Periodontal Bone Regeneration of CSC Telescopic Abutments for The Treatment of Cases Affected Severe Advanced Periodontitis with Secondary Occlusal Traumatism - A Retrospective Long-Term Study
Guey-Lin Hou1*
Former professor, Graduate Institute of Dental Science and Department of Periodontics, Kaohsiung Medical Center, School of Dental Medicine, Kaohsiung Medical University, Kaohsiung City, Taiwan
Submission: August 05, 2023; Published: August 15, 2023
*Corresponding author: Guey-Lin Hou, Former professor, Graduate Institute of Dental Science and Department of Periodontics, Kaohsiung Medical Center, School of Dental Medicine, Kaohsiung Medical University, Kaohsiung City, Taiwan. E-mail: hougl2001@yahoo.com.tw
How to cite this article: Guey-Lin Hou. Periodontal Bone Regeneration of CSC Telescopic Abutments for The Treatment of Cases Affected Severe Advanced Periodontitis with Secondary Occlusal Traumatism - A Retrospective Long-Term Study. Adv Dent & Oral Health. 2023; 16(3): 555939. DOI: 10.19080/ADOH.2023.16.555939
Abstract
The purpose was to investigate evidenced-based clinical trials of abutments with severely advanced periodontitis (SAP) as the effect for the long-term options.
Materials and Methods: The present study was based on a retrospective analysis from 26 patients affected severe advanced periodontitis and secondary occlusal traumatism (SOT). Proper informed consent was obtained from the patients and control individuals. All patients were in good health with no contraindications to dental treatment. The study was to focus on the abutments of results of via periodontal therapy procedures including therapeutic provisional prosthesis (TPP), non-surgical periodontal therapy (NSPT), and crown and sleeve-coping telescopic denture (CSCTD). Records confirmed that the samples received TPP, NSPT, and CSCTD from 5.1years to 39 years in maxillary and mandibular abutments.
Results: Results showed that of the 139 abutments examined, 5 non-molar and 6 molar abutments were lost, giving a success rate of 92.1% in maxillary abutments. A total of 131 teeth were evaluated on both 3 non-molar and 5 molar abutments were lost giving successful rates of 93.2 % in mandibular abutments.
Conclusions: The conclusions showed that cases affected SAP with SOT got the success rates of both maxillary and mandibular teeth abutments were 92.1% and 93.2%, respectively, using combined techniques of TPP, NSPT and CSCTD.
Keywords: SAP, SOT, TPP, NSPT, CSCTD
Abbreviations: SAP: Severely advanced periodontitis; SOT: Secondary occlusal traumatism; TPP: Therapeutic provisional prosthesis; NSPT: Non-surgical periodontal therapy; CSCTD: Crown and sleeve-coping telescopic denture; CAL: Clinical attachment levels; RABL: Radiographic alveolar bone loss; FI: Furcation involvement; SPT: Surgical periodontal therapy; GTR: Guided tissue regeneration; RSR: Root separation and /or resection; DSRIA: Digital scanning radiographic image analysis
Introduction
The published reports addressed that non-surgical periodontal therapy (NSPT) may not only dramatically improve clinical and microbiological parameters, but also resolve inflammation and arrests adult periodontitis [1-4]. There still exist some problematic areas, such as, FED, furcal concavity, osseous defects, usually correlated with deep pockets that may adversely respond to NSP because of these sites limited access to debride bacterial deposits. In addition, clinical studies indicated that deep pockets in the molar furcation involvements have prone to more attachment loss and higher mortality rate when observed over many years [5-8]. The finding of minimal bone fills after scaling and root planning contrasted with the findings of bone fills, which were reported by Rosling et al. [9] and Polson & Heijl [10] that abundant bone repair, post-surgically. There exists conflicting data regarding the bone fills of angular bony defects following surgical and non-surgical periodontal therapy. Renvert et al. [11] indicated that limited repair in treating intra-osseous defects using flap operation and there was virtually no bone fill after root planning. It can be argued that the lose rate of periodontal attachment levels is influenced by some deteriorative factors such as type of plaque infection, host susceptibility, and the local environment of chronically inflamed tissue, pathologically deepened pockets resulted from foods impaction, ill-fitting restorations, crowding of teeth, morphology of alveolar bone, trauma from occlusion etc. In cases of individuals with SAP were most affected by SOT. Once not only characterized by severe periodontal attachment loss and reduced height of the alveolar bone but frequently also reveal a remarkably increased mobility of teeth.
