Reference Range of Hemoglobin A1c In Sudan
Ibrahim A Ai*1, Hisham M Abdel Rahim1, Elmoataz H Taha2, Abdarahiem Alborai3, Abdelmohisen Hussein4, Kamal M Awad4, Naji Y Hajo5 and Omer A Musa1
1 Department of Physiology, The National Ribat University, Sudan
2 Department of Physiology, Dongola University , Sudan
3Department of Physiology, Omdurman Islamic University, Sudan
4 Department of Physiology, Gadarif University, Sudan
5Department of Physiology, National University, Sudan
Submission: August 28, 2018; Published: September 18, 2018
*Corresponding author: Dr. Ibrahim Abdelrhim Ali, Depertment of Physiology, Faculty of Medicine, The National Ribat University, Sudan.
How to cite this article: Ibrahim A A, Hisham M A R, Elmoataz H T, Abdarahiem A, Abdelmohisen H, et al. Reference Range of Hemoglobin A1c In Sudan. Curre Res Diabetes & Obes J. 2018; 8(4): 555745. DOI: 10.19080/CRDOJ.2018.08.555745.
Abstract
Background: Reference interval is crucial for disease screening, diagnosis, monitoring, progression and treatment efficacy. Due to lack of locally derived reference values for the parameters; clinicians use reference intervals derived from western population. But, studies conducted in different reference values have indicated differences between locally and western derived reference values. Hb A1c is now used largely for DM control, the normal values of Hb A1c in Sudanese must be established for the clinical diagnosis and follow up of DM
Objectives:The objective of this study is to establish the normal values of Hemoglobin A1c in Sudanese healthy adults and compare the result with the international values.
Methods:Cross sectional study was conducted during 2016-2018 in Sudan covering Khartoum state, Northern state, Gezira state, Red Nile state and North Darfur state, on adults of ages between 20-60 years and not known to be diabetic or suffering from any chronic illness. 1096 participants were assessed by a questionnaire covering age, family history of Diabetes Mellitus, physical activity, daily caloric intake and smoking history and BMI was calculated by measuring weight and height by weight & height measuring devices (scale). A sample of 5 ml venous blood was taken for FBG to exclude DM and measurement of Hb A1c using modified ELISA reader known as Cobas Integra 800 (Roch) machine. Correlations between the variables were estimated and P value < 0.05 was considered statistically significant.
Results:The overall mean value of Hb A1c was 4.6%±0.9 with a minmmus value of 1.2% and maximmus of 6.3. At 95% Confidence Interval the lower bound mean was 4.5% and the upper bound mean was 4.7%. In Sudanese states which cover under this study the highest mean of HbA1c was observed in Red Nile state (5.0%) and lowest mean was found in the Northern state (4.0%).
Conclusion:This study showed significant variations in the level of Hb A1c of healthy Sudanese in comparison with the reference ranges of international parameters. The study results revealed an urgent need to build national reference ranges for all haematological and other physiological parameters for Sudanese population in the near future.
Keywords: Hb A1c ; Normal values; Reference Range; Sudan
Introduction
In the mid-20th century, Grasbeck and Fellman published a paper entitled ‘Normal Values and Statistics’ as an initial study in the field of reference intervals (RIs). This was followed by a presentation by Grasbeck and Sais on ‘Establishment and Use of Normal Values’; intended to replace the more ambiguous concept of normal values and to ‘‘establish a well-defined nomenclature and recommended procedures in the field’’. [1,2]. In this first publication, there was a clear distinction between healthy reference values measured in healthy populations or individuals and patient reference values measured in patients having various diseases. It is now commonly accepted that reference values describe fluctuations observed in healthy populations or individuals, which makes the definition of health or characterization of health status a critical step. In subsequent years it was realized that the terminology of ‘normal values’ was not adequate, so the term ‘reference values’ came into use.
