Palliative Radiation Treatment for Previously Untreated Head and Neck Cancer - Why, When and How: A Comprehensive Review
Toms Vengaloor Thomas1*, Satyaseelan Packianathan1, Hiba Zara Ahmed1, Ashley Albert1, Sanjay Joseph1, Teessa Perekattu Kuruvilla1, Anu Abraham2,, Amy Parr1, Eldrin Bhanat1, Madhava Kanakamedala1, Divyang Mehta1 and Srinivasan Vijayakumar1
1Department of Radiation Oncology, University of Mississippi Medical Center, USA
2Department of Pathology, University of Mississippi Medical Center, USA
Submission: December 18, 2019;Published: January 27, 2020
*Corresponding author: Toms Vengaloor Thomas, Department of Radiation Oncology, University of Mississippi Medical Center, USA
How to cite this article: Toms Vengaloor Thomas, Satyaseelan Packianathan, Hiba Zara Ahmed, Ashley Albert, Sanjay Joseph, et al. Palliative Radiation Treatment for Previously Untreated Head and Neck Cancer - Why, When and How: A Comprehensive Review. Palliat Med Care Int J. 2020; 3(2): 555607. DOI:10.19080/PMCIJ.2019.03.555607
Abstract
Currently, there are no evidence-based guidelines regarding palliative radiation for untreated head and neck squamous cell carcinoma (HNSCC) patients who are ineligible for curative treatment. This article reviews the available literature for palliative head and neck radiotherapy. The life expectancy and performance status of patients are used to optimize the treatment recommendations.
Introduction
Head and neck cancer include a diversity of tumor sites including, oral cavity, pharynx, larynx, paranasal sinuses, salivary gland, and thyroid. It includes a wide variety of histologies, the most common being squamous cell carcinomas of the mucosa or skin. The vast majority have locally advanced disease and approximately 3% of patients present with metastatic disease at presentation [1,2].
The current standard-of-care treatment for well-performing (ECOG 0-1) metastatic head and neck cancer patients (American Joint Commission on Cancer Care [AJCC] Stage IV C) is palliative multi-agent systemic therapy. More specifically, for well-performing patients with non-nasopharyngeal primaries, the Category 1 defined first-line systemic therapy combinations are Cisplatin/Carboplatin and 5 Fluorouracil with Pembrolizumab or with Cetuximab [3-8]. While, for patients with nasopharyngeal primaries, the Category 1 recommendation is a combination of Cisplatin and Gemcitabine [9-11]. However, for selected patients with excellent performance status and limited metastasis, surgery, or a combination of radiation and systemic therapy is recommended [11].
Importance of Palliative Radiation in Head and Neck Cancers
The curative treatment of head and neck cancers may not be possible in many circumstances - especially, in the presence of distant metastatic disease, poor performance status, significant comorbidities, or significantly extensive local disease [11]. These patients can often suffer from associated symptoms which include pain, trismus, dysphagia, odynophagia, stridor, hoarseness, otalgia, cough, and respiratory distress from advanced locoregional disease, which often impairs their quality of life (QOL). Many patients will benefit from palliative locoregional treatments, which typically involves radiation therapy. These treatments will improve the locoregional control of the disease, quality of life, and possibly improve survival [1]. However, there are only a few evidence-based guidelines specifying dose, fractionation, treatment techniques or volumes. This article reviews the available literature for palliative head and neck radiotherapy to make recommendations based on patient life expectancy and performance status.
Materials and Methods
Articles published between 1980 and 2018 were selected from an English Medline literature search using the following keywords: metastatic head and neck cancer, palliation, palliative radiation, Quality of Life (QOL).
Discussion
Even though several retrospective studies compared palliative radiation dose and fractionation schedules for patients with incurable head and neck cancer, there were only a few phase II studies that had explored the optimal treatment regimen. Most of these studies included patients with the newly diagnosed disease who were ineligible for curative treatment due to comorbid conditions, poor performance status, or metastatic disease at diagnosis, resulting in a heterogeneous study population. We discuss available phase II and retrospective studies in detail below.