SOT of the jigging type with concomitant increased hypermobility of teeth induced a series of periodontal tissue alterations associated with clinical and radiographic symptoms such as teeth hypermobility, pathological migration, angular bone defects, disappearance of lamina dura, widening of periodontal ligament. To present a gradual mechanical extraction of teeth with SAP, splinting using the periodontal prosthetic therapy for full mouth oral rehabilitation should be carried out as a prevention of treatment purposes of masticatory function, the patient’s comfort, elimination of SOT, and esthetic dentistry. The purpose of this report was, retrospectively and longitudinally, to investigate survival rates of abutments with severely advanced periodontitis [SAP, alveolar bone loss > 60 %] with SOT using NSPT, temporary provisional prosthesis (TPP) and CSCTD (Figure 1) as the effect for the evidenced-based clinical trials options.
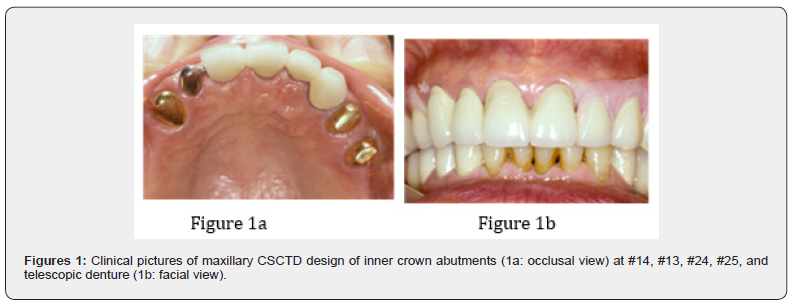
Materials and Methods
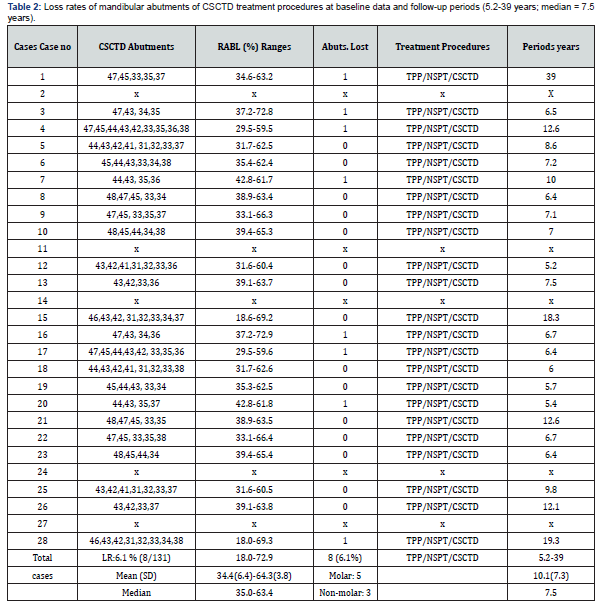
The present article is one of extension of our serial study on the field of periodontal prosthetic therapy for the treatment of individuals with severely advanced periodontitis (SAP, alveolar bone loss > 60 %). The present study was based on a retrospective analysis from 26 patients affected SAP and SOT. Proper informed consent was obtained from the patients and control individuals. The total abutments of 270 teeth were selected from graduate institute of dental sciences of medical university. Teeth consisted of both maxillary group [139 abutments] and mandibular group [131 abutments]. All patients were in good health with no contraindications to dental treatment. The individuals affected SAP and SOT treated using TPP, NSPT, and CSCTD (Figure 1) were signed as the treatment group. The present study was to focus on the survival rates of CSC telescopic abutments via routine periodontal therapy procedures including combination of TPP, NSPT, and CSCTD periodontal prosthetic procedures. The mean age of the samples was 54.4 ± 9.1. Record reviews confirmed that the total samples received TPP, NSPT, and CSCTD presented from 5.1years to 39 years with a mean 11.0±6.0 years [median 10.3 years] and 10.1±7.3 years [median 7.5 years] in maxillary and mandibular teeth, respectively (Tables 1 & 2).
