Biopsychosocial Approach to Attention Deficit Hyperactivity Disorder (ADHD) An Effective Means for The Prevention of Parental Deficiencies and The Abuse of Sick or Designated Sick Children in The Family
Issack Biyong1,2*, Irène Coretta Biyong Ngo Beguel3, Michel Botbol4,5 and Addo Boafo6
1PSY-SCAN Institute: Outpatient Consultation for Child and Adolescent, Neuchâtel, Switzerland
2Institute of Psych traumatology and Mediation (IPM) Clinic for Psychological Trauma and Transcultural Psychiatry (CTPT), Switzerland
3Centre of Psych traumatology and Mediation (CPM), Ottawa, ON, Canada, Counseling and Spirituality outpatient consultation, Switzerland
4Emeritus Professor of Child and Adolescent Psychiatry, University of Western Brittany, Brest, France
5Secretary for Scientific Publications of the World Psychiatric Association (WPA) Executive Committee, Geneva, Switzerland
6Children’s Hospital of Eastern Ontario, Ottawa. Department of Psychiatry, University of Ottawa, Ontario, Canada
Submission: December 4, 2023; Published: December 20, 2023
*Corresponding author: Issack Biyong, PSY-SCAN Institute: Outpatient Consultation for Child and Adolescent, Neuchâtel, Switzerland.
How to cite this article:Nihat A, Dario F, Özgür Ö, İlkay O. Effects of Passive Dehydration on Muscular Strength. Psychol Behav Sci Int J. 2023;21(3): 556064. DOI: 10.19080/PBSIJ.2023.21.556064.
Abstract
The study focuses on understanding the role of parental psychiatric conditions in family distress and the risk of parental deficiencies in healthy children, or those with ADHD. It highlights the importance of a biopsychosocial approach to addressing the issue, which is a significant public health concern with social, psychological, psychiatric, economic, and medico-legal implications. Methodology: A comprehensive examination of the case involving David, a child with ADHD, and his family, including the mother’s and father’s psychiatric conditions, was conducted. The study considered various factors contributing to family distress and the effect on the child’s ADHD symptoms. Results: The results showed that after systemic family therapy and pharmacological treatment for the mother’s and father’s psychiatric conditions, there was a significant improvement in the ADHD scores measured by Conners’ questionnaires for both parents and teachers. This highlights the relationship between the mother’s ADHD and parenting difficulties. Conclusion: The management of childhood ADHD as a symptom of family distress requires a biopsychosocial approach to address parental deficiencies, which may be related to existing mental health disorders in the family as a system. It is crucial to conduct extensive research and adopt a multidisciplinary approach to improve ADHD management and prevention, considering its far-reaching implications.
Keywords: Biopsychosocial Approach; ADHD; Prevention; Parenting Deficiency; Abuse; Designated Sick Children; Family
Abbreviations: ADHD: Attention Deficit Hyperactivity Disorder; CTPT: Clinic for Psychological Trauma and Transcultural Psychiatr; CPM: Centre of Psych traumatology and Mediation; WPA: World Psychiatric Association; WURS: Wender Utah Rating Scale; HAS: Hamilton Anxiety Scale; Y-B-TOC: Yale-Brown Obsessive Compulsive Scale; PSI: Psy-Scan Institute; GAF: Global Assessment of Functioning; OCD: Obsessive-Compulsive Disorder; IPTP: Integrated Psychiatric Treatment Plans; BDI: Beck Depression Inventory; ADD: Attention Deficit Disorder; GAD: Generalized Anxiety Disorder; HAS: Hamilton Anxiety Scale; ADDS: Attention Deficit Disorder Scale
Introduction
ADHD is often perceived as a behavioral disorder generally observed in children given the importance of research in recent decades on this subject [1]. In the medical field and in public opinion, talking about ADHD comes down to indexing the child by their parents and by the school in general. Parents who come to the child psychiatrist with a so-called hyperactive child are becoming more and more common in mental health services. ADHD is rarely if ever perceived as a family and systemic problem, but rather as an isolated disorder and the only person concerned is the sick child or, better said, as the designated patient. Seen in this perspective, the disorder is managed on a biomedical level, and the family and school increasingly invest in the doctor and medication for a quick solution. The hyperactive child puts the parents to the test in their exercise of "parenting." In some cases of indexed hyperactive children, the school and parents may not agree, the parents panic, the child plays their role as a patient in their own way without necessarily being hyperactive, at least from the point of view of medical and educational professionals. This is the subject of a case series study with his parents and a clinical case of a 7-year-old boy whom we have named David for the sake of confidentiality and anonymity. David is perceived as hyperactive and oppositional according to the mother. The absent father adheres to the mother's complaints but failing to be too present at home due to his almost obsessive dedication to work, he can only accept without conviction what the mother tells him. This "hyperactivity and opposition of the child to his mother" at least according to the latter who seems to be at the end of her rope and even says that if this continues, she risks divorcing to involve the father more in taking care of his son through shared custody. Faced with this maternal suffering and the son who becomes more and more anxious and depressed, two major problems arise for the clinician.
How to think of ADHD without psychological, psychiatric, or educational evidence from the school where the child spends his days from Monday to Friday? How do the parents position themselves in relation to their son who becomes difficult at home according to the mother but adapted to school? Here we can perceive a second problem, that of "parenting" being tested by a family situation that takes the child hostage and risks making him responsible for the parents' divorce, which the mother brandishes as a solution for relief. The request has just been reformulated in a medical environment. But it should be noted that in the face of such a situation, parents expect a diagnosis of their child's disorder and then target pharmacological and psychological treatment for the "designated patient" that is the child. In such a situation, if a diagnosis is not made, it is not possible to talk about the treatment plan that parents often expect for reassurance. Failing to advance a diagnosis aligned with the syndromic level, therefore, a well-known disorder, a "diagnostic hypothesis" or/and a working hypothesis must be formulated on a psychodynamic level, of a family or systemic dysfunction in the broad sense. The question we can ask is how to help parents play their role in the face of a diagnosis or in the face of a working hypothesis according to their expectation or not. To answer this question, we must first know what is meant by "parenting." The neologism "parenting" is increasingly successful in biopsychosocial care and involves multiple practices called "parental guidance," "Support for parenting." The French Ministry of Social Affairs then decided in 1993 to form a reflection and research group on this term, under the direction of Didier Houzel [2]. After 6 years of reflection, this multidisciplinary and multi-institutional group, consisting of lawyers, psychologists, educators, maternal and child protection (PMI) doctors, sociologists, etc., examined the term and proposed a reading of parenthood in three dimensions: exercise, experience, and practice of parenthood.