Phase II trials
Paris et al. reported on a phase II trial using the Radiation Therapy Oncology Group (RTOG) 85-02 fractionation scheme [12]. This protocol used 3.7Gy per fraction, twice daily (6 hours apart) for two consecutive days to deliver a total dose of 14.8Gy per course. This course repeated every four weeks for a total of 3 courses and a total dose of 44.4Gy. The reported objective response was 77%, with minimal acute toxicity and without any long-term toxicity [12]. The so-called ‘QUAD SHOT’ protocol was another phase II trial from Australia which treated patients with incurable head and neck cancer with 14Gy in four fractions: 3.5Gy given twice a day, at least 6 hours apart, and for two consecutive days [13]. This regimen was also repeated at four-week intervals for a further two courses if there was no tumor progression. The treatment was well tolerated. Seventy-seven percent of patients had a significant reduction or stabilization of their disease following treatment, and 44% of the evaluated patients showed improved QOL. The “Hypo Trial” is yet another phase II clinical trial from Australia, which treated patients with advanced HNSCC using a hypofractionated course of radiotherapy consisting of 30Gy in 5 fractions (6Gy/fraction) delivered at 2 fractions/week, with an optional 6Gy boost for small volume disease (<3cm) [14]. Eighty percent of patients had an objective clinical tumor response, and 62% had an improvement in QOL. Another phase II study from Canada by Fortin et al. treated patients with 25Gy in 5 daily fractions using intensity-modulated radiation therapy (IMRT) technique [15]. This treatment regimen was also well tolerated.
Retrospective studies
Retrospective data from Princess Margaret Hospital has shown that the radiation dose used is an independent predictor of both overall survival and treatment response, suggesting that even in the setting of metastatic disease higher doses may benefit certain well-selected patients [16]. The most commonly used fractionation regimen was a split course designed to deliver a total dose of 50Gy in 20 fractions (2.5Gy/ fractions) over six weeks and was composed of two cycles of 25Gy in 10 fractions given daily over two weeks and separated by a 2-week break between cycles.
A large retrospective series from India that included 352 patients, used a palliative radiation regimen of 20Gy in 5 fractions; it showed significant palliation of symptoms in 60% of patients [17]. Another large institutional study from Tata Memorial Hospital in India evaluated a hypofractionated palliative radiation scheme: 40Gy in 16 daily fractions (2.5Gy daily) [18]. The patients with any response after 40Gy received an additional 10Gy in 4 fractions to a total dose of 50Gy; only 25% of patients were able to receive the additional 10Gy, but 87% of all patients (either 40 or 50Gy) had symptomatic improvement.
Chen et al. [19] retrospectively reviewed patients from the University of California, Davis, who had received palliative radiation treatment. They reported that the most commonly used fractionation regimen was that from the RTOG 85-02 protocol, as described above. They also delivered 70Gy in conventional 2Gy fractions, 30Gy in 3Gy fractions, 37.5Gy in 2.5Gy fractions, or 20Gy in 4Gy fractions and concluded that the RTOG 85-02 regimen provided effective palliation for patients. The Memorial Sloan Kettering Cancer Center (MSKCC) also documented a similar experience using the RTOG 85-02 regimen; 65% of their patients had a positive response in terms of palliation [20].
Erkal et al. [21] from the University of Florida retrospectively reviewed HNSCC patients who received palliative radiotherapy. Patients with relatively better KPS received 30Gy in 10 fractions (3Gy/daily) in once-daily fractions, and patients with poorer KPS received a split course of 20Gy: two 10Gy fractions one week apart. Eighty-eight percent of patients had either complete or partial response to the treatment, and 57% of patients had continued response at 1-year post-treatment. A retrospective series from the Netherlands reported on the use of the “Christie’s” regimen for palliative radiation therapy, in which patients were treated to 50Gy in 3.125Gy fractions daily over 16 days [22]. These patients had a 73% response rate with tolerable toxicity. Another study from the United Kingdom used a split course hypofractionated regimen with an initial 20Gy in 5 fractions over one week, followed by a 2-week gap, finally followed by an additional 20Gy in 5 fractions over one week [23]. They found that approximately 80% of patients had symptomatic improvement with tolerable toxicity.