From 1987 to 1991, the International Federation of Clinical Chemistry (IFCC) published a series of 6 papers, in which it was recommended that each laboratory follow defined procedures to produce its own reference values [3-8]. Although there were very important developments and implementations between the 1990s and 2008 [9-12]; the C28- A3 guideline, published in 2008 by Clinical and Laboratory Standards Institute (CLSI) and IFCC constituted the most significant step in the development of RIs and is still in current use [13].
Different studies have shown variation in the normal ranges of Hb A1c. In Brazil Buffarini et al. performed a two cohort studies in 1982 and 1993 which were published later in 2016. It aimed at describing the distribution of Hb A1c levels according to earlylife and contemporary factors in adolescents and adults without diabetes mellitus and found the distribution of the Hb A1c was approximately 5.10% (±0.43), and 4.89% (±0.50) respectively [14].
In United Kingdom in 1989, Simon et al. reported the distribution of Hb A1c in 3240 healthy adult population. They found that the approximately normal distribution of Hb A1c was 5.03% (±0.53) [15]. In England at 2001 Gulliford and Ukoumunne performed a Cross-sectional survey and found a mean Hb A1c of 6.34% (±0.85) in a general population of 9,772 non-diabetic, white European subjects aged 16 years and older [16].
In 2010 Ghazanfari et al. in Iran performed a study to measure the association between Hb A1c and Fasting Blood Sugar (FBS) through a cross-sectional population-based study and found the mean of Hb A1c in non-diabetics was 5.61 % (±0.73) and in diabetics was 7.88% (±1.92) [17]. In 2011 Nathan et al. in UK reported the normal range of Hb A1c for non-diabetic people was found to be between 3.6-5.5 % [18]. According to a report published in 2009 by an International Expert Committee on the role of Hb A1c in the diagnosis of diabetes, Hb A1c can be used to diagnose diabetes and that the diagnosis can be made if the Hb A1c level is 6.5% or more and Hb A1c level below 6% is considered normal [19], although in Iran Hb A1c in diabetics was found to be 7.88 % (±1.92) [17].
Hb A1c results in the UK have usually been aligned to the assay used in the Diabetes Control and Complications Trial (DCCT), expressed as a percentage (DCCT- Hb A1c) - non-diabetic ‘normal’ range being 4-6% [20]. Diagnostic criteria for diabetes that made by (WHO report 2011) determined that Hb A1c of 6.5% was considered as the cut-off point for diagnosing diabetes. A value <6.5% does not exclude diabetes diagnosed using glucose tests [21]. Faerch et al. and Gulliford et al. both found somewhat higher levels of Hb A1c in men compared to women [16,22], but other studies found no sex-related differences in Hb A1c [23,24].
According to report published by the international diabetes fedaration- The IDF - Middle East and North Africa (MENA), there was over 1.4 million cases of diabetes in Sudan in 2015 [25]. Although the Hb A1c reference intervals for the general population in western countries are well established, reference intervals for healthy Sudanese people are not clearly defined. Most of the studies about Hb A1c that conducted in Sudan was pilot studies that done in small samples or studies considering abnormal Hb A1c such as Hb A1c in Diabetes Mellitus, anaemia, pregnancy, or patient with abnormal Hb structure. These abnormal values of Hb A1c were compared to the international normal one.
It is well known that the normal values used in Sudanese laboratories are mainly derived from European studies. Differences in the normal values in Sudan have been documented in some hematological values [26,27], respiratory function tests parameters, [28] Renal functions test [29] and serum electrolytes [30].
In Khartoum state at 2016 Ali et al. performed a Crosssectional study on 20 non-diabetic adult males of ages between 35-45 years and found a mean Hb A1c of 3.8 %±1.17 with a range of (1.2%-5.4%) [31]. Another cross-sectional study also done in Khartoum state at 2016 by Fadul et al. on 20 non-diabetic adult females, their ages was between 35-45 years and found a mean Hb A1c of 3.43 % ±1.17 with a range of (1.4-5.3%) [32].
