Abstract
Background: Pain after severe injuries is a well-known problem and a current topic during the so-called opioid epidemic. Open tibial fractures are associated with complications as osteomyelitis, soft tissue problems, amputations and chronic pain. The primary aim of this study was to determine risk factors for prolonged use of opioids among these patients, including consumption of opioids, benzodiazepines and antidepressants prior to the injury.
Methods: We performed a nationwide study based on Swedish national registers. We searched for all patients admitted due to an open
tibial fracture during 2007-2019. We cross-checked data with the National Register of Pharmaceuticals to determine the consumption of
pharmaceuticals related to psychiatric disorders. Logistic regression analysis was used to determine risk factors for opioid use at 24 months
after the injury. We included sex, age, injury severity and consumption of pharmaceuticals before the injury as variables.
Results: Out of the study population (3, 460 patients), 10 % had a dispatched opioid drug during three months before the injury. In adjusted
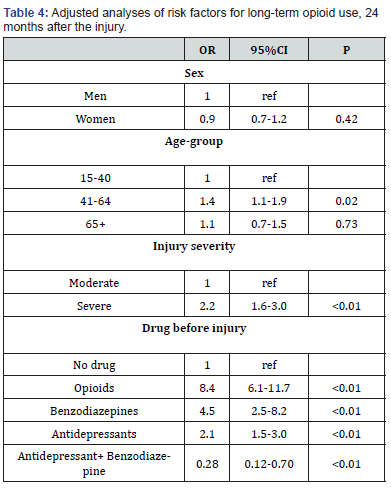
analysis, we found that a dispatched drug of opioids (OR 8.4, 95% CI 6.1-11.7), benzodiazepines (OR 4.5, 95% CI 2.5-8.2) or antidepressants (OR
2.1, CI 1.5-3.0) before the injury were associated with consumption of opioids at 24 months after the injury. Further risk factors were severe
injuries complicated by amputation and/or reconstructive surgery (OR 2.2, 95% CI 1.6-3.0), and age-group 41-64 years (OR 1.4, 95% CI 1.1-1.9).
Conclusion: Consumption of pharmaceuticals related to psychiatric disorders is more common among patients with open tibial fractures
compared with the total population. Pre-injury dispatched pharmaceuticals with ATC-codes representing opioids, benzodiazepines or
antidepressants are significant risk factors for opioid use at 24 months after the occurrence of an open tibial fracture. Pre-injury consumption of
pharmaceuticals should be considered when prescribing and de-escalating opioids after injury.
Keywords:Open Tibia Fracture; Opioid Use, Analgesic Consumption, Opioid Dependent Risk, Pain, Trauma
Abbreviations:SNPR: Swedish National Patient Register; SPDR: Swedish Prescribed Drug Register; ATC: Anatomical Therapeutic Chemical
Introduction
Open tibial fractures are associated with complications like infection, osteomyelitis, compartment syndrome, soft tissue problems, multiple surgeries, increased length of stay, repeated hospitalization and even amputations. Patients with open tibial fractures are heterogeneous, both the younger population of men that are exposed to high energy injuries and self-destructive behaviour as well the elderly and frail, prone to simple falls. Acute and chronic pain are well-known major problems for patients that have undergone orthopaedic surgery. Half of these patients report persistent pain after 3 months [1]. In recent years, a lot of attention has been given to overconsumption of opioid prescription for acute and chronic pain. Long-term opioid use has negative effects on different organ systems [2]. Several studies have been published on the topic of opioid consumption after fractures [3-7].
To our knowledge, there are no publication on the extent of opioid use after open tibial fractures, or risk factors for prolonged consumption. In Sweden, there are several national healthcare registers with a high coverage, thus suitable for population-based research [8]. The Swedish National Patient Register (SNPR) with a coverage of 98 % registers all admissions to Swedish hospitals. In a recent diagnosis validation study, the positive predictive value of the diagnosis open tibial fracture was high (87%) [9]. All pharmaceuticals, prescribed and dispatched, are registered in the Swedish Prescribed Drug Register [10,11]. The primary aim of this register study was to analyse the use of opioids before and after the occurrence of an open tibial fracture, and to examine the association with consumption of pharmaceuticals for psychiatric disorders. Secondary aims were to define populations at risk for prolonged use of opioid, and to define factors associated with long-term use.
