Palliative Care and Religiosity as a Way of Coping with Death in Latin America Palliative Care and Religiosity in Latin America
Caio Vinicius Botelho Brito*, Cassia Michelle Almeida Fernandes, Amalia Costa Coimbra and Ana Maria Costa Rodrigues
Department of medicine, Pará State University, Brazil
Submission: January 17, 2019; Published: February 19, 2019
*Corresponding author: Caio Vinicius Botelho Brito, Department of medicine, Pará State University, College of medicine, Avenida Cabanos, 2.264, Ed. Fort Lauderdale, apt. 1.101 CEP 66033-000. Belém/PA, Brazil
How to cite this article: Caio V B B, Cassia M A F, Amalia C C, Ana M C R. Palliative Care and Religiosity as a Way of Coping with Death in Latin America Palliative Care and Religiosity in Latin America. Palliat Med Care Int J. 2019; 2(1): 555579. 10.19080/PMCIJ.2019.02.555579
Abstract
Palliative care is an approach that aims to improve the quality of life among patients affected by terminal illnesses. It is not limited only to the relief of physical pain, but also includes psychological and spiritual care. The present review aims to understand how this process occurs in Latin American countries and how Latin American religiosities contribute to it. The inclusion criteria were studies placed in Latin America countries and dated back to the last five years. 12 articles were selected using the descriptors “Palliative Care” and “Spirituality” or “Religiosity” in databases of the Scientific Electronic Library online (SCIELO), the Latin American and Caribbean Literature in Health Sciences (LILACS) and the MEDLINE/PUBMED. Catholic, Evangelical, Spiritist and Umbandist patients were identified. Religiosity has been able to maintain belief in the healing process, to promote acceptance of death and to provide comfort and even improvement in symptoms. Moreover, relatives, caregivers and professionals also take benefit of religiosity. Nevertheless, in Latin American countries, the palliative care services are separated from other health services and there is still a deficit in students’ and professionals’ education about the theme, which demonstrates the need of greater investment in palliative care services in Latin America and the recognition of its importance in all aspects
Keywords: Palliative care; Religion and medicine; Latin America
Abbrevations: WHO: World Health Organization; SCIELO: Scientific Electronic Library online; LILACS: Latin American and Caribbean Literature in Health Sciences
Introduction
According to the World Health Organization (WHO), palliative care is defined as an approach that aims to improve the quality of life of patients with life-threatening illnesses and their families, through the relief of pain and of other psychosocial and spiritual problems. Therefore, it is not limited only to the relief of physical pain, also including relief to other distressing symptoms, support to the patient and the family in order to facilitate the coping process, promotion of active life and attention to the psychological and spiritual aspects of care [1-3]. Furthermore, it is also important that the palliative care strategy is developed by a multi-professional team that understands that the focus is not the disease itself, but the patient as a whole, who has the right to information and autonomy. It is worth emphasizing that healthcare, in its many aspects, must be distinguished and specific to the needs of each patient and their respective family [2,3]. In both rich and poor countries, there is a need for palliative care services; however, access to such services in low- and middle-income countries, such as African and Latin American countries, still remains variable and sometimes non-existent [4]. Often the focus of such countries is restricted to prevention and control of diseases, including in the academic setting, where learning about palliative care is often restricted to specific areas such as oncology. Another problem evidenced by WHO concerns the inadequate control of pain in these countries, due to the difficult access to opioids, such as morphine, by a large number of patients because of law-restricted availability of narcotics [5].
Among the principles of palliative care defined by WHO, the reaffirmation of life’s importance stands out, considering death as a natural process; hence, the established care to the patient must not accelerate the arrival of death. Thus, the palliative care approach is a form to help coping with death and grief [6]. In addition, spirituality is a personal subjective experience, often used as a way to find answers to questions about the meaning of life and death, with special importance given the variety of forms of religiosity in Latin America [7].
In this context, the importance of spirituality in the treatment of palliative care patients is noticeable; therefore, the present review aims to understand how this process occurs in Latin American countries and how Latin American religiosities contribute to it.
Method
The descriptors “Palliative Care” and “Spirituality” or “Religiosity” were used, in English, Portuguese and Spanish, in databases of the Scientific Electronic Library online (SCIELO), Latin American and Caribbean Literature in Health Sciences (LILACS) and MEDLINE/PUBMED. Original articles placed in Latin America, dated back to the last five years and related to the topic were chosen amongst others. The results obtained were filtered by reading the titles and abstracts and, later on, by the reading of the entire text. A total of 108 references were selected, 12 from LILACS, 13 from SCIELO and 83 from MEDLINE/ PUBMED. From these, 5 duplicated references were removed; then, 86 articles were excluded post reading their title and abstract given their incompatibility with the inclusion criteria, henceforth including 17 articles. Another 5 were excluded, then, because they presented methodological issues or did not fit the proper theme after the entire articles were read; ultimately, 12 articles were included in the qualitative synthesis (Figure 1).
