Clients of an HIV-Service NPO: Features of Self-Preservation Behavior
Nazarova Inna Borisovna1* and Nesterov Roman Sergeevich2
1Main Researcher, Institute of Socio Economic Studies of Population of the Federal Center of Theoretical and Applied Sociology of the Russian Academy of Sciences, Moscow, Russian Federation, Russia
2Department of sociology, Peoples’ Friendship University of Russia, Russia
Submission: December 20, 2022; Published: August 16, 2023
*Corresponding author: Nazarova Inna Borisovna, Main Researcher, Institute of Socio Economic Studies of Population of the Federal Center of Theoretical and Applied Sociology of the Russian Academy of Sciences, Moscow, Russian Federation, Russia
How to cite this article: Nazarova Inna B, Nesterov Roman S. Clients of an HIV-Service NPO: Features of Self-Preservation Behavior Psychol Behav Sci Int J. 2023; 21(1): 556051. DOI: 10.19080/PBSIJ.2023.21.556051.
Abstract
This study about men who have sex with men, clients of an HIV service NGO, who are a vulnerable group in terms of contracting and spreading HIV infection. The study was conducted in 2021 on the territory of Moscow and the Moscow Region. 3455 men were interviewed, Russians (63.7%) and citizens of other countries (36.3%). Most representatives of the study group (79.6%) are aware of their health-destroying behavior and are afraid of contracting HIV infection. Every tenth person is infected with HIV (12.3%), 7.5% have or have had syphilis, 2.2% hepatitis C, and 1.1% hepatitis B.
The behavior of the respondents is characterized as: one in ten is involved in prostitution (10.4%) or used the services of people involved in prostitution (14.3%), one in three (30.7%) had sex with HIV-infected people whose the status is confirmed, and every tenth had sex with a person whose HIV status the respondent was not sure of (11.3%). More than half of the study participants (54.7%) do not use protection during sex. Almost all additionally indicated that they had risky sexual contacts: with men (98.4%), and/or with women (14.9%), and/or with transgender people (6.6%). 19.4% use drugs, of which 2.8% inject and 18.7% non-inject, 2.1% inject and non-inject. 17.8% use drugs before and/or during sex.
Self-preserving behavior with general health-destroying behavior is most clearly manifested in checking one’s health status for the presence of syphilis (97.3% were tested before contacting an HIV service NGO). 79.6% of respondents were tested for HIV infection. 35.4% are regularly tested for socially significant infections / are regular clients of the HIV service NGO.
Keywords: HIV; Men who have sex with men; Self-preservation health
Introduction
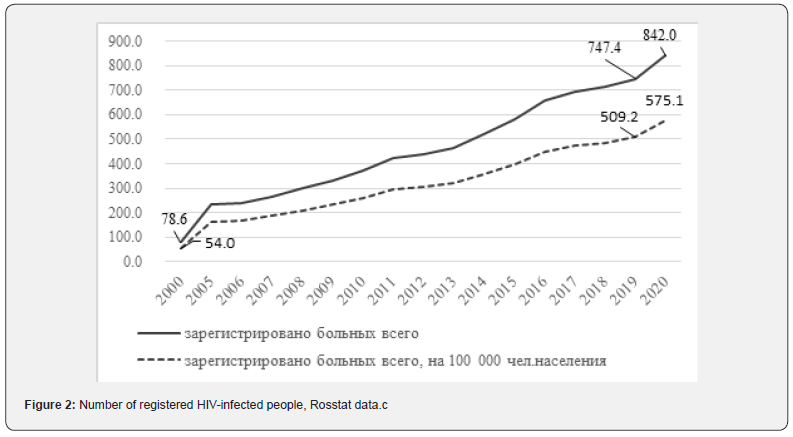
HIV infection is a complex chronic disease, and the number of new cases remains quite large, including the total number of Russians living with HIV, both among men and women, continues to increase [1]. According to official statistics, the number of registered patients diagnosed for the first time in their lives with a disease caused by the human immunodeficiency virus (HIV) in 2020 decreased and amounted to 60.1 thousand people (Figure 1). However, the number of all registered HIV-infected people is increasing annually and at the end of 2020 it amounted to 842.0 thousand people (Figure 2).
According to many domestic and foreign authors, the real incidence is many times higher than the recorded official statistics, since not all patients, especially socially maladapted, including HIV-infected, seek medical help. In addition, there are many who prefer the services of private clinics, where the incidence is not always recorded [2]. The largest number of those who live with HIV infection and diagnosis are people aged 20-40 years (both men and women) [1]. The portrait of HIV carriers has changed significantly over the past 25 years, as have the routes of transmission. Until 1997, the main route of transmission was homosexual contact, since 1997 - parenteral contact with drug use. And today there are two main ways of transmission of infection - parenteral and heterosexual contacts.