Clinical examination
The clinical examination of periodontal parameters conducted on the molars included gingival index, [12] plaque index, [13] periodontal probing depth, horizontal and vertical clinical attachment levels (CAL: the distance in mm between the CEJ and apical end of the probing depth) and root mobility recorded for six sites on each tooth surface, at the baseline, 6 months, 1 year, and follow-up throughout the end of study. The percentages of RABL at the alveolar bone crest for each abutment was determined by measuring the medial and distal alveolar crest with most apical defect to the root apex from standardized parallel periapical and /or vertical bite-wing radiographs at baseline, margin of TPP, and inner crown margin [14]. The superimposed and unclear radiographs could not be used to determine the levels of radiographic alveolar bone loss [RABL] in the mesial and distal osseous defects. The removable TPP was fabricated not only for splinting the mobile teeth, but also for stabilizing the teeth with SOT. This removable TPP design is prepared as the precursor of permanent periodontal prosthesis of CSC retainer and CSCTD [15,16]. All treatment was performed by the same clinician. Supportive periodontal treatment recalled for reinforced oral hygiene instruction at two to three month’s appointments for personal plaque control by patient, as well as professional plaque control by clinician.
Results
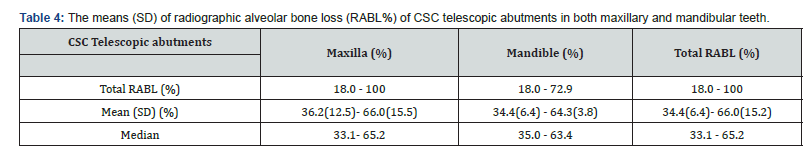
Results showed the list of CSCTD abutments location, ranges of RABLs, abutment loss, treatment procedures and successful rates, follow-up periods from 5.1 to 39 years in a both maxillary and mandibular teeth in a total of 28 cases. The means (SD) and ranges of initial radiographic alveolar bone loss (RABL) from 36.2±12.5 % to 66.0±15.5 % (ranged from 18.0% to 100 %) versus from 34.4±6.4 % to 64.3±3.8 % (from 18.0 % to 72.9 %) for maxilla and mandible, respectively. (Tables 1 & 2). Table 3 demonstrated the failure rates of teeth as the CSC telescopic abutments in both maxilla and mandibular arches using the combination of TPP, NSPT, and CSCTD techniques. Among 139 maxillary abutments, treated by the combined procedures of TPP, NPT, and CSCTD examined, 11 abutments were lost, giving a loss rate of 7.9 % and survival rate of 92.1% and after the end of study with a means elapsed time of 11.0±6.0 years. Of the 139 abutments examined, 5 non-molar abutments were lost, giving a loss rate of 3.6% in maxillary non-molar abutments, while 6 molar abutments were lost, giving a loss rate of 4.3%.
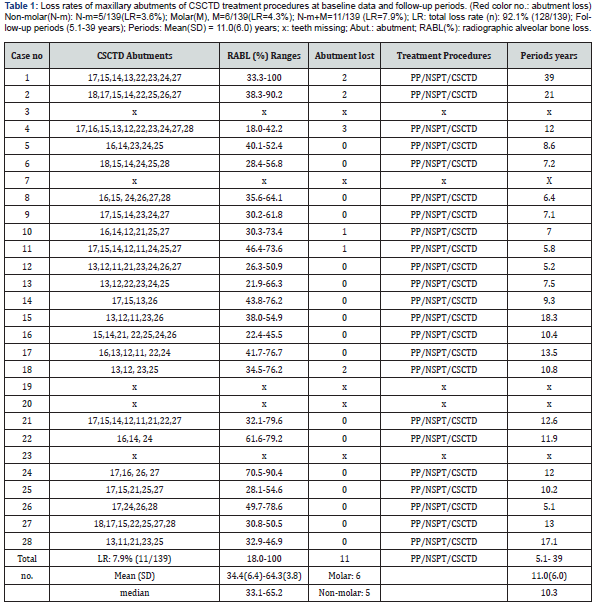
Non-molar(N-m): N-m=5/139(LR=3.6%); Molar(M), M=6/139(LR=4.3%); N-m+M=11/139 (LR=7.9%); LR: total loss rate (n): 92.1% (128/139); Follow-up periods (5.1-39 years); Periods: Mean(SD) = 11.0(6.0) years; x: teeth missing; Abut.: abutment; RABL(%): radiographic alveolar bone loss.
