Effects of Manual Lymphatic Drainage Combined with Press-Release Method Orthopedic Manual Lymphatic Physiotherapy on Upper Extremity Edema and Shoulder Joint Range of Motion and Pain in Patients with Breast Cancer
Seong Hyeok Song1, Ju Sang Kim2*, Sung-il Park3 and Sang-Min Park4
1Department of Physical Therapy, Korea Pediatric Integrative Manual Therapy Association, Korea
2Department of Physical Therapy, College of Biomedical Science, Daegu Haany University, Korea
3Department of Physical Therapy, Korean Academy Lymph Manual Therapy Association, Korea
4Department of Physical Therapy, Rhin Convalescent Rehabilitation Medical Center, Korea
Submission: May 28, 2024; Published: June 03, 2024
*Corresponding author: Ju Sang Kim, Department of Physical Therapy, College of Biomedical Science, Daegu Haany University, Korea, Email: soahpt@hanmail.net
How to cite this article: Seong Hyeok Song, Ju Sang Kim*, Sung-il Park and Sang-Min Park. Effects of Manual Lymphatic Drainage Combined with Press-Release Method Orthopedic Manual Lymphatic Physiotherapy on Upper Extremity Edema and Shoulder Joint Range of Motion and Pain in Patients with Breast Cancer. Open Access J Surg. 2024; 15(4): 555916. DOI: 10.19080/OAJS.2024.15.555916.
Abstract
Purpose: The purpose of this study is to investigate the effectiveness of orthopedic manual lymphatic drainage techniques to move fluid and soften hardened tissues using functional assessment of the upper extremity of patients after breast cancer surgery, as well as edema and pain scales.
Methods: The study included 24 patients diagnosed with lymphedema following mastectomy surgery, who received the intervention twice a day, three times a week for six weeks, and were evaluated for upper extremity swelling volume assessment and shoulder joint range of motion and pain sensory.
Results: In conclusion, this study demonstrates that the integrated lymphatic therapy approach of orthopedic manual lymphatic physiotherapy is an effective treatment for reducing edema, improving shoulder joint range of motion, and reducing pain sensory in the upper extremity in postoperative patients with breast cancer.
Conclusion: Orthopedic manual lymphatic physiotherapy with press-release techniques was effective in improving upper extremity edema, shoulder joint range of motion, and pain in a post-breast cancer surgery patient.
Keywords: Edema; Manual Lymph Drainage; Orthopedic manual lymphatic physiotherapy; Interstitial fluid; Alpha waves
Abbreviations: CDT: Complete Decongestive Therapy; DASH: Disabilities of the Arm, Shoulder, and Hand; NRS: Numeric Rating Scale; MLD: Manual Lymphatic Drainage; MWF: Mobilization with Facilitation; KPIMT: Korea Pediatric Integrative Manual Therapy; SF-MPQ: Short-Form McGill Pain Questionnaire
Introduction
In recent years, breast cancer is ranked second in the five-year cancer prevalence rate among women in Korea with 21.9% per 100,000 population, and the incidence of breast cancer has also increased rapidly, ranking first among newly diagnosed malignant neoplasms in women with 20.3%, and by age group, it is ranked first in the 35-64 age group with 29.1%, and the five-year survival rate is 96.8%, showing a high survival rate [1].
Lymphedema, which occurs after cancer progression and treatment, was found to occur in more than 50% of breast cancer patients [2], who underwent surgery to remove the lymph nodes in the armpit and radiation therapy, and in more than 64% of patients who underwent surgery to remove the lymph nodes in the groin or pelvis [3]. Lymphedema is a soft tissue swelling caused by the accumulation of proteinaceous fluid in the pericellular space of cells. This reduces the carrying capacity of the lymph and increases the lymphatic load. The severity of lymphedema is graded using the International Society of Lymphology’s scale [4]. Lymphedema is a chronic, progressive condition in which the swollen area increases in size and weight, limiting motion and joint movement with postural changes and pain in daily activities. Conservative treatment with radiation therapy is associated with decreased shoulder joint range of motion, localized dysfunction, and the development of lymphedema [5].
