Nursing before the Hospice Care in Oncology: Integrative Review
Eliana Lessa Cordeiro1, Thais Almeida da Silva2, Liniker Scolfild Rodrigues da Silva3*, Isabelle Albuquerque Alcoforado Ferreira4, Caroline Conceição Nascimento Ribeiro5, Deborah Targino Campos5, Erick Nascimento Oliveira5 and Iara Lopes Bezerra5
1Master in Neurosciences, Federal University of Pernambuco (UFPE), Brazil
2Master in Nursing, Federal University of Pernambuco (UFPE), Brazil
3Faculty of Medical Sciences (FCM), University of Pernambuco (UPE), Brazil
4Master in Animal Biology, Federal University of Pernambuco (UFPE), Brazil
5Salgado de Oliveira University (Universe) reef (PE), Brazil
Submission: January 04, 2019; Published: February 27, 2019
*Corresponding author: Liniker Scolfild Rodrigues da Silva, Nurse Midwife, Resident in the Multidisciplinary Residency Program in Public Health, Faculty of Medical Sciences (FCM) / University of Pernambuco (UPE), Recife (PE), Brazil
How to cite this article: Eliana L C, Thais A d S, Liniker S R d S, Isabelle A A F, Caroline C N R, Deborah T C, et al. Nursing before the Hospice Care in Oncology: Integrative Review. Palliat Med Care Int J. 2019; 2(2): 555583. 10.19080/PMCIJ.2019.02.555583
Abstract
Introduction: Cancer is still a dreaded disease for many, even in the nineteenth century and is generally associated with death. Palliative care in nursing are a set of procedures that aim to ease the pain and suffering of patients terminally ill. The nurse must act applying palliative care in order to mitigate or remedy any discomfort the patient and / or family present, providing support, assess cancer pain, guide and implement effective therapy. Objective: To analyze through literature review how to read and apply nursing palliative care in cancer patients. Methods: The study was based on a survey in nursing journals in the period from 2010 to 2015 in Google’s academic databases and BIREME. Conclusion: It was concluded by the study that palliative care in patients without healing possibilities are understood humanized practices with the team and with the concern to ease the pain of cancer patients and their families. Results: humanized care; Cancer pain relief and interpersonal relationships.
Keywords: Oncology nursing; Palliative care; Cancer
Introduction
Cancer is still a dreaded disease by many even in the twenty-first century and is generally associated with death. Therefore, requires specialized care due to its complexity, it reaches patients in pain and various diseases, such as the meaning of death generally attributed to the disease, arising physical discomfort of the various types of treatment, high costs of medication, long time to treat, possible sequelae from mutilating operations, among other things [1]. Initially palliative care was provided to patients with cancer and later were extended to other areas. The palliative care in nursing is a set of procedures to alleviate the pain and suffering of terminally ill patients, that is, when the cure is not possible [2].
According to Santos et al. [3], palliative care are part of an integrated and multidisciplinary therapeutic modality to the advanced stage cancer carrier without therapeutic possibility of healing. These precautions involve low-tech and close contact, in order to provide quality of life for the remaining days for each patient. Nursing plays an important role in the team of professionals involved in palliative care where the humanization has main focus because “considers not only the physical, but also psychological concerns, social and spiritual needs of the patient” [3]. Palliative care is differentiated care approach, to improve the patient’s quality of life with advanced disease with no possibility of healing, and their families, through proper assessment and treatment for the relief of pain and symptoms. This is a psychosocial and spiritual support [1]. In oncology, the goals of care in palliative care are in line with what is required by the World Health Organization (WHO). Thus, this assistance consists of the promotion of quality of life, psychosocial and spiritual support offered to patients and their families still at relief of symptoms [4].
