An Attempt to Deliver Home-Based Palliative Care to Children with Cancer in Sub-Saharan African Villages-Our Cameroon Experience
Wharin PD1*, Hesseling PB2, Kouya F3, Kaah J4 and Afungchwi GM5
1Beryl Thyer Memorial Africa Trust, UK
2Department of Paediatrics and Child Health, Stellenbosch University, South Africa
3Oncology Medical Supervisor, Cameroon Baptist Convention Health Services, Cameroon
4Children’s palliative care nurse, Banso Baptist Hospital and Mbingo Baptist Hospital, Cameroon
5Programme Manager, Cameroon Baptist Convention children’s cancer treatment service, Cameroon
Submission: May 16, 2019; Published: May 21, 2019
*Corresponding author: Wharin PD, Beryl Thyer Memorial Africa Trust, UK
How to cite this article: Wharin PD, Hesseling PB, Kouya F, Kaah J, Afungchwi GM. An Attempt to Deliver Home-Based Palliative Care to Children with Cancer in Sub-Saharan African Villages-Our Cameroon Experience. Palliat Med Care Int J. 2019; 2(3): 555590. 10.19080/PMCIJ.2019.02.555590
Keywords: Palliative care; Own homes; Health services; Baptist hospitals; Children’s cancer; Mbingo; Mutengene; HIV/AIDS; paediatric illness; Burkitt lymphoma; Cyclophosphamide; Adapted protocols; Tumour; Adequate analgesia
Abbrevations: PC: Palliative Care; CBCHS: Cameroon Baptist Convention Health Services; BBH: Baptist Hospitals Banso; BL: Burkitt Lymphoma
Introduction
This article describes our experience in the development of an outreach palliative care (PC) service to children with cancer in a resource limited, sub-Saharan African setting: an attempt to reach children at considerable distance from the nearest hospital and provide palliative care in their own homes. Our service is an integral part of the Cameroon Baptist Convention Health Services (CBCHS) children’s cancer treatment programme. The CBCHS is a faith-based healthcare organisation which provides care in six of Cameroon’s 10 regions. Data presented in this article relates to our work in the North west and South west (anglophone) regions of Cameroon at three Baptist hospitals: Banso (BBH) and Mbingo (MBH) in the North west, and at Mutengene (BHM) in the South west. Treatment for the majority of children is free at point of need thanks to the Beryl Thyer Memorial Africa Trust (UK) which undertakes to support the cost of drugs and covers all CBCHS hospital bills, and the charity, World Child Cancer, which has engaged in capacity building and parent support since 2011
Historically within our own setting the delivery of palliative care has focussed on adults and HIV/AIDS. In the past children with the common cancer, Burkitt lymphoma, often disappeared into the bush after a single dose of cyclophosphamide: they were lost to follow-up and any palliative care. In comparison with a European setting there are cultural as well as socioeconomic differences in approach to paediatric illness, which combined with the lack of concept of “cancer” in rural Cameroon create unique challenges to the delivery of palliative care to children with cancer in their own homes. Palliative care is holistic by definition and begins when the illness is diagnosed. It does not equate with terminal care. Our aim is to improve quality of life for children with cancer and their families. Our objective is that all children dying at home receive supervised and adequate analgesia and that all parents/carers receive appropriate support and counsel.
Background
A Burkitt lymphoma (BL) treatment programme began at BBH in 2003 using a protocol designed for a resource limited setting by Professor P.B. Hesseling, emeritus Professor of Paediatrics and Child Health at Stellenbosch University and Tygerberg Hospital, Cape Town. This was a low cost, low toxicity, high frequency cyclophosphamide-based regimen. The programme later extended to MBH and BHM. Since that date we have treated approximately 1000 children with this cancer. A survey in 2013 in which we attempted to contact children treated since 2003 showed a long term survival of 55%. 738 families were reached with a median follow-up time of 3.7 years [1]. We make great effort to achieve one year follow-up (over 96%) and beyond. We know our outcomes and have been able to steadily improve our BL treatment protocol. Our current protocol gives a one year event-free survival of over 60% [2]. Treatment of Wilms tumour began in 2007, followed by Kaposi sarcoma in 2011 and retinoblastoma in 2013, using SIOP recommended protocols. Adapted protocols are used for other cancers (Table 1).