In addition, lymphedema occurs in about 20 to 40 percent of patients after surgery, such as mastectomy and lymph node dissection, and is associated with upper arm dysfunction, including numbness, pain, limited range of motion in the shoulder joint and neck, tendonitis of the rotator cuff, and decreased muscle strength [6,7]. In recent years, some researchers have been working on controlled studies to determine the effectiveness of orthopedic manual physical therapy with Manyal Lymph Drainage (MLD), but the results are still controversial. Multiple Continuous compression is accepted as an essential part of treatment [8]. This effect has been shown to reduce edema by 7-17 % when compression methods such as compression stockings are applied without any other treatment [9].
MLD improves the appearance of edema by improving microvascular tone and increasing mobility, but because MLD is usually performed in conjunction with compression, it is difficult to conclude that it is effective in reducing edema by more than 60%. It would be unreasonable to attribute this effect to MLD alone, The Other Study demonstrated a 20% reduction in edema with a low-elastic bandage and orthopedic manual physical therapy with MLD, while Johansson et al. validated the effectiveness of orthopedic manual physical therapy with MLD alone with a statistically significant difference of more than 7% in favor of MLD over bandage alone [10,11].
Therefore, this study aimed to investigate the effects of applying orthopedic manual physical therapy with MDL technique using upper extremity orthopedic manual physical therapy using mobilization with Facilitation technique and Press - Release technique, a new physiotherapy treatment method, on changes in upper extremity swelling circumference, shoulder joint range of motion assessment, and pain sensation in breast cancer patients, and to provide a basis for future research on physiotherapy intervention programs.
Methods
Participation
In this study, 24 patients who were diagnosed with lymphedema after mastectomy surgery at J Hospital Cancer Specialized Rehabilitation Center located in Jeollanam-do were included in the study from the beginning of June 2023 to the end of March 2024, and the circumference of the swelling area and the contralateral upper limb differed by more than 2 cm, the skin condition of the upper limb was not problematic for applying the bandage method, and the patient was able to perform upper limb exercises according to the therapist’s instructions.
Inclusion criteria for the study were:
Diagnosed with unilateral lymphedema.
No active cancer.
No joint movement restrictions.
Not taking any medications, foods, etc. that may affect the reduction of edema, such as diuretics that may affect edema reduction.
No neurological conditions that could affect measurements.
Guardian has agreed to participate in the study.
Before participating in this study, all subjects were fully informed of the purpose, content, and methods of the study, and only those who voluntarily signed an informed consent form were included in the study. Patients with any of the following conditions were excluded from the study.
Individuals with cardiac dysfunction and acute thrombosis.
Individuals with dermatitis.
Those with acute malignant lymphedema.
Subjects with arm paralysis and vascular disorders.
Participation in a study like this study within the last 1 year.
Measures and Procedure
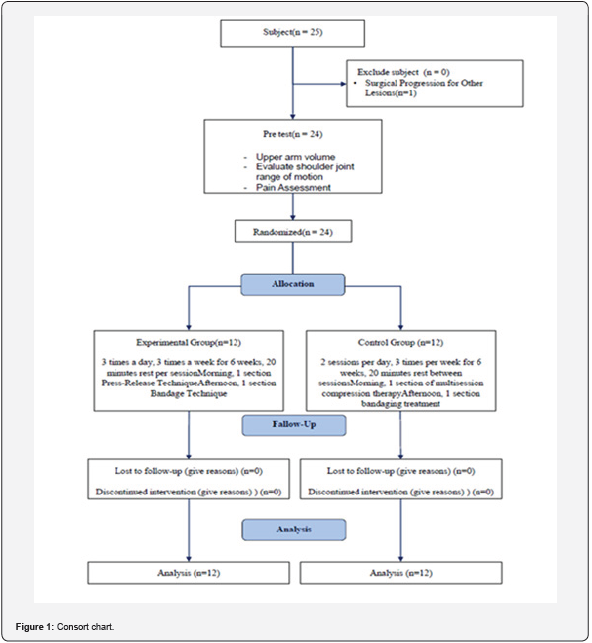
This case study was conducted after obtaining informed consent in accordance with the Declaration of Helsinki. The procedure of this study is as follows (Figure 1). The G-Power 3.0 program (IBM Inc., USA) was used to determine the sample size of this study. To calculate the sample size, the significance level (α) was selected as 0.05, the power (1-β=0.8) was selected as 0.48, and the effect size (d) was calculated using the preliminary experiment.