The dimension of exercising parenthood (Dimension of Rights and Duties)
Being a parent means being invested with responsibility, parental authority as per article 371-1 of the civil code (modified in 2002): "Parental authority is a set of rights and duties aimed at the best interests of the child. It belongs to fathers and mothers until the child reaches the age of majority or becomes emancipated, to protect their safety, health, and morality, to ensure their education and allow their development while respecting their person. Parents involve the child in decisions that concern them, according to their age and degree of maturity." This dimension also includes the genealogical aspect; the parent places the child in a symbolic lineage.
The dimension of the subjective experience of parenthood (psychic and emotional dimension)
This dimension refers to the intimate experience, the imaginary and emotional experience; that is to say, how does the parent perceive their child? How do they feel in this experience as a parent or non-parent of this child here or that other one there? For M. Lamour and M. Barraco [3], "Parenthood is the set of psychic and emotional readjustments that allow adults to become parents, i.e., to meet the child's needs at three levels: the body, emotional life, and psychic life." Several authors agree to represent "parenthood" in terms of a maturities mental process. Therefore, it is a matter of being able to deal with one's own experiences and childhood suffering to become a parent to one's real child and not just the parent of that former child they were themselves, but of that other child they had according to the vicissitudes of life, whether genetic or legal. This concerns transgenerational repetitions and the possibility for everyone to separate from their own childhood history and family history. Separating does not mean creating an amnesic break, but being able to reorganize and put into perspective what has been experienced by oneself, avoiding consciously confusing it with what the child here and now brings us, regardless of our own history. So, how can each parent, with their history, separate from that former child they were and that they continue to be unconsciously, and interact with their real child? This is indeed an ongoing elaboration work for everyone in the possibility of becoming a parent.
The axis of the practice of parenthood (dimension of concrete acts of daily life)
The practice of parenthood refers to the implementation of parental care and interactions, such as domestic tasks, supervision, care, education, socialization, etc. Some parents occupy these three dimensions, but others sometimes struggle or fail in one or more of these three axes. Authors have agreed to talk about "partial parenthood" or "dysparenthood" [4]. Based on the work of the Houzel group, it is possible to retain Catherine Sellenet's [5] attempt to define parenthood, also considering more singular forms of parenthood: "Parenthood is the set of rights and duties, psychic readjustments and affects, and care and education practices, implemented for a child by a parent (by law or choice), regardless of the chosen family configuration."
The concept of "filiation
Through the concept of filiation, we can also understand the notion of "parent" by considering its three aspects.
i. Symbolic filiation, the legal parent who is recognized as the child's parent according to the law of society.
ii. Biological filiation, the biological parent.
iii. Affective filiation, a sketch of the definition of parenthood. We can believe that parenthood, as defined above, is not innate but is acquired through the experiences of parents or a parent as a child and then as a parent once they become a mother or father. To imagine "normal" or, better said, balanced parenthood requires good genetic and transgenerational educational foundations, good mental, physical, and social health, and even financial health if we consider the World Health Organization's definition of health: "Health is a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity" [6].
In the case of David, who is considered ADHD by his mother but not by the school or the child psychiatrist, we can ask if the mother needs care, support, or parental guidance. Additionally, we can wonder if the mental health of the mother, the couple, and the family is good. Does David's family environment make him "restless, anxious, oppositional, sad, and aggressive towards his 2-year-old little sister," according to his mother's statements? Seen from this angle, the biomedical model is limited for better care of this child (perceived and designated as hyperactive) and his family.
Method
We used several spaces for interviews, evaluations, and integrated psychiatric and psychotherapeutic treatment: interviews with the mother-child dyad, interviews with the designated sick child, interviews with the complaining mother, interviews with the parental couple, and interviews with the family.
Interview with the mother-child Dad
First, interviews with the mother and the designated sick child. The purpose of these interviews is to listen to the mother's request in a clinical consultation space for the child and his mother during the first interviews, a privileged space to observe the mother-child interaction and to observe the child's and mother's verbal and non-verbal language.
Interviews with the designated sick child
Second, listen to the child presented as sick or as a disturbing element but also as a suffering subject needing his space in this care process to create a therapeutic relationship with his pediatric psychiatrist. This space is used to show David that he has the right to complain, to say how he experiences his relationship as a child with his mother, his father, and his 2-year-old little sister. To make him understand the role of the pediatric psychiatrist in such an outpatient follow-up setting for a child his age who needs to be accompanied by his mother, his father, or both parents at the same time, and even by the whole family with the presence of his little sister.
Individual Interviews with the mother
Given the intensity of the suffering expressed by the mother during our interviews with her son, the anger, irritability, and anxiety she exudes in this space initially reserved for her son, we felt the mother needed interview spaces for her to vent and also for a real psychiatric evaluation of a possible psychiatric disorder such as attention deficit disorder, anxiety, depression, or an Axis 2 disorder or the presence of couple problems with her husband.
Individual Interview with the father
These interviews aimed to understand the This interview allowed us to objectify the descriptions of David's behavior according to the mother's version and to see if the father, although too absent from home, also perceived his son in the same way as his wife as a hyperactive child or not. What was his perception of his emotional relationship with his son and his little girl and the atmosphere in his couple and family according to him?
Interviews with the couple and the whole family
These interviews aimed to understand the dynamics of the couple's system versus the family in the presence of the two children, David, 6 years old, and his 2-year-old sister.
Psychometric assessments
Various questionnaires and psychometric scales were used to quantify the intensity of symptoms of the disorders considered for different diagnoses in David and his mother mainly, and partially in the father. Among these tools, we have selected: The Conners Questionnaire [7] for parents and teachers, allowing to see the quantitative perception of ADHD symptoms in children in the family and at school by teachers. The ADD-Brown Attention Deficit Questionnaire [8], the Wender Utah Rating Scale (WURS) [9] for children and adolescents, and the Utah, Brown, and Copeland ADHD Questionnaire for the mother. For depression and anxiety in the mother, we used the Beck Depression Inventory (BDI) [10] and the Hamilton Anxiety Scale (HAS) [11]. For the father, we administered the Y-B-TOC (Yale-Brown Obsessive Compulsive Scale), Mollard E, Cottraux J & Bouvard M France [12], and for both parents, the SCID-II [13] for personality disorders.
Return to our two Case Studies (The Son, the mother, and the father))
Our clinical case is a child designated as ADHD by his family in a "situation of difficulty in their role as parents and a couple in crisis". Moreover, this child's parents have undiagnosed mental health problems.
