The Impact of Health Risk Behaviors on Mental Health of Minority Young Adults Living in High HIV Prevalence Urban Community
Meya Y B Mongkuo1*, Maurice Y Mongkuo2, Nicole Lucas2, Frederick Ayivi2 and Gregory DeLone2
1Virginia State University, United States of America
2Fayetteville State University, United States of America
Submission: February 14, 2020; Published: February 28, 2020
*Corresponding author: Meya Y B Mongkuo, Virginia State University, United States of America
How to cite this article:Mongkuo M.Y.B., Mongkuo M.Y., Lucas, N., Ayivi, F., & Delone, G. The Impact of Health Risk Behaviors on Mental Health of Minority Young 00129 Adults Living in High HIV Prevalent Urban Community. Psychol Behav Sci Int J. 2020; 14(4): 555892. DOI:10.19080/PBSIJ.2020.14.555892.
Abstract
Aim: Young adulthood is a period when individuals engage in health risk behaviors such as tobacco use, alcohol consumption and illicit substance use that may predispose them to mental problems. Minority young adults living HIV prevalent urban communities are especially more likely to engage in these behaviors. With the disproportionate representation of minority young adults with co-occurrence of HIV infection and mental problems in the United States, few studies have assessed the predictive influence of these health risk behaviors among this vulnerable population. The aimed of this study was to begin this line of inquiry to gender by examining the magnitude of effect of alcohol consumption, tobacco use and illicit substance use on mental health of minority young adults living in a high HIV prevalent urban community.
Methods: Survey data of the level of tobacco use, alcohol consumption, illicit substance use and mental health were collected from minority young adults living in an HIV prevalent urban community. The data subjected to descriptive and structural equation modeling (i.e., exploratory factor and confirmatory factory analysis) statistical analysis procedures. The magnitude of statistical and practical significance effect of the exogenous constructs on the endogenous construct was determined by calculating the standardized coefficient (Beta weight) and effect size (Cohen’s d) in the multivariate model.
Result: The study found that illicit substance use had a large statistically significant and practically significant positive effect on mental health disorder of minority young adults (B=0.69; t=16.090; p=001). Alcohol consumption had a weak statistically insignificant negative effect on mental health of minority young adults (B= -0.12; t=-1.783; p=.075). Tobacco use had a weak statistically insignificant positive effect on mental health disorder of minority young adults (B=.09; t=1.313; p=.189). The causal model was reliable with Cronbach’s alpha based on standardized items for each variable in the causal model exceed the acceptable lower bound threshold of 0.60 (alcohol consumption=.785; tobacco use=.843; illegal substance use=.896). The causal model was internally valid with comparative fit indexes adequate for a model of this complexity (CFI=.996; TL=.994; RMSEA=.024). The likelihood that the model’s parameter estimates from the original sample cross-validating across in future samples showed Akaike’s (1978) Information Criterion (AIC) and Bozdogen’s (1987) consistent version of the AIC (CAIC) values of the hypothesized model lower (AIC=67.980; ECVI=.137) compared to the independent model (AIC=70.000; ECVI=.141) and saturated model (AIC=1803.335; ECVI=3.628 suggesting an appropriate fit to the data. Adequate model fit for the χ2 test showed Hoelter’s Critical N (CN) was 527 for 0.05 CN and 674 for 0.01 CN indicative of the structural model’s adequacy in representing the sample data. Normality of the distribution of the model’s variables showed Mardia’s normalized estimate of multivariate kurtosis value of .34 reflexive of normal distribution. Multivariate outliers showed squared Mahalanobis distance (D2) for each case with D2 values not standing distinctively apart from all the other D2 values, indicative of no outlier.
Conclusion: These finding supports our research hypothesis that illicit substance use has an adverse effect on mental health of minority young adult; but does not support the hypotheses that tobacco use, and alcohol consumption have an adverse effect on mental health of minority young adults. We recommend that prevention programs aimed at reducing mental health minority adults living in high HIV prevalence communities should focus on evidence-based illicit substance use prevention strategies. Also, to externally validate these findings, future cross-sectional and longitudinal studies, preferably Latent Growth Curve (LGC) model withing the framework of structural equation modeling, should be conducted on minority young adults living in high HIV prevalent communities.
Keywords: Excessive alcohol consumption; tobacco use; Substance use; Mental health; Structural equation modeling; Exploratory factor analysis; Confirmatory factor analysis; Cohen’s effect size; Risky health behavior; Practical significance; Statistical significance; Minority young adults. HIV prevalence community; Pre-experimental one-shot case study
Abbreviations: STIs: Sexually Transmitted Infections; CIHPP: Comprehensive Integrated HIV Prevention Program; HPG: Hypothalamic-Pituitary-Gonadal; HPT: Hypothalamic-Pituitary-Thyroid; RCT: Randomized Clinical Trials; HPP: Hypothalamic-Pituitary-Adrenal; AVP: Arginine Vasopressin; PVN: Paraventricular Nucleus; HPA: Hypothalamic-Pituitary-Adrenal; ACTH: Adrenocorticotropic Hormone; CRH: Corticotropin-Releasing Hormone; IRB: Institutional Review Board’s; CFA: Confirmatory Factor Analysis; FIML: Full Maximum Information Likelihood; RMSEAs: Root Mean Square Errors of Approximation; CFI: Comparative Fit Index; TLI: Tucker-Lewis Index; CAIC: Consistent Version of the AIC; ECVI: Expected Cross-Validation Index; CN: Critical N; LGC: Latent Growth Curve
Introduction
Mental health problems account for half of the disease burden for young adults in US [1], and many psychological disorders first occur in late adolescence or early adulthood, Kitzrow [2], with most before age 24 [3]. Mental health problems refer to any diagnosable mental, behavioral, or emotional disorder such as depression, stress, anxiety, and disruptive behavior [4]. In 2013, approximately 25% of adults in the United States had some form of mental disorder, and those adults consume 40% of all cigarette smoke by adults [4]. Among young adults, research shows a disproportionate number of people with mental health problems engage in risky sexual behavior such as excessive alcohol consumption, tobacco use, and illegal substance use [5].
Risk behaviors is defined as the taking of any substance whether alcohol, drugs, and/or tobacco for mood-altering purposes that would lead to risky sexual behaviors [6]. In this study, excessive alcohol consumption refers to binge drinking or heavy drinking. Binge is defined as drinking five or more alcohol drinks on the same occasion (i.e., at the same time or within the same a couple of hours of each other) on at least one day in the past 30 days [7]. The alcohol-related mental health problems include depression [8-16], anxiety [17], cognitive impairment [18-20]. Heavy drinking is drinking five or more on the same occasion on each of 5 or more days in the past 30 days [7]. Excessive alcohol consumption has been identified as one of the major barriers to physical and mental health among young adults in the United State, costing the U.S. healthcare system approximately $223 billion per year. However, the effect of light or moderate alcohol consumption on health outcomes is less clear [21]. For example, while a number of previous research has shown that light/moderate alcohol consumption may be associated with improved health outcomes related to cardiovascular disease, [22-24], diabetes [25]; dementia [26], reduced sickness absence and disability pension award [27-29] and less mortality [30,31], other researchers have dismissed the finding of these studies as based on systematic biases, confounding factors, or reverse causality [32].
Tobacco use refers to smoking cigarettes, cigars, smokeless tobacco, e-cigarette and pipe tobacco in past year and past month [4]. Studies show that one in five individuals within the U.S. have a mental health disorder, yet this population consumes almost half of all cigarettes sold within the U.S. [33,34]. As a result, individuals with mental health disorder account for more than 40% of tobacco related deaths each year [35,36] and incur additional social constraints such as discrimination and stigma which contribute to increased alienation and poorer mental health [36-38]. Illicit substance includes, but not limited to, ecstasy, opioid, crack cocaine, methamphetamine, and inhalants that reduce pain, including prescription drugs and heroin which has been found to be associated with increased HIV risk if people share needles and other injection equipment; WHO/UNAIDS (2004); WHO (2005); CDC (2005); ScienceDaily (2007). Recent data indicate that one-third of new HIV infection the United States attributed to noninjection substance use such as ecstasy, methamphetamine, inhalants, and crack cocaine [39-42]. Mental health problem includes depression, anxiety and ADHD, stress, lack of self-esteem, unstable school environment, attitude, peer delinquency, and street involvement [43-47].
Risk behavior and HIV prevalence
Existing data show that risk behavior is higher among minority young adults than other racial and age groups in the United States, and accounts for a higher rate of sexually transmitted infections (STIs), including HIV, than other racial age groups. This high risky sexual behavior in turn has led to high prevalence of STD, including HIV in minority communities across the United States making STD prevention a top priority. For example, in the last decade alone, the U.S. Department of Health and Human Services has invested heavily by awarding over 100 million dollars in grants to community-based organizations and institutions of higher learning to design and implement innovative culturally and linguistically appropriate evidence-based strategies to reduce health risk behaviors among this subpopulation. One such strategy is the comprehensive integrated HIV prevention program (CIHPP). The CIHPP is a high impact approach to HIV and other infectious diseases prevention targeted to at-risk populations. The approach has been highly endorsed by the Center for Disease Control, Health Resource and Service Administration and the Institute of Health as the most effective evidence-informed strategy to prevent infection and spread of HIV and other infectious diseases among at-risk populations.
This approach to HIV prevention is premise on the ecological epistemology framework which recognizes that health risk behaviors such as excessive alcohol consumption, illicit substance use, and tobacco use involve complex interactions between social and biological factors [48-51]. This framework is derived from Jessor’s [52] problem behavior theory (PBT) which proposes interrelated conceptual domains of risk factors for adolescent and young adults [52]. This theory proposes that young adult risk factors consist of personality system, social environment, and behavior. The theory has been extended to the domain of psychosocial theory that view health risk behaviors as co-occurring [52,53] among young adults. Collectively, these theories suggest that assessing the effectiveness of prevention programs should include an examination of the association between externalizing problems (such as alcohol consumption, illicit substance use, and tobacco use) and internalizing problems (such as depression, anxiety, disruptive behavior, etc.). Based on Bronfenbrenner's [54] ecological epidemiology framework, effective prevention strategies should identify and address predisposition of high sexually transmitted prevalence of sexually transmitted infections individuals and communities at all four levels (i.e., individual, interpersonal, community, and societal) that predispose minority young adults to risky sexual behavior. The prevalence of individual level risk behavior includes having multiple sex partners, having sex without condoms, having concurrence partnerships, sharing infected needles, etc. that are affected by community alcohol, illicit substance and tobacco environment. The prevalence of interpersonal risk behavior refers to social and sexual network structural (i.e., network size, density, mixing, and turnover) and compositional factors (i.e., characteristics of network members) that influence minority young adult HIV transmission. Community level risk factors include density of alcohol, tobacco, and illicit substance outlets [55-59].
