published within the last ten years. Of these, seven met the remaining inclusion criteria. The results showed that arginine, with or without hydroxyurea, increased nitric oxide levels and improved patient clinical condition. Conclusion: It seems that arginine increased levels of nitric oxide, a potent vasodilator. These studies encourage new clinical trials to evaluate the use of arginine in SCA.
Keywords: Arginine; Sickle cell anemia; Nitric oxide; Clinical trial; Hydroxyurea
Abbreviations: SCA: Sickle Cell Anemia; HbS: Hemoglobin S; HU: Hydroxyurea; NO: Nitric Oxide; ROS: Reactive Oxygen Species
Introduction
Sickle cell anemia (SCA) is a genetic disease caused by a point mutation at position six of the beta chain, resulting in hemoglobin S (HbS). Erythrocytes whose predominant content is HbS take on a sickle shape when HbS polymerizes. As a result, microcirculation becomes difficult and may result in obstruction of capillary blood flow [1].
Sickle cell anemia is the most prevalent monogenic disease worldwide. In Brazil, it is found in about 0.1% to 0.3% of the black population, and it is estimated that there are over two million carriers of HbS [2].
Patients with sickle cell disease have a heterogeneous clinical picture. The magnitude of their anemia ranges from mild to severe and may include high rates of morbidity and mortality of painful vaso-occlusive crises [3].
The treatment of SCA using oral hydroxyurea (HU) has multiple direct effects on the pathophysiological mechanism.
Synthesis of fetal hemoglobin is increased, reducing infra-erythrocytes and HbS polymerization in deoxygenation conditions. At the same time, the number of neutrophils is decreased along with erythroid hydration and the expression of adhesion erythrocytes, and the synthesis of nitric oxide (NO) and its bioavailability is increased [4].
Unfortunately, HU is a chemotherapeutic agent that is both cytotoxic and genotoxic, so it is important to study other various SCA treatment options. In addition, some patients do not respond to treatment or suffer from male infertility and myelo suppression [5].
Arginine is an amino acid that is a substrate for the synthesis of NO, a potent vasodilator that is deficient in SCA. High consumption of the reactive oxygen species (ROS) and NO by free Hb in plasma leads to lower bioavailability of NO and a reduction of the availability of the substrate of the nitric oxide synthase [6].
In this context, the goal of this review was to assess the articles that discuss using L-arginine in the treatment of patients with SCA.
Material and Methods
A systematic review of articles found in the scientific literature was performed. PubMed, Lilacs, Embase, the Cochrane library, and Google Scholar were used to locate the articles. Search terms such as “arginine” and “sickle cell anemia” were used. The main descriptors in the search strategy were: (“arginine” [MeSH Terms] or “arginine” [All Fields]) and (“anemia, sickle cell” [MeSH Terms] or (“anemia” [All Fields] and “sickle”[All Fields] and “cell”[All Fields]) or “sickle cell anemia”[All Fields] or (“anemia”[All Fields] and “sickle”[All Fields] and “cell”[All Fields]) or “anemia sickle cell” [All Fields]).
After evaluation, those reports published from 2006-2016 in Portuguese, English, or Spanish describing experiments that were conducted only in humans were included. Narrative reviews were excluded. The articles were then evaluated for methodological quality. Only those approved were included in the review.
Results and Discussion
Of the 139 articles resulting from the search, 65 were published in the last ten years. Of these, seven articles met the remaining inclusion criteria (Table 1).
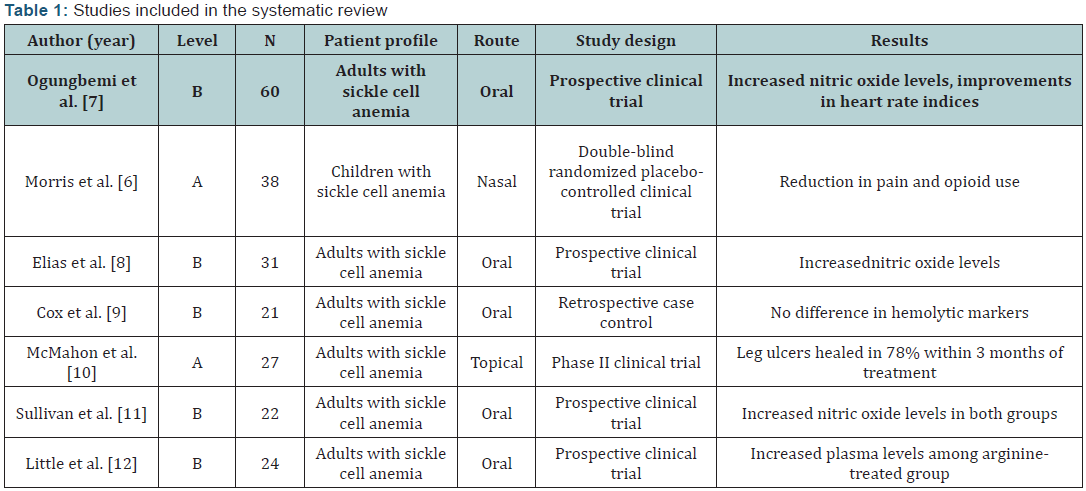
The use of supplementation with L-arginine in SCA was studied by Ogungbemi et al. [7] utilizing 28 patients who were compared to a control group of 32 people. The authors observed that oral supplementation with L-arginine increased the availability of NO and improved heart rates in patients with SCA.