According to Avanci [2], both patients and their families are faced with stigma and myths about cancer, which is often seen as synonymous with death. And that causes complex psychosocial impacts, such as: fear, anguish, anxiety, psychosomatic changes. then it is up to the nursing staff to develop a comprehensive care, where the verge of death is present. Thus, the nurse must act applying palliative care to ease any discomfort to the patient and/or family present. In addition, its role is to provide support, assess cancer pain, guide and implement effective therapy for the disease development. For this it is essential that the nurse know about the pain and thus reach a position to assess and measure its complexity [5]. The palliative care in nursing is a set of procedures designed to mitigate the pain and suffering of terminally ill patients, that is, when the cure is not possible [2]. For this study could parse through literature how to read and apply nursing palliative care in cancer patients
Method
This is an integrative review study featuring a synthesis of knowledge and incorporation of the applicability of results through a survey of significant studies in practice with data collection performed from secondary sources seeking publications of journals: palliative care, nursing cancer and cancer between the years 2010-2015. For the selection of items databases were used: Google Scholar and Bireme searched articles 20 and 05 deleted; Google Scholar were investigated 19 and 03 deleted; In Medicine® they were searched and deleted 06 02. Using the following descriptors: “Palliative Care”, “Oncology” and “Nursing”. Articles published between 2010-2015 in English focusing on the objective of the study were included. As for the exclusion criteria of items for selection specify include: items that do not reflect the full content; equal articles published in the two databases; articles fleeing the purpose theme which summary and full text is not available online.
The data were performed by said subject in accordance with the objectives segments giving the criterion of: identifying items after reading the summaries and analysis of data collected in the results of each article. We use for the records a data collection instrument to dispose through tables the information gathered in focus: palliative care; oncology; nursing care to cancer patients
Results and Discussion
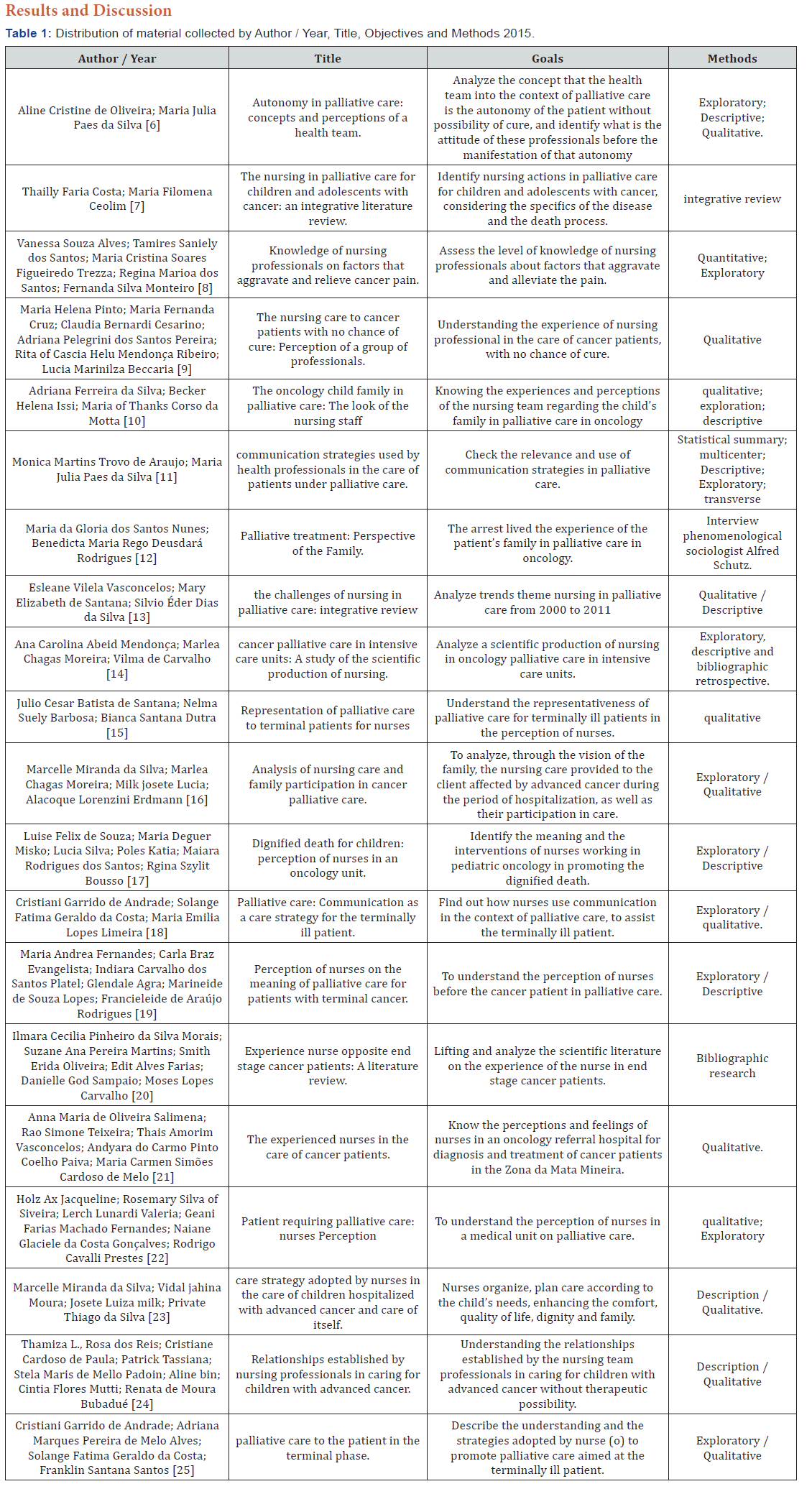