Societal level risk factors encompass public policies that shape the environment of the community such as policies that promote high density of alcohol outlets in poor and minority neighborhoods leading to segmentation of drinkers in hot spots for HIV risk behaviors and HIV transmission [60]. In essence, the ecological epistemology framework is a multilevel structure in which social and environmental structures and contexts are thought to influence health outcomes such as mental health problems. This framework, and by extension Jessor’ problem behavior theory proposes a complex disease system characterize by disease and/or mental health problem with multiple causative factors that are manifested in both social and physical contexts in a particular population. The multiple level of influence is concentric circles beginning with the individual level, the neighborhood or community level, and societal level [51,54]. The framework in based on the idea that individuals operate within spheres of influence at the individual, interpersonal, community, and societal levels. The individual level is considered the microsystem where individual operate within their family and home environment, school and peers, work-peer networks, peer support, family support, parental mentoring, parental involvement in health risk behaviors networks. This individual level characteristics is nested within the larger community which consists of community norms attitude regarding health risk behavior, cultural norms, gender norms, spiritual and religious norms and ideological and political norms. The individual level health risk behavior may include excessive alcohol consumption, tobacco use, and illicit substance use, and unsafe sexual practice or behavior. Interpersonal characteristics are social and sexual network, social norms, illicit substance use, and setting/situational factors. Community health risk behaviors include alcohol access environment, community social and economic disadvantages, crime, and homelessness. Societal health risk are racism, stigma, segregation, formal and informal public policies, and religious and cultural norms. The micro-policy level may also include biological and physiological status of important systems of the body that regulate behavior including the nervous system, endocrine system, the digestive system, immune system, and renal system. Macro-policy level consists of advertisements and marketing policy related to health risk behaviors. Hence, effective prevention strategies and policies should include a continuum of activities that address these multiple spheres of influence to achieve desired health outcomes.
The ecological epidemiology framework of the comprehensive HIV prevention program implies identifying the prevalence of HIV infection and transmission rates in the target population by conducting needs assessment of measurable constructs at each level or domain of influence, as well as cross-level connections at both at the micro and macro levels, as well as examining the macrosocial and microsocial or protective factors (risk regulators) that can either constrain or promote the occurrence of individual-level behavior associated with the risk of HIV infection. The needs assessment, in turn, provide objective data for developing a strategic HIV prevention plan for the target population and community.
Alcohol consumption and mental health
Regarding the effect of alcohol consumption on mental health, research has found that excessive alcohol consumption has an adverse effect on two important systems (i.e., the endocrine system and the nervous system) that are essential for controlling the raid flow of information between different organs and cells of the body [61,62]. Specifically, the nervous system is responsible for rapid transmission information between different body regions, while the endocrine system, which is composed of a complex system of glands that produce and secret hormones directly into the blood stream, has longer lasting actions. together, these two systems ensure proper communication between various organs of the body to maintain a constant internal environment called homeostasis of the human body that regulates and stabilizes behavior.
Almost all the organs of the human body that regulate behavior are affected by the hormones that are secreted by the endocrine system including hormones that control metabolism and energy levels, electrolyte balance, growth and development, reproduction, response to, and appropriately cope with, changes in the internal and external environments such as changes in temperature and the electrolyte composition of body fluids, and response to stress, anxiety and injury [61,63-67]. Both acute and chronic alcohol consumption induces hormonal disturbance of the endocrine system that can disrupt the body's ability to maintain homeostasis and may eventually lead to various disorders including cardiovascular diseases, reproductive deficits, immune dysfunction, certain cancers, bone disease, and psychological and behavioral disorders. Research have shown that indulgence in health risk behaviors does not only have an adverse effect on the HPA axis, but practically all hormonal systems of the body including hypothalamic-pituitary-gonadal (HPG) axis [63], the hypothalamic-pituitary-thyroid (HPT) axis [68], hypothalamic-pituitary-growth hormone/insulin-like growth factor-1 (GH/IGF-1) axis [69-75] and hypothalamic-posterior pituitary (HPP) axis [61,76-79].
A recent review of studies on youth and adolescents similarly suggests that hypothalamic-pituitary-adrenal (HPA) axis dysfunction and exposure to stress are critical components that interact to convey risk for developing AUDs. For example, several randomized clinical trials (RCT) has found that excessive alcohol consumption has adverse effect on normal functioning of the nervous and endocrine systems, both of which are responsible for proper communication between various organs and cells of the body to maintain a stable internal environment or homeostasis [80,81]. Interference of the normal functions of these communication systems sets in motion a series of adverse physiological activities including disruption of the hormonal control of metabolism and energy levels, electrolyte balance, growth and development, and reproduction of the body. These disruptions in turn inhibits the body’s ability to respond to, and appropriately adapt to changes in body temperature or the electrolyte composition of the body’s fluids, response to stress and injury, and psychological and behavioral disorders [61,65,82,83]. As for the nervous system, excessive consumption of alcohol disrupts the vital hormonal flow of the hypothalamic-pituitary-adrenal (HPP) axis that is responsible for cognitive brain functioning. The HPP axis includes two neuropeptides called arginine vasopressin (AVP) and oxytocin.
Other research has focused on the progressive alterations in HPA axis function crucial for understanding the underlying brain mechanisms of substance use disorders. These studies found that in contrast to mood and affective disorders, alcohol dependence has a biphasic effect on HPA axis dynamics as a person traverses through the various phases of heavy hazardous drinking, including dependent drinking, withdrawal, abstinence, and relapse. Generally speaking, these developmental stages seem to be mirrored by a shift between hyper- and hyporesponsiveness of the HPA axis to stressful events [84]. For example, hyperresponsiveness has been identified in people with a family history of alcoholism [66,37], a population that is at increased risk for alcohol dependence [85]. This observation raises the question whether heightened stress responsivity is clinically meaningful to the development of alcoholism. This view is supported by studies showing that cortisol responsivity correlates with the activity of the regulatory function of the nervous system called the mesolimbic dopaminergic pathway, which is a central neural reward pathway [86]. With transition to alcohol dependence, compensatory allostatic mechanisms result in injury to HPA axis function and elevation of stress peptide levels (e.g., corticotropin-releasing factor (CRF) in brain regions outside the hypothalamus. Allostasis refers to the process through which various biological processes attempt to restore homeostasis when an organism is threatened by various types of stress in the internal or external environment [61,87]. Allostatic responses can involve alterations in HPA axis function, the nervous system, various signaling molecules in the body, or other systems. Allostatic alterations in HPA axis function have been posited to, among other things, injure brain reward pathways, contribute to depressed mood (i.e., dysphoria) and craving, and further contribute to the maintenance of problem drinking behavior.
A close examination of the physiology of the hypothalamic-pituitary-adrenal (HPA) axis reveal that the body responds to stress with self-regulating, allostatic processes aimed at returning critical systems to a set point within a narrow range of operation that ensures survival [61,63]. These self-regulating processes consist of multiple behavioral and physiological components. Perhaps the best-studied component of the stress response in humans and mammals is activation of the HPA axis. This line of inquiry has found the neurons in the paraventricular nucleus (PVN) of the hypothalamus release two neurohormones—CRF and arginine vasopressin (AVP)—into the blood vessels connecting the hypothalamus and the pituitary gland (i.e., hypophysial portal blood). Both hormones stimulate the anterior pituitary gland to produce and secrete adrenocorticotropic hormone (ACTH) into the general circulation. The ACTH, in turn, induces glucocorticoid synthesis and release from the adrenal glands, which are located atop the kidneys.
The main glucocorticoid in humans is cortisol; the main glucocorticoid in rodents, which frequently are used as model systems to investigate the relationship between stress and alcohol use, is corticosterone. Hypothalamic activation of the HPA axis is modulated by a variety of brain signaling (i.e., neurotransmitter) systems. Some of these systems have inhibitory effects (e.g., g-aminobutyric acid [GABA] and opioids), whereas others have excitatory effects (e.g., norepinephrine and serotonin) on the PVN. Thus, the central nervous system (CNS) and the hormone (i.e., endocrine) system are tightly interconnected to coordinate glucocorticoid activity [88,89]. To protect against prolonged activity, the HPA system is carefully modulated through negative-feedback loops designed to maintain predetermined hormone levels (i.e., set points) and homeostasis. To this end, secretion of CRF, AVP, and ACTH in part are controlled by sensitive negative feedback exerted by cortisol at the level of the anterior pituitary gland, PVN, and hippocampus. There are two types of receptors for cortisol—mineralocorticoid (type-I) and glucocorticoid (type-II) receptors— both of which participate in the negative feedback mechanisms. Cortisol binds more strongly (i.e., has higher binding affinity) for the mineralocorticoid receptors (MRs)1 than the glucocorticoid receptors (GRs). Because of this difference in binding affinity, the MRs help maintain the relatively low cortisol levels circulating in the blood during the normal daily (i.e., circadian) rhythm. Only when the cortisol concentration is high (e.g., during a stressful situation) does it bind to the GRs with lower affinity; the resulting activation of the GRs terminates the stress response. This delicate negative feedback control mechanism maintains the secretion of ACTH and cortisol within a relatively narrow bandwidth. This is an extremely important homeostatic mechanism because too much or too little exposure AVP is secreted in response to osmotic stimuli and is involved in regulating the concentration of dissolved molecules (i.e., osmolality) in the blood fluid by retaining water in the body and constricting blood vessels [78,90]. Some AVP are released directly in the brain, and research suggest that it play an important role in social behavior, sexual motivation and pair bonding, as well as maternal response to stress [91,92].