In a case review, Ampil et al. reported improved survival for patients diagnosed with head and neck cancers with synchronous distant metastasis treated with a prolonged “definitive” course of radiation therapy, defined as a total dose >50Gy and daily dose fractions ranging from 1.8 to 3Gy, as opposed to a shorter “palliative” course of radiation [24]. More recently, Laursen et al. [25] from Denmark reported the use of an extended hypofractionated palliative regimen delivering 52-56Gy in 13-14 fractions at 4Gy per fraction twice weekly using IMRT techniques. Seventy-five percent of the patients completed the intended treatment, and 45% of patients had either complete or partial response of their locoregional disease. Acute toxicity was relatively higher, 25% and 15% of patients reported Grade III or IV mucositis and dermatitis, respectively. Patients with poor performance status, however, did not tolerate this regimen well, and the authors concluded that it was not suitable for these patients.
“SCAHRT” (Split-Course Accelerated Hypofractionated Radiotherapy) is another palliative radiation regimen, reported from Yale University [26]. This regimen consists of 3Gy daily for 10-12 fractions and repeated after 3-5 weeks to a total dose of 60- 72Gy. The authors reported that 89% of the patients completed both treatment courses, with a total tumor response of 91%. A retrospective study from the Netherlands compared 2- and 3-D techniques to IMRT for a palliative regimen of 48Gy in 12 fractions with 3-4 fractions per week and reported a statistically significant difference in the occurrence of mucositis favoring IMRT.43 They concluded that IMRT should be considered the modality of choice, even for purposes of palliation.
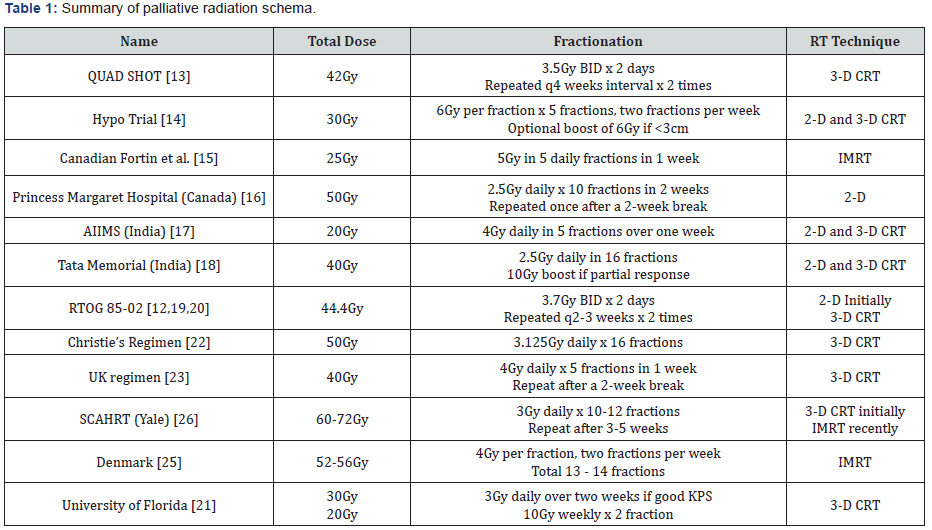
A randomized, open-label, parallel study performed in India compared three palliative radiation therapy regimens for head and neck cancer - (i) the QUAD SHOT, (ii) Christie’s regimen, and (iii)the conventional palliation fractionation scheme used in India (20Gy in 4-Gy daily fractions over 5 days, repeated once after 3 weeks) [27]. They performed a prospective analysis assessing QOL using the University of Washington QOL questionnaire, version 4. There was no significant difference in local control or overall response rate between the regimens. The grade III mucositis and treatment discontinuation rates were found to be higher in patients treated with Christie’s regimen. The quality of life was better, albeit only minimally, in patients who received the “QUAD SHOT” regimen compared to the two other regimens. In conclusion, the authors recommended the “QUAD SHOT” regimen for palliation of head and neck cancers given the comparable response rates, symptom relief, improved toxicities, and posttreatment QOL. These different palliative radiation regimens and studies are summarized in Table 1.