In Khartoum state at 2018 Ali et al. performed a large Crosssectional study on 444 healthy non-diabetic sudanese adults and found the mean of HbA1c was 4.2±1.8% and with a range of 1.2- 6.5% [33]. Despite this variation the normal level of Hb A1c was generally taken as less than 6% and these values were applied to diabetic patients in Sudan, could there be a difference in the normal level of Hb A1c in Sudanese population is clearly a valid a question.
Most of the studies about normal Hb A1c were obtained in Western countries. These countries have totally different environment, ethnic groups, nutritional habits and body mass index, compared to Sudan. Currently, there are no known big scale studies conducted to investigate the normal reference range of Hb A1c in Sudanese people, and the normal reference range of Hb A1c in Sudanese hospitals and clinics is obtained from non-Sudanese subjects depending on the international American and British Guidelines. In this study, the normal level in healthy Sudanese people will be investigated.
Methods
A Cross sectional study conducted during 2016-2018 on Healthy Sudanese subjects of both sexes with age group 20-60 years. 1096 Sudanese adult volunteers were included and the study covering Khartoum state, Northern state, Gezira state, Red Nile state and North Darfur state. All subjects had a normal fasting blood glucose (FBG). The exclusion criteria of this study include Pregnant ladies, abnormal FBG, Diabetes mellitus, Hypertension, Renal failure, Liver disease, Cancer, Chronic diseases (cardiac diseases, TB, asthma, thyroid disorders), Haematological disorders., Recent acute diseases (Malaria, typhoid fever …etc), Lactation., History of recent surgery (splenectomy), History of schistosomiasis and Subjects not consenting. Written consents were obtained from all participants after fully explaining to them the project. A questionnaire was filled by all volunteers to obtain the data about name, age, address, medical history, drug use, and lifestyle. Weight, height, and blood pressure were measured with standard techniques. Complete clinical examination was performed. After informed consent, five ml of venous blood was collected by a standard procedure from each participant under complete aseptic conditions in the morning and after an overnight fasting. 2.5ml was placed in fluoride oxalate containers, and then used for FBG measurement with autoanalyzer A 15. The other 2.5ml was placed in EDTA container and used for Hb A1c analysis. (Icteric, lipemic, haemolyzed or bacterially contaminated samples were not used). Hb A1c was measured using modified ELISA reader known as COPAS Integra 800 using commercial reagent kits from Roche Company. All techniques and equipment were standardized. All data collected in this study was analysed using the SPSS computer programs, (t-test for mean and p. value P≤0.05 for significance).
Ethical consideration
Ethical Approval of this study was obtained from the Federal Ministry of Health in Sudan (FMOH) and The National Ribat University (NRU). The objectives of the study were explained to all individuals participating in the study. An informed consent was obtained from each participant in the study.
Results
A total of 1163 volunteers were identified as eligible; satisfying the inclusion criteria and approved to be enrolled after filling the consent, filling the questionnaire and fit on the physical examination. 67 subjects (5.7%) were excluded due to abnormal Fasting blood sugar which was discovered by the FBG and they were not known to be diabetics. 808 (73.3%) of the study sample were females and 272 were males (24.8%) and 16 were missing (1.5%). The mean of age was found to be 25.18±9.58 years with a range of 20-77 years. 444 of the participants were living in Khartoum state, 174 in Red Nile state, 91 in Gezira state, 215 Northern state and 172 were from North Darfur state. The overall mean value of Hb A1c was 4.6%±0.9 with a range of 1.2 to 6.3 which is lower than all international values (Figure 1).
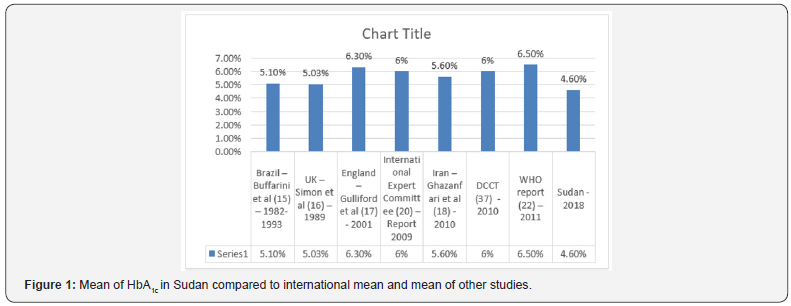
In Sudanese states which were covered under this study the highest mean of Hb A1c was observed in Red Nile state (5.0%) and lowest mean was found in the Northern state (4.0%) as mention (Figure 2).