Materials and Methods
Registers
For this study, we used three national registers, all held by the National Board of Health and Welfare. The Swedish National Patient Register (SNPR) has a coverage of 98%, and includes all patients admitted to Swedish hospitals. Available data are i.e. basic demographic information, main diagnoses, additional diagnoses and surgical procedures. The Swedish Prescribed Drug Register (SPDR) was started in 2005 and comprises individual data on all prescribed drugs that are dispensed from Swedish Pharmacies. All pharmaceuticals are grouped according to the Anatomical Therapeutic Chemical (ATC) Classification. The Cause of Death Register includes data on all deaths in Sweden since 1961, including underlying cause of death and date of death.
Population
We extracted data from the SNPR for all patients (aged 15 years and older) that were admitted to Swedish hospitals with the diagnosis open tibial fractures during 2007-2019. The ICD codes for fracture of the proximal part, the tibial shaft and the distal part of the tibia were searched for (S82.11, S82.21 and S82.31). No exclusions were made. All individuals were characterized with sex and age as basic demographic variables. For this population, we extracted data on pharmaceuticals from the SPDR during 2006-2019. Hence, for each individual, data from prescribed and dispatched pharmaceuticals were collected from one year before the fracture until two years after the fracture. The population was cross-referenced with the Causes of Death Register, to identify patients that died during the study period and to get a correct estimation of opioid use in the population. We chose to define the patients´ injuries as severe or moderate. Severe injuries were when patients had major complications, defined as a coded procedure for amputation and/or reconstructive surgery (flap). For this selection, the following procedures and corresponding codes were selected from the SNPR: above-knee amputation (NFQ19), knee disarticulation (NGQ09), below-knee amputation (NGQ19), pedicled flap (ZZS), free flap (ZZQ) and skin graft (ZZA).
Pharmaceuticals included
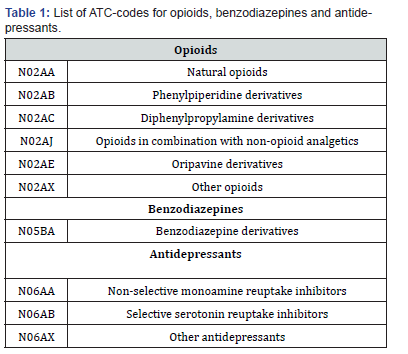
For this study we included the following drugs that were divided into 3 groups: opioids (“strong” as well as “weak” opioids), benzodiazepines and antidepressants. We chose these pharmaceuticals as indicators of psychiatric disorders, i.e. depression, anxiety or drug dependence. All drugs in this study were prescribed and not available over the counter. ATC-codes for all selected drugs are shown in Table 1. Data from the SPDR include the name of the drug, the date for the prescription, the drug strength, the prescribed amount, the dosage and the date of dispatch. Only drugs that were actually dispatched, were taken into account for our analysis. For all patients, we assessed any prescribed and dispatched drugs with the above ATC-codes during 3 months before the injury.
For further analysis, we evaluated the prescription of opioids at 6, 12 and 24 months after the injury. Dispatch or no dispatch of a prescription within 3 months, was regarded as a dichotomous variable. Patients that died during the respective time period were excluded. We chose the following variables for risk factor analysis: sex, age, moderate or severe injury, previous dispatch of pharmaceuticals from one or more groups of drugs, during a 3-month period before the injury. The pharmaceuticals were grouped as opioids, benzodiazepines or anti-depressants. We defined 3 age groups: 15-40 years, 41-64 years and 65 years or older. We defined the patients that were still taking opioids at 6, 12 or 24 months after the injury. We described these patients regarding age, sex, severe or moderate injury and we analysed their intake of prescribed drugs before the injury.
