Palliative Care in Congenital Syndrome of the Zika Virus: A Series of Cases
Aline Maria de Oliveira Rocha*, Maria Julia Gonçalves de Mello, Juliane Roberta Dias Torres, Natalia de Oliveira Valença, Alessandra Costa de Azevedo Maia and Nara Vasconcelos Cavalcanti
Department of Integral Medicine, Institute of Integrale Medicine, Universidade de Pernambuco, Brazil
Submission: December 06, 2018; Published: January 04, 2019
*Corresponding author: Aline Maria de Oliveira Rocha, Institute of Integrale Medicine, Rua dos Coelhos, 300, Boa Vista, Recife- PE, Brazil
How to cite this article: Aline M d O R, Maria J G d M, Juliane R D T, Natalia d O V, Alessandra C d A M, et all. Palliative Care in Congenital Syndrome of the Zika Virus: A Series of Cases. Palliat Med Care Int J. 2019; 1(3): 555565. 10.19080/PMCIJ.2019.01.555565
Abstract
Background: Congenital syndrome of zika virus (CSZV) is associated with neuromotor and cognitive developmental disorders, limiting the independence and autonomy of affected children and high susceptibility to complications, so palliative care needs to be discussed and applied. Aim: Observe hospitalizations of patients with CSZV and clinical interventions performed from the perspective of palliative care. Design: A cross-sectional observational study. Data were collected between May and October 2017 through the review of medical records and interviews with relatives of patients hospitalized. Setting/Participants: Developed in a tertiary care hospital involving patients with confirmed CSZV born as of August 2015 and followed up until October 2017. Patients under investigation were excluded. Results: Were observed 13 hospitalizations in this period, which occur at an early age and were accompanied by a high number of invasive procedures and interventions. An approach in palliative care was only identified in two hospitalized patients. Conclusion: For the patient with known severe malformations caused by congenital infection by the zika virus with indication of palliative care, this approach could be used in order to allow life without suffering and disproportionate invasive method.
Keywords: Microcephaly; Zika virus; Palliative care; Hospitalization
Abbrevations: WHO: World Health Organization; HC: Head Circumference; VPS: Ventriculo-Peritoneal Shunt; CSZV: Congenital Syndrome of Zika Virus; MR: Magnetic Resonance; CSF: Cerebrospinal Fluid; VPS: Ventriculo-Peritoneal Shunt; nasogastric tube (NGT), PVP: Peripheral Venous Punction; CVP: Central Venous Punction; GTT: Gastrostomy; OTT: Orotracheal Tube; CPAP: Continuous Positive Airway Pressure; DVC: Delay Vesical Catheter; MRR: Metropolitasna Region of Recife; ICU Indic: Indicates Intensive Care Unit
Introduction
Between August and November 2015, a substantial increase in the number of cases of newborns with microcephaly [1], characterized by the World Health Organization (WHO) as an “anomaly in which the head circumference (HC) is less than two or more standard deviations than the reference for sex, age or gestational age” [2]. This clinical condition leads to medicalization, hospitalization and invasive procedures such as ventriculo-peritoneal shunt (VPS) and gastrostomy. The innumerable associated morbidities and limited quality of life emphasize the need to discuss palliative care in this group [3-6]. It was possible to correlate such an aggravation to the infection by zika virus during pregnancy, which is transmitted to the fetus, and may result in miscarriage [7], fetal death or congenital anomalies in several organs, being characterized as Congenital Syndrome of Zika virus (CSZV) [8-11]. CSZV has become a clinical condition associated with several complications, with a disabling and non-curable nature [12-16].