A minimum of 12 subjects were required for each group, for a total of 24 subjects. The subjects were randomly assigned to the MLD group and the control group. The subjects were randomly assigned and grouped using randomization software (Random allocation software version 1.0, University of Medical Sciences, USA). In this study, the intervention was delivered three times a week, twice a day for six weeks, for a total of 36 sessions. The pretest included general characteristics, upper extremity edema assessment, shoulder joint range of motion, and pain sensation (Figure 2).
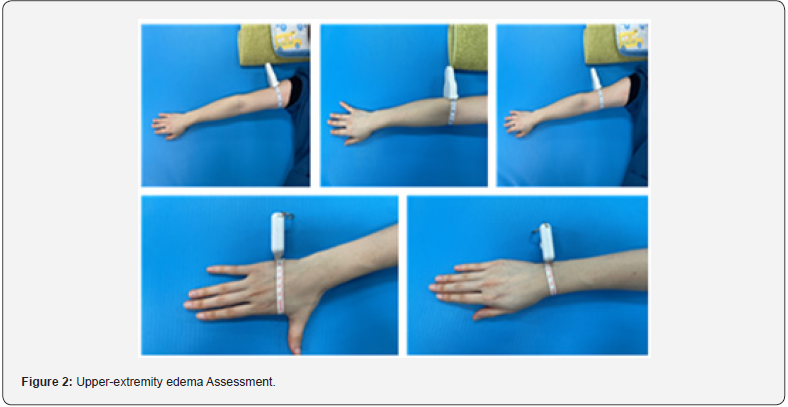
Assessment of Edema of the Upper Extremities
When Assessment upper extremity (Figure 2) edema, upper extremity circumference was measured 10 cm below the patient’s elbow joint with a measuring tape (Arm Circumference Gauge, Sammons Preston, USA), a method proven reliable in Taylor’s experiment [12].
Assessment of Range of Motion of Shoulder Joint
To observe the range of motion of the upper extremity before and after treatment, the shoulder joint range of motion was tested using a goniometer. Active flexion, abduction, and external rotation of the shoulder joint were measured in the edema position. The flexion of the shoulder joint was measured while lying supine, bending the knees and hip joints, and placing the feet flat on the floor to prevent hyperextension of the lumbar spine. The elbow joint was extended, and the forearm and palm were kept supinated. The axis of the joint goniometer was aligned with the acromion process of the scapula, which passes through the humeral head. The fixed arm was positioned at the mid-axillary line of the torso, and the movable arm was measured after being positioned at the outer midline of the humerus.
Shoulder joint abduction was measured in the supine position with knees and hips bent and feet flat on the floor. The arm being measured was placed in an anatomical position, and the elbow joint was maintained in an extended state. The axis of the joint goniometer was aligned with the anterior part of the acromion process of the scapula through the center of the humeral head. The fixed arm was parallel to the midline of the sternum and placed on the lateral surface of the anterior surface of the ribcage, and the movable arm was parallel to the midline of the humerus and placed on the anterior surface of the arm before measurement. External rotation of the shoulder joint was measured in the supine position with the knees and hip joints flexion and the feet flat on the floor.