Excessive alcohol consumption lowers the level of AVP to the brain leading to impaired cognitive performance [93]. Like AVP, oxytocin is produced by both magnocellular and parvocellular neurons of the hypothalamus, and functions both as a peripheral hormone and a signaling molecule in the central nervous system [94] to regulate adaption of the body to respond effectively to internal physiological and environmental changes or disruptions. Research on people with a history of excessive alcohol consumption shows that hyper responsiveness of the stress response mediated by the HPPA axis [66] leading to mental health problems. In addition, research on animal found acute ethanol administration to rats increased plasma ACTH and corticosterone levels by enhancing CRF release from hypothalamus [95,96]. Chronic alcohol consumption was found to be associated with anxiety-producing (i.e., anxiogenic) behavior [97]. Collectively, these studies show that excessive or chronic alcohol consumption attenuates basal ACTH and corticosterone levels and increases stressful and anxiogenic behaviors. Other studies have found an association between excessive alcohol consumption and depression among young adults [98-100].
Tobacco use and mental health
Individuals with mental health problems represent a priority population for tobacco prevention and control due to disparities in tobacco use and subsequent adverse health effects. Young adulthood is a period in life for substance experimentation and increased mental problems including the use of tobacco products and increased mental health problems. The Royal College of Psychiatrists [101] reports that the prevalence of tobacco use-related mental health problems is higher among minority groups with substance and alcohol-dependent than non-minority groups. Similar to alcohol consumption, research has found that tobacco use stimulates the HPA axis and proceeds through a central mechanism to stimulate and elevate the level of corticotropin-releasing hormone (CRH) and arginine-vasopressin (AVP) and release of adrenocorticotropic hormone (ACTH) from the anterior pituitary [102] leading to disruption of the regulatory function of HPA axis. This HPA dysregulation causes stress which exacerbates mental health disorder manifested in withdrawal symptoms including irritability, depression, frustration, poor mental concentration, insomnia, and restlessness [103-108].
Numerous studies have found that the adverse health effects of mental activity among young adults who use tobacco is numerous, including internalizing problems such as depression [109-113], anxiety [17,114-117] and adverse cognitive outcomes, such as memory deficits [18-20] such as disruptive behavior [117-119] oppositional defiant disorder and attention deficit/hyperactivity disorder [120,121] and adverse cognitive outcomes, such as memory deficits [18-20]. Furthermore, tobacco users had greater stress, role limitations from emotional problems, and poorer health satisfaction than non-tobacco users [122]. Other studies show that one in five individuals within the U.S. have a mental health disorder, yet this population consumes almost half of all cigarettes sold within the U.S. [33,34].
As a result, individuals with mental health disorders account for more than 40% of tobacco related deaths each year [35,36] and incur additional social constraints such as discrimination and stigma which contribute to increased alienation and poorer mental health [36-38]. Hence, in the United States, individuals with mental health problems who use tobacco represent a priority population for tobacco prevention and control due to disparities in use and subsequent health effects. To date, however, research findings on the relationship between tobacco use on mental health has been mixed. For example, some studies have found tobacco use to be associated with adverse cognitive outcomes, such as memory deficits [18-20]. Studies on cannabis users, however, found no association between tobacco use and cognitive deficits such as episodic memory loss [123,124], and deficits in visual recognition, verbal fluency, or delayed visual recall [125].
Illicit substance use and mental health
Numerous studies have identified a number of predictors of substance use on mental health among young adults including gender, low socio-economic status, parental substance use, peer influence, social support, and broken families. Other studies have found a positive correlation between substance use and mental health disorder (e.g., schizophrenia, bipolar and major mood disorder). Other research found that persons with comorbid psychiatric and substance disorder engage in more overall HIV risk-risk behavior than persons who have substance use disorder alone, including a number of HIV-risk sexual behaviors such as sex with intravenous drug users and engagement in sex for money/gifts and have a greater likelihood of reporting HIV/AIDS diagnosis [159]. In a recent study involving 270 adults with substance use disorder who are receiving mental health treatment, Majer et al. in 2015 found a strong positive association between substance use and severity of mental illness.
Co-occurrence of risky sexual behavior and mental health
Research on people engaged in any combination of these risky sexual behaviors (i.e., alcohol use, tobacco use and illegal substance use) have found a positive correlation between these behaviors and mental health problems [126,127]. Another study has found a link between co-occurrence of substance and alcohol use, and internalizing and externalizing mental health disorders among young adults [5]. Research on co-occurrence of tobacco use and alcohol consumption found a strong positive relationship between the two health risk behaviors at the individual level among young adults [128-131]. For example, a survey by SAMHSA [4] found that adults with mental illness use more tobacco (36.5%) than adults with no mental illness (25.3%).
Gateway theory states that people who use tobacco and alcohol have a higher likelihood of transitioning towards illicit substance use such as injected drugs, marijuana, and prescribed psychoactive [126,132-134], found substance abusers are more nicotine dependent than non-abusers. This finding is supported by numerous studies that found high prevalence of cigarette smoking among illicit substance users [126]. More recently, research on tobacco use have found that heavy smokers were more likely to report substance use such as pain-killer use and binge drinking [135]. Another study has found a link between co-occurrence of substance and alcohol use and internalizing and externalizing mental health disorders among young adults [5]. It suggests, therefore, that the design and assessment of a comprehensive HIV program should incorporate co-occurrence of these risk factors.
Purpose and objectives of the study
The purpose of this study was to begin a line of inquiry in closing this gap in research by assessing the effect of risky behaviors on mental health of minority young adults in high HIV prevalent communities. Understanding the effect of risky behaviors on the mental health of minority young adults living in high risk HIV communities is critical for effective evidence-informed HIV prevention interventions designed to control the disproportionate spread of HIV infection and other sexually transmitted infections in this most vulnerable population in the United States. Existing research on the effect of risky behavior factors on mental health of minority young adults is limited. While research on the link between risky behaviors and mental health problems have been quite impressive, the units of analysis of almost all these studies have been on the general population as a whole, not minority young adults who, as discussed above, are disproportionately endowed with risk behavior-related mental health problems. Moreover, almost all the studies using the epidemiological theoretical framework outlined above have focused on the general population, not exclusively on minority young adults. The objective of this study was to fill this gap in research by systematically determining the magnitude of effect of risky sexual behaviors such as tobacco use, illicit substance use, and excessive alcohol consumption on the mental health of minority young adults living in HIV prevalent communities. We hypothesized that tobacco use, illicit substance use, and excessive alcohol consumption have an adverse effect on the mental health of minority young adults living in high HIV prevalent communities.
Research questions
What is the effect of alcohol consumption on mental health of minority young adults living in a high HIV prevalent community?
What does the effect of tobacco use on mental health of minority young adults living in a high HIV prevalent community?
What is the effect of illicit substance use on mental health of minority young adults living in a high HIV prevalent community?
Research hypothesis
Alcohol consumption has a negative effect on mental health of minority young adults living in a high HIV prevalent community.
Tobacco use has a negative effect on mental health of minority young adults living in a high HIV prevalent community.
Illicit substance use has a negative effect on mental health of minority young adults living in a high HIV prevalent community.
Methods
Research design
The study used a pre-experimental One-shot case Study Design [136-138]. A schematic representation of the study design is displayed in Figure 1. Where X is a minority young adult’s level of tobacco use, illicit substance use, and excessive alcohol consumption. O2 is the level of a minority young adult’s level of mental health problem. The limitations of this type of research design is outlined in the discussion section of this article.

Participants and procedure
Participants in this study were a random sample of minority young adults (18-24 years old) living in a high prevalent community in the southeastern United States who volunteered to participate in the study. After receiving Institutional Review Board’s (IRB) approval, culturally and linguistically appropriate announcements and advertisements were made to residents of the high HIV prevalence community through various young adult outlets including social media, radio, print media, community organizations, word-of-mouth and distribution of flyers in the community to attend a community health events and participate is a healthy living event. Attendees at the health event were informed that a survey was being conducted to obtain their opinion about key risky behaviors that may predispose people to mental health problems. They were also informed that their participation was strictly voluntary and that they may either opt not to participate in the survey and leave or not provide a response to any of statements. In addition, the community residents were informed that a no-cash incentive in the form of $10 gift card would be provided for their participation in the study. The community residents who agreed to participate in the survey were provided with a linguistically appropriate consent form to read, sign and date. The consent form explained to the community residents that their participation was be voluntary and that their identity would be kept strictly confidential, and their names would not appear in any report.
The survey instrument used in this study is the National Minority Substance/HIV Prevention Initiative Adult Questionnaire approved on March 15, 2016 by the United States Office of Management and Budget. Items measuring the four constructs (i.e., tobacco use, alcohol consumption, illicit substance use and mental health) of this study were extracted from this Questionnaire. It should be noted that the validity of the constructs in this measurement instrument has not been validated. Hence, we had to use the data collected from participants in the EBI to validate the instrument using confirmatory factor analysis (CFA). The questionnaire included items measuring the four constructs of the study (the level of tobacco use, alcohol consumption, illicit substance use and mental health), and demographic information of the participants. Upon IRB approval, we administered the survey to the participants who volunteered, read and signed the consent form. We adhered to all American Psychological Association research guidelines. The survey was anonymous in that no identifying information was connected to individuals or included in the study data set. Participants completed the survey in less than 25 minutes during the event and returned them before leaving. Total of 518 minority young adults participated in the survey, and 499 of them completed the entire survey representing a 96 percent response rate.
Measures
The items measuring tobacco use, alcohol consumption, illicit substance use, and mental health were extracted from the National Minority Substance/HIV Prevention Initiative Adult Questionnaire.
Alcohol consumption was measured by 2 items such as “During the past 30 days, on how many days did you drink one or more drinks of alcohol beverage?” The items were scored on a Likert Scale ranging from 0 days = 0 to 30 days = 30.
Tobacco use was measured by 3 items such as, “During the past 30 days, on how many days did you use tobacco products?” The items were scored on a Likert Scale ranging from 0 days = 0 to 30 days = 30.