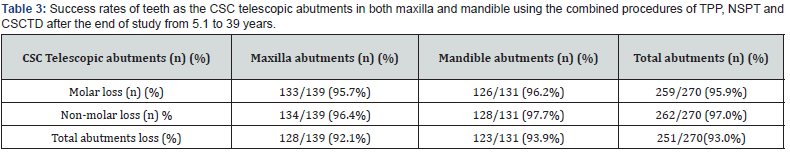
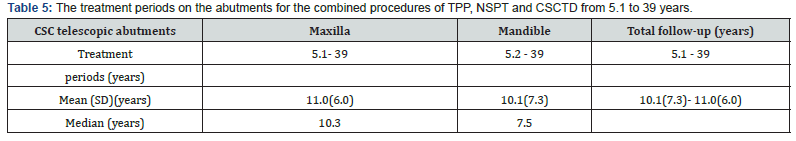
(Table 3) Out of 131 mandibular abutments, treated by the combined procedures of TPP, NSPT, and CSCTD evaluated, 8 abutments [3 non-molar and 5 molars] were lost, giving a 6.1% loss rates and survival rates of 93.9% after the end of study with a mean elapsed time of 10.1±7.3 [median=7.5] years. Both the 97 non-molar and 34 molar abutments a [total of 131 abutments] were evaluated, both molar (3/131) and non-molar (5/131) abutments were lost, giving a loss rate of 2.3 % and 3.8 % only, respectively (Table 3). (Table 4) indicated that the total RABL (%) mean (SD) ranges of RABL (%) and median on the CSC telescopic abutments in both maxillary and mandibular arches. The loss of RABL (%) in maxillary abutments was 18.0 % to 100%, where there in mandibular abutments was 18.0% to 72.9%, respectively. The total RABL (%) loss of both maxillary and mandibulr abutments was 18.0% to 100%. The means (SD) of RABL in maxillary and mandibular abutments were from 36.2±12.5% to 66.0±15.5% with a median 33.1% to 65.2%, and 34.4±6.4 to 64.3±3.8 with a median 35.0% to 63.4%, respectively. (Table 5) illustrated the treatment on the CSC telescopic abutments in both maxillary and mandibular arches using combined procedures of TPP, NSPT, and CSCTD in longitudinal clinical trials during 5.1 to 39 years. The treatment periods of maxillary and mandibular abutments were 5.1 to 39 years and 5.2 to 39 years. Result also showed that the means (SD) years of maxillary and mandibular abutments were 11.0±6.0 years with a median 10.3 years and 10.1±7.3 years with a median 7.5 years, respectively.