The axis of the joint goniometer was aligned so that the direction of the humeral head coincided with the olecranon process of the ulna passing through the humeral body. The fixed arm was positioned perpendicular to the floor, and the movable arm was measured after being positioned on the ulnar body in the direction of the styloid process of the ulna [13].
Assessment of Pain sensory
The short-form McGill pain questionnaire (SF-MPQ) was used to measure pain sensory, and the reliability of the measurement tool was r=.89.14 The SF-MPQ consists of a total of 15 questions, including 11 questions in the sensory domain and 4 questions in the emotional domain, and can evaluate the sensory and emotional components of pain [14,15]. Each item is rated on a 4-point Likerd scale from 0 (no pain), 1 (mild pain), 2 (moderate pain), and 3 (severe pain). The higher the summed score, the higher the pain sensation. A physical therapist explained to the subjects how to fill out the questionnaire, and self-assessed the questionnaire while the subjects were stable.
Intervention
Experimental Group
The intervention for the MLD technique of the Press-Release technique was administered twice a day, three times a week for six weeks, and was applied for 20 minutes each. The subject was asked to lie down on the treatment table, place a pillow under the knees, bend the hip joint at 70°, and relax the muscles as much as possible. Korea Pediatric Integrative Manual Therapy (KPIMT) Press Release Therapy and Mobilization with Facilitation therapy [16,17]. KPIMT muscular skeletal factor kalten born segmental movement and mulligan concept where there is an arbitrary restriction of movement of the incorrect musculoskeletal system [18,19].
The coordinative control of the use of the arms and hands mixed with the spine, through the handling input of the therapist, with the distribution of various contacts, sufficient proprioceptive and somatosensory input, and through the guiding and assisting of the hand, the sensor light is sufficiently turned on. Mobilization with Facilitation (MWF) technique and stretching release technique and press release technique are applied to each joint junction for inputting somatosensory and proprioceptive sensory information of the muscle when providing sufficient support for the ability to recover balance from touch to come.16 Provides joint stability and Recovers pain by stimulating the parasympathetic nerve and increasing lymph vessel flow [16].
PR technique treatment area and pressure stage; The pressure level of the treatment is divided into skin surface, dermis layer, fascia surface, and submuscular area according to the depth, and the level of force is divided into 1-4 levels, changing depending on the treatment area.
Before all lymphatic physical therapy, pump Jugular angle area 25 times before performing the next treatment [16].
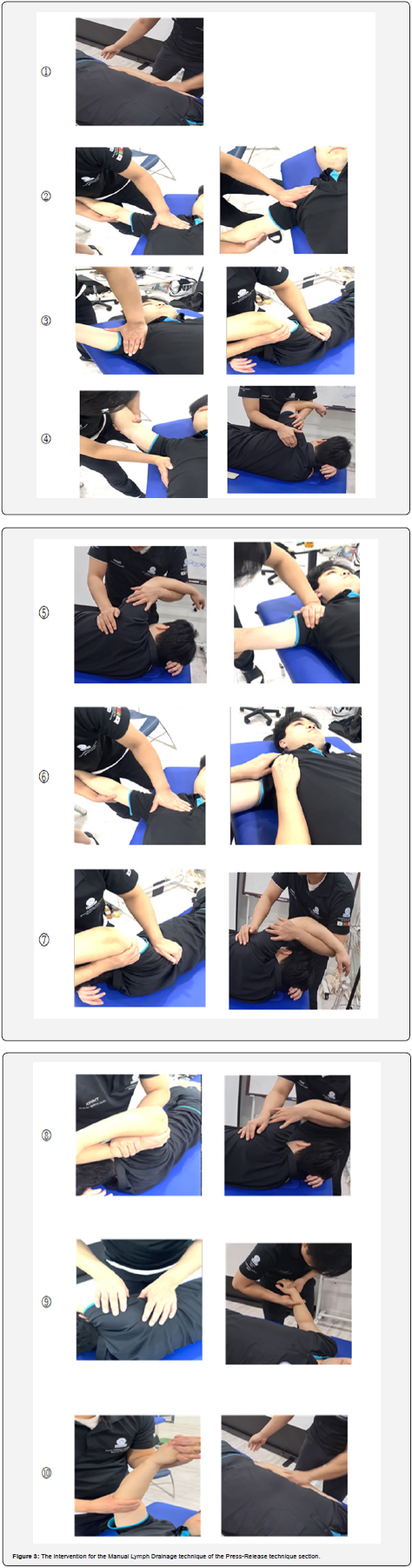