Such clinical manifestations have caused from the first semester of life on, for example, a high frequency of epileptic seizures, changes in tone, posture and mobility, irritability, intracranial hypertension secondary to hydrocephalus, and swallowing problems with greater predisposition to gagging and respiratory infections [16-18]. Palliative care is understood as active and total approach to care, which begins from diagnosis of life-limiting or life-threatening conditions and continues throughout the child’s life and death [6]. Therefore, this type of care is clearly indicated for diseases with severe and incapacitating neurological manifestations, such as CSZV. The goal of the present study was observe the hospitalizations and interventions performed of patients with CSZV, analyzing them according to the perspective of palliative care
Material and Methods
A cross-sectional observational study involving patients with CSZV. The research involved patients born with CSZV as of August 2015 and followed up until October 2017 and data collection occurred between May and October 2017. Patients with characteristic neurological images on computed tomography (CT) and magnetic resonance (MR) and/or positive IgM serology for Zika virus in cerebrospinal fluid (CSF) were included. A list of patients accompanied at the clinic specialized in CSZV was made, followed by an analysis of the medical records and a search in the hospital’s internal information system.
The inpatients’ companions were informed about the purpose of the study and, upon agreeing to participate, a free informed consent form was requested, and the questioner was completed by interview and analysis of medical records. This project was approved by IMIP’s Ethics Committee in Research under protocol no. 54701516.1.0000.5201.
Results and Discussion
It was possible to observe hospitalizations of 13 patients prospectively and the data are shown on Table 1. Almost all these patients (92.3%) underwent invasive procedures during hospitalization, the most common being peripheral venous puncture (92.3%). Such procedures provoke pain during its accomplishment and discomfort during the period of use. Therefore, procedures may become useless and an idle cause of suffering if they are not indicated [19]. Two (15.4%) of the patients had their records requested for a first-time ICU vacancy, both due to acute respiratory failure. After a better understanding by the medical team that assisted them regarding the functionality, characterization of the clinical condition and associated with the basis disease, the request for a vacancy in the ICU was suspended and after conversation and clarification with companions, palliative care measures were indicated: patient number three was submitted to palliative extubation according to precepts of palliative care and airway support was installed with continuous positive pressure and patient number nine had the bladder catheter of delay and central venous access removed; for both the order of non-resuscitation was expressed and symptom control measures were performed (analgesia).