Statistics
Logistic regression analysis was used to evaluate associated factors for the dispatch of opioids at 6, 12 and 24 months after the injury. Dispatch or no dispatch during the last 3 months was regarded as a dichotomous variable. The crude results were adjusted for age, sex, serious injury/moderate injury and dispatched drugs during 3 months before the injury. Combinations of dispatched drugs as risk factors were analysed with stepwise logistic regression, where non-significant results were excluded.
Ethics
This study was approved of by the National Board of Ethics in Stockholm (2008/266-31/3, 2009/837-31/32011/1280-32, 2014/1641-31, 2018/992-32, 2020-02950,)
Results
Characteristics of the study population
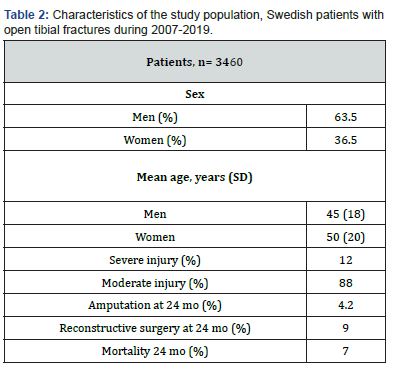
We identified 3,460 patients that sustained an open tibial fracture during 2007-2019, (67% males). Out of these patients, 12% had a severe injury that required amputation and/or reconstructive surgical procedures, at a follow-up time of 24 months (Table 2). Out of the study population, 146 (4%) were amputated during the study period and 313 (9%) had a flap or a skin graft. Mortality at 12 months was 5% and at 24 months 7%.
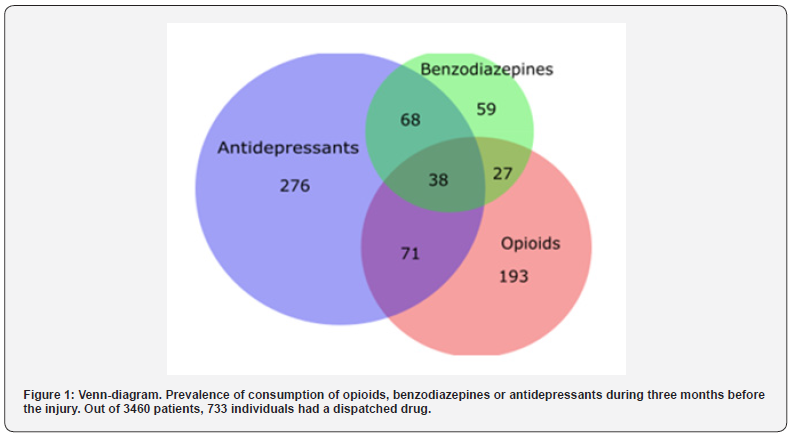
Prevalence of drug consumption
The subgroup that had one or more dispatched drug during 3 months before the injury consisted of 733 patients. Opioids were consumed by 332 patients, which is 10 % of the study population. Benzodiazepines were consumed by 192 (6 %) and antidepressants by 455 (13 %) patients. The consumption of different drug combinations in shown in (Figure 1). After the injury, the opioid use increased to 22% of the population at 6 months after the injury. At 24 months, the opioid use decreased to 10%, which was the same proportion as before the injury.
Characteristics of the opioid-consuming population
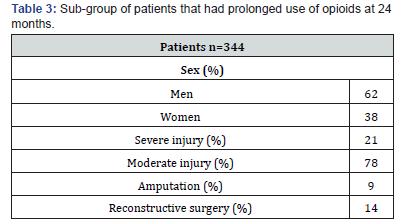
The sub-populations of patients (344) that used opioids after 6, 12, 18 and 24 months were characterized (Table 3). This subgroup had more complications than the total study population, exemplified by 9% who were amputated and 14% who had performed reconstructive surgery at 24 months.
Risk factors for prolonged use of opioids
Risk factors for opioid use at 6, 12 or 24 months after the injury did not mainly differ. The use of drugs in all different combinations shown in Figure 1 was analysed by stepwise logistic regression. Significant risk factors were for opioids, benzodiazepines and antidepressants, whereas combinations did not add extra risk. Other significant risk factors were age-group 41-64 years and severe injury. The combination benzodiazepines and antidepressants showed a decrease of risk. Results from the logistic regression at 24 months are shown in Table 4. After 6 months, the risk for opioid use was increased for both oldest age groups.