Illicit substance use was measured by 5 items such as “During the past 30 days, on how many days did you use marijuana or hashish?” The items were scored on a Likert Scale ranging from 0 days=0 to 30 days=30. Mental Health was measured by 1 item such as “Now think about your mental health, which includes stress, depression, and problems with emotions, for how many days during the past 30 days was your mental health NOT good?” The item was scored on a Likert scale with scores ranging from 0 day = 0 to 30 days = 30.
Statistical Analysis
Latent variable structural equation modeling analysis was performed to assess the influence of excessive alcohol consumption, tobacco use and illicit substance use on mental health disorder using Analysis of Moment Structure (AMOS) 24.0 [139]. Specifically, in response to research question 1 above, exploratory factor analysis (EFA) was performed to determine the factorability of the each of the latent constructs. Internal consistency of the constructs was assessed by Cronbach’s Alpha test with alpha of 0.07 considered to be adequate internal consistency. The goal of these analyses and test is dimension reduction of the latent constructs of interest [140]. In essence, the interest was in placing substantive meaning on the factors extracted. Once the factorability was determined, confirmatory factor analysis (CFA) was performed to assess the fit of model to the data, and to estimate the magnitude and significance of the effect of each of the exogenous constructs on the endogenous latent construct, academic success. To make full use of the available data, full maximum information likelihood (FIML) estimation procedure was used. A number of indices was used to evaluate the goodness of fit of the three-factor orthogonal health risk-related mental health problems structural model. The model absolute fit was assessed using chi-square statistics, χ2, with low χ2 considered good fit [141]. Incremental fit was evaluated using the Root Mean Square Errors of Approximation (RMSEAs) with a value less than 0.06 indicating a relatively good fit, along with Comparative Fit Index (CFI) and Tucker-Lewis Index (TLI) with values of 0.95 or greater considered desirable [141-144]. The likelihood that the model’s parameter estimates from the original sample was cross-validated across in future samples will be assessed by examining Akaike’s [145] Information Criterion (AIC) and Bozdogen’s [146] consistent version of the AIC (CAIC) with lower values of the hypothesized model compared to the independent and saturated models considered to be appropriate fit. The likelihood that the model cross-validates across similar-sized samples from the same population was determined by examining the Expected Cross-Validation Index (ECVI) with an ECVI value for the hypothesized model lower compared to both the independent and saturated models considered to represent the best fit to the data. Finally, Hoelter’s [147] Critical N (CN) was examined to determine if the study’s sample size was sufficient to yield an adequate model fit for a χ2 test [148] with a value in excess of 200 for both 0.05 and 0.01 CN indicative of the structural model’s adequacy in representing the sample data.
Normality of the distribution of the model’s variables was assessed by Mardia’s [149,150] normalized estimate of multivariate kurtosis with a value of 5 or less reflexive of the normal distribution. Multivariate outliers were detected by computation of the squared Mahalanobis distance (D2) for each case with D2 values standings distinctively apart from all the other D2 values as indicative of an outlier [151]. The magnitude of effect of excessive alcohol consumption, tobacco use, and illicit substance use on mental health was determined by estimating the standardized regression lower than 0.05 too small to be considered meaningful influences on academic success, even when they are statistically significant; those between 0.0 and 0.10 considered modest influence; those between 0.10 to 0.25 were considered moderate influences on academic success; and those above 0.25 were considered large effects on academic success [152].
Results
Analysis of the data shows that the sample for the study was approximately representative of the population. For example, the frequency distribution of the sample by race show that a majority of the students (73%) was African Americans, 14% was whites, 6% was biracial, 5% was Hispanics, and 2% was other races. For age group, 77% was 18-24 years old, 14% was 26-44 years old, 5% was 35-44 years old, and 4% was above 4 years old. Gender distribution shows that majority of the respondents were female (63%) compared to 37% male. The breakdown by academic class shows that majority of the respondents (42%) were freshmen, 25% were sophomores, 19% were juniors, and 12% were seniors. These results suggest that the study sample distribution was similar to the population distribution described above, and therefore can be considered representative of the PBC student population of this study.
The result of the effect of excessive alcohol consumption, tobacco use, and illicit substance use on mental health disorder is displayed in Table 1 and Figure 2. The table and figure show the standardized parameter coefficients with factor loadings of latent construct onto the measured variables and the direct effects within the structural portion of the tested structural model. Table 1 shows that the standardized regression weights or factor loadings range from 0.64 to 0.86, which is within the acceptable factor loading range [141]. These standardized weights represent the factor loading of items or observed variables on their individual latent constructs in the measurement model. Test of the absolute fit of the structural model showed a good fit of the data to the model (χ2 (9, 498) = 15.980., p=.067). Evaluation of 1ncremental fit indicated a relatively good fit with Root Mean Square Errors of Approximation (RMSEAs) = .04; Comparative Fit Index (CFI)= .996; Tucker-Lewis Index (TLI) = .988). Hence, convergence validity is confirmed. The result of the likelihood that the model cross-validates across similar-sized samples from the same population showed an Expected Cross-Validation Index (ECVI) value for the hypothesized model higher compared to the independent model, but lower than the saturated models (Default Model = 0.195; Saturated Model = 0.094; Independent model = 3.399).
The result of the effect of the excessive alcohol consumption, tobacco use, and illicit substance use is presented in Table 1 and Figure 2. The table and figure show the standardized parameter coefficients with factor loadings of latent construct onto the measured variables and the direct effects within the structural portion of the tested structural model. Table 1 shows that the standardized regression weights or factor loadings range from 0.71 to 0.97. These standardized weights represent the factor loading of items or observed variables on their individual latent constructs in the measurement model. Hence, convergence validity of the motivation measurement model as a whole is confirmed. Also, the fit of the overall health risk-related mental health problem model of this complexity is good (χ2 (9, N=498) = 15.980, p =.067; CFI= .996; TLI= .99; RMSEA = 0.04). The AIC fit statistics of 67/980 for the independent model is lower compared to the both the saturation model (AIC=70.000) and the independent model (AIC=1803.335), indicative fit of the fit of the model to the data. The result of the likelihood that the model cross-validates across similar-sized samples from the same population showed an Expected Cross-Validation Index (ECVI) value for the hypothesized model lower compared to both the saturated model and the independent model (Default Model = 0.137; Saturated Model = 0.141; Independent model = 3.628). This finding suggests that the model did represent the best fit to the data. Hoelter’s (1983) Critical N (CN) show that the study’s sample size was sufficient to yield an adequate structural model fit representing the sample data for a χ2 test (CN for 0.05 = 527 and 0.01 = 674). The result showed the sample did cross-validate across in future samples (AIC for hypothesized model = 73.621; Saturate model = 70.000, Independent model = 2,819.308).

The model explained 48.0% of the variance in mental health problems among the sample of minority young adults studied. Mardia’s normalized estimate of multivariate kurtosis (C.R. value) is -4.64 which is reflexive of a normal distribution. The square Mahanalobis distance (D2) values showed minimal evidence of multivariate outliers. Table 2 displays the estimate standardized coefficients (β) associated with each of the exogenous latent constructs in the structural equation causal model. Illicit substance use had a large positive and statistically significant effect on the mental health of minority young adults (β = 0.69, t = 16.077, p =0.001). Tobacco use had a moderate positive and statistically insignificant effect on mental health of minority young adults (β = 0.08, t = 1.315, p =0.188). Excessive alcohol consumption had a modest negative and statistically insignificant effect on mental health of minority young adults (β = -0.028, t = -1.791, p =0.073). With the exception of illicit substance use, these findings are not consistent with previous health risk behavior-related mental health problem findings of non-minority young adults’ population [126,132-134].
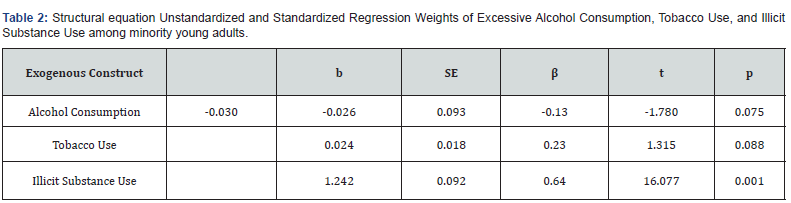
Endogenous Construct: Mental Health Disorder; Square Multivariate Correlation = 48.0% N=498.
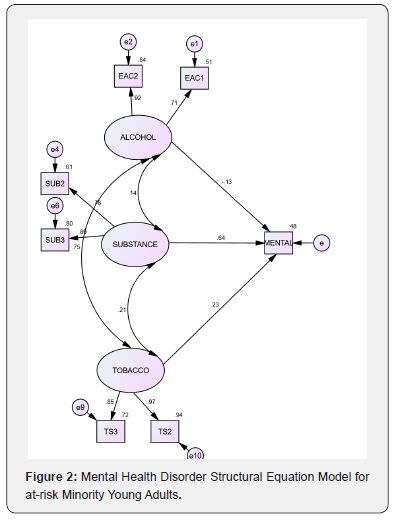
It is important to note that the effects of all the independent variables on the dependent variable in multiple regression model were all not statistically significant. However, many researchers have criticized statistical significance test as not a valid measure of the effect of independent variables on a dependent variable for many reasons [153-156]. First, significance test is based on the null hypothesis which seeks to support or not to support it from the data, as well as claiming to determine whether or not findings occur by chance or not [136]. However, this basis and claim rely on random sampling which in practice, such random sampling rarely occur [156] as in the present study. Furthermore, numerous researchers argue that even if true random sampling is assumed to occur, this does not solve the problem of assuming that the null hypothesis given that in significance testing the true null hypothesis is unknown ([153] p.380);[157]. As Carver ([153] p.381) asserts, “Statistical significance simply mean statistical rareness, not certainty”. Second, statistical significance varies with the sample size of the study. Second, statistical significance varies with the sample size of the study. Ziliak & McCloskey [155] assert that calculating statistical significance as a function of sample size makes it highly unlikely to find statistically effect if large samples are used. Third, since statistical significance is seen as arbitrary in its cut-off points and not so helpful obstacle rather than facilitator, Keith [152] cautions that it may encourage dichotomous thinking where a finding may be considered or not be considered statistically significant. Finally, and perhaps more germane to our study, statistical significance does not tell us what we want to know, that is, the magnitude of effect that the independent variables have on the dependent variable [155,158]. A measure of effect sizes such beta coefficients may be more useful than statistical significance. In fact, Cohen and colleagues assert that statistical significance on its own is no indication of effect or impact, which is what we want to establish.