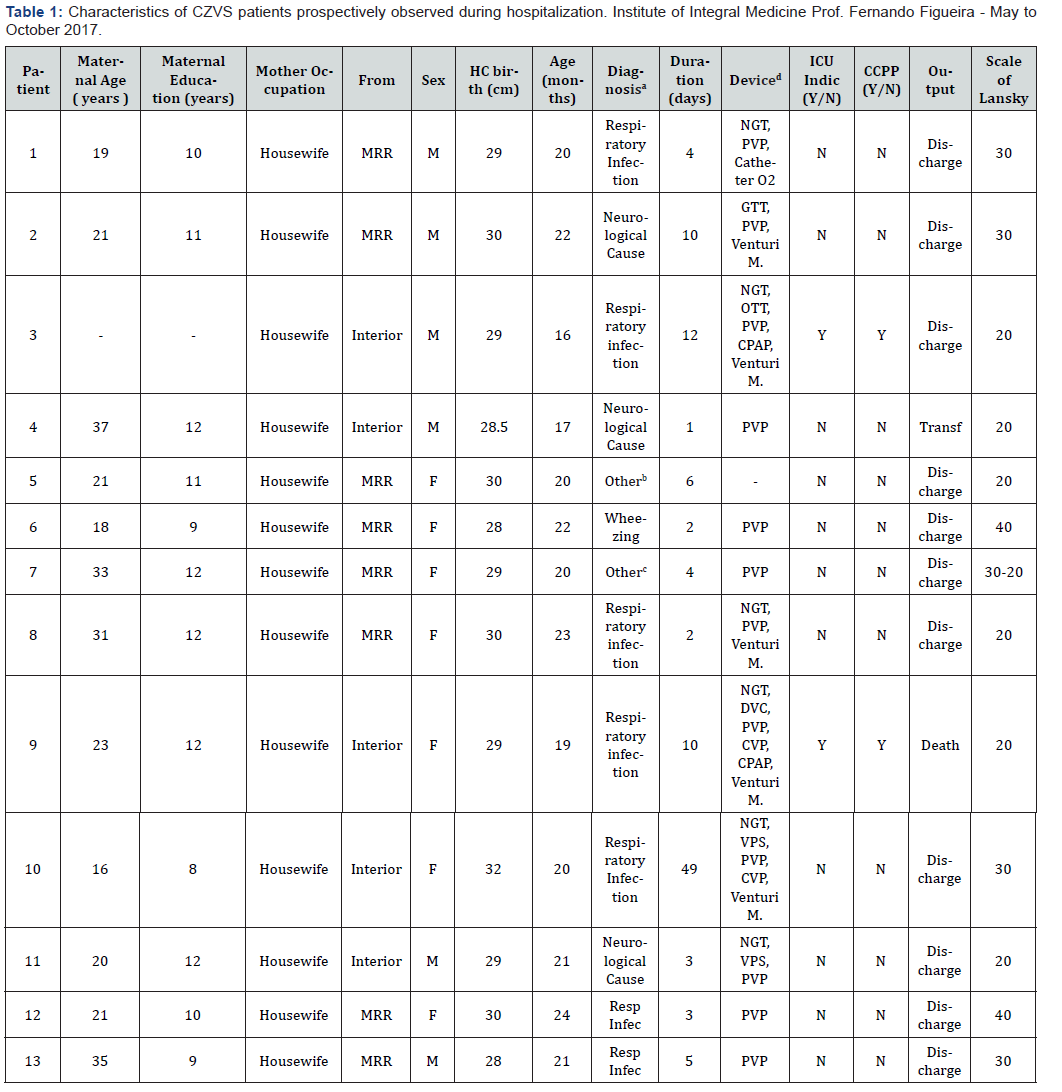
hydrocephalus); Wheezing; Others. b: Other: Conjunctivitis. c: Other: Fever without localized signs. d: Abbreviation of devices: nasogastric tube (NGT), peripheral venous punction (PVP), central venous punction (CVP), gastrostomy (GTT), orotracheal tube (OTT), Continuous Positive Airway Pressure (CPAP), Venturi mask (Venturi M.), Delay vesical catheter (DVC), ventriculo-peritoneal shunt (VPS). e: Acronyms / Abbreviations: Metropolitasna Region of Recife (MRR) Transference (Transf) , Male/Female (M/F), Yes/No (Y N), Indicates Intensive Care Unit (ICU Indic), Palliative Care (CCPP) .
However, most families and caregivers received no approach to palliative care during hospitalizations, despite the basic conditions of the children. It is understood that, as an emerging aspect of pediatric practice, professionals postpone such an approach until the end of life or do not use it [19]. The need to perform surgical interventions and long hospitalizations in ICU is frequent in children born with malformations, which implies in thinking about the limits of the therapeutic effort in these cases [19]. According to precepts of palliative care, obstinate therapeutic investments in patients without a cure perspective, should be avoided [4,5].
One of these patients died during hospitalization at 19 months of age and the family was present at all times, including death. The other patient with indication of palliative measures received discharge from hospital with written guidelines in summary over the care plan that was drawn up during and after hospitalization. The remaining patients were discharged and there was no report or description of approach in palliative care intended for them
Conclusion
Despite the short life span of children with CSZV, it could be observed through this study that they were submitted to an excessive invasive procedures. It is understood that the patient with severe malformations already known as those caused by congenital infection by zika virus could be identified early for care that would allow life without suffering and without any disproportionate invasive method
Acknowledgement
Rui Neves Rehabilitation Center’s team and the medical records system’s team of the Institute of Integral Medicine Prof. Fernando Figueira. Relatives and patients who collaborated to the research. PGMB for the contribution during the development of the study.
Conflict of Interest
The authors declares that there is no conflict of interest
References
- saude.gov.br/svs
- WHO (2017) Birth defects surveillance: a manual for program managers. World Health Organization, Switzerland.