Summary of the evaluation of the child as the designated patient
1st Session
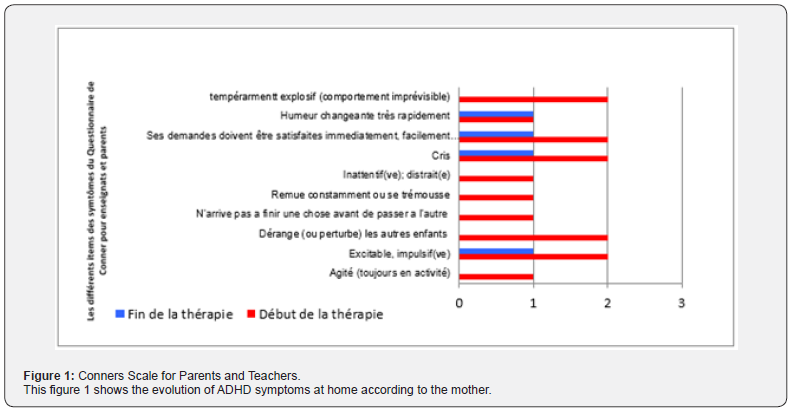
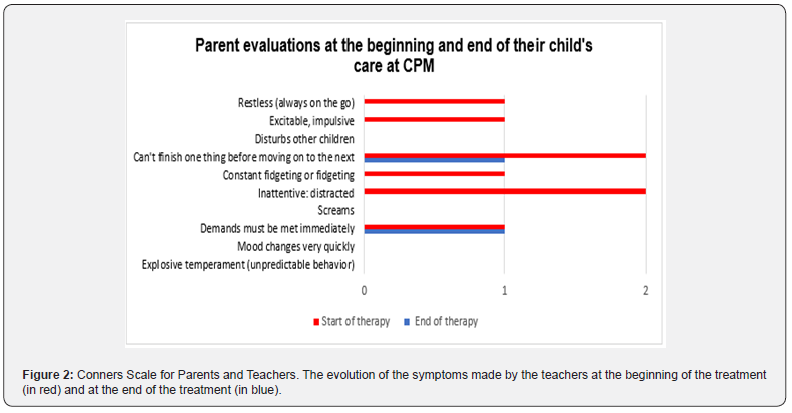
First consultation of David, 6 years old, brought by his mother for evaluation and management in child psychiatry at the Psy-Scan Institute (PSI) in Neuchâtel (Switzerland) for: lack of appetite, no interest in food, attention deficit hyperactivity disorder (ADHD) and elements of opposition to the mother. The mother also presents him as violent and mean towards his 2-year-old little sister. According to the mother, the onset of these behavioral problems dates to a year and a half ago when David was 4 and a half years old, a few months after his sister's birth. He began to show less and less interest in regular food, apart from sweets. Upon consulting the pediatrician, he told the mother to be firm. The mother's attempts to introduce him to products in stores did not change anything. The father often yells, which worries both the mother and the child, creating a vicious circle that becomes difficult to break, according to the mother. Moreover, the mother describes her son as presenting ADHD symptoms, which she reports to Conner (Figure 1). This evaluation by Conner, taken up by the teachers at school, does not confirm ADHD (Figure 2), the mother's descriptions of her son's behavior, which she describes as hyperactive. There are no reported child psychiatric or psychological antecedents in David. Regarding medical and surgical antecedents, David has a cleft palate malformation with surgery at the 3rd month, resulting in assisted feeding for 5 weeks with lukewarm food. After that, the child has never been able to adapt to hot or cold food, according to the mother. No medical history except for recurrent ear infections at the age of one. David was born full term with an episiotomy performed on the mother; the labor duration was 29 hours and 30 minutes. No respiratory distress or neonatal suffering occurred. The mother and child left the hospital together. The birth weight was within the norm. In terms of schooling, since the 1st and 2nd kindergarten years, David is sociable, not showing phobic behavior but quite combative at school. He welcomed the birth of his little sister Eva, who is currently two years old, has a lively character, and is doing well. The father is very difficult and selective when it comes to food. He eats well what he chooses. The mother maintains a good appetite.
Mental examination of david
Overall good condition, good hygiene, and well-behaved during the interviews, very alert and good contact with his mother and the child psychiatrist. He is well-oriented in all three modes and maintains good eye contact and gestures. David is in a slightly anxious and depressive mood. He sits up straight in front of what he considers false accusations from his parents, especially his mother. David thinks his parents do not want to recognize that they are the ones causing his problems, according to his statements. He blames his mother's nervousness and his father's complete absence at home and from the family. He likes and eats sweets but resists home-cooked food. He hayearappetite from 0 to 1 and a half years old, but after that, his appetite decreased, which he recognizes but does not bother him, he confided. He tends to fixate on certain tastes. He knows he doesn't have a good appetite, but he doesn't see a problem with that since he feels strong and plays well at school. He acknowledges that he does not disturb his classmates at school, that he works well in class, and respects his teachers. He accuses his parents of paying more attention to his little sister and not considering when she comes to disturb his toys in his room. He says he loves his little sister, but she provokes him, which is why he sometimes defends himself. He presents a coherent and logical thought process, no suicidal or homicidal thoughts. He shows excellent introspection, as he recognizes that he is sometimes sad, nervous, and anxious because he misses his father. He thinks his mother is not there to educate him and that it is his father's role, but unfortunately, his father is absent from home, which is very frustrating for David. He sleeps well and does not show daytime sleepiness or fatigue. After multiple interviews with the mother, the couple, and the functional analysis of symptoms, the child psychiatric, systemic, and family assessment through quantitative and qualitative psychometry, a hetero assessment was done by the parents and David's schoolteacher. Following this mental examination of David, we diagnosed the son as follows.
Multiaxial diagnosis according to dsm-5 for the son
We found in axis 1 for David, unspecified anxiety disorder and mild depression, and oppositional disorder according to the mother's descriptions, who believes that David completely challenges her maternal authority. Then, in axis 4, as a psychosocial and environmental stress factor, an anxious mother with ADHD. The mother's condition causes stress in the child, and on the other hand, the father's absence at home leads to conflict in the couple and the mother-child dead. However, from the point of view of the Global Assessment of Functioning (GAF), David seems quite resilient, with an estimated GAF of 80, facing maternal distress and the father's total absence at home and in family activities.