Morris et al. [6] conducted a double-blind randomized placebo-controlled trial with inhaled L-arginine in 38 patients with vessel occlusion, finding a significant reduction in pain and in the use of opioids.
Elias et al. [8], in a clinical trial with 31 patients, evaluated hematological parameters and demonstrated that NO increased in patients with SCA. This demonstrates the action of oral arginine associated with HU in increasing the availability of NO with the intent of reducing pain and vessel oclusion.
In a Tanzanian case-control study between July 2007 and June 2009, patients with SCA were evaluated for plasma amino acids. No difference was found in hemolytic markers between a group of young African patients and older Americans, possibly reflecting differences in cause of death and disease severity [9].
A phase II clinical trial conducted by Mc Mahon et al. [10] treated patients with SCA and ulcers of the lower refractory members with a standard treatment for at least 6 months. They demonstrated that topical use of butyrate arginine cured 30% of the patients at 12 weeks and 78% after 3 months.
In turn, Sullivan et al. [11] aimed to determine the effect of oral arginine on NO levels in patients with sickle cell disease with and without acute chest syndrome, using a group of healthy people as a control. After arginine supplementation, the NO increased in all groups to a similar degree, and lung function and physiological parameters, such as blood pressure and heart frequency, were minimally affected.
Little et al. [12] studied patients with SCA who used oral L-arginine and sildenafil. L-arginine increased plasma ornithine and arginine, but not citrulline. Thus, the author discusses the possibility that arginase was offset by the plasma for NO production.
Conclusion
Using the studies meeting our inclusion criteria, it seems that NO, a potent vasodilator, increases and leg ulcers heal when arginine is used as part of the treatment. These studies encourage further clinical trials to examine whether, in fact, there are improvements in clinical and hematological parameters when arginine is supplemented in patients with SCA.
Acknowledgment: This work was supported by the National Council of Technological and Scientific Development (CNPq).
References
- Rees DC, Williams TN, Gladwin MT (2010) Sickle-cell disease. Lancet 376(9757): 2018-2031.
- Soares LF, Oliveira EH, Lima IB, Silva JM, Mota JT, et al. (2009) Hemoglobinas variantes em doadores de sangue do Centro de Hematologia e Hemoterapia do estado do Piauí (Hemopi): conhecendo o perfil epidemiológico para construir a rede de assistência. Rev Bras Hematol Hemoter 31(6): 471-472.
- Sonati MF, Costa FF (2008) Genética das doenças hematológicas: as hemoglobinopatias hereditárias. J de Pediatr 84(4): S40-S51.
- Figueiredo MS (2007) Agentes indutores da síntese de hemoglobina fetal. Rev Bras Hematol Hemoter 29(3): 313-315.
- Cançado RD, Lobo C, ÂnguloIL, Araújo PIC, JesusJA (2009) Protocolo clínico e diretrizes terapêuticas para uso de hidroxiureia na doença falciforme. Rev Bras Hematol Hemoter 31(5): 361-366.
- Morris CR, Kuypers FA, Lavrisha L ,Ansari M, Sweeters N, et al. (2013) A randomized, placebo-controlled trial os arginine therapy for the treatment of children with sickle cell disease hospitalized with vasooclusive pain episodes. Haematologica 98(9): 1375-1382.
- OgungbemiSI, Anigbogu CN, Kehinde MO, Jaja SI (2013) L-arginine increases nitric oxide and attenuates pressor and heart rate responses to change in posture in sickle cell anemia subjects. Niger J Physiol Sci 28(1): 45-50.
- Elias DBD, Barbosa MC, Rocha LBS, Dutra LLA, Silva HF, et al. (2013) L-arginine as an adjuvant drug in the treatment of sickle cell anaemia. Br J Haematol 160(3): 410-412.
- Cox SE, Makani J, Komba AN, Soka D, Newton CR, et al. (2011) Global arginine bioavailability in Tanzanian sickle cell anaemia patients at steady-state: a nested case control study of deaths versus survivors. Br J Haematol 155(4): 522-524.
- McmahonL, Tamary H, Askin M, Adams-Graves P, Eberhardt RT, et al. (2010) A randomized phase II trial of Arginine Butyrate with standard local therapy in refractory sickle cell leg ulcers. Br J Haematol 151(5): 516-524.
- SullivanKJ, Kissoon N, Sandler E, Gauger C, Froyen M, et al. (2010) Effect of oral arginine supplementation on exhaled nitric oxide concentration in sickle cell anemia and acute chest syndrome. J Pediatr Hematol Oncol 32(7): 249-258.
- Little JA, Hauser KP, Martyr SE, Harris A, Maric I, et al. (2009) Hematologic, biochemical and cardiopulmonary effects of L-arginine supplementation or phosphodiesterase 5 inhibition in patients with sickle cell disease who are on hydroxyurea therapy. Eur J Haematol 82(4): 315-321.






