There is a feminization of HIV infection: among new cases of HIV infection in the last 5 years, the proportion of women has been increasing and by the end of 2020 in the Russian Federation, among those infected with HIV, women and girls accounted for 37.4% (531,326) of all registered cases of HIV infection and 28.8% of all deceased patients [1]. It is also difficult to reach some high-risk social groups that practice dangerous behavior both for their health and others. According to experts, representatives of vulnerable groups of the population are either ignored by official health care, or do not report their belonging to the group [3,4]. This paper will investigate the self-preservation behavior of one of the risk groups for HIV infection, men who have sex with men (MSM), regardless of their sexual orientation.
1The parenteral route is the route of transmission of HIV with material containing the virus, for example, with blood, using common injection equipment.

Empirical Basis
The study uses a database containing information on men who have sex with men who are clients of an HIV service NGO. In 2021, 3455 men were interviewed who had sex with men in the last twelve months or those who consider themselves homosexual. Russians (2201 people - 63.7%) and citizens of other countries (1254 - 36.3%). The study was conducted in Moscow and the Moscow Region by the Charitable Foundation for Support of Social Initiatives and Public Health (the Foundation) as part of preventive work on HIV infection, viral hepatitis B and C, tuberculosis and sexually transmitted infections (syphilis, gonorrhea, chlamydia, etc.).
Justification of the Choice of the Study Group
Despite the fact that homosexual contacts are not the main route of HIV transmission today, nevertheless, men who have sex with men and women, considering themselves heterosexual, are usually classified as a vulnerable group of the population, since they have a higher risk of contracting HIV and other infections, mainly sexually transmitted infections, than among the general population [5-7]. In addition, MSM, having intergroup sexual communication, puts at risk the health of women with whom they have sexual contact and the children who may be born as a result of these contacts. The Foundation works with representatives of high-risk groups (respondents, clients, MSM), trying to reach people who, for one reason or another, do not know their HIV status, do not try to establish it, or know, but do not seek qualified medical help (possibly continuing to aggravate their health condition and harm the health of partners).
Methodological Basis
The behavior of men who have regular sex with men or who have similar experiences will be considered from the point of view of self-preservation behavior. As a self-preservation behavior, we mean behavior with the aim of preventing illness during the period of well-being and during the period of illness in order to cure or not aggravate the situation. We also proceed from the fact that the ideal self-preservation model of behavior is to maintain a healthy lifestyle, choose safe living conditions, safe working conditions, prevent diseases and timely access to a specialist and treatment in case of illness [7]. In general, self-preservation behavior is a system of actions and attitudes aimed at preserving health, at setting the extension of life [8]. At the heart of self-preservation behavior is the individual’s need for self-preservation, formed by economic, social and psychological motives [9].
Individual choice of behavior is formed under the influence of values, emotions and knowledge, while there is no a priori premise that the individual always acts rationally or in search of pleasure [10]. Self-preservation is not always the preservation of health. In some cases, a person risks his health for the sake of preserving life, the opportunity to engage in certain work activities, material wellbeing or other values [7]. As a result, various types of behaviors are formed that can lead to the destruction of health. In particular, there is a link between the high risk of HIV infection with risky sexual behavior, drug use [11]. On the other hand, similar social circumstances lead to the spread of the same diseases [12,13].
Literature Review
Based on statistics and expert data, there are risk groups, belonging to which leads to loss of health. Such groups primarily include people who use drugs (PUD), have multiple sexual contacts, homosexual contacts (including transgender people - TGL) and neglect of protective equipment, including people engaged in prostitution, persons in prisons, youth, migrants (foreign citizens). Young people with no life experience who are just starting to have sex cannot fully appreciate their vulnerability. It has been revealed that various forms of deviant behavior and sexually dangerous behavior very often accompany each other: adolescents who practice one type of problem behavior are likely to have others. The relationship between the use of psychoactive substances and sexual behavior was revealed [14]. On the other hand, medical experts note the combination of not only risks in behavior, but also in the incidence of social diseases [15].