Discussion
The purpose of this study was to determine the effect of sexual risk behaviors (i.e., excessive alcohol consumption, tobacco use, and illicit substance use) on mental health disorder of minority young adults living in a high HIV prevalence community. The goal study was to begin a line of inquiry aimed at generating relevant data for developing targeted evidence-informed behavioral interventions to effectively reduce mental health disorder which predisposes minority young adults to HIV infection. Tobacco use and alcohol consumption had no meaningful adverse effect on mental health of minority young adults. This finding is not consistent with previous studies on non-minority populations. The study found that illicit substance use was found to have a strong adverse effect on mental health. This finding is consistent with previous studies. Given the strong fit of the causal model of this study, the uniqueness these findings may well be probable for minority young adults living in high HIV prevalence communities only. However, as a contribution to theory-building for developing effective behavioral evidence-informed HIV prevention strategies and public health policies, we recommend that future studies should be conducted on similar minority young adult populations.
Also, given that this study did not examine the effect of co-occurrence of risky sexual behaviors (i.e., combination of alcohol consumption, illicit substance use, and tobacco use) on mental health, we recommend that future studies should examine the predictive influence of co-occurrence of these exogenous constructs on mental health of minority young adults. This line of is important in testing whether the research hypothesis from previous studies that co-occurrence of these risky sexual behavior enhances the adverse effect on mental health holds true for minority young adults [5,126,132-135].
Finally, although this study provides useful insight into the effects of health risk behaviors of young minority adults living in an HIV prevalent community, the units of analysis consisted of a random sample of this population that participated in a short-term (i.e., 6 months) Comprehensive Integrated HIV Prevention program only. Given that previous studies on non-minority young adults found a little or no adverse effect of acute alcohol consumption and tobacco use on mental health, it is recommended that future studies should assess or evaluate the long-term of these health risk behaviors on mental health outcomes of minority young adults who participated in comprehensive integrated HIV prevention programs .impacts using Latent Growth Curve (LGC) model within the framework of structural equation modeling [160-192].
Role of Funding Source
This research was supported by the Substance Abuse and Mental Health Service Administration (grant number SP021335). SMHSA had no role in the study design, collection, and analysis, or interpretation of the data, writing the manuscript, or the decision to submit the paper for publication. The content is solely the responsibility of the authors and does not necessarily represent the official views of the Substance Abuse and Mental Health Service Administration, or the United States Department of Health and Human services, or the United States Government.
References
- Hunt J, Eisenberg D (2010) Mental Health Problems and help-seeking behavior among college students. Journal of Adolescent Health 46(1): 3-10.
- Kitzrow MA (2009) The mental needs of today's college students: Challenges and recommendations. NASPA. Journal 46(4): 646-660.
- Kessler RC, Davis CG, Kendler KS (2005) Childhood adversity and psychiatric disorder in the US National Comorbidity Survey. Psychological Medicine 27(5): 1101-1119.
- Substance Abuse and Mental Health Services Administration (2013) Results from the 2012 National Survey on Drug Use and Health: Summary of National Findings. NSDUH Series H-46, HHS Publication No. (SMA) 13-4795.
- Conway KP, Green VR, Kasza KA, Silveira ML, Borek N, et al. (2018) Co-occurrence of tobacco product use, substance use and mental health problems among youth: Findings from wave 1 (2013-2014) of the population assessment of tobacco and health (PATH) study. Addictive Behavior 76: 208-217.
- Glossary of Terms for Nebraska Behavioral Health System (2006) Mental Health board Training Self-Study.
- Center for Disease Control and Prevention [CDC] 2014. Alcohol use and public health: data, trends, and maps.
- Churchill SA, Farrell (2017) Alcohol and depression: Evidence from the 2014 health survey for England. Drug and Alcohol Dependence 180: 86-92.
- Manninen L, Potkolainen K, Vartiainen E, Laatikainen T (2006) Heavey Drinking occasions and depression. Alcohol 41(3): 293-299.
- Huang R, Ho S, Wang M, Lam T, Lo WS (2016) Reported alcohol drinking and mental health problems in Hong Kong Chinese Adolescents. Drug Alcohol Dependence 164: 47-54.
- Bell S, Britton A (2014) An exploration of the dynamic longitudinal relationship between mental health and alcohol consumption: A prospective cohort Study. BMC Med 3: 12-91.
- Adams RE, Boscarino JA, Galca JA (2006) Alcohol use mental health status and psychological well-being 2 years after World Trade Center attacks in New York City. American Journal of Drug Alcohol Abuse 32(2): 203-224.
- Davidson KM (1995) Diagnosis of alcohol dependence: change in the prevalence of drinking status. British Journal of Psychiatry 166(2): 199-204.
- Brown RA, Monte PM, Myers MG, Martin RA, Rivinus T, et al. (1998) Depression among cocaine abuser in treatment: Relations to cocaine and alcohol use and treatment outcomes. American Journal of Psychiatry 155(2): 220-225.
- Regier DA, Farmer ME, Rae DS, Locke BZ, Keith SJ, et al. (1990) Comorbidity of mental disorders with alcohol and other drug abuse: results from the Epidemiologic Catchment Area (ECA) study. JAMA 264(19): 2511-2518.
- Merikangas KR, Gelernter CS (1990) Comorbidity of alcoholism and depression. Psychiatric Clinic of North America 13(4): 613-632.
- Cranford JA, Eisenberg D, Serra AM (2009) Substance use behaviors, mental health problems, and use of mental health services in a probability sample of college students. Additive Behaviors 34(2): 134-145.
- Hill AK, Hunt J, Welling LLM, Cárdenas RA, Rotella MA (2003) Quantifying the strength and form of sexual selection on men's traits. Evolution and Human Behavior 34(5): 334-341.
- Nooyens AC, van Gelder EMS, Verschuren WM (2005) Smoking and cognitive decline among middle-aged men and women: The Doethnchen Cohort study. American Journal of Public Health 98(12): 2244-2250.
- Otts AK, Dewey ME, Letenneur I, Boonyne C, Copeland JRM, et al. (2004) Effect of smoking on global cognitive function nondementiated elderly. Neurology 65(6): 920-924.
- Rehm J, Room R, Graham K, Monteiro M, Gmel G, et al. (2003) The relationship of average alcohol volume of consumption and paterrn of drinking to burden of disease: n overview. Addiction 98(9): 1209-1228.
- Corrao G, Rubbiati L, Bagnardi V, Zambo A, Poikolainen K (2000) Alcohol and coronary heart disease: a meta-analysis. Addiction 95(10): 1505-1523.
- Costanzo S, Di Castelnuovo A, Donati MB, Iacoviello L, de Geaano G (2010) Alcohol consumption and mortality in patients with cardiovascular disease: a meta-analysis. JACC 55(13): 1339-1347.
- Ronksley PE, Brien SE, Turner BJ, Mukumal KJ, Ghali WA (2011) Association of alcohol consumption with selected cardiovascular disease outcomes: a systematic review and meta-analysis. BMJ 342-d671.
- Howard S, Coleen R Sparkman, Howard G Cohen, Gina Green, Stanislaw H (2004) A comparison of intensive behavior analytic and eclectic treatments for young children with autism. Research in Developmental Disability 26: 359-383.
- Letenneur L (2004) Risk of Dementia and alcohol and wine consumption: a review of recent results. Biological Research 37(2): 189-193.
- Upmark M, Moller J, Romelsjo A (1999) Longitudinal population based-study of self-reported alcohol habits, high levels of sickness absence and disability pension. Journal of Epidemiology Community Health 53(4): 223-229.
- Karlamanla AS, Sarkisian CA, Kado DM, Dedes H, Liao DH, et al. (2009) Light to moderate alcohol consumption and disability: variable benefits by health status. American Journal of Epistemology 169(1): 96-104.
- Skogen C, Tormod B, Ann Kristin Knudsen AK, Hysing M (2013) Psychometric properties and concurrent validity of the CRAFFT among Norwegian adolescents. Ung@hordaland, a population-based study. Addictive Behaviors 38(10): 2500-2505.
- Di Castelnuovo A, Costanzo S, Bagnardi V, Donati MB, Iacoviello L, et al. (2006) Alcohol dosing and total mortality in men and women: an updated meta-analysis of 34 prospective studies. Archive of Internal Medicine 166(22): 2437-2445.
- Klatsky AL, Udaltsova N (2007) Alcohol drinking and total mortality risk. Annals of Epistemology 17(5): S63-S67.
- Fillmore KM, Stockwell T, Chikritzhs T, Bostrom A, Kerr W (2007) Moderate alcohol use and reduced mortality risk: a sysyematic error perspective studies and new hypotheses. Annal of Epidemiology 17(5): S16-S23.
- Grant BF, Hassin DS, Chou SP, Stinson FS, Dawson DA (2004) Nicotine dependence and psychiatric disorder in the United States: Results from the National Epidemiology Survey and related conditions. Archive of General Psychiatry 61(11): 1107-1115.
- Lasser K, Boyd JW, Woolhandler S, Himmelstein DU, McCormick D, et al. (2000) Smoking and mental health illness: a population-based prevalence study. Journal of the American Medical Association 284(20): 2606-2610.
- Colton CW, Manderschheld RW (2006) Congruence in increase mortality rate, years of potential life lost, and causes of death among public mental health clients in eight states. Preventing Chronic Disease 3(2): A42.
- Prochaska JJ, Das S, Young-Wolff KC (2017) Smoking, mental illness, and public health. Annual Review of Public Health 38(1): 165-185.
- Brown-Johnson CG, Cataldo JK, Orozco N, Lisha NE, Hickman NJ, et al. (2015) Validity and reliability of internalized stigma of smoking inventory: An exploration of shame, isolation, and discrimination in smokers with mental health diagnosis: Smoking stigma Scale. The American Journal on Addictions 24(5): 410-418.
