Pain Managment in Adult Palliative Patients
Jelena Hodak*
Department of Anesthesiology, Clinical hospital centre of Zagreb, Croatia
Submission: May 16, 2019; Published: May 22, 2019
*Corresponding author: Jelena Hodak, Department of Anesthesiology, Clinical hospital centre of Zagreb, Croatia
How to cite this article: Jelena Hodak. Pain Managment in Adult Palliative Patients. Palliat Med Care Int J. 2019; 2(4): 555591. 10.19080/PMCIJ.2019.02.555591
Abstract
There are many campaigns in the world aimed at fight against the pain and public awareness and healthcare professionals about the problem of adult pain in the palliative patient and the possibilities of its better quality with the least possible side effects. The World Day of against Pain marks October 17, and each year is dedicated to a certain type of pain, proclaimed by the International association for study of pain (IASP). The 2019 was declared the global year against of pain in vulnerable populations divided into major groups: older adults, children and infants, persons with intellectual disabilities, survivors of torture and persons requiring palliative care. As human life is prolonged, an increasing number of people will suffer from more comorbidities, weaknesses and chronic diseases and conditions such as kidney, heart or lung failure. It is estimated that by 2050, population older than 60 years will be doubled. In addition, older people can experience significant psychosocial stress due to dependence on someone else’s help. Palliative care aims to preserve or improve the quality of life and alleviate the suffering through early identification, detailed assessment and treatment of symptoms. In older people, it is necessary to combine geriatric medicine and palliative care with an emphasis on comprehensive assessment, integrating social, spiritual and environmental factors. In palliative care, we take into account the concept of ‘complete pain’ which explores psychological difficulties that may affect the perception of pain and suffering.
Keywords: Pain; Palliative; Vulnerabile population; Patient
Introduction
The International association for study of pain (IASP) defines pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage or description in terms of such damage.” There are many campaigns in the world aimed at fight against the pain and public awareness and health professionals about the problem of adult pain in the palliative patient and the possibilities of its better quality with the least possible side effects. The World Day of fight against Pain is marked on October 17, and each year is dedicated to a certain type of pain, proclaimed by IASP. The year 2019. was marked by the global year of fight against pain in vulnerable populations divided into major groups: older adults, children and infants, persons with intellectual disabilities, survivors of torture and persons requiring palliative care. As human life is prolonged, an increasing number of people will suffer from more comorbidities, weaknesses and chronic diseases and conditions such as kidney, heart or lung failure. It is estimated that by 2050, population older than 60 years will be doubled [1]. In addition, older people can experience significant psychosocial stress due to dependence on someone else’s help. The influence of pain in the functioning of the organism is the fact that it has been declared “the fifth vital sign”.
Discussion
Palliative care aims to preserve or improve the quality of life and alleviate the suffering through early identification, detailed assessment and treatment of symptoms [2]. In older people, it is necessary to combine geriatric medicine and palliative care with an emphasis on comprehensive assessment, integrating social, spiritual and environmental factors. It also requires understanding of multi-morbidity, safe regulation and multidisciplinary approach. Good communication needs to be given priority, taking into account autonomy, involvement in decision-making and the existence of ethical dilemmas. Likewise, working with older people and their families in their environment, whether it is a home for elderly people, long-term care, hospice, hospital, or other. When assessing the pain of older people experiencing pain reporting, mediates a number of social and psychological factors, including stoicism, which can lead to pain reduction [2]. The “Golden Standard” remains a self-report [3]. The questions of pain include three key dimensions: 1) sensory, 2) affective and 3) influence of dementia and cognitive dementia [4]. Reporting pain can be a challenge for older people with cognitive impairment resulting from dementia and other neurodegenerative diseases such as stroke, cultural or linguistic factors. Many people with dementia can reliably report pain, but it is important to get good medical records [5]. Direct observation or validated scores for pain assessment recognize how pain or discomfort can lead to behavioral change [6]. Due to inadequate pain management in adult palliative patients, negative clinical outcomes such as deep vein thrombosis, pulmonary embolism, coronary ischemia, acute myocardial infarction, pneumonia, poor wound healing, insomnia, reduced motivation and cognitive dysfunction (Table 1) [3].