People in difficult life situations (homeless, sheltered) are at high risk of substance abuse and unsafe sexual behavior [16]. Young people in general tend to have several sexual partners (simultaneously or consecutively) [14]. For example, even in a relatively prosperous student environment, in a short period of sexual life, young men managed to change from 3 to 12 partners (an average of 6 partners), girls - 2-3 partners [17]. The less young people know about AIDS and the more confident they are, the less often they tend to protect themselves during sex [18]. Drug use can exacerbate other behavioral risks. A number of drugs are consumed in order to increase sexual activity. And, in particular, injecting drug users play a special role in the spread of HIV infection [19].
A study of networks of groups at risk of HIV infection (injecting drug users and prostitutes) showed that STIs are a risk factor for HIV infection, increasing its risk by 1.5-2.0 times (the effect is cumulative). In addition, at risk there is an intersection of sexual networks through which STI pathogens spread, which leads to the emergence of a significant number of cases of infection with various pathogens [3]. People who engage in risky sex are either not aware of the possible risks or are prone to self-destruction, for example, MSM who have an example (visual image) of someone in the later stages of AIDS are more likely to reduce the number of their sexual partners [20].
2A queer person is a person whose sexuality and/or gender identity differs from that of the social majority.
The behavior of HIV-infected people in relation to health is characterized by the fact that they are characterized by denial, in which negative information is not allowed to consciousness, as a result of which they cease to perceive recommendations from medical specialists, including in relation to a healthy lifestyle [21]. HIV-infected people do not come to the solution of emerging problems, but try to get positive emotions in ways already known to them, including using alcohol and drugs. At the same time, men more easily than women find false reasons to justify their behavior [22].
The Results of the Study
Socio-Demographic Characteristics of the Study Group
The Foundation’s clients are citizens with a high risk of HIV infection or already HIV-infected, including MSM, who make up a significant share of the total pool of clients who receive consultations from the Foundation’s employees or are tested by the Fund (2019 – 52.5%, 2020 – 73.2%, 2021 – 63.2%). The complexity of the attainability of the group indicated by us is confirmed by the fact that the Foundation’s employees work with a large number of clients, inviting them to the Foundation for testing, but only one in five of those invited by the Foundation’s employees (21.4%) reaches testing in the Foundation.
The age of the respondents ranged from 18 to 93 years, the majority were young people 20 to 30 years old (60% of the total). People 50 years and older accounted for only 1%. All clients identified their gender according to their gender – men. The majority of study participants identify themselves as homosexuals (78.0%), less often bisexuals (16.9%), a small number consider themselves heterosexuals (3.0%) and queer ( 2.1%). The majority of respondents are Russians (2201 people - 63.7%). Foreign citizens make up a third of all respondents (36.3% - 1254 people), most of whom (97.1%) named work (labor migration) as the reason for their stay in Russia. 76.6% reported temporary or permanent registration in Moscow or the Moscow region. Most often, the Foundation deals with people who have been staying in Russia for three years: 44.9% since 2019, 23.8% since 2020, 12.6% since 2018, and 12.2% for less than a year. The rest (6.5%) are between five and fifteen years old.
Customers’ Readiness for Health Status Checks
One of the significant characteristics of the group is its inaccessibility, therefore, employees are attracted to work in the Fund, who are able, firstly, to identify the client, and secondly, to arrange him to communicate and convince him to be tested. Representatives of the social groups with which the Fund has to work, including HIV-infected people and former or current drug users, are doing a good job in this work. Employees come into contact with potential customers on relevant thematic sites (for example, for drug users), inform representatives of the group in places of recreation and localization, and offer them free information about their health.
During 2021, the Foundation’s employees tried to communicate with 16,146 potential clients of the Foundation. In the end, only 30.2% sought advice and came for testing or conducted a self-test (testing at home, without consultation) and 21.4% (our respondents) came to the Foundation’s office. Almost half (48.4%) refused to visit the Fund for unknown reasons. A visit to the Foundation and a willingness to be tested, to find out the status of one’s health can be considered one of the manifestations of self-preservation behavior. Every third (32.9%) received information about the Foundation from acquaintances (acquaintances could also be employees of the Foundation, volunteers of the Foundation), 17.5% found information on the Internet (posted by the Foundation’s employees), 18.3% learned directly from communication with the Foundation’s employees, the rest from printed materials, mailings in thematic mobile applications. In brothels, the Foundation’s employees met and persuaded every tenth (13.7%) to be tested, the rest - on the street, points of prostitution, in places of entertainment, in pharmacies when trying to buy personal protective equipment (condoms) or syringes (6.0%). For 35.4%, the visit to the Foundation was not the first: some clients monitor their health and undergo testing regularly (in case of suspicion of HIV infection).