Summary of the mother's psychiatric assessment
This is a 32-year-old woman who looks her age. She has good personal hygiene, but her clothing and cosmetics are neglected for her age and gender. She maintains good eye contact and gestures with the psychiatrist but is overly intrusive and constantly watches her son as if he should not make the slightest move. She is overwhelmed by her two-year-old daughter, Eva (pseudonym given for anonymity purposes), who seems "more hyperactive" than David and touches everything and cannot sit still. This atmosphere of agitation and dispute with David exacerbates the situation at home, especially since their father is always absent, overwhelmed by work or fatigue when he returns home. He does not have time to go for walks by the lake with the family or play with the children, according to the mother's statements, which are confirmed by David and later by the father. She presents an anxious and depressive mood with congruent affect, sometimes with teary eyes in a surge of rebellion and manifest anger. She has no suicidal or homicidal thoughts, but she is considering divorcing her husband if nothing changes. She feels she has reached the end of what she can offer to the family and the couple. She describes herself as living like the mother of three children, with her husband being perceived as the first child. Her thought process remains logical and coherent. She describes her performance anxiety as a sommelier, which causes her to work only two days a week. Her fears of not being up to par or worries that something will happen to her husband at work paralyze her. He works even on Saturdays and sometimes Sundays. When he does not work on Sundays, he spends his time sleeping due to fatigue. The patient also describes herself as tired, with restless nights, nightmares, and sometimes insomnia. She describes attention deficit problems at work and home, which makes her even more anxious because she forgets a lot, and this slows down her performance at work and home. She has good introspection of her condition, no suicidal or psychotic thoughts or behavior. She shows a lack of anger and stress management when dealing with her children and difficulty controlling her nervousness when things do not go as she wishes. Faced with this analysis and taking a step back, we considered inviting the mother alone for a few sessions to investigate her anxiety and irritability. During these interviews with the mother, the data from the questioning, personal history, and psychometric evaluation confirmed the following diagnosis in her, as mentioned below.
12th Session (22nd Week)
This session focuses on the mother's evaluation interview with good listening and empathy, as her distress with two young and lively children and her demanding part-time job as a sommelier is apparent. The diagnosis is as follows: Multiaxial diagnosis according to DSM-5 of the mother: We found in axis 1 a generalized anxiety disorder (GAD), depression, and attention deficit hyperactivity disorder (ADHD) with a predominance of attention deficit (AD). Theaxis 4, the psychosocial and environmental stress factor is secondary to undiagnosed and untreated GAD and ADHD, causing stress in the relationship with her son David. ADHD since childhood is confirmed in the mother by the WURS psychometry. The absence of the father at home and in family activities leads to a latent conflict in the couple, without confrontation since the father adopts avoidant behavior due to his regular absence at home. The mother's Global Assessment of Functioning (GAF) is estimated at 65-70. The presence of GAD and ADHD with a predominance of AD in the mother confirmed by the quantitative and qualitative psychometric evaluation at HDS, WURS, and Brown's ADD reverses the initial reason for consultation, which identified the child as the ill person in the family according to the parents, especially according to the mother.
Biopsychosocial Treatment Plan (PTBP) For the Child and His Family
This PTBP is, in fact, an integrated psychiatric and psychotherapeutic treatment (TPPI) that considers the mother's request for her son, the son's request for his mother, the father's place in the family dynamics, and the school's perspective. The psychiatric evaluation data of the child, the mother, and the father will be considered and integrated into this PTBP.
1st Session after the complete child psychiatric evaluation
In the first session between the child psychiatrist and David, a dynamic exchange takes place during the interview, leading to an affective bridge that allows the therapist to know which games the child likes or dislikes. When asked by his child psychiatrist which game he likes, David mentions that "I don't have any other games; I don't like games I don't know." His therapist turns this denial into an affective bridge to give the child an opportunity to "discover new things." The lesson learned by David is "to learn to discover new things, to want and to be motivated." This session also addresses the concern of David's mother, who worries about his lack of motivation when it comes to certain games and food.
2nd Session, after 7 days
The 2nd session focuses on a motivational interview about the desire to discover new things. This desire and motivation found by David allows the child psychiatrist in this session to talk about and suggest the idea of visiting the cheese factory where his father works. During this session, which becomes a privileged communication space between David and his child psychiatrist, the latter slides his interlocutor into hypnotic communication without hypnosis, and the child literally sees himself visiting the cheese factory and meeting his father. He then describes during this trance visit and tells his therapist, quite drowsy: "I eat cheese. I like cheese. Cheese gives me strength to play ice hockey, and also by eating well, I can become a great athlete." David responds to a personal need and then to a request made by his mother that he does not like to eat things he does not know well, including the cheese that his father brings home from the factory where he works. The lesson learned by David is "to like certain unknown things, new things like cheese, for example, because food gives strength," and this strength can help become a great athlete according to David's own statements.
3rd Session, after 14 days
David shows opposition to assert himself by saying, "I like fish because others don't like it." His mother thinks that "David has problems with food, he stays at the table for 1 hour 15 minutes, watching others without eating. He never stops moving his feet, at home, he jumps from one thing to another, talks about everything and nothing. He has been biting his nails since the age of 3-4. He accepts criticism very poorly and tends to have tantrums. He enjoys some games, but he remains a sore loser," according to his mother's statement. At home, he refuses to eat but manages to eat after 30 to 60 minutes at the table; he talks a lot and forgets to eat. The dialogue between his father and him: he is used to saying, "Mom, tell that to dad." At school, his mother says that everything is going well because "David does drawing, writing, and games with pairs. But during meals, "he has to extend the mealtime: is it a way to prolong the pleasure of being together?" the therapist remarks. During this session, David is at school; kative at home, according to his mother: "He says everything he does at school, he is always restless and does many things at once, even at the table." Therapist (T): Why do you bite your nails?
D (David): When I'm hungry, and mom doesn't give me anything to eat.
Therapist: If we ask you not to bite your nails, what would you ask for instead?
D: I would ask for chocolate all the time.
T: Do you know what it means to be tense?
D: Yes, it means being excited, upset, etc. We note that for his age, David is very intelligent, expresses himself well, and always gives appropriate answers.
T: Are you often tense?
D: One day yes and one day no.
T: Why are you often tense?
D: Because my parents get angry with me, and I would like to get angry with them too.
David is used to complaining all the time, according to his mother: every day at school, someone hits him; tension in the evening at home; the mother is tense and starts to "yell" at him.
D: I notice that mom doesn't stop yelling at me. I'm not going to stop doing the same thing to her either.
David says it firmly. The young patient has the impression that everything is forbidden to him. David shows and expresses sibling jealousy towards his little sister: regressive fantasy, his mother often wonders. "I want to become my little sister," according to David's own statements. He would like to attract attention to be loved, to be taken care of more, like his little sister.
4th Session after 21 days
This session takes place between David and me, to help him clearly express what he feels. His mother agrees and agrees to wait in the waiting room if needed in some sessions at my request or David's request. He tells me that he sleeps well, that things are going better between his little sister and him. Now he eats well and is less demanding. He says that now he doesn't eat salad but grass, meaning spinach.
5th Session after 28 days
i. First part: David comes to the session with his mother and his little sister Eva, who is already about 2 years and 5 months old. Even during the session, David shows jealousy (verbally or not) towards his little sister; he even asks his mother to give him a little brother.
ii. Second part of the session: David draws a soccer team. I introduced this exercise for David to calm down because he likes soccer, and in the meantime, I asked his mother to wait in the waiting room. David tells me bluntly that I am his doctor and not his little sister's doctor, "because she gets everything she wants at home, and mom and dad give her everything she asks for."