- Shroeder SA, Morris CD (2010) Confronting a neglected epidemic: Tobacco cessation for persons with mental illnesses and substance abuse problems: Annual Review of Public Health 31(1): 297-314.
- Kurtz SP, Stall RD, Mance E Buttram, Surratt HL, Chen M (2013) A Randomized Trial of a Behavioral Intervention for High Risk Substance-Using MSM. AIDS Behav 17(9): 2914-2926.
- Oldenburg CE, Amaya G, Perez-Brumer, Biello KB, Landers SJ, et al. (2015) Transactional Sex Among Men Who Have Sex with Men in Latin America: Economic, Sociodemographic, and Psychosocial Factor. American Journal of Public Health’s 105(5): e95-e102.
- Kirst M, Mecredy G, Borland T, Chaiton M (2014) Predictors of substance use among young adults transitioning away from high school: A narrative review. Substance Use and Misuse 49(13): 1795-1807.
- Large MM, Smith G, Sara G, Paton MB, Kedzior KK, et al. (2012) Meta-analysis of self-reported substance use compared with laboratory substance assay in general adult mental health settings. International Journal of Methods in Psychiatric Research 21(2): 134-148.
- Brook D, Brook J, Zhang C, Whiteman M, Cohen P, et al. (2008) Developmental trajectories of cigarette smoking from adolescence to early thirties: Personality and behavioral risk factors. Nicotine and Tobacco Research 10(8): 1283-1291.
- Ferguson CJ, Meehan DC (2011) With friends like these…: peer delinquency influences across age cohorts on smoking, alcohol and illegal substance use. Journal of European Psychiatry 26(1): 6-12.
- Glass K, Flory K (2010) Why does ADHD confer risk for cigarette smoking? A review of psychosocial mechanisms. Clinical Child and Family Psychology Review 13(3): 291-313.
- Goodman I, Peterson Badali M, Henderson J (2011) Understanding substance treatment: The role of social pressure during the transition to adulthood. Addictive Behaviors 36(6): 660-668.
- AbadiMH, Shamblen SR, Thompson K, Collins DA, Johnson K (2011) Influence of risk and protective factors on substance use outcomes across developmental periods: a comparison of youth and young adults. Subst Use Misuse 46(13): 1604-1612.
- Sudhinaraset M, Wigglesworth C, Takeuchi D (2018) Social and cultural contexts of alcohol use: Influences of a Social-Ecological Framework. Alcohol Research Current Reviews 38(1): 35-45.
- March D, Susser E (2006) The eco- in eco-epistemology. International Journal of Epistemology 35(6): 1379-1383.
- Dahlberg LL, Krug EG (2002) Violence: A global public health problem. In: Krug E, Dahlberg LL, Mercy JA, Lozano R (Eds.), World report on violence and health, World Health Organization, Geneva, Switzerland, pp. 1-56.
- Ralph J DiClemente, Laura F Salazar, Richard A Crosby (2007) A review of STD/HIV preventive interventions for adolescents: Sustaining effects using an Ecological approach. J Pediatr Psychol 32(8): 888-906.
- Jessor R (1991) Risk behavior in adolescence: a psychosocial framework for understanding and action. Journal of Adolescence Health 12(8): 597-605.
- Catalano RF, Hawkins JD, Berglund ML, Pollard JA, Arthur MW (2002) Prevention science and positive youth development: competitive or cooperative frameworks? Journal of Adolescent Health 31 (6): 230-239.
- Bronfenbrenner U (1994) Ecological models of human development. International Encyclopedia of human development. (2nd edn), Elsevier, Oxford, United Kingdom, pp. 1643-1647.
- Gruenewald PJ, Millar AB, Treno AJ (1993) Alcohol availability and the ecology of drinking behavior. Alcohol Health & Research World 17(1): 39-45.
- Paul J Gruenewald (2007) The spatial ecology of alcohol problems: Niche theory and assortative drinking. Addiction 102: 870-878.
- R A Scribner, D A Cohen, W Fisher (2000) Evidence of a structural effect of alcohol outlet density: a multilevel alcohol analysis. Alcohol Clin Exp Res 24(2): 188-195.
- Scriber R, Theheal KP, Simonsen N, Robinson W (2010) HIV risk and the alcohol environment: Advancing an ecological epidemiology for HIV/AIDS. Alcohol Res Health 33: 179-183.
- Treno AJ, Grube JW, Martin SE (2003) Alcohol availability as a predictor of youth drinking and driving: A hierarchical analysis of survey and archival data. Alcohol Clin Exp Res 27(5): 835-840.
- Richard A Scribner, Sandy A Johnson, Deborah A Cohen, William Robinson, Thomas A Farley, et al. (2008) Geospatial methods for identification of core groups for HIV/AIDS. Subst Use Misuse 43: 203-221.
- RachdaouI N, Sakar DK (2018) Pathophysiology of the effect of alcohol abuse on the endocrine system. Alcohol Research Current Reviews 38(2): 255-276.
- Stephens MAC, Ward G (2018) Stress and the HPA axis: Role of Glucocorticoids in alcohol dependence. Alcohol Research: Current Reviews 34(4): 460-484.
- Sakar DK, Gibbs DM (1984) Cyclic variation of oxytocin in the blood of pituitary portal vessels of rats. Neuroendocrinology 39(5): 481-483.
- Plosky PM (1991) Pathway to the secretion of adrenocorticotropin: A view from the portal. Journal of Neuroendocrinology 3(1): 1-9.
- Jenkins JS, Connolly J (1968) Adrenocortical response to ethanol in man. British Medical Journal 2(5608): 804-805.
- Uhart M, Oswald M, McCaul ME, Chong R, Wand GS (2006) Hormonal response to psychological stress and family history of alcoholism, Neuropsychopharmacology 31(10): 2255-2263.
- Zimmermann U, Spring K, Kunz-Ebrecht SR, Uhr M, Wittchen HU (2004) Effect of ethanol on hypothalamic-pituitary-adrenal system response to psychosocial stress in sons of alcohol-dependent fathers. Neuropsychopharmacology 29(6): 1156-1165.
- Elie G Aoun, Mary R Lee, Carolina L Haass Koffler, Robert M Swift, Giovanni Addolorato, et al. (2015) Relationship between the thyroid axis and alcohol craving. Alcohol Alcohol 50(1): 24-29.
- Eve Van Cauter, Federica Latta, Arlet Nedeltcheva, Karine Spiegel, Rachel Leproult, et al. (2004) Reciprocal interaction between GH axis and sleep. Growth Horm IGF Res14(Suppl A): S10-S17.
- De Marinis L, Mancini A, Fiumara C, Conte G, Iacona T, et al. (1993) Growth hormone response to growth-hormone releasing hormone in early abstinence alcoholic patients. Psychoneuroendocrinology 18(7) 475-483.
- Land WE (1999) Alcohol, slow wave sleep, and somatotropic axis. Alcohol 18(2-3): 109-122.
- Valimaki M, Pelknen R, Harkonen M, Ylikahri R (1984) Hormonal changes in noncirrhotic male alcoholics during ethanol withdrawal. Alcohol and Alcoholism 19(3): 235-242.
- Coiro V, Vescovi PP (1995) Alcoholism abolishes the growth hormone response to sumatriptan administration in man. Metabolism 44(12): 1577-1580.
- Coiri V, Vescovi PP (1998) Alcoholism abolishes the effects of melatonin on growth hormone secretion in humans. Neuropeptides 32(3): 211-214.
- Moller N, Jorgensen JO (2009) Effects of growth hormone on glucose, lipids, and protein metabolism in human subjects. Endocrine Reviews 30(2): 152-177.
- Ross HE, Young LJ (2009) Oxytocin and the neural mechanisms regulating cognitive and affiliative behavior. Front Neuroendocrinol 30(4): 534-547.
- Insel TR (2010) The challenge in translation in social neuroscience: A review of oxytocin, vasopressin, and affiliative behavior. Neuron 65(6): 768-779.
- Iovino M, Guastamacchia E, Giagulli VA, Licchelli B, Triggiani V, et al. (2012) Vasoprissin secretion control: Central neural pathways, neurotransmitters and effect on drugs. Current Pharmaceutical Design 18(30): 4714-4724.
- McGregor IS, Bowen (2012) Breaking the loop: Oxytocin as a potential treatment for drug addiction. Horm Behav 61(3): 331-333.
- de Wied D, Diamant M, Fodor M (1993) Central nervous system effects on the neurohypophyseal hormone and related peptides. Forntiers in Neuroimmunoassay 14(4): 251-302.
- Stoop R (2014) Neuromodulation by oxytocin and vasopressin in the central nervous system as abasis for their rapid behavioral effects. Current Opinion in Neurobiology 29: 187-193.
- Varlinskaya EI, Spear LP (2004) Differences in social consequences of ethanol emerge during the course of adolscene in rats: Social facilitation, social inhibition, an oxiolysis. Developmental Psychology 48(2): 148-161.
- Thayer JF, Hall M, Soller JJ, Fischer JE (2006) Alcohol use, urinary cortisol, and heart rate variability in apparently healthy men: Evidence for impaired inhibitory control of the HPA axis in heavy drinkers. Internal Journal of Psychophysiology 59(3): 244-250.
- Upadddhyaya, HP, Rose K, Wang W, O Rourke K, Sullivan B (2005) Attention-deficit/hyperactivity disorder, medication treatment, and substance use among adolescents and young adults. Journal of Child and Adolescent Psychopharmacology 15(5): 799-809.
- Mason W, Windle M (2001) Family, Religious, peer influences on adolescence alcohol use: A longitudinal study. J Stud Alcohol 62(1): 44-53.
- Lynn M Oswald, Dean F Wong, Mary McCaul, Yun Zhou, Hiroto Kuwabara, et al. (2005) Relationship between ventrl striatal dopamine release, cortisol secretion, and subjective responses to amphetamine. Neuropsychopharmacology 30(4): 821-832.
- Koob GLA (2008) A role for brain stress system in addition. Neuron 59(1): 11-34.
- Myers B, McKlveen JM, Herman JP (2012) Neural regulation of stress response: The many faces of feedback. Cellular and Molecular Neurobiology 32(5): 683-694.
- Herman JP (2018) Neural pathways of stress integration: Relevance to Alcohol Abuse. Alcohol Res 34(4): 441-447.