Usual Practices of the Fund’s Clients
In general, over the past year (before the survey), respondents practiced behaviors that could well lead to HIV infection, other STIs or hepatitis. First of all, we are talking about the use of drugs, about sex without means of protection. One in three (30.7%) had sex with HIV-infected people whose status was confirmed, and one in ten had sex with a person whose HIV status the respondent was not sure about (11.3%). In addition, more than half did not use a condom (54.7%), every tenth person is involved in prostitution (10.4%) or used the services of people engaged in prostitution (14.3%), 6.2% do not remember whether they had contact with such people or not. Most claim that they use protective equipment when resorting to sex services (except in isolated cases).
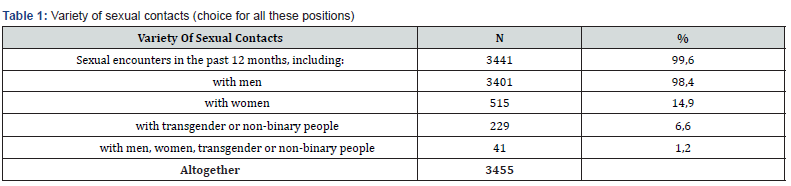
In the last 12 months before the survey, almost all clients (99.6%) had sexual contacts, primarily with men (98.4%), less often with women (14.9%), with transgender or non-binary people (6.6%). Only a few practice sex with representatives of all the above-mentioned socio-demographic groups (Table 1). At the same time, contacts with women in the last year were among men who definitely consider themselves homosexuals (2.7%). In general, 19.4% use drugs, of which 2.8% are injected and 18.7% are non-injected, 2.1% are injected and non-injected (Table 2). In isolated cases, common injection equipment is used (less than 1% - 12 people). Respondents named up to 17 types of narcotic substances that they use. Two types of drugs are most often used (9.7%), three or four types - 7.5%. At the same time, 17.8% use drugs before and/or during sex (chemsex) in order to make sexual sensations are brighter or longer-lasting.

The behavioral practices of respondents and their partners are complicated by a negative state of health - the presence of diseases that are transmitted during drug use or sexual intercourse. Every tenth person is infected with HIV (12.3%): 5.4% already knew about their positive HIV status before joining the Fund, 8.8% were diagnosed with HIV infection in the Fund. 7.5% are sick or have had syphilis, 2.2% have hepatitis C, and 1.1% have had hepatitis B. 1.1% of the Foundation were diagnosed with tuberculosis, which is not an STI, however, is closely associated with HIV infection. These data indicate that the prevalence of HIV infection or STIs among the representatives of the study group is much wider than the average among the adult population of Russia.
Specific Health Care Practices
It is obvious that the Fund’s clients are aware of their vulnerability to social diseases and are taking some necessary actions aimed at mitigating or preventing the situation of infection. Almost all were tested for the presence of syphilis (97.3%), obviously, it is this disease that causes the greatest concern among the contingent with a designated lifestyle (Table 3). The fear of HIV infection is also very high – in 79.6% of clients. 79.4% applied to the Foundation to be tested for HIV infection, some of them repeatedly. The study group is tested for the presence of gapatitis less often than for the presence of HIV infection: 48.8% were tested for the presence of hepatitis C, and 30.4% for the presence of hepatitis B. 26.4% are vaccinated against hepatitis A and 26.3% are vaccinated against hepatitis B. Half of the MSM who agreed to visit the Foundation’s office indicated that they came because they consider it necessary to monitor their health (54.6%) and/or find out their HIV status (57.3%). A few indicated that they had been asked to do so by a partner or before stopping using a condom with their partner (˂1%, 28 people). Almost all additionally indicated that they had risky sexual contacts and this now worries them. Such contacts were with men in 98.0% of clients, with women in 14.9% and with transgender people (within three percent).

Of course, the self-preservation behavior of the study group and its elements differ significantly from the self-preservation behavior of an ordinary person, when there is no need to talk about a lot of dubious sexual partners, involvement in prostitution and the need for constant health monitoring for the presence of social diseases. The self-preservation behavior of the study group consists of the main types of actions that can prevent the disease, cure or improve well-being:
a) ongoing actions aimed at preventing one’s own illness and the partner’s illness or treatment in the event of an existing illness (for example, do not use drugs or do not use common injection equipment, are not associated with prostitution, use condoms);
b) single actions taken to establish a diagnosis, start treatment or change an unhealthy and dangerous lifestyle (contacting a specialist in order to solve the problem of determining health status, receiving recommendations from a specialist, including vaccination).
c) possible actions (for which we have not received data) - lifestyle changes, including: quitting drug use, stopping prostitution or resorting to the services of people engaged in prostitution.