Representative Case
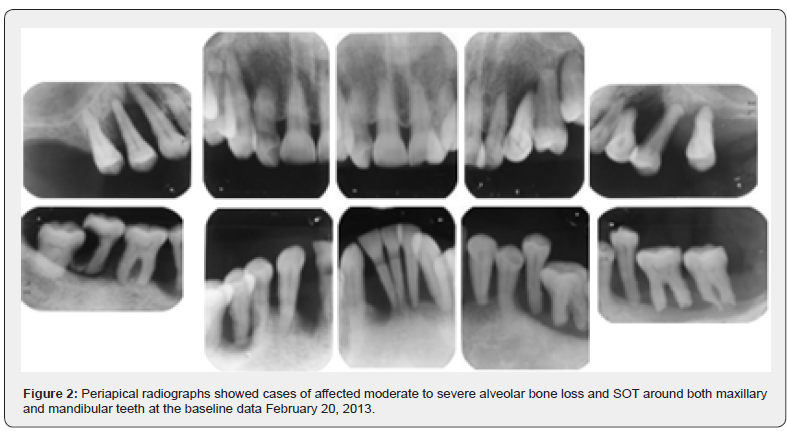
A 51-year-old female Taiwanese was referred from a local dental clinic for seeking the management of her severe advanced periodontitis in 2013. According to the chief complaints of patient included gingival bleeding, gingival recession, recurrent swelling with purulent exudation and generalized hypermobile teeth of full mouth. Severe advanced alveolar bone destruction, pathological teeth migration over bilateral maxillary premolars and molars and all around the anterior and posterior mandibular teeth, respectively. [Figure 2] Deep caries were noted at molar #47. Periodontal parameters of gingival index, (12) plaque index (13) revealed 2 to 3 scores. Grade III tooth mobility were noted at maxillary teeth #14, #13, # 23, #24, # 25, and mandibular teeth from #34 to #37, #33, #32 to #41 and #43, #45, #47, respectively. Initial probing pocket depths of maxillary and mandibular teeth were 7 mm or more, even reach to 10 mm, irrespective of both arches except maxillary teeth # 14, #12, # 11, #21, #22 and mandibular teeth #34, #43, and # 48. Molar furcation involvements were found at the teeth of #37, #36, #46, and #47. Periapical radiographs showed from moderate to severe alveolar bone loss around both maxillary and mandibular teeth. According to the related data associated with symptoms and signs of intraoral soft tissue and clinical evaluation of periodontal supporting hard tissues, a diagnosis of generalized aggressive periodontitis affected molar FI II to III with secondary occlusal traumatism (SOT) was established.
Treatment (Figure 2).
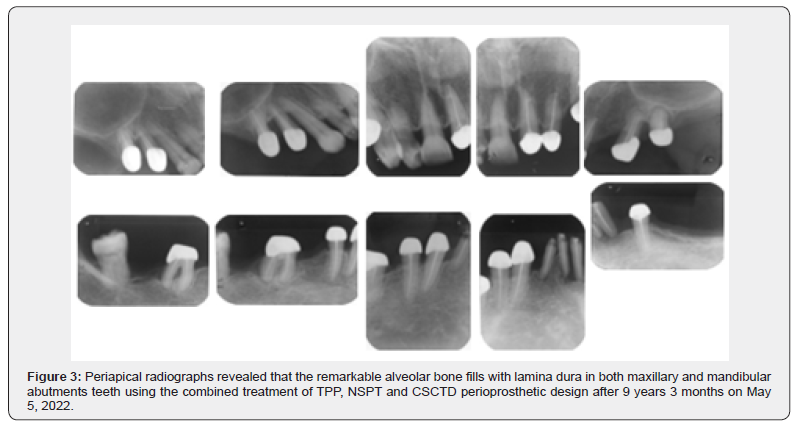
The treatment plan of periodontal and prosthetic procedures was consisted of oral hygiene instruction, TPP, NSPT. The patient was instructed in oral hygiene of personal and professional plaque control, routine meticulous scaling, root planning and subgingival curettage under the periodontist. Chlorhexidine gluconate solution (0.12%) was used for routine pocket irrigation following professional subgingival scaling and curettage. Removed hopeless teeth of maxillary tooth #23 and mandibular #35, #36, #37, #45, and #47. To reduce torque force and fulcrum line and stabilize periodontal support due to massive loss of periodontal bone. In addition, to decrease the crown root ratio on the CSC telescopic abutments, endodontic treatment of root canal therapy included both maxillary teeth at the #15, #14, #21, #22, #24, #25 and mandibular teeth at #34, #31, #41, #42, #43, #44 and #46 was necessary. Periodic recall visits for monitoring and reinforcement of professional plaque control were established during the first year. The provisional oral rehabilization using TPP was constructed, then, NSPT follow-up with 2 to 4 weeks periods for 12 months. One year later, the results of clinical evaluation for the periodontal soft and hard tissues following TPP, NSPT, and periodontal prosthetic designs applications. To increase proprioception, improve retention, increase rigid vertical support and stability of the periodontal prosthesis, CSC telescopic denture was used as the more reliable and effective design. [17-19]. Regarding the periodontal bone healing on the CSC telescopic denture design at the baseline as compared to the treatment after 9 years and 3 months. Results showed the combined use of TPP, NSPT, and CSCTD effective not only provided periodontal soft tissue healing, but also promote peridontal bone gains. Periapical radiographs revealed that the remarkable alveolar bone fills with lamina dura in both maxillary and mandibular abutments teeth using CSCTD perioprosthetic design after 9 years 3 months (Figure 2 & 3).