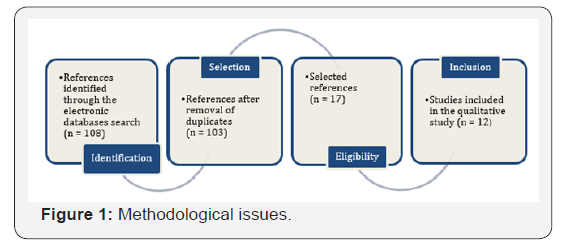
Discussion
Spirituality can be understood as a set of personal values that guide choices and perspectives, and it may or may not be manifested through religiosity, which represents a set of practices and beliefs for the purpose of explaining life and death [8]. In Latin America, considering the migratory movements since the colonization, as well as the historical presence of several indigenous groups, there is now a great variety of religious practices, including Eastern religions, Judaism, Afro-American religions and spiritism, despite the known predominance of the catholic and evangelical religions. In Brazil, according to the 2010 census, 65% of the population was Catholic, 22.4% evangelical and 8% without religion [9,10]. In the present study, twelve articles were selected concerning the topic of spirituality in palliative care, carried out in Latin America, involving patients, caregivers and health professionals. It was observed how religiosity is able to influence the way in which patients face the disease and the treatment, as well as the presence of a great variety of religions in the health services. Among those, patients identified as Catholics, Evangelicals, Spiritists, Umbandists (a syncretic African-Brazilian religion) and, also interactions between religious practices [11-13].
One of the main contributions of religiosity to the treatment of patients with terminal diseases is the possibility of providing hope even under unfavorable prognoses. According to Benites et al. [11] oncology patients in exclusive palliative care were able to maintain belief in healing and plans for the future based on religiosity. Moreover, even when this hope was not sustained, religiosity was able to promote acceptance of death’s process through understanding it not as the end of life, but as a temporary form. This point of view is also shared by other studies, in which even under the idea of inevitable death, patients were able to associate it with continuity in order to give meaning to their sufferings [12].
Furthermore, those beliefs are important means of support to the patient with terminal illnesses, for example as a complement to the therapeutic resources. Many patients have reported comfort and even relief and improvement in symptoms through activities such as reading religious texts, prayers, meditation, visiting spiritual assistants, minsters and priests; and listening to songs related to their respective religions. Acknowledgment of the importance of these activities by health professionals makes them, in many cases, more part of their patients’ daily routines. In this context, faith and science can be seen as interdependent ways of promoting well-being [12,14]. It is also worth emphasizing that spirituality can affect the quality of life. In a study comparing cancer patients in palliative care with healthy patients, both groups listed religiosity as an important part of their lives, most using faith in a positive way. On the other hand, among those who did negative associations, the majority were from the group of cancer patients. Such associations were related to the sensation of guilt, anger and understanding the disease as a punishment [15,16]. Nevertheless, some patients also saw death as a form of relief from physical suffering and pain, reporting the desire to “settle the scores” with a superior entity [12].
Under facing the process of death, many patients in palliative care start to give more value to simple daily activities and to approach family and friends [11,12]. In addition, relatives and caregivers themselves benefit from religiosity by helping them to deal with the physical and emotional overload they are subjected to, using it as a source of motivation and comfort, as well as support for the suffering caused by the illness of their loved ones [17,18]. This understanding can also be extended to health professionals, whose religiosity often provides meaning to the work performed, especially when there are no more therapeutic measures available. Many professionals report the opportunity to bethink about their lives and a type of comfort based on religion when a patient is lost [14]. Regardless of the religiosity of those professionals, it has become increasingly important that the multi-professional team recognizes the meaning of spirituality for the patient and respects their religious expressions. Several patients and professionals report that when the professional understands and interacts with the patient’s beliefs, the trust in the treatment increases and even the meaning that the patient puts in the situation that they are living. [19,20] Albeit, not all professionals are prepared to address the subject with their patients, and often have difficulty understanding it [21].
In the same context, the lack of preparation of some professionals reflects the broad heterogeneity of palliative care services around the world. While most countries in Europe and North America already have well-applied and integrated services in health systems, in Latin America, except for Chile, Costa Rica, and Uruguay, palliative care services are performed isolated, usually apart from other health services or restricted to oncological units. Thus, there is still a deficit in training professionals on the subject, and some countries do not include palliative care in the curricula of their medical schools. Therefore, the need for greater investment in palliative care services in Latin America and the recognition of its importance in all aspects, including the religious one, stands out due to the variety of beliefs in the area and the impact of this facet in the treatment of many patients [22,23].