Discussion
HbA1c measurement is one of the diagnostic tests used in the diagnosis of diabetes and monitoring hyperglycemia in uncontrolled diabetic patients. Hb A1c is a relevant predictor of diabetes related complications and of mortality [35]. As Hb A1c is now used largely for DM control, the normal values of Hb A1c in Sudanese have been addressed by this study.
Since Hb A1c reference intervals currently used in Sudan have been adopted from textbooks or guidelines referring mainly to European or American populations and according to some discrepancies in the normal reference intervals observed between Sudanese populations compared to European and American countries which has been documented in hematological values [27,28], respiratory function tests parameters [29], Renal function tests [30] and serum electrolytes [31]; this study was conducted to determine the Hb A1c reference intervals of healthy adults Sudanese.
In previous pilot studies conducted in Khartoum state by Ali et al. [32] and Fadul et al. [33] we have found that Hb A1c level was lower in Sudanese compared to the international values; but they were done in a small sample size. On the other hand, another large study conducted later by Ali et al [34] in Khartoum state with a bigger sample size has confirmed that Hb A1c in Sudanese is lower than the international. Normal mean distribution of Hb A1c in Sudanese adult males was 4.2% (±1.8%) with the range of 1.2-6.5% which is lower than the international range (3.6-6.5%).
The Purpose of this study was to establish normal reference range for Hb A1c in Sudanese non-diabetic adults. The population selected for this study was 1096 subjects. According to the international recommendations of the IFCC-LM and the CLSI, this size of sample can be considered to be representative of the adult population of the studied provinces (number of individuals ≥120 for each group) [36].
A1c samples were analyzed and the results outcome showed that the normal mean distribution of HbA1c in Sudanese adults was 4.6% (±1.0%) and the range was 1.2–6.3% which is lower than in international range (3.6–6.5%). Also, the American medical association added Hb A1c as a criterion in the diagnosis of diabetes mellitus and considered 6.5% as the cut off point for diagnosis [20,22,37].
Based in our findings, the mean and the maximum HbA1c for Sudanese population is 4.6% and 6.3% respectively, a figure with a significant gap from 6.5% and still lagging away from the international threshold for the diagnosis of any evolving diabetes. So, one can expect that relying on international reference values, will diagnose diabetes in this group only when Hb A1c increased significantly indicating poor control.
If the maximum is 6.3% for Hb A1c in Sudanese, then the cutoff point of 6.5% which was recommended by the WHO for DM diagnosis need to be revised in Sudan [20].
According to our study, Sudanese population has clearly lower normal values of Hb A1c when compared to international reference values. Subsequently, using these international thresholds in our local population might result in under diagnosing diabetes and slowing the recognition of cases of poor control subjecting them to complications of the disease before aggressive measurement can be instituted.
Noteworthy and to our knowledge, this is the first study with large sample size about the Hb A1c reference intervals in Sudan but still due to the variations between the states a national study with a bigger sample size and possibly a different sampling method should be performed. Why do we have a lower level of Hb A1c needs further analysis to correlate it with caloric intake and Hb level. In conclusion this study showed significant variations in the level of Hb A1c of healthy Sudanese in comparison with the reference ranges of international parameters.
The study results re¬vealed an urgent need to build national reference ranges for all hematological and other physiological parameters for Sudanese population in the near future. Further studies to confirm these results and establish reference range for Hb A1c in different age groups, Hb A1c in pregnancy, Hb A1c in different categories of BMI, Hb A1c in different Sudanese tribes and Hb A1c in athletes are highly recommended.
References
- Grasbeck R, Saris NE (1969) Establishment and use of normal values. Scand J Clin Lab Invest 110: 62-63.