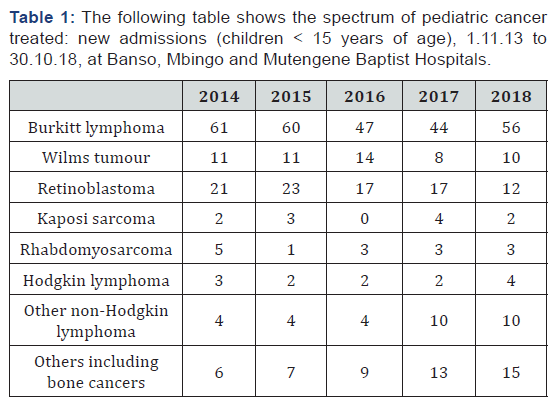
Approximately 50% of these children were beyond cure because of late presentation, or because their cancers were resistant to the best treatment protocols that we can offer in a resource limited setting. We have no access to radiotherapy at the present time.
Method
A 3 month survey at BBH in 2011 revealed that the great majority of our patients with Burkitt lymphoma lived beyond range (15Km radius of the hospital) of the 4-wheel drive vehicle used by the hospital palliative care team. A motorbike can travel further and faster into the bush, using tracks too narrow for a 4-wheel drive vehicle. We decided to purchase a tough off-road motorbike and to train a male nurse with pediatric nursing experience to ride over rough terrain. The latter objective proved more difficult to achieve. The riding is potentially dangerous and we decided that the dangers for our nurse would be reduced if he used motorbike taxis which are commonplace in Cameroon. He rides as the pillion passenger rather than the driver.
Our nurse has undertaken further training, achieving a diploma in palliative care from the University of Cape Town. His training in palliative care is ongoing. Most importantly he is an integral part of the ward team (at two hospitals) and therefore involved with counselling of both child and guardian from the time of first admission. When he later makes a home visit he does so as a known and trusted professional, not as a stranger. The team as a whole (including the chaplain) make the decision to end “curative” chemotherapy and discharge the child to home PC. We are very conscious that our PC nurse’s role is a lonely and demanding one without direct supervision in the home, but as part of the hospital team he has colleagues with whom to share his concerns. The transport of morphine and other medication has not proved problematic. Morphine sulphate solution is stable. It is prescribed by a doctor attached to the childrens cancer ward.
Result
The following table gives quantitative data on numbers of home visits. These have increased dramatically over the last 4 years as the programme has developed, though outreach visits have been curtailed recently by political unrest in N.W. Cameroon. Armed conflict and frequent road blocks have prevented travel by our palliative care nurse in the later months of 2018 (Table 2).
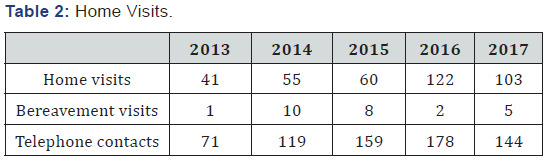
Most patients received one to three home visits, Burkitt lymphoma being the commonest diagnosis as expected from our cancer spectrum on presentation. A small sub group of Burkitt patients with residual paraplegia secondary to a treated spinal tumour received more than 3 home visits, partly to arrange and supervise rehabilitation in the community. The mean age of patients receiving home palliative care was 9 years with an age range of 7 months to 18 years. If we exclude the Burkitt patients with residual paraplegia, survival after discharge from the ward with a “terminal” diagnosis ranged from 2 weeks to more than 2 years.
Our PC nurse travels on average within a 55Km radius of the hospital, but some trips take him as far as 100Km from the hospital and will involve an overnight stay with colleagues at a distant health clinic. Distant visits are organised so as to visit several patients, not just those requiring PC but also 6 month or 1 year follow-up visits to children treated at one of our hospitals. Colleagues have rightly questioned the cost effectiveness of this form of health care delivery, but we believe that it is impossible to place a value on the visit of a caring PC professional to the home of a dying child. An attempt was made in 2015 to assess the impact of our PC home visits on quality of life issues for both patients and their guardians by Dr Mona Tamannai and colleagues [3]. Her findings were fundamentally positive, but raised many new questions, particularly regarding the expectations of parents who often thought that the visit of the PC nurse was an extension of curative treatment.