For a better explanation of the articles were placed in Table 1 all 20 articles organized by author / year, title, objectives and methods. The bonds were placed in full. The publications covered the period covered by this study, distributed according to the year of its publication. In the 20 articles studied, it is noted that in Table 1 most published studies were in 2012 and 2013. The study aimed to: “The nurses experience on palliative care in cancer patients,” “The perception of nurses for palliative care, “the communication strategy used by nurses “and” Understanding the vision of the family in palliative care. “ This makes us think that nurses are increasingly using in the context of palliative care, as the main tool humanization, and can count as well as its great ally family that cancer patients with no prospect of cure, this union is of paramount importance to the patient. It can thus be offered more comfort, quality of life, dignity and ease cancer pain.
It was observed that of the 20 items surveyed the most used method was the quality that has as its goal “The not want to explain events with people, individually or collectively, listing and measuring their behaviors or quantitatively correlating events of their lives (Table 2). But he wants to know their background experiences and their representations these people have these life experiences”. The authors Oliveira et al. [6] say that the verbal and non-verbal communication is reaffirmed as elements essential to the definition and recognition of the autonomy of the patient without possibility of cure. The Costa authors; Ceolim [7], says that the complexity of care to children / adolescents with cancer, especially during palliative care, nursing practice requires the solidarity actions and guided compassion, so that offer support for parents and children
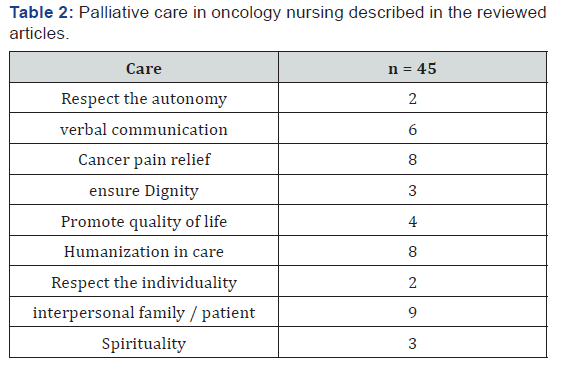
The authors Alves et al. [8] speaks of the need for a better preparation of the professional for the care provided to patients with cancer pain, so there is a proper evaluation and recording this, aiming to better results in pain management, is tyingknowledge and action. The authors Pinto et al. [9] says that patient care was restricted to physical care and confrontation occurred with individual strategy may jeopardize patient safety. The unpreparedness of the professionals for the emotional care was the main difficulty reported with evidence of their training needs. The authors Silva et al. [10] says that by exposing their conceptions of what they consider palliative care professionals bring the specifics of care that has been improved over time professional in the pediatric oncology, the share of existence with the children and their families.