- Verbalis JG (1993) Osmotic inhibition of neurohypophysial secretion. Annals of the New York Academy of Sciences 689: 146-160.
- Doring DK, Herzenstiel MN, Kample H, Jahn H, Pralle L, et al. (2003) Persostent alteration of vasopressin and N-terminal proatrial ntruiretic peptide [Plasma level in long-term abstinent alcoholics. Alcoholism Clinical and Experimental Research 27(5): 849-861.
- Ehrenreich H, Tom Dereck K, Gefeller O (1997) Sustained elevation of vasopressin plasma level in healthy young men., but not in abstinent alcoholics, upon expectation of novelty. Psychoneuroendocrinology 22(1) 13-24.
- Laczi F, Laszlo FA, Kovacs GL, Telegdy G, Szász A, et al. (1987) Differential effect of desglycinamide9-(Arg8)-vasopressin on cognitive functions of diabetes insipidus and alcoholic patients. Acta Endocrinol (Copenh) 115(3): 392-398.
- Buijs RM, De Vries GJ, Van Leeuven FW, Swaab DF (1983) Vasopressin and oxytocin: Distribution and putative functions of the brain. Progress in Brain Research 60: 115-122.
- DD Rasmussen, BM Boldt, CA Bryant, DR Mitton, SA Larsen, et al. (2000). Chronic daily ethanol and withdrawal: 1. Long Term changes in the hypothalamic-pituitary-adrenal axis. Alcohol Clin Exp Res 24(12): 1836-1849.
- Rivier C, Lee S (1996) Acute alcohol administration stimulates the activity of Hypothalamic-pituitary axis that express corticotropin-releasing factor and vasopressin. Brain Res 726(1-2): 1-10.
- King A, Munisamy G, de Witt H, Lin S (2006) Attenuated cortisol response to alcohol in heavy social drinkers. Int J Psychophysiol 59(3): 203-209.
- Prestage G, Jin F, Bavinton B, Hurley M (2004) Sex workers and their clients among Australian gay and bisexual men. AIDS Behavior. 18(7): 1293-1301.
- Wu CYYS, Wu JF, Lee SY, Huang L, Yu HC, et al. (2008) The association between DRD2/ANKK1, 5_HTTLPR gene, and specific personality trait on antisocial alcoholism among Han Chinese in Taiwan, American Journal of Medical Genet B Neuropsychiatry Genet 147B(4): 447-453.
- Bellos S, Skapinakis P, Rai D, Zitko P, Araya R, et al. (2013) Cross-cultural patterns of the association between varying levels of alcohol consumption and the common mental disorders of depression and anxiety: secondary analysis of the WHO Collaborative Study on Psychological Problems in General Health Care. Drug Alcohol Dependence 133(3): 825-831.
- (2013) Royal College of Physicians, Royal College of Psychiatrists. Smoking and mental health: Royal College of Psychiatrists Council Report CR178. RCP, London, United Kingdom.
- Matta SG, Beyer HS, McAllen KM, Sharp BM (1987) Nicotine elevates rat plasma ACTH by a central mechanism. Journal of Pharmacology Experiment & Theory 243(1): 217-226.
- Paolini M, De Biasi M (2011) Mechanistic insights into nicotine withdrawal. Biochemical Pharmacology 82(8): 996-1007.
- Daban C, Vieta E, Mackin P, Young AH (2005) Hypothalamic-pituitary-adrenal axis and bipolar disorder. The Psychiatric clinics of North America 28 (2): 469-480.
- Pariante C, Lightman S (2008) The HPA axis in major depression: classical theories and new developments Trends in Neurosciences 31(9): 464-468.
- Non-AL, Binder AM, Barault L, Rancourt RC, Kubzansky LD, et al. (2012) DNA methylation of stress-related genes and LINE-1 repetitive elements across the healthy human placenta. Placenta 33(3): 183-187.
- Oberlander TF, Weinberg J, Papsdorf M, Grunau R, Misri S, et al. (2008) Prenatal exposure to maternal depression, neonatal methylation of human glucocorticoid receptor gene (NR3C1) and infant cortisol stress responses. Epigenetics 3(2): 97-106.
- Perroud N, Dayer A, Piguet C, Nallet A, Favre S, et al. (2014) Childhood maltreatment and methylation of glucorticoid receptor gene NR3C1 in bipolar disorder. British Journal of Psychiatry 204(1): 30-35.
- Lechner WV, Janssen T, Kahler CW, Audrian-McGovern j, Leventhal AM (2007) Bi-directional associations of electronic and combustible cigarette use onset pattern with depressive symptoms in adolescents. Preventive Medicine 96: 73-78.
- Leventhal AM, Strong DR, Sussman S, Kirkpatrick MG, Unger JB, et al. (2015) Psychiatric comorbidity in adolescent electronic and conventional cigarette use. Journal of Psychiatric Research 73: 71-78.
- Mistry R, Babu GR, Mhapatra T, McCarthy WJ (2014) Cognitive Mediators and disparities in the relation between teen depressiveness and smoking. Drug and alcohol Dependence 140: 56-62.
- Vidrine DJ, Arduino RC, Gritz ER (2007) The effects of smoking abstinence on symptom burden and quality of life among persons living with HIV/AIDS. Aids Patient Care Standards. AIDS Patient Care STDS 21(9): 659-666.
- Tercyak KP, Audrain J (2002) Psychosocial correlates of alternate tobacco product use during early adolescence. Preventive Medicine 35(2): 193-198.
- Kwan MY, Arbour-Nicitopoulos KP, Duku E, Faulkner G (2016) Patterns of multiple risk behaviors in university students and their association with mental health: Application of latent class analysis. Health Promotion Chronic Disease Prevention 36(8): 168-170.
- Pelletier JE, Lytle LA, Laska MN (2016) Stress, Health Risk behaviors, and weight status among Community College Students. Health Education & Behavior 43(2): 139-144.
- Marmorstein NP, White H, Chung T, Hipwell A, Stouthamer-Locker M (2010) Association between first use of substances and change in internalizing symptom among girls: differences by symptom trajectory and substance use type. J Clin Child Adolesc Psychol 39(4): 545-558.
- Zehe JM, colder CR, Read JP, Wieczorek WF, Lengua L (2013) Mental health and cigarette use in early adolescence: The moderating role of perceived peer norms. Additive Behaviors 38(4): 1931-1939.
- Armstrong TD, Costello EJ (2002) Community Studies on Adolescent Substance Use, Abuse, or Dependence and Psychiatric Co-morbidity. J Consult Clin Psychol 70(6): 1224-1239.
- National Center for Chronic Disease Prevention and Health Promotion (US) Office of Smoking and Health (2012) Prevention tobacco use among youth and young adults: A report of the surgeon general, 3, The Epidemiology of tobacco use among people in the United States and worldwide. Atlanta (GA): Center for Disease Control and Prevention (US).
- Irene J Elkins 1, Matt McGue, William G Iacono (2007) Prospective effect of attention-deficit/hyperactivity disorder, conduct disorder, and sex on adolescent substance use and abuse. Arch Gen Psychiatry, 64(10): 1145-1152.
- Lee SS, Humphreys KL, Flory K, Liu R, Glass K (2001) Prospective association of childhood attention-deficit/hyperactivity disorder (ADHD) a substance use and abuse/dependence: A meta-analytic review. Clin Psychol Rev 31(3): 328-341.
- Lovell ME, Bruno R, Johnson A, Matthew A, McGregor I, et al. (2018) Cognitive, physical, and mental health outcomes between long-term cannabis and tobacco users. Addictive Behaviors 79: 178-188.
- Meier MH, Avshalo C, Amblere A, Harrington H, Houts R, et al. (2012) Persistent cannabis users show neuropsychological decline from childhood to midlife. Proceedings of the National Academy of Science of the United State. 109(40): E2657-E2664.
- Schuster RM, Crane NA, Mermelstein R, Gonzalez R (2012) The influence of inhibitory control and episodic memory on the risky sexual behavior of young adult cannabis users. J Int Neuropsychol Soc 18(5): 827-833.
- McHale S, Hunt N (2008) Executive function deficits in short‐term abstinent cannabis users. Human Psychopharmacology: Clinical and Experimentation Research 23(5): 409-415.
- Substance Abuse and Mental Health Services Administration (SAMHSA). (2009). Results from the 2008 National Survey on Drug Use and Health: National Findings (NSDUH Series H-36, HHS Publication No. SMA 09-4434). Rockville, MD: Author.
- Linda Richter, Brandie S Pugh, Philip H Smith, Samuel A Ball (2017) Co-Occurrence of nicotine and other substance use and addiction among youths and adults in the United States: Implication for research, practice and policy. American Journal of Drug and Alcohol Abuse 43: 132-145.
- Brenner ND, Collins JL (1998) Co-occurrence health risk behaviors among adolescents in the United States. Journal of Adolescence Health 22(3): 209-213.
- Topolski TD, Patyrick DL, Edwards TC, Huebner CE, Connell FA, et al. (2001) Quality of life and health-risks behaviors among adolescents. Journal of adolescence Health 29(6): 426-435.
- Jackson C, Geddes R, Haw S, Frank J (2012) Intervention to prevent substance use and risky behavior in young people: a systematic review. Addiction 107(4): 733-747.
- Orlando M, Tucker PL, Ellickson JS, Klein DJ (2005) Concurrent use of alcohol and cigarettes from adolescence to young adulthood: an examination of developmental trajectories and outcomes. Substance Use Misuse 40(8): 1051-1069.
- Chen K, Kandel DB (1995) The Natural History of Drug Use from Adolescence to the Mid-Thirties in a General Population Sample. Am J Public Health 85(1): 41-47.
- Kandel DB, Logan JA (1984) Patterns of drug-use from adolescence to young adulthood: 1. Periods of risk for initiation, continued use, and discontinuation. Am J Public Health 74(7): 660-666.
- Yamaguchi K, Kandel DB (1984) Patterns of drug-use from adolescence to young adulthood. Predictors of progression. Am J Public Health 74: 673-681.