This section deals with the axillary group and hand arm region. the muscle each group muscles (apex, base, medial lateral posterior, anterior). ① Effleuage→ ② Treatment of the Apex part of infraclavicle lymph nodes → delto-pecto lymph nodes → axillary lymph nodes and trapeziurs and deltoid muscle (pressrelease technique 20 ) → ③ Treatment of the Base part of Latissimus dorsi and teres major (press-release technique 15) → ④ Treatment of the Medial Border part of serratus anterior and inter costalis muscle (press-release technique 15) → ⑤ Treatment of the lateral border part of Coracobrachialis and bicepce muscle (press-release technique 15) → ⑥ Treatment of the Anterior wall of Pecto major and minor and subclavicles muscle with anterior wall Cord bending technique (press-release technique 15) → ⑦ Treatment of the posterior wall of Latissimus dorsi and teres minor muscle (press-release technique 15) → ⑧ External Rotation Techniques to increase scapulo-humeral joint range of motion → ⑨ Posterior wall Cord bending technique → Pump stroke stage of Upper arm (Deltoid → Biceps → Triceps 15section) and Lower arm (Supnation and Pronation Scoope stroke) → Hand Pump ans thumb circle strock→ Ocillization ⑩ Effleuage (Figure 3).
In the afternoon section treatment, the upper limb bandaging method was performed for 20 minutes followed by a 10-minute rest. The bandaging method applied to the patient’s upper limb was to fold a 4 cm bandage in half, wrap it loosely around the finger, and then apply a cotton stockinette to the upper limb. I wound it on. Afterwards, an undercast pad was added to the wrapped from the fingers upward to the upper limb [20]. For the compression bandage, Lohmman and Rauscher’s low elastic bandage (Germany) was used in both the experimental and control groups.
Control Group
The control group intervention was performed three times a day, every other day for six weeks, with subjects in the supine position on the treatment table, as relaxed as possible, receiving 20 minutes of multi-chamber pneumatic compression per intervention, followed by 10 minutes of relaxation for 10 minutes. The pressure was kept below 30mmHg to prevent further damage to the lymphatic system in the upper extremity. In the afternoon section, the treatment consisted of 20 minutes of upper extremity bandaging followed by 10 minutes of rest. In the afternoon section, bandaging was performed in the same way as in the experimental group.
Statistical Analysis
The data collected in this study were subjected to statistical analysis using SPSS for windows (version 21.0). Descriptive statistical methods were used to determine the subject’s age, weight, height, medical treatment, and area of edema, and an independent samples t-test was performed to determine the homogeneity of the experimental and control groups. For the differences in arm circumference, shoulder joint range of motion, and pain sensation for comparison of edema volume before and after treatment between the experimental and control groups, a Wilcoxon rank test was performed to test the significance before and after treatment of each group, and the differences between each group were performed. To find out, the Mann-Whitney U test was performed. The significance level was set at 0.05.