The authors Araujo et al. [11] says that the most cited verbal strategies were questioning nature of the disease, treatment and, in the non-verbal, stood out the affective touch, look, smile, physical closeness and active listening. They showed little knowledge of communication strategy. professional training regarding communication in palliative care it is necessary. The authors Nunes et al. [12] says that it is up to the nurse to develop comprehensive care from the perspective of interdisciplinary palliative approach as a role model to give visibility to patientfamily- professional relationship. The authors Vasconcelos et al. [13] says that nursing can act to support the patient and the family group, making it possible to minimize the fears and anxiety and collaborate with the appropriate involvement of both in the process. We see the need for training of palliative care professionals that meet the needs not only of patients but to enable a support to the family and the care of the patient
The authors Mendonca et al. [14] says that in regard to the obstacles to the implementation of the oncology palliative care in the ICU, highlighted the lack of knowledge about this type of therapy by the professionals working in these units. This problem is also given attention in Brazil, given the design of vocational training policies. Santana et al. [15] says that one sees a short unpreparedness of nurses in dealing with situations involving end-of-life. In the hospital the nursing staff is the one that deals with patients in the final stage of life, which brings him both physical and emotional distress, as to provide quality care requires that nurses beyond the knowledge and skills are good about yourself. The authors Silva et al. [16] says that the family value that nursing care is empathetic with good humor, competent, based on communication, participate in the care and may have physical and psychosocial needs of order. Nursing should contribute to the strengthening of relations with family members, and seek to serve their needs, aiming at quality of care.
The authors Sousa et al. [17] says that nurses participating in the study identified the child’s dignified death characteristics and described the interventions used to promote dignified death, especially pain relief and family care. Given these results identify not only intrinsic aspects for the promotion of dignified death, such as maturity of the professional and meaning it attaches to the death, as well as extrinsic factors, such as autonomy and comfort. The authors Andrade et al. [18] says that communication between nurses and the terminal patient, emphasizes the importance of a patient-centered care in its entirety, and not only in their disease. The communication is configured as an effective element of care to the terminally ill patient and is of paramount importance for the promotion of palliative care. The authors [19] says that the nurse recognizes that reaching the final destination with dignity is a process that involves respect to the condition and the patient’s opinions about being who experiences a phase of life with limitations, fears and anxieties. the nurse involved recognize the importance of the multidisciplinary team, providing the nurse reflections on the use of communication as an essential element of care for patients and family in palliative care.
The authors Morais et al. [20] says that the experiences of nurses is marked by conflicting situations, exposing these professionals to an atmosphere of negative feelings that interfere with patient care and health professionals, in some cases. The use of coping techniques and psychological support that the institution offering this professional can reduce stress. The authors Salimena et al. [21] says that the nursing care can be understood in its technical aspects, ethical and human, since it enables the further development of interpersonal relationships among those who care and those maintained. For nurses to patient care is not only in performing technical tasks, but have skills to learn to listen, talk and realize that a simple conversation with the patient makes the assistance be given quality.
The authors Machado et al. [22] says that it was realized that there is difficulty in performing palliative care due to lack of knowledge on the part of the nurses and the institutional structure, which is not directed to palliative care. An apparent theme of ignorance on the part of the nurses interviewed and that despite this, the implementation of palliative care for shares is made and valued in their doing. The authors Silva et al [23] says that the nurse who works in the oncology area is housed in a complex and challenging situation facing the possibility of dealing with the death and dying process in their daily work. Nurses organized, plan and implement care according to the child’s needs. The authors Paula et al. [24] speaks of the difficulty nurses experience in dealing with children with cancer and their families. Professionals spend to develop palliative care as a way to make the experiences of childhood cancer suffered the least possible, both for children and for your family. The authors Andrade et al. [25] realize the importance of centralized patient care in the terminal phase. Professionals appreciate not only the biological aspects of the patient, but also other dimensions, psychological, social and spiritual [26-30].
Final
Through this study, we address some of view of nurses with a focus on palliative care in oncology, and how the same are dealing with and applying this care in patients with no prospect of cure [31-37]. All cited palliative care, we observed a greater concern of nursing with the humanization and cancer pain of these patients, in addition to the way that nurses deal with their families, causing the same to be involved in the action of caring for a way that adds value to staff and for the patient, contributing to the emotional and psychological comfort during the period of hospitalization. No easy task for the nurse that act of caring without possibility of cure, experiencing the death and dying every day. It is almost impossible there is no emotional involvement. Still they implement, plan and organize palliative care for the patient and his family go through this difficult time maintaining the dignity of this patient, respecting their autonomy and individuality, keeping the verbal and nonverbal and finally respecting their spirituality.