- Sunderman FW (1975) Current concepts of ‘‘normal values,’’ ‘‘reference values,’’ and ‘‘discrimination values’’ in clinical chemistry. Clin Chem 21(13): 1873-1877.
- Solberg HE (1987) International Federation of Clinical Chemistry (IFCC), Scientific committee, Clinical Section, Expert Panel on Theory of Reference Values, and International Committee for Standardization in Haematology (ICSH), Standing Committee on Reference Values. Approved recommendation (1986) on the theory of reference values. Part 1. The concept of reference values. J Clin Chim Acta 25(5): 337-342.
- Petit Clerc C, Solberg HE (1987) International Federation of Clinical Chemistry (IFCC). Approved recommendation on the theory of reference values. Part 2. Selection of individual for the production of reference value. Clin Chim Acta 170: S1-S12.
- Solberg HE, Petit Clerc C (1988) International Federation of Clinical Chemistry (IFCC). Approved recommendation on the theory of reference values. Part 3. Preparation of individuals and collection of the specimens for the production of reference values. Clin Chim Acta 26(9): 593-598.
- Solberg HE, Stamm D (1991) International Federation of Clinical Chemistry (IFCC). Approved recommendation on the theory of reference values. Part 4. Control of analytical variation in the production, transfer and application of reference values. Clin Chim Acta 13(5): 231-234.
- Solberg HE (1987) International Federation of Clinical Chemistry (IFCC). Approved recommendation on the theory of reference values. Part 5. Statistical treatment of collected reference values. Clin Chim Acta 170: S13-S32.
- Dybkaer R, Solberg HE (1987) International Federation of Clinical Chemistry (IFCC). Approved recommendation on the theory of reference values. Part 6. Presentation of observed values related to reference values. Clin Chim Acta 20(11): 841-845.
- Harris EK, Boyd JC (1990) On dividing reference data into subgroups to produce separate reference ranges. Clin Chem 36(2): 265-270.
- Harris EK, Wong ET, Shaw ST (1991) Statistical criteria for separate reference intervals: race and gender groups in creatine kinase. Clin Chem 37: 1580-1582.
- Fuentes-Arderiu X (2006) Biological reference intervals and ISO 15189. Clin Chim Acta 364(1-2): 365-366.
- Henny J, Petitclerc C, Fuentes-Arderiu X, Petersen PH, Queralto JM, et al. (2000) Need for revisiting the concept of reference values. Clin Chem Lab Med 38(7): 589-595.
- CLSI, IFCC, C28-A3 document (2008) Defining, establishing and verifying reference intervals in the clinical laboratory: approved guideline- third edition 28: 1-76.
- Buffarini R, Restrepo-Méndez MC, Silveira VM, Miranda JJ, Gonçalves HD (2016) Distribution of Glycated Haemoglobin According to Early- Life and Contemporary Characteristics in Adolescents and Adults without Diabetes: The 1982 and 1993 Pelotas Birth Cohorts. PLOS ONE 11(9): e0162614
- Simon D, Senan C, Garnier P, Saint-Paul M, Papoz L (1989) Epidemiological features of glycated haemoglobin A1c-distribution in a healthy population. The Telecom Study. Diabetologia 32(12): 864-869.
- Gulliford MC, Ukoumunne OC (2001) Determinants of glycated haemoglobin in the general population: associations with diet, alcohol and cigarette smoking. Eur J Clin Nutr 55(7): 615-623.
- Ghazanfari Z, Haghdoost AA, Alizadeh SM, Atapour J, Zolala F (2010) A Comparison of Hb A1c and Fasting Blood Sugar Tests in General Population. Int J Prev Med 1(3): 187-194.
- Hill NR, Oliver NS, Choudhary P, Levy JC, Hindmarsh P (2011) Normal Reference Range for Mean Tissue Glucose and Glycemic Variability Derived from Continuous Glucose Monitoring for Subjects Without Diabetes in Different Ethnic Groups .Diabetes Technology & Therapeutics 13(9): 921-928.