- Andrea C Villanti, Gary A Giovino, Dianne C Barker, Paul D Mowery, Varadan Sevilimedu, et al. (2012) Menthol brand switching among adolescents and young adults in the National Youth Smoking Cessation Survey. Am J Public Health 102(7): 1310-1312.
- Cohen L, Manion L, Morrison K (2018) Research Methods in Education. Routledge Taylor & Francis Group, London, United Kingdom.
- Isaac L, Michael WB (2014) Handbook in Research and Evaluation. EdIT Publisher, San Diego, United Sates.
- McNabb DE (2018) Research Methods in Public Administration and Non-Profit Management quantitative and qualitative approaches. (4th edn), Armonk, USA.
- Arbuckle JL (2007) Amos 17.0 User’s Guide. AMOS Development Corporation, Crawford United State.
- Hans-Vaughn DL (2017) Applied Multivariate Statistical Concepts. (1st edn), Routledge, USA, pp. 1-662.
- Hair JF, Black WC, Babin BJ, Anderson RE, Tatham RL (2006) Multivariate Data Analysis. (2nd edn), Pearson Education Limited, United Kingdom, pp. 1-739.
- Hu L, Bentler PM (1999) Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling 6(1): 1-55.
- Blunch NJ (2010) Introduction to Structural Equation Modeling Using SPSS and AMOS. Los Thousand Oaks, CA: Sage Publications, California, United States.
- Brown TA (2006) Confirmatory Factor Analysis for Applied Research. Guilford Press, New York, United States.
- Akaike H (1987) Factor analysis and AIC. Psychometrika 52: 317-332.
- Bozdogan H (1987) Model selection and Akaike’s information criteria (AIC): The general theory and its analytic extensions. Psychometrika 52: 345-370.
- Hoelter JW (1983) The analysis of covariance structure with incomplete data: A developmental perspective. In: Little TD, Bovaird JA, Card NA (eds.) Modeling contextual effects in longitudinal studies, pp. 13-32.
- Hu L, Bentler PM (1995) Evaluating model fit. In: Hoyle RH (Ed.), Structural equation modeling: concept, issues, and applications. Sage, United Kingdom, pp. 79-99.
- Mardia KV (1970) Measure of multivariate skewness and kurtosis with applications. Bikometrika 57(3): 519-530
- Mardia KV (1974) Application of some measures of multivariate skewness and kurtosis in testing normality and robustness studies. Sankhya 36(2): 115-128.
- Mertler CA, Reinhart RV (2017) Advanced and Multivariate Statistical Methods: Practical Application and Interpretation. (6th Edtn), Routledge, USA, pp. 1-374.
- Keith T (2006) Multiple Regression and Beyond. In: (2nd edn), Boston MA, USA.
- Carver S (1978) The case against significance testing. Harvard Education Review 48(3): 378-399.
- Falk R, Greenbaum CW (1995) Significance tests die hard: the amazing persistence of a probabilistic misconception. Theory & Psychology 5(1):75-98.
- Ziliak ST, McCloskey DN (2008) The cult of statistical significance. Michigan University Press, An Arbor, Michigan, United States.
- Gorard S (2016) Damaging real lives through obstinacy: Re-emphasizing why significance testing is wrong. Sociological Research Review Online 21(1): 102-115.
- Cohen J (1994) The earth is round (p<0.05). American Psychologist, 49(12): 9917-1003.
- Ellis PD (2010) The Essential Guide to Effect Size. Cambridge: Cambridge University Press, United Kingdom.
- Dausey DJ, Desai RA (2002) Psychiatric comorbidity and the prevalence of HIV infection in a sample of patients in treatment for substance abuse. The Journal of Nervous and Mental Disease 191(1): 10-17.
- Bandeira FC, Loukas AV, & Perry CL (2016) Association between tobacco and nicotine use and depression symptoms among college students in Texas. Addictive Behaviors 63: 19-22.
- Blasé SL, Gilbert AN, Anastopoulos AD, Costello EJ, Hoyle RH, et al. (2009) Self-reported ADHD an adjustment in college: Cross-sectional and longitudinal findings. Journal of Attention Disorders 13(3): 297-309.
- Boden JM, Fergusson DM (2011) Alcohol and depression. Addition 106: 906-914.
- Bridges S Gill V, Omolo T, Sutton R, Wight V (2011) Smoking, drinking and drug use among young people in England in 2010. National Center for Social Research and National Foundation for Educational Research. London, United Kingdom.
- Brooks PJ, Enoch MA, Goldman D, Li TK, Yokoyama A (2009) The alcohol flushing response: An unrecognized risk factor for esophageal cancer from alcohol consumption 6(3): e50.
- Brown R, Lewinson P, Seeley J, Wagner S (1996) Cigarette smoking, major depression and other psychiatric disorder among adolescents. Journal of the American Academy of Child and Adolescents Psychiatry 32(12): 1602-1610.
- Byrne BM (2010) Structural equation modeling with AMOS: Basic concept, applications, and programming. (2nd edn), Routledge, Taylor & Francis Group, New York, United States.
- Calhoun HM, Song W, Poulier NR (1998) Blood pressure screening, management and control in England: Results from the health survey for England. Journal of Hypertension 16(6): 747-752.
- Carer A, Obremski Brandon K, Goldman M (2010) The college and noncollege experience: A review of the factors that influence behavior among young adults. Journal of Studies on alcohol and Drugs 71: 745-750.
- Center for Disease control and Prevention [CDC] (2013) Youth risk behavior surveillance system-United States. Morbidity and Mortality Weekly Report 63(4): 1-168.
- Cote J, Arnett J, Tanner J (2006) Emerging Adulthood as an Institutional Moratorium: Risk and Benefits to Identity Formation. American Psychological Association, Washington DC, United States.
- Crowley R, Kirschner N, Dunn AS, Bornstein SS (2017) Committee of American College of Physicians. Health and public policy to facilitate effective prevention and treatment of substance use disorder involving illicit and prescription drug: an American College of Physicians position paper. Annals of Internal Medicine 166(10): 733-736.
- Gerbie, Cheryl G Davis, Tsegaye Habtemariam, Berhanu Tameru, David Nganwa, et al. (2011) The association between substance use and risky sexual behaviors among middle school children. Journal of Substance Use 16(5): 339-347.
- Sherryl H Goodman, Matthew H Rouse, Arin M Connell, Michelle Robbins Broth, Christine M Hall, et al. (2011) Maternal Depression and Child Psychopathology: A Meta-Analytic Review. Clin Child Fam Psychol Rev 14(1): 1-27.
- Guilamo-Ramos V, Litardo HA, Jacard J (2005) Prevention program for reducing a problem behavior in adolescence: implication of the co-occurrence of problem behavior in adolescence. Adolescence Health 36(1): 82-86.
- Gomez-Fraguela JJ Luengo MA, Romero E (2003) Drug-abuse Prevention in the school: four-years follow-up of a programme. Psychology Spain 7(1): 29-38.
- Grossman JB, Tierney JP (1998) An impact study of Big Brother Big Sister program. Evaluation Review 22(3): 403-426.
- Hall J, Valente T (2009) Adolescent smoking networks: The effect of influence and selection on future smoking. Addict Behav 32(12): 3054-3059.
- Hammond D (2005) Smoking behavior among young adults: Beyond youth prevention. Tobacco Control 14(3): 181-185.
- (2010) The science of adolescence risk-taking. Institute of Medicine Committee on the Science of Adolescence Health. workshop Summary. National Academies of Press, Washington DC, United States p.1-4.
- Kenny SR, Di Guiseppi GT, Meisel MK, Balestrieri SG, Barnett NP (2018) Poor metal health, peer drinking norms, and alcohol risk in a social network of first-year college students. Additive Behaviors 84: 1651-1659.
- Lai HM, Cleary M, Sitharthan T, Hunt GE (2015) Prevalence of comorbid substance use, anxiety and mood disorders in epidemiological surveys. Drug and alcohol dependence 1(154): 1-13.
- Lenz BK (2004) Tobacco, depression, and lifestyle choices in the pivotal early college years. Journal of American College Health 52(5): 213-219.
- Kaley MacFadyen, Rebecca Loveless, Brandon DeLucca, Krystal Wardley, Sumeet Deogan, et al. (2016) Peripheral oxytocin administration reduce ethanol consumption in rat. Pharmacol Biochem Behav 140: 27-32.
- Nachmias CF, Nachmias D (2008) Research methods in the social sciences. Worth Publishing, New York, USA.
- Malley SS, Krishnan-Sarin S, Farren C, Sinha R, Kreek MJ (2002) Naltrexone decreases as alcohol self-administration in alcohol-dependent subjects and activates the hypothalamic-pituitary-adrenocortical axis. Psychopharmacology (Berlin) 160(1): 19-29.
- Pudney S (2003) The road to ruin? Sequences of initiation of drug use and crime in Brit. Economics Journal 113(486): C183-C198.
- Jens Christoffer Skogen, Ann Kristin Knudsen, Arnstein Mykletun, Sverre Nesvåg, Simon Overland (2012) Alcohol consumption, problem drinking, abstention and disability pension award. The Nord-Torndelag Health Study. Addiction 107(1): 98-108.
- Szatkowski L, McNeill A (2015) Divergent trends in smoking behaviors according to mental health status. Nicotine Tobacco Research 17(3): 356-360.
- Timko C, Ilgen M, Haverfield M, Shelley A, Breland JS (2017) Polysubstance use by psychiatry inpatients with co-occurring mental health and substance use disorders. Drug and Alcohol Dependence 180: 319-322.
- Upaddhyaya HP, Carpenter HJ (2008) Is attention deficit disorder (ADHD) symptom severity associated with tobacco use? American Journal of Additions 17(3): 195-198.
- Wynne O, Sarkar DK (2013) Stress and neuroendocrine-immune interaction: A therapeutic role for B-endorphin. In: Kusnecov A, Anisman H (Eds.), The Wiley-Blackwell Handbook of Psychoneuroimmunology. Wiley-Blackwell, Oxford, United Kingdom pp. 198-211.
- Yegidis BL, Weinbach RW, Myers LL (2018) Research Methods for Social Workers, Pearson Publishers, New York, United States.






