References
- Franca JRF, de S, et al. (2013) Importância da comunicação nos cuidados paliativos em oncologia pediátrica: enfoque na Teoria Humanística de Enfermagem. Rev Latino Am Enfermagem 21(3): 780-786.
- Avanci BS, Carolindo FM, Goes FGB, Cruz Netto NP (2009) Cuidados paliativos à criança oncológica na situação do viver/morrer: A ótica do cuidar em enfermagem. Esc Anna Nery 13(4): 708-716.
- Santos MCL, Pagliuca LMF, Fernandes AFC (2007) Cuidados paliativos ao portador de câncer: reflexões sob o olhar de Paterson e Zderad. Rev Latino-Am Enfermagem 15(2): 350-354.
- Silva MM da E, Moreira MC (2011) Sistematização da assistência de enfermagem em cuidados paliativos na oncologia: visão dos enfermeiros. Acta paul enferm 24(2): 172-178.
- Waterkemper R, Reibnitz KS (2010) Cuidados paliativos: a avaliação da dor na percepção de enfermeiras. Rev Gaúcha Enferm 31(1): 84-91.
- Oliveira AC, Silva MJP (2010) Autonomia em cuidados paliativos: conceito e percepções de uma equipe de saú Acta Paul Enfem 23(2): 212-217.
- Costa TF, Ceolim FA (2010) enfermagem nos cuidados paliativos a criança e adolescente com câncer: revisão integrativa e literatura. Rev Gaúcha Enferm porto alegre 31(4): 776-784.
- Alves SV, Santos TS, Trezza MCSF, Santos RM, Monteiro FS (2011) Conhecimento de profissionais da enfermagem sobre fatores que agravam e aliviam a dor oncoló Revista Brasileira de Cancerologia 1(1): 19-32.
- Pinto MH, Cruz MF, Cesarino CB, Pereira APS, Ribeiro RCM, et al. (2011) O cuidado de enfermagem ao paciente oncológico fora de possibilidade de cura: percepção de um grupo de profissionais. Cogitare Enferm 16(4): 647-653.
- Silva FA, Issi HB, Motta MGC (2011) A família da criança oncológica em cuidados paliativos: o olhar da equipe de enfermagem. Cienc Cuid Saude 10(4): 820-827.
- Araújo MMT, Silva MJP (2012) Estratégia de comunicação utilizadas por profissionais de saúde na atenção à pacientes sob cuidados paliativos. Rev Esc Enferm 46(3): 626-632.
- Nunes MGS, Rodrigues BMRD (2012) Tratamento paliativo: perspectiva da famí Rev Enferm UERJ 20(3): 338-343.
- Vasconcelos EV, Santana ME, Silva SED (2012) Desafios da enfermagem nos cuidados paliativos: revisão integrativa. Enfermagem em foco 3(3): 127-130.
- Mendonça ACA, Moreira MC, Carvalho V (2012) Atenção paliativa em unidade de terapia intensiva: um estudo da produção cientifica da enfermagem. Esc Anna Nery 16(4): 817-823.
- Santana JCB, Barbosa NS, Dutra BS (2012) Representatividade dos cuidados paliativos aos pacientes terminais para o enfermeiro. Rev de enfermagem 15(1): 549-554.
- Silva MM, Moreira MC, Leite JL, Erdmann AL (2012) Análise do cuidado de enfermagem e da participação dos familiares na atenção paliativa oncoló Texto Contexto Enferm 21(3): 658-666.
- Souza LF, Misko MD, Silva L, Poles K, Santos MR, et al. (2013) Morte digna da criança: percepção de enfermeiros e uma unidade de oncologia. Rev Esc Enferm 47(1): 30-37.
- Andrade CG, Costa SFG, Lopes MEL (2013) Cuidados paliativos: a comunicação como estratégia de cuidado para o paciente em fase terminal. Ciência & Saúde Coletiva 18(9): 2523-2530.