Conclusion
All incurable head and neck cancer patients should be evaluated in a multidisciplinary tumor board to choose the optimum treatment. The physicians should assess the patient’s performance status and goals of care very carefully. Palliative radiotherapy is a useful tool in improving the symptoms and should be offered as a treatment option. There are multipledose fractionation regimens currently being used for palliative radiation treatment, and the decision should be based on the patient’s performance status. For selected patients with limited metastatic disease and excellent performance status (ECOG 0-1), an aggressive treatment approach with a higher dose of radiation is a valid option. Patients with worse performance status (ECOG 2 or worse) will benefit from a hypofractionated palliative radiation treatment.
References
- Goldstein NE, Genden E, Morrison RS (2008) Palliative care for patients with head and neck cancer: I would like a quick return to a normal lifestyle. JAMA 299(15): 1818-1825.
- Kuperman DI, Auethavekiat V, Adkins DR, Nussenbaum B, Collins S, et al. (2011) Squamous cell cancer of the head and neck with distant metastasis at presentation. Head Neck 33(5): 714-718.
- Rischin D, Harrington KJ, Greil R, Soulieres D, Tahara M, et al. (2019) Protocol-specified final analysis of the phase 3 KEYNOTE-048 trial of pembrolizumab (pembro) as first-line therapy for recurrent/metastatic head and neck squamous cell carcinoma (R/M HNSCC). Journal of Clinical Oncology 37(15_suppl): 6000.
- Vermorken JB, Trigo J, Hitt R, Koralewski P, Diaz-Rubio E, et al. (2007) Open-label, uncontrolled, multicenter phase II study to evaluate the efficacy and toxicity of cetuximab as a single agent in patients with recurrent and/or metastatic squamous cell carcinoma of the head and neck who failed to respond to platinum-based therapy. J Clin Oncol 25(16): 2171-2177.
- Vermorken JB, Peyrade F, Krauss J, Mesía R, Remenar E, et al. (2014) Cisplatin, 5-fluorouracil, and cetuximab (PFE) with or without cilengitide in recurrent/metastatic squamous cell carcinoma of the head and neck: results of the randomized phase I/II ADVANTAGE trial (phase II part). Ann Oncol 25(3): 682-688.
- Vermorken JB, Specenier P (2010) Optimal treatment for recurrent/metastatic head and neck cancer. Ann Oncol 21(Suppl 7): vii252-261.
- Vermorken JB, Mesia R, Rivera F, Remenar E, Kawecki A, et al. (2008) Platinum-based chemotherapy plus cetuximab in head and neck cancer. N Engl J Med 359(11): 1116-1127.
- Mesía R, Rivera F, Kawecki A, Rottey S, Hitt R, et al. (2010) Quality of life of patients receiving platinum-based chemotherapy plus cetuximab first line for recurrent and/or metastatic squamous cell carcinoma of the head and neck. Ann Oncol 21(10): 1967-1973.
- Jin Y, Shi YX, Cai XY, Xia XY, Cai YC, et al. (2012) Comparison of five cisplatin-based regimens frequently used as the first-line protocols in metastatic nasopharyngeal carcinoma. J Cancer Res Clin Oncol 138(10): 1717-1725.
- Zhang L, Huang Y, Hong S, Yang Y, Yu G, et al. (2016) Gemcitabine plus cisplatin versus fluorouracil plus cisplatin in recurrent or metastatic nasopharyngeal carcinoma: a multicentre, randomised, open-label, phase 3 trial. Lancet 388(10054): 1883-1892.
- NCCN (2019) National comprehensive cancer network guidelines.
- Paris KJ, Spanos WJ, Lindberg RD, Jose B, Albrink F, et al. (1993) Phase I-II study of multiple daily fractions for palliation of advanced head and neck malignancies. Int J Radiat Oncol Biol Phys 25(4): 657-660.