Approximately 30% of children discharged to home PC will be taken by parents to a traditional healer, most often the village practitioner, a respected man of influence in the community. Our “powerful medicine” will be seen to have failed and the village practitioner may well reiterate that the true diagnosis is “witchcraft”. On two occasions our child patient has been taken to the home of a village practitioner and our PC nurse denied access. We can only counteract this by vigorous counselling , which begins from the point of first admission of the child for treatment, and includes teaching about the nature of “cancer” and the clear statement that we cannot guarantee cure. A significant problem for us is that there is little or no concept of “cancer” in rural Cameroon. We respond to this with a vigorous outreach teaching programme mainly directed towards health workers and village practitioners
The official languages of Cameroon are French and English, but Cameroon is an ethnically and linguistically rich part of Africa. There are 280 native languages. Sixty -five percent of homes visited are recorded as having English as their main language, 35% French. On a very few occasions our PC nurse has needed to engage a local interpreter, making symptom review and meaningful communication with parents much more difficult.
Sixty percent of our children discharged to home-based PC were discharged with a supply of morphine sulphate, pain control being stabilised at the time of discharge. The requirement for opiate pain relief seems to have diminished with time, our PC nurse making full use of non-opiates on the WHO analgesics ladder. Bisacodyl is our drug of choice for constipation, but natural and easily available remedies are emphasised. Pain assessment is a core part of every visit with repeated teaching of parents and guardians regarding breakthrough pain. We have experienced no problems with morphine delivery (until the recent political strife) or with morphine misuse. Mouth care, skin and wound care, exercise and dietary advice are recorded as regular parts of PC nurse visit. We find that approximately 30% of our children have been offered traditional medicines in addition to prescribed medication. This requires careful counselling by our PC nurse and a knowledge of possible interactions. Faith is a vital support to most African families and our PC nurse will often be requested to pray with carers.
Conclusion
It is possible to deliver home based, end-of-life palliative care to children in African villages, but good outcomes are heavily dependent on effective counselling prior to discharge of the child to their home. In our experience the main carer is mother or grandmother, but sometimes more distant relatives (or non-relatives) are involved. This makes the challenge of providing counselling for all caring for the child and especially for those in a decision making role (sometimes not an immediate relative!) even greater. We try to involve other members of the wider community, particularly the pastor and school teacher. Dr Tamannai et al. [3] found that children with cancer at home were often isolated. We have been able to encourage class members to visit and even to bring school work to the child.
The most common complaint presented to our PC nurse is that of family impoverishment, because one carer, usually mother, has to relinquish work and stay with the child. We can sometimes help by facilitating community support. Questions relating to prognosis are commonly asked by parents, but often reveal little understanding of the nature of palliative care. Almost every home visit was greatly appreciated and received with thanks.
References
- Hesseling PB, Kouya F, Mbah G, Wharin P, McCormick P, et al. (2015) Burkitt lymphoma: long term outcome in 738 Patients treated with cyclophosphamide- based protocols in rural Cameroon from 2003 to 2013: o-043. Pediatric Blood & Cancer 62: S156.
- Hesseling PB, Njume E, Kouya F, Katayi T, Wharin P, et al. (2008) The Cameroon 2008 Burkitt lymphoma protocol: improved event- free survival with treatment adapted to disease stage and response to induction therapy. Pediatr Hematol Oncol 29(2): 119-129.
- Tamannai M, Kaah J, Mbah G, Ndimba J, DSouza C, et al. (2015) An evaluation of a palliative care outreach programme for children with Burkitt lymphoma in rural Cameroon. Int J Palliat Nurs 21(7): 331-337.






