Discussion
In this study, we found that prior use of pharmaceuticals for psychiatric disorders was a significant risk factor for prolonged opioid consumption after an open tibial fracture. Additionally, we found that patients in the study population had a higher prevalence of dispatched drugs of all 3 pharmaceutical groups (opioids, benzodiazepines and antidepressants) compared with the total Swedish population. In our study group, 10% had a dispatched opioid, 6% had a benzodiazepine and 13% had an antidepressant during a 3-month period before the injury. According to statistics from the National Board of Health and Welfare for the year 2015 [11] retrieved from https://www.socialstyrelsen.se/statistik-ochdata/ statistik/statistikamnen/lakemedel/), 9% of the Swedish population had a dispatched opioid drug during the entire year. Corresponding numbers for benzodiazepines were 4% and for antidepressants 11%.
The trauma population consists most of men. Women, on the other hand, consume more pharmaceuticals compared to men. In Sweden, women consume more prescribed drugs from all ATC groups used in our study.
Our findings that the consumption of opioids, benzodiazepines and antidepressants are risk factors for prolong use of opioids are supported by the literature. In a study by Sabesan et al, patients with opioids had an 8-fold increased risk for post-operative use after reverse shoulder-arthroplasty, regardless of the underlying diagnosis [7]. Sun et al found in a study of over 600,000 patients, that drug dependency, depression, use of anti-depressants and benzodiazepines was associated with chronic use of opioids after surgery [12]. The combination of antidepressants and benzodiazepines showed a decreased risk for opioid consumption. This is potentially a different group of patients and further explanation would include analysis of their charts. Patients with severe injuries as indicated by amputations or reconstructive surgery are at risk for pro-longed use of opioids. This could be explained by multiple surgeries, increased length of stay, slower healing of the injury and often high energy trauma.
In our study, patients in the age group 41-64 had an increased risk for long term use compared with both the younger (15-40 years) and the elderly (65 years and older). We don’t know the specific reason for the higher consumption among middle-aged individuals, but it should be considered during prescription and de-escalation. Patients with open tibial fractures are part of a heterogeneous population. The sub-group with prolonged opioid use are at risk for adverse effects, where drug dependence is only one. In this study, we show that many of these individuals can be recognized already at admission. Also, we found that risk factors for prolonged use were highly consistent through the timeperiod from 6 to 24 months. Consumption of pharmaceuticals related to psychiatric disorders and opioids is a significant risk factor for long-term use of opioids. In the LEAP (Lower extremity assessment study) study, they found that psychological distress after open tibial fractures was high, and that psycho-social and mental health support was low [13].
Many studies have shown the association between psychological factors like deficient coping-skills and perceived pain. Catastrophic thinking, low self-efficacy and depression have been linked to increased pain, and opioid use has been linked to increased experience of pain and request for opioids [14-17]. In a study by Finger [6] the authors found that higher opioid intake was not linked to pain relief, improvement of disability or satisfaction with pain management. Opioids were rather associated with more pain. Interventions have been proposed [18], including specific choices for management of acute pain, as well as de-escalation of opioids in outpatient care and with help of an inpatient addiction unit. Improving coping skills through cognitive behavioural therapy has been suggested [6]. Apparently, these patients´ psychiatric comorbidities (depression, anxiety and drug dependence) have to be addressed during their first admission. In this study, we could show that already before the injury, the prevalence of mental health problems was high, indicated by the relatively high consumption or drugs for these conditions. We think that there are possibilities for improvement. A multiprofessional assessment of psychosocial factors, overconsumption of opioids and psychiatric disorders would be beneficial for this sub-group of patients. Today, after-care and follow-up is often limited to the orthopaedic out-patient clinic. Availability of inpatient units for drug de-escalation is limited.
Conclusion
The consumption of opioids, benzodiazepines and antidepressants is higher in the study population of patients with open tibial fractures than in the total Swedish population. The consumption of opioids, benzodiazepines or antidepressants before injury is a predictor of prolonged opioid use after injury. The prescription of opioids for patients with a history of psychiatric disorders or other risk factors should be carefully monitored.