- Fernandes MA, Evangelista CB, Platel ICS, Agra G, Lopes MS, et al. (2013) Percepção dos enfermeiros sobre o significado dos cuidados paliativos em pacientes com câncer terminal. Ciência & Saúde Coletiva 18(9): 2589-2596.
- Martins ASP, Sampaio DD, Soares EO, Farias EA, Morais ICPS, et al. (2013) Vivencia do enfermeiro frente ao paciente oncológico em fase terminal: uma revisão da literatura. Rev Interdisciplinar 6(1): 96-104.
- Salimena AMO, Teixeira SR, Amorim TV, Paiva ACPC, Melo MCSC (2013) O vivido dos enfermeiros no cuidado paliativo ao paciente oncoló Cogitare enferm 18(1): 142-147.
- Machado JH, Silveira RS, Lunardi VL, Fernandes GFM, Gonçalves NGC, et al. (2013) Paciente que requer cuidados paliativos: percepção de enfermeiras. Enferm Foco 4(2): 102-105.
- Silva MM, Vidal JM, Leite JL, Silva TP (2014) Estratégia de cuidados adotadas por enfermeiros na atenção à criança hospitalizada com câncer avançado e no cuidado de si. Cienc Cuid Saúde 13(3): 471-478.
- Bin A, Paula CC, Mutti CF, Bubadue RM, Padoin SMM, et al. (2014) Relações estabelecidas pelos profissionais de enfermagem no cuidado às crianças com doença oncológica avanç Aquuichan 14(4): 496-508.
- Alves AMPM, Andrade CG, Santos FS, Costa SFG (2014) Cuidados paliativos ao paciente em fase terminal. Revista Baiana de Enfermagem 28(2): 126-133.
- Benarroz MO, Faillace GBD, Barbosa LA (2009) Bioética de saúde pública e nutrição em cuidados paliativos oncológicos em adultos. Cad Saúde publica 25(9): 1875-1888.
- Boemer RM (2009) About palliative care (sobre cuidados paliativos). Rev Esc de enfermagem 43(3): 65.
- Correia FR, Carlo MRP (2012) Avaliação de qualidade de vida no contexto dos cuidados paliativos: revisão integrativa de literatura. Rev latino-Am enfermagem 20(2): 401-410.
- Fioriani CA, Schramm FR (2008) Cuidados paliativos: interfaces, conflitos e necessidades. Ciencia saúde coletiva 13(Suppl 2): 2123-2132.
- Fonceca JVC, Rebelo T (2011) Necessidades de cuidados de enfermagem do cuidador da pessoa sob cuidados paliativos. Revista Bras Enferm 64(1): 180-184.
- González JS, Ruiz MDCS (2012) Historia os paliativos em las sociedades primitivas :revision integrativa: Revisão integrativa. Rev esc enferm 46(4): 1015-1022.
- Lopes VF, Silva JLAM (2007) The professional nursing perception about palliative cares to oncologic pediatric is of cure possibility patient: a study in phenomenological boarding of the relation human beings. online brazilin journal of nursing home 6(3).
- Pinheiro TRSP (2010) Avaliação do grau de conhecimento sobre cuidados paliativos e dor dos estudantes de medicina do quinto e sexto anos. Mundo da saúde 34(3): 320-326.
- Rodrigues IG, Zago MMF (2012) A morte e o morrer: maior desafio de uma equipe de cuidados paliativos. ciêcui saúde 1(supplement): 031-038.
- Souza KC, Carpigiani B (2010) Dito, Não ditos e entreditos: a comunicação em cuidados paliativos. Psicol teor prat 12(1).
- Silva VA, Sales CA (2013) Encontro musicais como recurso em cuidados paliativos oncológicos a usuários de casas de apoio. Rev Esc enferm 47(3): 626-633.
- Silva MM, Moreira CM (2010) Desafios a sistematização da assistência de enfermagem em cuidados paliativos oncológicos: uma perspectiva da complexidade. Rev Eletr 12(3): 483-490.






