Conclusion
Latin America has a great variety of religions, and religiosity is very important for patients in palliative care, promoting coping with death, hope of healing, relief of symptoms and the strengthening of affective relationships. It is extremely important that health professionals know how to approach spirituality of patients in palliative care, however, in many countries in Latin America, there is still no adequate preparation of these professionals on the subject and these services are performed separately to other health services.
References
- World Health Organization (WHO) (2009) Definition of Palliative Care. Geneva: WHO, Switzerland.
- Donato SC, Matuoka JY, Yamashita CC, Salvetti MG (2016) Effects of dignity therapy on terminally ill patients: a systematic review 50(6): 1014-1024.
- Bhattacharya P, Dessain SK, Evans TL (2018) Palliative Care in Lung Cancer: When to Start. Curr Oncol Rep 20(11): 90.
- Downing J, Boucher S, Daniels A, Nkosi B (2018) Paediatric Palliative Care in Resource-Poor Countries. Children (Basel) 5(2).
- Schrijvers D (2007) Should palliative care replace palliative treatment for cancer in resource-poor countries? Lancet Oncol 8(2): 86-87.
- Rodrigues IG, Zago MMF (2012) A morte e o morrer: maior desafio de uma equipe de cuidados paliativos. Cienc Cuid Saude 11: 31-38.
- O Brien MR, Kinloch K, Groves KE, Jack BA (2019) Meeting patients’ spiritual needs during end of life care: A qualitative study of nurses’ and healthcare professionals’ perceptions of spiritual care training. J Clin Nurs 28(1-2): 182-189
- Oliveira SG, Sartor SF, Morais ES, Maya NF, Gervini CMB, et al. (2017) Espiritualidade, religiosidade e terminalidade: temas possíveis nas visitas domiciliares realizadas a cuidadores familiares. Reupfi 6(2): 69-73.
- Oro AP, Ureta M (2007) Religião e política na América Latina: uma análise da legislação dos paí Horiz Antropol 13(27): 281-310.
- Brazilian Institute of geography and statistics (2010) Demographic sense. General characteristics of the population, religion and people with disabilities.
- Benites AC, Neme CMB, Santos MA (2017) Significance of spirituality for patients with cancer receiving palliative care. Estud Psicol 34(2): 269-279.
- Arrieira ICO, Thofehrn MB, Millbrath VM, Schwonke CRGB, Cardoso DH, et al. (2017) O sentido da espiritualidade na transitoriedade da vida. Esc Anna Nery 21(1): 1-6.
- Silva JO, Araujo VMC, Cardoso BGM, Cardoso MGM (2015) Spiritual dimension of pain and suffering control of advanced cancer patient. Case report Rev Dor São Paulo 16(1): 71-74.
- Arrieira ICO, Thoferhn MB, Schaefer OM, Fonseca AD, Kantorski LP, et al. (2017) The sense of spiritual care in the integrality of attention in palliative care. Rev Gaúcha Enferm 38(3):
- Meneguin S, Matos TDS, Ferreira MLSM (2018) Perception of cancer patients in palliative care about quality of life. Rev Bras Enferm 71(4): 1998-2004.
- Matos TDS, Meneguin S, Ferreira MLS, Miot HÁ (2017) Quality of life and religious spiritual coping in palliative cancer care patients. Rev Latino Am Enfermagem 25: e2910.
- Rocha RCNP (2017) Experiences and spiritual needs of the family caregiver of cancer patient receiving palliative care [thesis]. Niterói: uff nursing faculty.
- Paiva BS, Carvalho AL, Lucchetti G, Barroso EM, Paiva CE (2015) “Oh, yeah, I’m getting closer to god”: spirituality and religiousness of family caregivers of cancer patients undergoing palliative care. Support Care Cancer 23(8): 2383-2389.
- Evangelista CB, Lopes MEL, Costa SFG, Abrão FMS, Batista PSS, et al. (2016) Spirituality in patient care under palliative care: A study with nurses. Esc Anna Nery 20(1): 176-182.
- Manchola C, Brazão E, Pulschen A, Santos M (2016) Palliative care, spirituality and narrative bioethics in a specialized unit. Rev bioét (Impr) 24(1): 165-175.
- Silva BS, Costa EE, Picasso IGS, Silva G, Silva AE, et al. (2016) Perception of nursing team on spirituality in end of life care. Cogitare Enferm 21(4): 1-8.
- Gutierrez NR (2016) The wandering of death: Palliative care, utopia or reality? Medunab 19(1): 46-55.
- Pastrana T, De Lima L, Wenk R, Eisenchlas J, Monti C, et al. (2014) Atlas of palliative care in latin america. (1st edn), IAHPC Press, Houston, Texas, USA, 28(10): 1231-1238.






