In general, the behavior of the Foundation’s clients can be dangerous, destructive, for their own health and the health of partners, since every third of them has previously or currently had one or more social diseases, including HIV infection. One in three has had sexual contact with HIV-infected people whose status has been confirmed, and one in ten has had sex with a person whose HIV status the respondent was not sure of. Less than half are protected (use a condom). One in ten is involved in prostitution or has resorted to the services of people engaged in prostitution.
References
- Pokrovsky VV, Ladnaya NN, Sokolova EV (2021) HIV infection: newsletter No. 46. M. 2021. Russia, p.
- Lipova EV, Tarasenko GN, Gryazeva NV (2012) Epidemiological aspects of human papillomavirus infection and associated malignant neoplasms. Russian Journal of Skin and Venereal Diseases 3: 51-55.
- Plavinsky SL, Barinova AN, Eroshina KM, Bobrik AV, Novozhilov AV, et al. (2009) Sexually transmitted infections (STIs) and HIV infection in at-risk groups. Do pathogens spread through the same networks? Russian family doctor 1: 26-31.
- Peterson JA, Reisinger HS, Schwartz RP, Mitchell SG, Kelly SM, et al. (2008) Targeted Sampling in Drug Abuse Research: A Review and Case Study. Field Methods 20(2): 155-170.
- UNAIDS (2022) Global AIDS Monitoring. Geneva: Joint United Nations Programme on HIV/AIDS, p.216.
- Beyrer C, Baral SD, Griensven VF, Goodreau SM, Chariyalertsak S, et al. (2012) Global epidemiology of HIV infection in men who have sex with men. Lancet 80(9839): 367-77.
- Nazarova IB (2007) Health of the employed population. Moscow: Maks Press, p. 526.
- Antonov AI (1998) Microsociology of the family (methodology of research of structures and processes): Textbook. Nota Bene M(ed.), manual for universities, p.360.
- Antonov AI (2005) Microsociology of the family: a textbook for students. universities, training. by special. 020300 "Sociology": Classical university textbook. In: MV Lomonosov (ed.), In: 2nd (edn), Moscow State University named after, p. 368.
- Etzioni A (2002) Socioeconomics: further steps. Economic sociology 3(1): 65-71.
- Antonova DV, Bocharov VV, Khrustaleva NS (2019) Risky sexual behavior of persons with human immunodeficiency virus. Medical-biological and socio-psychological problems of safety in emergency situations 4: 79-87
- Cassel J (1964) Social science theory as a source of hypotheses in epidemiological research. American Journal of Public Health and the Nation’s Health 54(9): 1482-1488.
- Krieger N (2001) A glossary for social epidemiology. J Epidemiol Community Health 55(10): 693-700.
- Bruno VV (2019) Risky sexual behavior of modern adolescents in Russia Part II. Sociological Science and Social Practice 7(1): 113-126.
- Nechaev VV, Ivanov AK, Yakovlev AA, Musatov VB, Fedunyak OI, et al. (2018) Epidemiology of socially significant co-infections. Risk factors for lethal outcomes 3(73): 68-71.
- Ennett ST (1999) Social network characteristics associated with risky behaviors among runaway and homeless youth. Journal of Health and Social Behavior 40: 63-78.
- Pyshkina AS, Zhabina UV, Osmanov EM, Vedishchev SI (2011) On the issue of reproductive attitudes of modern student youth. Tambov University Review, Series: Natural and Technical Sciences 16(6-1): 1532-1534.
- Morales A, Méndez X, Orgilés M, Espada JP (2017) Personality profiles of sexual risk among Spanish adolescents. Journal of Clinical Psychology with Children and Adolescents 4(1): 41-49.
- Pozdnyakova ME (2018) Risky sexual behavior as a factor in the spread of HIV infection in Russia. Part 2 4(24): 105-116.
- McKusick L, Horstman W, Coates TJ (1985) AIDS by gay men in San Francisco. Am J Public Health 75(5): 493-496.
- Tulupyeva TV, Pashchenko AE, Tulupyev AL, Golyanich VM (2010) Models of HIV-Risk Behavior in the Context of Psychological Protection and Adaptation. Petersburg University Review. Series 12. Psychology. Sociology. Pedagogy. SPb 1: 108-115.
- Tulupyeva TV, Tulupyev AL, Pashchenko AE (2007) Psychological protection and coping strategies of HIV-infected people from the standpoint of danger to public health: automation of data collection and research results 4: 357-387






