- Corry J, Peters LJ, Costa ID, Milner AD, Fawns H, et al. (2005) The 'QUAD SHOT'--a phase II study of palliative radiotherapy for incurable head and neck cancer. Radiother Oncol 77(2): 137-142.
- Porceddu SV, Rosser B, Burmeister BH, Jones M, Hickey B, et al. (2007) Hypofractionated radiotherapy for the palliation of advanced head and neck cancer in patients unsuitable for curative treatment--"Hypo Trial". Radiother Oncol 85(3): 456-462.
- Fortin B, Khaouam N, Filion E, Nguyen-Tan PF, Bujold A, et al. (2016) Palliative Radiation Therapy for Advanced Head and Neck Carcinomas: A Phase 2 Study. Int J Radiat Oncol Biol Phys 95(2): 647-653.
- Stevens CM, Huang SH, Fung S, Bayley AJ, Cho JB, et al. (2011) Retrospective study of palliative radiotherapy in newly diagnosed head and neck carcinoma. Int J Radiat Oncol Biol Phys 81(4): 958-963.
- Mohanti BK, Umapathy H, Bahadur S, Thakar A, Pathy S, et al. (2004) Short course palliative radiotherapy of 20Gy in 5 fractions for advanced and incurable head and neck cancer: AIIMS study. Radiother Oncol 71(3): 275-280.
- Agarwal JP, Nemade B, Murthy V, Ghosh-Laskar S, Budrukkar A, et al. (2008) Hypofractionated, palliative radiotherapy for advanced head and neck cancer. Radiother Oncol 89(1): 51-56.
- Chen AM, Vaughan A, Narayan S, Vijayakumar S (2008) Palliative radiation therapy for head and neck cancer: toward an optimal fractionation scheme. Head Neck 30(12): 1586-1591.
- Lok BH, Jiang G, Gutiontov S, Lanning RM, Sridhara S, et al. (2015) Palliative head and neck radiotherapy with the RTOG 8502 regimen for incurable primary or metastatic cancers. Oral Oncol 51(10): 957-962.
- Erkal HS, Mendenhall WM, Amdur RJ, Villaret DB, Stringer SP, et al. (2001) Squamous cell carcinomas metastatic to cervical lymph nodes from an unknown head and neck mucosal site treated with radiation therapy with palliative intent. Radiother Oncol 59(3): 319-321.
- Al-mamgani A, Tans L, Rooij VPH, Noever I, Baatenburg DJRJ, et al. (2009) Hypofractionated radiotherapy denoted as the "Christie scheme": an effective means of palliating patients with head and neck cancers not suitable for curative treatment. Acta Oncol 48(4): 562-570.
- Kancherla KN, Oksuz DC, Prestwich RJ, Fosker C, Dyker KE, et al. (2011) The role of split-course hypofractionated palliative radiotherapy in head and neck cancer. Clin Oncol (R Coll Radiol) 23(2): 141-148.
- Ampil FL, Kim DD, Ghali GE, Baluna RG (2012) How intensive should radiotherapy for head and neck cancer with synchronous distant metastases be? Review of cases. J Oral Maxillofac Surg 70(3): 730-733.
- Laursen M, Specht L, Kristensen CA, Gothelf A, Bernsdorf M, et al. (2018) An extended hypofractionated palliative radiotherapy regimen for head and neck carcinomas. Front Oncol 8: 206.
- Bledsoe TJ, Noble AR, Reddy CA, Burkey BB, Greskovich JF et al. (2016) Split-Course accelerated hypofractionated radiotherapy (scahrt): a safe and effective option for head and neck cancer in the elderly or infirm. Anticancer Res 36(3): 933-939.
- Soni A, Kaushal V, Verma M, Dhull AK, Atri R, et al. (2017) Comparative evaluation of three palliative radiotherapy schedules in locally advanced head and neck cancer. World J Oncol 8(1): 7-14.






