6th Session after 42 days
After two weeks, the observation is unanimous; everything is going well for David both at school and at home. "David is doing better, gets along with his sister, and eats better," according to his mother's own statements.
7th Session after 56 days
David is doing well. He says he no longer bites his nails. When he grows up, he would like to work in mechanics like his dad (identification) with manufactured and controlled machines. He spends this session with me drawing the factory and the machines, inside he shows a head and says that it is his father who is working inside. He confides in me, saying, "Doctor, I miss my father, I don't play with him anymore because he is always at work, sometimes he comes back when I am asleep. Even when he finds me awake, he is too tired to answer my questions or play with me."
8th Session after 70 days
After two weeks, I met the mother in this session to discuss her request. I summarize the mother's request in the presence of the child. Definition of the therapeutic framework and the expected objective. Guidelines: Absolute rules (framework and values set and explained by the parents, necessary for a non-permissive education that helps the child know the limits and build their values through their family values). Relative Rules (Flexibility in the Relationship): David does not think he disobeys his mother; he has fun with her. He obeys his father because he is afraid of him. During this session, although the mother reported a good evolution of David, he remains faithful to the "family culture" which considers the mother a source of affection, tenderness, and not authority on a disciplinary level. David does not hold back in his statements; he is ready to obey his father, but unfortunately, the latter is absent from family life due to his almost obsessive and perfectionist passion for the machines at the factory where he works. Everything’s there on Sundays to reassure himself that everything will be fine at the beginning of the next working week, that is, Monday.
T: David, do you love your mom?
D: Sometimes yes, sometimes no. Anyway, I will never obey her; I will always have fun with her. He explains that he does not obey his mother because he does not like doing homework.
"I wish it were my father who asked me to do my homework and not my mother; it's not my mother's job," he adds in his mother's presence. His mother's job is cooking, laundry, etc. He says he obeys the teachers but not his mom at home, as she is not the father.
T: How is your relationship with your father?
D: My father is like he is not my father; he just works. Now, it's starting to bother me that he's absent. I would like my father to be summoned to the next session here, Doctor.
9th Session after 84 days
This family session is marked by the father's presence. He has promised to try to reduce his working hours and spend time with his family. He acknowledged that he gave more to his work than to his family and promised to remedy the situation. According to him, his child is not hyperactive, and he would not like psychotropic drugs to be prescribed to his young child, barely six years old. Positive reinforcement is given in this session to support the father in taking his place, which allows him to restore order and discipline, as David, his son, declared openly here that he could not obey his mother but you, his father. David believes that it is the father who, as the head of the family, is responsible for ensuring the discipline of the children. His mother, for David, should remain in her affectionate and nurturing role. She is the “mother" of the family and not a "schoolteacher" according to David's statements.
10th Session after 98 days
This tenth session with David (the son), his father, mother, and little sister of about 2 years and 5-6 months, and the child psychiatrist. This session took place after a two-week interval (14 days). The purpose of the session was to review the therapeutic framework and rules that will enable us to achieve the objectives of this biopsychosocial care. The main objectives, according to the mother's consultation reason, are aimed at otherwise, there is a risk of eating disorder behavior in adulthood (very good session). This session takes place at the end of November, a very busy time for both the child psychiatrist and the family due to the approach of the holiday season. David expresses his desire to have a good Christmas, unlike the others, with his father who should take vacations, and his father promises him that.
11th Session after 126 days
This session takes place in January; promises have been kept, and the established educational framework has been well respected by both David (the son) and his parents. He is becoming calmer. In this session, for the first time, he consults with his father, who acknowledges a significant improvement in the behavioral relationship between the mother and their son. David also points out in this same father-son session that his parents have changed positively. His father is more present at home, according to David's statements. His father confirms this but without much comment, as he is very reserved and does not appreciate confiding in psychiatrists, as for him, it is a sign of weakness.
12th Session after 147 days
We are in the first week of February, and we find that David (the son) is doing well, but at school, his inattention begins to suggest ADHD. Consider assessing ADHD with your teacher. We have the impression of having several Davids. His ADHD is variable; sometimes, he is calm and focused, follows instructions well, and is very respectful. But there are days or weeks when his behavior suggests ADHD, according to Conner's questionnaire for parents and teachers. This same behavior of several types of David depending on the days or weeks is also reported by the parents. A case of variable ADHD in terms of ecology and chronology suggests a reactive behavioral disorder in a child of this age, which leads us to investigate genetic, psycho-affective, and environmental factors that would explain David's chameleon behavior. The search for ADHD in the family begins with the mother, always present in consultation and always complaining and accusatory. The father's withdrawal at home, with subtle avoidance of being a couple or family, suggests that there is discomfort somewhere in the couple's relationship, discomfort borne more by David, who would express it through his "chameleon behavior" but not taken seriously, as everything is focused on the designated patient, who is the eldest son in this family of two children. Faced with this dilemma, we embark on the assessment of the mother, who is more prone to complain about David and seems less patient. I suggest that in the next session, it is the mother alone who will come without David or the father.
13th Session (23rd week)
In this individual interview, we find that David is doing very well at home and at school. David himself acknowledges that everything is fine. "Before, we didn't get along. They yelled at me; now, it's going very well," he says with a big sigh of relief. "Dad is also more present at home, and I like being with him and also with mom," he adds.
The revised biopsychosocial (family and systemic) treatment plan considering psychiatric evaluations and diagnoses
Pharmacological treatment for GAD, depression, and ADHD in the mother was based on SSRIs (Escitalopram 20mg in the morning) and a psychostimulant (Methylphenidate) at a dose of 20mg SR in the morning. Treatment for the mother-son dad aimed at psychoeducation and guidance for the mother's parenting skills. Explanation of negative emotional interferences and cognitive distortions secondary to Axis 1 disorders in the mother.
Treatment for the couple
Psychoeducation on the wife's Axis 1 disorders and the husband's lack of support in the education and guidance of the two children.
Family treatment
Family sessions aimed at psychoeducation and psychodynamics to identify the real causes of the family's discomfort, discomfort carried by the designated patient, David, which leads to induced behavioral problems in him. Lack of emotional and educational presence from the father, failing emotional support from the mother who invests more in her 2-year-old 6-month-old daughter, exacerbating David's unease.
Systemic treatment
Family, school, and parents to stabilize the mother-son relationship, father-son relationship, and the couple's relationship. Supportive interview in the presence of David's teacher, David's family, and the child psychiatrist. David's agitation has nothing to do with ADHD but is a symptom that expresses the general climate within the family and often reports this unease to the school.