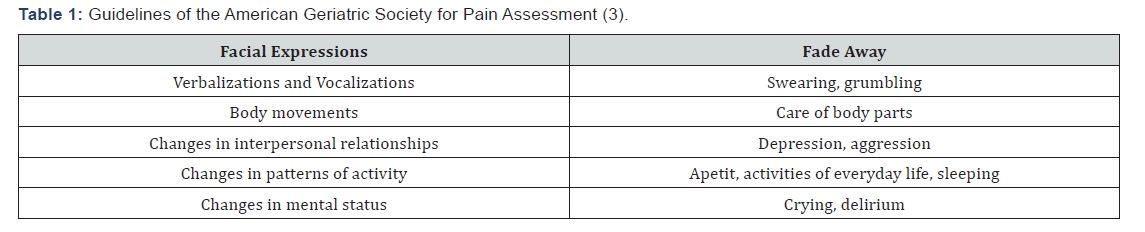
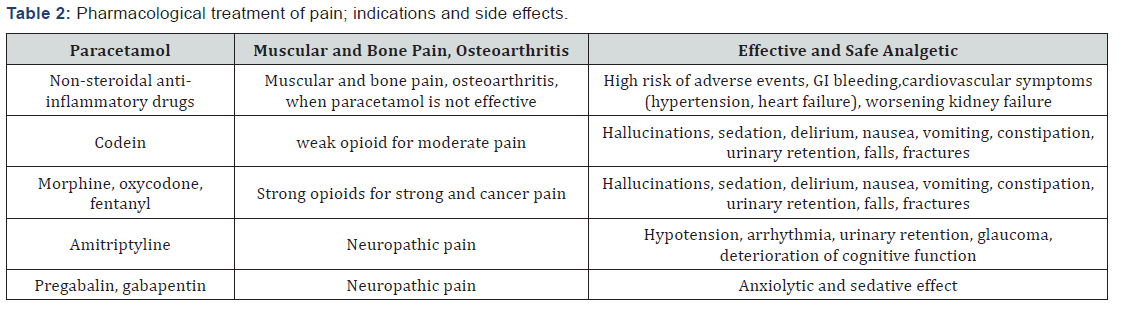
Most of the pain assessment tools contain these items. Common tools include pain scale [7], pain assessment in advanced dementia PAINAD [8]. A control list for the elderly with limited communication capability (PACSLAC) can also be used [9]. Non-pharmacological treatment such as exercise, aids or relaxation or current preparations, including NSAIDS for localized musculo-skeletal pain, may be effective as the first choice [2]. Pharmacological treatment of pain in older people can be challenging. Polymerization is common and changes in the way drugs are metabolized and excreted increase the risk of interactions and side effects (Figure 1) (Table 2).

Conclusion
Approach to an adult patient in palliative care as a vulnerabile individual ensures regular re-examination of symptoms and treatment goals. Discussing the “upper border of care” with the patient or his family for the development of a treatment plan allows for a good managment of pain. Considerations such as abolishing painful interventions are also considered [10]. It is possible to reduce the risks for people who are going through a difficult period at the end of life, especially at the hospital [9]. In palliative care, we take into account the concept of ‘complete pain’ which explores psychological difficulties that may affect the perception of pain and suffering [10]. Pain is a subjective feeling and every patient is experiencing differently. Adequate pain managment is the basic human right of patients and the responsibility of healthcare professionals. Also, by exchanging knowledge and experience, we can improve and relieve adult palliative patients of their pain all over the world
References
- World Health Organisation (2017) Global Health Observatory (GHO) data; mortality and global health estimates, USA.
- Abdulla A, Bone M, Adams N, Elliott AM, Jones D, et al. (2013) Evidence-based clinical practice guidelines on management of pain in older people. Age Ageing 42(2): 151-153.
- American Geriatrics Society (2002) The management of persistent pain in older persons. J Am Geriatr Soc 50(6 Suppl): S205- S224.
- Royal College of Physicians, British Geriatrics Society, British Pain Society (2007) The assessment of pain in older people: national guidelines. Concise guidance to good practice series 8: 1-13.
- Zwakhalen SM, Hamers JP, Berger MP (2006) The psychometric quality and clinical usefulness of three pain assessment tools for elderly people with dementia. Pain 126(1-3): 210-220.
- Scherder E, Herr K, Pickering G, Gibson S, Benedetti F, et al. (2009) Pain in dementia. Pain 145(3): 276-278.
- Abbey J, Piller N, De BA, Esterman A, Parker D, et al. (2004) The Abbey pain scale: a 1-minute numerical indicator for people with end-stage dementia. Int J Palliat Nurs 10(1): 6-13.
- Warden V, Hurley AC, Volicer L (2003) Development and psychometric evaluation of the Pain Assessment in Advanced Dementia (PAINAD) scale. J Am Med Dir Assoc 4(1): 9-15.
- Fuchs-Lacelle S, Hadjistavropoulos T (2004) Development and preliminary validation of the pain assessment checklist for seniors with limited ability to communicate (PACSLAC). Pain Manag Nurs 5(1): 37-49.
- Sampson LE, Pautex S (2019) Palliative Care for older person in pain. Internacional association for the study of pain.






