- International Expert Committee (2009) International Expert Committee report on the role of the A1c assay in the diagnosis of diabetes. Diabetes Care 32(7): 1327-1334.
- Weykamp C, John WG, Mosca A (2009) A Review of the Challenge in Measuring Hemoglobin A1c. J Diabetes Sci Technol 3(3): 439-445.
- Use of Glycated Haemoglobin (Hb A1c) in the Diagnosis of Diabetes Mellitus: Abbreviated Report of a WHO Consultation. World Health Organization (2011), Geneva , Switzerland.
- Faerch K, Borch-Johnsen K, Vaag A, Jorgensen T, Witte DR (2010) Sex differences in glucose levels: a consequence of physiology or methodological convenience? The Inter99 study. Diabetologia 53(5): 858-865.
- Kilpatrick ES, Dominiczak MH, Small M (1996) The effects of ageing on glycation and the interpretation of glycaemic control in Type 2 diabetes. Q J Med 89: 307-312.
- Modan M, Meytes D, Rozeman P, Yosef SB, Sehayek E, et al. (1988) Significance of high Hb A1c levels in normal glucose tolerance. Diabetes Care 11(5): 422-428.
- International fedaration- The IDF - Middle East and North Africa (MENA).
- Hamad IM, Musa OA (2013) Reference Hb value in apparently healthy Sudanese children in Khartoum state. 37th Congress of IUPS Proc 37th IUPS, PCA297, Birmingham, UK.
- Taha EH, Elshiekh M, Alborai A, Hajo EY, Hussein A, et al. (2018) Normal range of white blood cells and differential count of Sudanese in Khartoum state. Int J Adv Med 5(4): 784-787.
- Bashir AA, Musa OA (2012) Reference spirometric values in Sudanese cohort. EMHJ 18(2): 147-154
- Abeadalla AA, Bashir AA, Abdalla IM, Abdelrhim IA, Awad KM, et al. (2018) Normal reference value of adult sudanese serum creatinine and urea in Khartoum state. Int J Health Sci Res 8(6): 19-24
- Ayat A Hassan, Hager M Osman, Ibrahim A Ali, Omer A Musa (2018) Reference Values for Serum Electrolytes (Na+, K+, Ca++) in Khartoum State. Saudi Journal of Medical and Pharmaceutical Sciences 4(7): 753- 757.
- Ali IA, Abdalarhim HM, Musa OA (2016) Reference values for hemoglobin A1c in males living in Khartoum state pilot study. Sudan Med Monit 11(3): 91-96.
- Fatima Ahmed Fadul, Hisham Mohammed Abdelrhim, Ibrahim Abdelrhim Ali, Omer Abdelaziz Musa (2017) Normal Values of Hemoglobin A1c among Women in Khartoum State: (A Pilot Study, 2016). International Journal of Science and Research 6 (9): 391-396
- Ibrahim A Ai, Hisham M Abdel Rahim, Babiker Almobasher, Rihab M Badi, Abdarahiem Alborai, et al. (2018) Reference Range of Hemoglobin A1c in Khartoum State. Anatomy Physiol Biochem Int J 4(4)
- Tennyson C, Lee R, Attia R (2013) Is there a role for Hb A1c in predicting mortality and morbidity outcomes after coronary artery bypass graft surgery? Interact Cardiovasc Thorac Surg 17(6): 1-9
- CLSI (2008) Defining, establishing, and verifying reference intervals in the clinical laboratory: approved guideline-Third Edition CLSI document C28-A3 (ISBN 1-56238-682-4). Clinical and Laboratory Standards Institute,19087-1898, Wayne Pennsylvania, USA.
- International Expert Committee (2009) International Expert Committee report on the role of the A1c assay in the diagnosis of diabetes. Diabetes Care 32(7): 1327-1334.
- Executive summary: Standards of medical care in diabetes-2010 (2010) Diabetes Care 33 (Suppl 1): S4-S10.






