The father was referred to the family doctor because the idea of being followed by a psychiatrist annoys him and for fear of societal stigmatization (by his employer) and denial on his part. We suggested to his family doctor to treat his obsessive-compulsive disorder (OCD) that we strongly suspect and propose as pharmacological treatment with his family doctor, an SSRI such as Sertraline and that he be followed by a psychologist if medication alone does not resolve his OCD. Following the individual interview, he had in psychiatry and the anamnestic data on his obsessive perfectionism at the factory to the point of forgetting to enjoy weekends with his family, we diagnosed Axis 1 OCD. A trial pharmacological treatment for OCD initiated by his family doctor under psychiatric Concilium made a difference. His wife reported that he had completely changed, was less irritable, less worried about his work, and more present on Saturdays and Sundays at home. He participates more in the family's recreational activities. The restitution and synthesis sessions with the school network (2 sessions), the mother-son dyad sessions 2 times, the couple sessions 3 times, focused on communication, parental guidance, and psychoeducation on the nature of the wife's mental condition. The family sessions 2 times and 3 individual sessions with the mother and 2 more individual sessions with the father focused on support and psychoeducation of his behavior and the impact of his absence on the family and couple balance and the father-son and mother-son relationships. He understood that his behavior had the appearance of obsessive-compulsive disorder (OCD) following our two interviews and the administration of the Yale-Brown OCD scale, Mollard, E, Cottraux J, & Bouvard M (France, 1989) and in its original English version by Goodman, W., Price, H., Rasmussen S et al. (1989.) Individual sessions with David's mother focused on the importance of psychopharmacology, psychometric evaluations, psychoeducational support, parental guidance, and cognitive-behavioral therapy for her predominantly inattentive ADHD. This biopsychosocial treatment plan was carried out as mentioned above in 14 sessions for the child and his family during the acute phase and the restoration of balance in the mother-son relationship, and 6 individual follow-up sessions for the mother's inattentive ADHD evolution and her rehabilitation and reintegration into work with a gradual increase in the employment rate from 40% to 60% as a sommelier in a restaurant. The improvement in the couple's relationship and the rehabilitation of the mother's and father's parenting status allowed the parents and children to regain the family and emotional framework they were missing.
Results
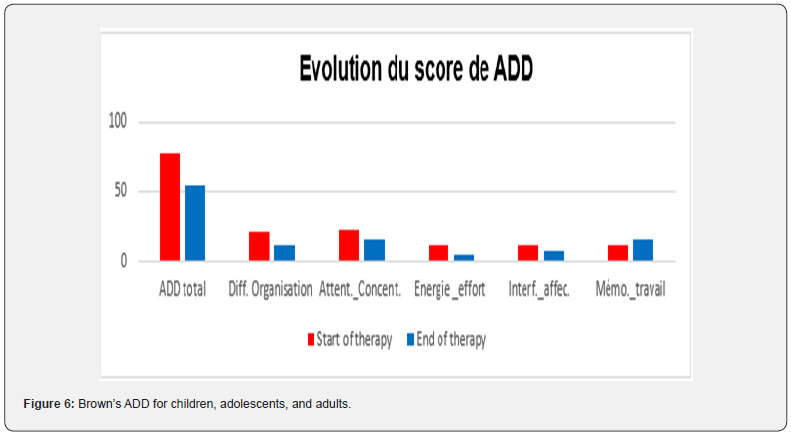
The results mentioned below come from various quantitative and qualitative psychometric evaluations performed on David (parents and teachers) and the mother by the child psychiatrist, before, during, and at the end of the intervention. This Figure 1 shows the evolution of ADHD symptoms at home according to the mother. Figure 2 shows the evolution of the symptoms made by the teachers at the beginning of the treatment (in red) and at the end of the treatment (in blue). Figure 3 shows parent and teacher perception of the severity of ADHD) presented by the child. The perception of severity by is in blue by parents and in red by teachers. Figure 4 shows the progression of the mother's GAD and DM symptoms before and after pharmacological, family, and systemic management. Figure 5 Interpretation: Easy to pass with a duration of 15 minutes allows to see the decree of suffering and especially of introspection in the patient for her disorder in our present case. Brown's ADD total = Intensity of Attention Deficit in the patient, which here is 55 points. Figure 6 shows the progression of ADHD symptoms with ADD predominance in the mother before and after biopsychosocial (pharmacological, family, and systemic) management. Series 1 (blue) describes the vitiation of ADD symptoms listed by the Brown Flow Scale at the end of the treatment. Allowing for a retrospective assessment of hyperactivity in childhood in adults suspected of having ADHD.
Discussion
Discussion of the Results
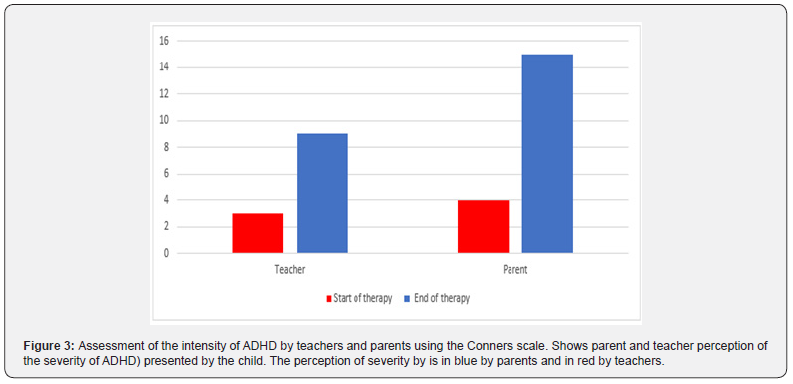
The results were obtained through quantitative psychometrics using scales commonly used in the evaluation of attention deficit hyperactivity disorder (ADHD). In this case, we are faced with the distress of a mother and her child. The mother brings her son to a child psychiatry consultation because she suspects that her child suffers from hyperactivity and attention deficit. However, during the various mother-child and family assessment interviews, it is noticed that the child is doing well and that it is rather the mother who has an attention deficit disorder (ADD) and generalized anxiety disorder (GAD), and the absent father who creates this situation. We can see the evolution of the mother under integrated psychiatric and psychotherapeutic treatment (IPPT) and of the father and the child under family and systemic therapy in relation to the teaching team of his school. Monitoring David's follow-up at school and at home was done through the Conner's questionnaire filled out by the teacher and parents about the child at home and at school. In the evaluation of ADHD at home according to the mother (Figure 1), we see that the mother evaluates her son at the beginning of therapy as having many ADHD symptoms (screaming, explosive temperament, excitable, impulsive) whereas at the end of family and systematic therapy, we see a significant change in her evaluation. There is a decrease in all the items of the Corners questionnaire symptoms. By looking at the child's evaluation by the teachers (Figure 2), we can suspect that the mother has evaluated her son severely. We see that the teachers at the beginning of treatment report fewer symptoms compared to the mother's evaluation. At the end of therapy, in the teachers' evaluation, we see a decrease in the intensity of all the symptoms presented in the Conner's questionnaire. The symptoms are almost non-existent at the end of therapy. Referring to Figure 1 and Figure 2, we notice a difference in the intensity of David's (the child's) symptoms perceived by parents and the teacher. Figure 3 clearly shows the perception by parents and teachers of the severity of the disorder (ADHD) presented by the child. We can see from this graph that the symptoms according to the parents' perception are twice as intense as those of the teachers.