- Teixeira MG, MCN Costa, Oliveira WK de, Nunes ML, Rodrigues LC (2016) The epidemic of zika virus-related microcephaly in Brazil: Detection, control, etiology and future scenarios. Am J Public Health 106(4): 601-605.
- Iglesias SOB, Zollner ACR, Constantino CF. Pediatric palliative care. Resid Pediatr. 2016; 6 (Suppl 1): 46-54.
- Chambers L, Dodd W, McCulloch R, McNamara-Goodger K, Thompson A (2003) A Guide to the Development of Children's Palliative Care Services.
- Ministry of Health, Secretariat of Health Surveillance, Secretariat of Health Care. (2017) Integrated guidelines for surveillance and health care within the Public Health Emergency of National Importance: procedures for monitoring changes in growth and development from gestation to the first childhood, related to the infection by zika virus and other infectious etiologies within the operational capacity of SUS. Brasília.
- State Secretariat of Health of Pernambuco (2015) Executive Secretariat of Health Surveillance. Clinical and Epidemiological Protocol for investigation of microcephaly cases in the state of Pernambuco. Pernambuco, Brazil.
- Araújo TVB, Rodrigues LC, Ximenes RAA, Miranda-Filho DB, Montarroyos UR, et al. (2017) Association between microcephaly, zika virus infection, and other risk factors in Brazil: final report of a case-control study. Lancet Infec Dis 18(3): 328-336.
- Schaub B, Vouga M, Najioullah F, Gueneret M, Monthieux A, et al. (2017) Analysis of blood from zika virus-infected fetuses: a prospective case series. Lancet Infec Dis 17(5): 520-527.
- Melo ASO, Malinger G, Ximenes R, Szejnfeld PO, Sampaio SA, et al. (2016) Zika virus intrauterine infection causes fetal brain abnormality and microcephaly: tip of the iceberg? Ultrasound Obstet Gynecol 47(1): 6-7.
- Pan-American Health Organization. Epidemiological Alert: Neurological syndrome, congenital malformations and zika virus infection: Implications for public health in the Americas.
- Neta TJC, Fernandes AS, Furtado G, Al E (2016) Actions developed at the Institute of Integrale Medicine Prof. Fernando Figueira for coping with microcephaly by zika virus. Rev Bras Saúde Matern Infant 16(Suppl 1): 17-22.
- Campo M, Feitosa IML, Ribeiro EM, Horovitz DDG, Pessoa ALS, et al. (2017) The phenotypic spectrum of congenital Zika Syndrome. Am J Med Genet 173(4): 841-857.
- Alves LV, Cruz DCS, Van der Linden AMC, Falbo AR, Mello MJG, et al. (2016) Seizures in children with Congenital Syndrome of zika virus. Rev Bras Saúde Matern Infant 16(Suppl 1): 33-37.
- Gomes ALZ, Othero MB (2016) Palliative care. Estudos avançados 30(88): 155-166.
- Forgotten and unprotected - The impact of the zika virus on girls and women in northeastern Brazil. Humans Right Watch. 2017.
- Aragao MFVV, Holanda AC, Petribu NCL, Castillo M, Van der Linden V, et al. (2017) Nonmicrocephalic infants with congenital Zika Syndrome suspected only after neuroimaging evaluation compared with those with microcephaly at birth and postnatally: How large is the zika virus “Iceberg”? Am J Neuroradiol 38(7): 1427-1434.
- França GVA, Schuler-Faccini L, Oliveira WK, Henriques CMP, Carmo EH, et al. (2016) Congenital Zika virus syndrome in Brazil: a case series of the first 1501 livebirths with complete investigation. Lancet 388(10047): 891-897.
- Chanes IR, Monsores N (2016) A bioethical and sanitary reflection on the side effects of the zika virus epidemic: an integrative review on euthanasia/orthanasia in cases of fetal anomalies. Cad Ibero-Amer Dir Sanit 5(2): 56-72.






