Discussion
Provisional crown has been recommended as a final approach of a therapeutic periodontal prosthesis (TPP) in the treatment of severely advanced periodontitis (SAP) with guarded prognosis. [15,20-22] The prosthetic design above techniques provided some advantages, including stabilizing hypermobile abutments, easy plaque control, decrease torque force, and reduce leveling force on the weak abutments affected SAP with SOT. The present study showed that clinical assessments of periodontal parameters using TPP, NSPT, and CSCTD (Figure 1a, 1b) restoration design revealed a remarkable soft and hard periodontal healing in both anterior and posterior abutments. Additionally, periapical radiographs revealed severe bone lose at the baseline; after follow-up periods over 9 years 3 months, results showed that complete repair of bony defects by bone fills, and reappearance of the lamina dura surrounding periodontal areas (Figure 2 & 3).
The majority of the discrepancy focused on the high prevalence of complications, such as root morphology, root fracture, recurrent invasion of furcation involvement (FI), incomplete plaque control over the residual root concavity, and treatment modalities. In addition, some studies. [4, 21-23] reported that factors such as anatomy and bony defects size between the bone and tooth, and amount and dimension of remaining periodontal tissues close to the defect are also important. However, these have more literature related to the treatment of the abutments affected SAP with SOT using surgical periodontal therapy (SPT) and combined SPT with guided tissue regeneration (GTR). Although, there still have many literatures associated with treatment of less periodontal bony support using the CSC retainers, but most of the public- shed data related to the successful treatment are limited on the case reports. [15,17] Recently, there are numerous reports associated with case series of SAP affected severe bony defects, SOT, molar FI using the combined periodontal and prosthetic treatments of TPP, NSPT and CSCTD (Figure 3) were presented. [18,19,24-26]. More recent literatures indicated a remarkable improvement in the periodontal parameters in advanced Class II and Class III molar FIs with root separation and /or resection (RSR) as compared to those without RSR [27]. Little or limited report associated with the longitudinal study on the survival rate of teeth as the abutments of CSCTD restoration in patient affected SAP with SOT. The former study seems also to be the first report using the digital scanning radiographic image analysis (DSRIA) to explore and, retrospective to evaluate the periodontal bone levels of a treatment option using a conservative periodontal therapy of TPP, NSPT combined with the CSCTD restoration [28]. Therefore, the long-term evaluation of perioprosthetic design of TPP, NSPT, and CSCTD may be provided an effective treatment philosophy for cases affected SAP with SOT.
References
- Bowers RC (1979) Furcation morphology relative to periodontal treatment: Furcation root surface anatomy. J Periodontol 50(70): 366-374.
- Yukna RA (1992) Clinical human comparison of expanded polytetrafluoroethylene barrier membrane and freeze-dried dura mater allografts for guide tissue regeneration of lost periodontal support. I. Mandibular molar Class II furcation. J Periodontol 63(5): 431- 442.
- Hou GL, Chen SF, Wu YM, Tsai CC (1994) The topography of the furcation entrance in Chinese molars. Furcation entrance dimensions. J Clin Periodontol 21(7): 451- 456.
- Muller HP, Eger T, Langer DE (1995) Management of furaction-involved teeth. A retrospective analysis. J Clin Periodontol 22(12): 911- 917.
- Hirshfeld L, Wasserman B (1978) A long-term survey of tooth loss in 600 treated periodontal patients. J Periodontol 49(5): 225- 237.
- Ramfjord SP (1980) Root planning and curettage. Intern Dent J 30(2): 93-100.
- Mcfall jr WT (1982) Tooth loss in 100 treatment patients with periodontal disease: a long-term study. J Periodontol 53(9): 535-549.
- Hou GL, Tsai CC (1987) Relationship between periodontal furcation involve- ment and molar cervical enamel projection. J Periodontol 58(10): 715-721.