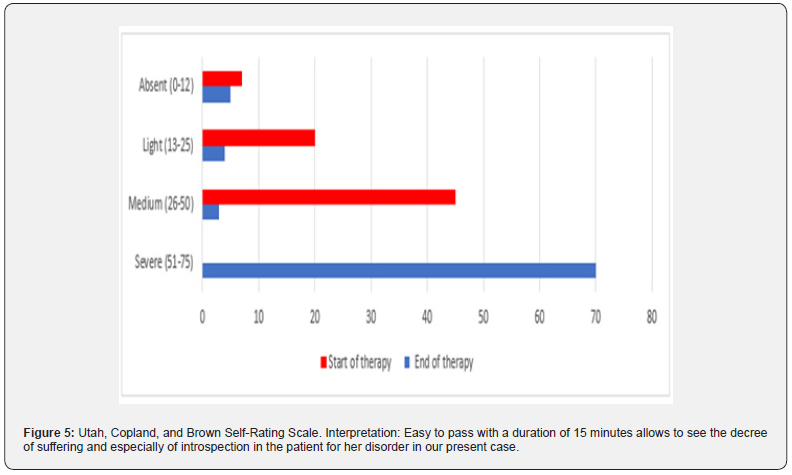
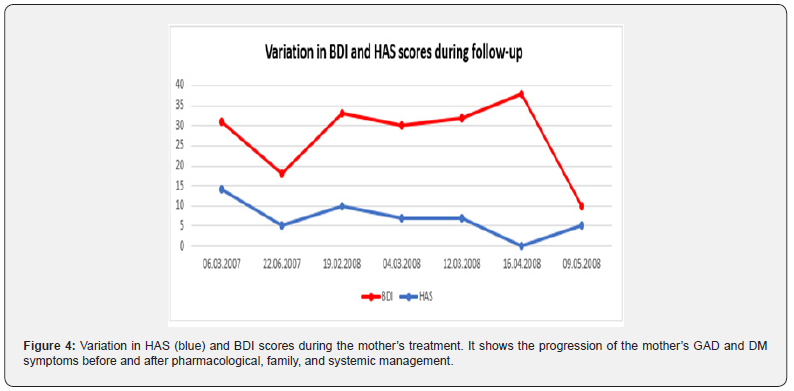
When we confront the mother's subjective complaints about her mental health, we see that Figure 4 confirms the presence of generalized anxiety disorder (GAD) at high intensity on the "Hamilton Anxiety Scale (HAS)" at the beginning of this treatment; the HAS had a score of 31 points. Throughout the pharmacological, family, and systemic treatment, the HAS confirms her anxiety symptoms and their significant decrease, i.e., less than 10 points during and at the end of the mother's therapy. We also see a decrease in her depressive symptoms according to her "Beck Depression Inventory (BDI)" score of 5 points. In Figure 5, we note that after the mother's treatment, there is a decrease in her ADD symptoms with Brown's attention deficit disorder question, ("Brown Attention Deficit Disorder Scale (ADDS)"). This decrease in symptoms in the mother correlates with the decrease in symptoms perceived by her in her child. This decrease in the clinical picture in David is confirmed by the same mother, the father, and the school as well. Pharmacological treatment of GAD and ADD with a good evaluation of the mother changes David's behavior, confirmed in mother-son interviews, the whole family, and by observations of the teachers at school. "David remains calm and attentive and works very well at school," according to the confirmation of the schoolteachers. In total, Figures 1,2, and 3 illustrated below show a significant improvement in David (the son). This is confirmed by the evolution of scores obtained from the Conners Questionnaire for teachers and parents at home and school, before and after family and systemic therapy and pharmacological treatment for the mother's psychiatric condition.
Discussion in Relation to the Literature Review
Despite the scarcity of studies on adult ADHD compared to childhood ADHD, it should be noted that recent research on adult ADHD confirms that the presence of ADHD in adults, especially in women, is more often ADD [14] than mixed, and that there is always the presence of psychiatric comorbidities such as anxiety and depression [15], as seen in David's mother. The diagnosis should always confirm a history of childhood ADHD [1] and problems in academic and professional performance [16], as in the case of our young patient's mother. If studies on adult ADHD are rare in general and particularly on ADHD and parenting issues [17], it should be noted that in this case, by establishing a connection between parenting problems and the mother's ADHD, we were able to identify the mother's suffering. It is rather the studies on parenting and family issues associated with childhood ADHD that are cited [18]. This is surprising because ADHD is well known to be a biological psychiatry issue, thus known as hereditary psychiatric or child psychiatric disorders closely or distantly related to the family genogram [19]. The scarcity of studies on parenting problems and the mother's or father's ADHD ill-prepares medical, paramedical, social, and educational professionals to deal with the difficulties parents suffering from this disorder face in meeting the demands of managing the parenting issues. Parents with ADHD or who have one or more children with ADHD feel guilty and disqualified in their parenting role [20]. For some, resorting to placement in medical-educational institutions is the solution, and for the less fortunate, it is resorting to substance abuse by parents and/or children [21], delinquency [22], dropping out of school or work [23] for both children and parents [24]. This is why genuine evidence-based biopsychosocial care programs are lacking in our medical, educational, and mental health institutions, as well as in child psychiatry programs. David's mother presents difficulties in the five clusters of Brown's ADHD scale, Figure 5, namely:
i. Organization of energy at work
ii. Supporting attention in concentration
iii. Supporting energy and effort
iv. Managing emotional interference
v. Using working memory and recalling memories.
This suffering is further exacerbated by depression and generalized anxiety as psychiatric comorbidities, which explains the distress of David's mother, her lack of judgment regarding her son's and daughter's normal behaviors, and her inability to work more than 30% as a sommelier while taking care of her household chores and her children.