References
- Fuzier R, Rousset J, Bataille B, Salces-y-Nédéo A, Maguès JP (2015) One half of patients reports persistent pain three months after orthopaedic surgery. Anaesthesia Critical Care & Pain Medicine 34(3): 159-164.
- Baldini A, Von Korff M, Elizabeth HB Lin (2012) Review of Potential Adverse Effects of Long-Term Opioid Therapy: A Practitioner's Guide. The Primary Care Companion for CNS Disorders 14(3).
- Weiss RJ, Montgomery SM, Stiller CO, Wick MC, Jansson KÅ (2012) Long-term follow-up of opioid use in patients with acetabular fractures. Injury Extra 43(7): 49-53.
- Al Dabbagh Z, Jansson KA, Stiller CO, Montgomery S, Weiss RJ (2016) Long-term pattern of opioid prescriptions after femoral shaft fractures. Acta Anaesthesiologica Scandinavica 60(5): 634-641.
- Nicholson AD, Kassam HF, Steele JL, Passarelli NR, Blaine TA, et al. (2019) Development of a clinical risk calculator for prolonged opioid use after shoulder surgery. Journal of Shoulder and Elbow Surgery 28(11): 2225-2231.
- Finger A, Teunis T, Hageman MG Ziady ER, Ring D, et al. (2017) Association Between Opioid Intake and Disability After Surgical Management of Ankle Fractures. Journal of the American Academy of Orthopaedic Surgeons 25(7): 519-526.
- Sabesan VJ, Meiyappan A, Montgomery T, Quarless C, Al-Mansoori A, et al. (2019) Diagnosis can predict opioid usage and dependence in reverse shoulder arthroplasty. JSES 34: 316-319.
- Swedish Board of Health and Welfare (Socialstyrelsen).
- Tampe U, Frank S, Weiss RJ, Jansson KÅ (2020) Diagnosis of open tibial fracture showed high positive predictive value in the Swedish national patient register. Clinical Epidemiology 12: 1113-1119.
- Astrand B, Hovstadius B, Antonov K, Petersson G (2007) The Swedish national pharmacy register. Studies in Health Technology and Informatics 129: 345-349.
- Swedish Board of Health and Welfare.
- Sun EC, Darnall BD, Baker LC, Mackey S (2016) Incidence of and Risk Factors for Chronic Opioid Use Among Opioid-Naive Patients in the Postoperative Period. JAMA InternMed 176(9): 1286–1293.
- McCarthy ML, MacKenzie EJ, Edwin D, Bosse MJ, Castillo RC, et al. (2003) Psychological Distress Associated with Severe Lower-Limb Injury. The Journal of Bone & Joint Surgery 85(9): 1689-1697.
- Nunziato C, Fatehi A, Driscoll M, Koenig K, Ring D, et al. (2021) Catastrophic Thinking and Pain Alleviation After Lower Extremity Surgery. Journal of Orthopaedic Trauma 35(3): e89–e95.
- Helmerhorst GTT, Vranceanu AM, Vrahas M, Smith M, Ring D (2014) Risk factors for continued opioid use one to two months after surgery for musculoskeletal trauma. Journal of Bone and Joint Surgery - Series A 96(6): 495-499.
- Vranceanu AM, Jupiter JB, Mudgal CS, Ring D (2010) Predictors of Pain Intensity and Disability After Minor Hand Surgery. Journal of Hand Surgery 35(6): 956-960.
- Taenzer P, Melzack R, Jeans ME (1986) Influence of psychological factors on postoperative pain, mood and analgesic requirements. Pain 24(3): 331-342.
- Devin CJ, Lee DS, Armaghani SJ, Bible J, Shau DN, et al. (2014) Approach to pain management in chronic opioid users undergoing orthopaedic surgery. Journal of the American Academy of Orthopaedic Surgeons 22(10): 614-622.






