- Rosling B, Nyman S, Lindhe J (1976) The effect of systematic plaque control control on bone regeneration in infra-bony periodontal defects. J Clin Periodontol 3(1): 38-53.
- Polson AM, Heijl LC (1978) Osseous repair in infra-bony periodontal defects. J Clin Periodontol 5(1): 13-23.
- Renvert S, Badersten A, Nilveus R, Egelberg J (1981) Healing after treatment of periodontal intraosseous defects. I. Comparative study of clinical methods. J Clin Periodontol 8(5): 387-399.
- Loe H, Silness J (1963) Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand 21: 533-551.
- Silness J, Loe H (1964) Periodontal disease in pregnancy. II. Correlation between oral hygiene hygiene and periodontal condition. Acta Odontol Scand 22: 121-135.
- Lin CH, Hou GL, Shieh TY, Tsai CC (1996) A cross-sectional radiographic study of proximal alveolar bone loss in molars with adult periodontitis. Kaoshiung J Med Sci 12(12): 716-727.
- Yalisove IL (1966) Crown and sleeve-coping telescopic retainers for removable partial denture. J Prosthet Dent 16(6): 1069-1085.
- Hou GL, Tsai CC, Weisgold AS (1999) Treatment of molar furcation involvement using root separation and a crown and sleeve-coping telescopic denture. A longitudinal study. J Periodontol 70(9): 1098-1109.
- Yalisove IL, Dietz JB (1977) Telescope Prosthetic Therapy, Biomechanics of the Crown and Sleeve-coping Prosthesis, 1st , Chapter 5, Philadelphia, Strickly pp. 65-82.
- Hou GL (2021) A long-term evaluation of bone levels using digital scan- ning radiographic image analysis on the CSC telescopic abutments in severe advanced periodontitis affected secondary occlusal traumatism. Advan in Dent & Oral Health 14(5): 555897.
- Hou GL (2022) Comparison of radiographic alveolar bone level using crown and sleeve-coping telescopic denture design on the abutments of non-molars for periodontal and prosthetic treatments - A long-term study. Advan in Dent & Oral Health 15(2): 555907.
- Hou GL, Chen SF, Wu YM, Tsai CC (1994) The topography of the furcation entrance in Chinese molars. Furcation entrance dimensions. J Clin Periodontol 21(7): 451-456.
- Hou GL, Tsai CC, Weisgold AS (1999) Treatment of molar furcation involvement using root separation and a crown and sleeve-coping telescopic denture. A longitudinal study. J Periodontol 70(9): 1098-1109.
- Hou GL, Tsai CC, Huang JS (1997) Relationship between molar root usion and localized periodontitis. J Periodontol 68(4): 313-319.
- Hou GL, Hou LT, Weisgold AS (2016) Survival rate of teeth with periodontally hopeless prognosis after therapies with intentional replantation and perioprosthetic procedures: a study of case series for 5 - 12 years. Clin and Experimental Dental Research 2(2): 85-95.
- Hou GL (2021) Differences of annual radiographic alveolar bone loss rates of anterior and posterior teeth of individuals affected with secondary occlusal traumatism between with and without perioprosthetic therapy. Advan Dent & Oral Health 14(4): 555892.
- Hou GL, Hong YI (2022b) Evaluation of treatment for advanced periodontitis affected with molar furcation involvements and secondary occlusal traumatism. Modern Research in Dentistry 7(2): 725-729.
- Hou GL, Hou LT (2019) Therapeutic outcomes using the Sandwich’s technique in treating severe advanced periodontitis with secondary occlusal traumatism: A long-term study for 5.1-39 years. Intern J Dent and Oral Health 5(7): 76-85.
- Hou GL (2020) A non-surgical root separation and/or resection for the treatment of advanced furcation involved molars - A longitudinal study for 5 - 18 years. Journa of Dentistry & Oral Disorders 6(7): 1- 5.
- Hou GL (2020) Survival rates of CSC telescopic abutments of severe advanced periodontitis with secondary occlusal traumatism using periodontal and prosthetic therapies. A long-term study of case series for 5.1-19.3 years. Advances in Dentistry & Oral Health 13(1): 555854.






