Conclusion
According to our experience and research [25], only biomedical, family, and systemic biopsychosocial support can give hope to these children and their parents in psychosocial distress. Research in multidisciplinary teams with larger samples of children, parents, and families suffering from ADHD involved in therapeutic program evaluation studies will give us a better indication for best practices with integrated psychiatric treatment plans (IPTP) for this population, which is estimated at 5 to 8% in some studies [26]. This is a real public health problem with social, psychological, psychiatric, economic, and legal consequences. For authors like Hodgins et al. [27], more than 50% of the prison population suffers from psychiatric problems. Among these problems, ADHD (attention deficit hyperactivity disorder) is often estimated to be around 25.5% of the prison population [28]. A study published in the Journal of Abnormal Psychology examined the relationship between ADHD and delinquency in adolescents. The authors concluded that ADHD was a significant risk factor for delinquency in adolescents [29]. In conclusion, addressing childhood ADHD as a symptom of family distress requires a biopsychosocial approach to restore certain parental deficiencies. These parental deficiencies may be secondary to disorders related to affective relationships within the family, the couple, or to existing mental health disorders, known or undiagnosed and untreated, in the parents or siblings. It is essential to conduct thorough research and adopt a multidisciplinary approach to improve the management and prevention of ADHD. This is a public health issue with social, psychological, psychiatric, economic, and medico-legal implications.
References
- American Psychiatric Association (2013) Diagnostic and Statistical Manual of Mental Disorders (5th edn.). Arlington, VA: American Psychiatric Publishing.
- Houzel D (1999) Les enjeux de la parentalité. Toulouse: Éditions érès.
- Lamour M, Barraco M (1998) Souffrances autour du berceau, Gaëtan Morin.
- Clément R (1993) Parents en souffrance, Paris, Stock.
- Sellenet C (2007) La parentalité, un concept en mouvement. Spirale 40: 13-24.
- Organisation mondiale de la Santé (1946) Constitution de l'Organisation mondiale de la Santé. Genève, Suisse: OMS.
- Conners CK (1997) Conners' Rating Scales-Revised: User's Manual. North Tonawanda, NY: Multi-Health Systems Inc.
- Brown TE (1996) Brown Attention-Deficit Disorder Scales for Children and Adolescents. San Antonio, TX: The Psychological Corporation.
- Wender PH, Wolf LE, Wasserstein J (2001) Adults with ADHD. An overview. Ann N Y Acad 931: 1-16.
- Beck AT, Ward CH, Mendelson M, Mock, J, Erbaugh J (1961) An inventory for measuring depression. Arch Gen Psychiatry 4(6): 561-571.
- Hamilton M (1959) The assessment of anxiety states by rating. Br J Med Psychol 32(1): 50-55.
- Goodman W, Price H, Rasmussen S, Mazure C, Fleischmann RL, et al. (1989) The Yale-Brown Obsessive-Compulsive Scale (Y-BOCS). Part I. Development use and reliability. Arch Gen Psychiatry 46(11): 1006-1011.
- First MB, Gibbon M, Spitzer RL, Williams JBW, Benjamin LS (1997) Structured Clinical Interview for DSM-IV Axis II Personality Disorders (SCID-II). Washington, DC: American Psychiatric Press, Inc.
- Biederman J, Petty CR, Evans M, Small J, Faraone SV (2010) How persistent is ADHD? A controlled 10-year follow-up study of boys with ADHD. Psychiatry Res 177(3): 299-304.
- Ginsberg Y, Quintero J, Anand E, Casillas M, Upadhyaya HP (2014) Underdiagnosis of attention-deficit/hyperactivity disorder in adult patients: a review of the literature. The Primary Care Companion for CNS Disorders 16(3): PCC.13r01600.
- Barkley RA (2006) Attention-deficit hyperactivity disorder: A handbook for diagnosis and treatment (3rd edn.). Guilford Press.
- Chronis-Tuscano A, Clarke TL, O'Brien KA, Raggi VL, Diaz Y, et al. (2013). Development and preliminary evaluation of an integrated treatment targeting parenting and depressive symptoms in mothers of children with attention-deficit/hyperactivity disorder. J Consult Clin Psychol 81(5): 918-925.
- Rostain AL, Ramsay JR (2006) A combined treatment approach for adults with ADHD--results of an open study of 43 patients. J Atten Disorder 10(2): 150-159.
- Franke B, Michelini G, Asherson P, Banaschewski T, Bilbow A, et al. (2018) Live fast, die young? A review on the developmental trajectories of ADHD across the lifespan. Eur Neuropsychopharmacol 28(10): 1059-1088.
- Babinski DE, Waxmonsky, JG, Pelham WE, Waschbusch DA (2019) The impact of parental attention-deficit/hyperactivity disorder symptoms on parent and child outcomes: Conceptual issues and a review of the evidence base. Clin Psychol Rev 72: 126-142.
- Bussing R, Koro-Ljungberg M, Gary F, Mason D, Garvan C (2005) Exploring help-seeking for ADHD symptoms: A mixed-methods approach. Harv RevPsychiatry13(2): 85-101.
- Sibley MH, Pelham WE, Molina BSG, Gnagy EM, Waxmonsky JG (2012) When diagnosing ADHD in young adults emphasize informant reports, DSM items, and impairment. J Consult Clin Psychol 80(6): 1052-1061.
- Chang Z, Lichtenstein P, D'Onofrio BM, Sjölander A, Larsson H (2014) Maternal age at childbirth and risk for ADHD in offspring: A population-based cohort study. Int J Epidemiol 43(6): 1815-1824.
- Bussing R, Koro-Ljungberg M, Gary F, Mason D, Garvan C (2005) Exploring help-seeking for ADHD symptoms: A mixed-methods approach. Harv Rev Psychiatry 13(2): 85-101.
- Cortese S, Holtmann M, Banaschewski T, Buitelaar J, David C, et al. (2013) Practitioner Review: Current best practice in the management of adverse events during treatment with ADHD medications in children and adolescents. J Child Psychol Psychiatry 54(3): 227-246.
- Polanczyk G, De Lima MS, Horta BL, Biederman J, Rohde LA (2007) The worldwide prevalence of ADHD: A systematic review and meta regression analysis. Am J Psychiatry 164(6): 942-948.
- Hodgins S, Côté G, Toupin J (2006) Major mental disorders and crime: An updated review. In: Hodgins S, Müller-Isberner R, eds. Violence, Crime and Mentally Disordered Offenders: Concepts and Methods for Effective Treatment and Prevention. John Wiley & Sons p. 29-50.
- Young S, Moss D, Sedgwick O, Fridman M, Hodgkins P (2015) A meta-analysis of the prevalence of attention deficit hyperactivity disorder in incarcerated populations. Psychol Med 45(2): 247-258.
- Loeber R, Burke JD, Lahey BB, Winters A, Zera M (2000) Oppositional defiant and conduct disorder: A review of the past 10 years, part I. J Am Acad Child Adolesc Psychiatry 39(12): 1468-1484.






