Results
The total number of subjects in the study was 24 women, and the medical characteristics of the subjects in the study were as follows: 12 (45%) of the 24 subjects received combined radiotherapy and chemotherapy, 9 (40%) received chemotherapy, and 3 (15%) received radiotherapy. An independent samples t-test was performed to test the homogeneity of the experimental and control groups. The location of the edema in the study included 16 (75%) left upper extremity, 8 (35%) right upper extremity, and 24 (100%) had edema in both proximal and distal parts of the upper extremity (Table 1).
Pre-post Treatment Upper Extremity Volume Changes to Assess Edema in Experimental and Control Groups: The volume of the upper arm and forearm of the experimental group decreased significantly from pre-treatment to post-treatment. In the control group, the decrease was significant for the upper arm but not for the forearm (Table 2) (p<0.05).
Compare the Range of Motion of the Shoulder Joint: Changes in pre-post treatment range of motion of the shoulder joint between the experimental and control groups There were statistically significant differences in the pre-post treatment range of motion of the shoulder joint between the experimental and control groups for flexion, abduction, and external rotation, and only for abduction in the control group (p<0.05) (Table 3).




Comparison of Pain Sensory: The changes in pain sensation of the experimental group and control group according to the intervention are as follows (Table 4). The pain sensation before and after the intervention for each group was compared by paired sample t-test, and there was a statistically significant difference after the intervention in the experimental group (p<.05) (Table 4).
Discussion
This study aims to explore a manual lymphatic drainage (MLD) therapy program that incorporates upper extremity orthopedic lymphatic physiotherapy, which is more effective than compression methods used in physical therapies for the therapeutic management of upper extremity lymphedema following mastectomy.
Specifically, this study evaluates effects on edema, range of motion, and pain sensation in the upper extremities of patients with lymph edema. The overall mean age of the participants was 52.25±8.96 years; this is slightly higher than the findings of the Korea Central Cancer Registry, reporting the highest incidence of breast cancer in women aged 40-49 years in Korea.
However, this could be attributed to the random selection of patients within a specific period and the overall incidence rate is expected to align with the Registry’s findings [21]. Tumor locations were 55.0% left-sided and 45.0% right-sided, aligning closely with the findings reported by the Korean Breast Cancer Society, with 51.6% left-sided, 47.5% right-sided, and 0.9% bilateral [22]. Lee and Bae [23] also reported a similar pattern, with a higher number of patients with left-sided breast cancer than those with right-sided [23]. According to the American Cancer Society, one in eight American women is expected to develop breast cancer, with incidence rates being exceptionally high among women aged 50-59 years, like the findings of the Korea Central Cancer Registry [24].
In addition, Siotos [25] found the upper outer quadrant of the breast at a 36.2% incidence as the most common tumor location, followed by the upper inner quadrant at 13.1%, the lower outer quadrant at 9.8%, the lower inner quadrant at 7.2%, the nipple at 1.2%, the axillary tail at 0.3%, and overlapping regions at 24.7% [25]. Post-surgical treatment among the 24 participants included radiation and chemotherapy in 45%, chemotherapy alone in 40%, and radiotherapy alone in 15%, with radiation identified as a significant risk factor for lymphedema [26]. However, this study selected patients exhibiting lymphedema on both the proximal and distal sides of the upper extremity that differed by more than 2 cm from the normal side, irrespective of their medical treatment type, limiting the correlation between treatment method and lymphedema occurrence in the participants.
The results of this study showed a significant decrease in pain sensation after intervention (p<.05). The lymphatic system plays a crucial role in maintaining homeostasis of macromolecules, lipid absorption, immune function, and interstitial fluid regulation. Its main feature is the ability to remove interstitial fluid and proteins from the interstitial space, draining them from the interstitial space into the vasculature [27]. In their study on the use of physiotherapy and exercise therapy after mastectomy in women aged 65 years and older, Tunay et al [28], found significant reductions in pain and improvements in shoulder function, range of motion during flexion, abduction, and external rotation, muscle strength, physical function, and quality of life, as well as a decrease in lymphedema volume [28]. In another study, Cho et al [29], compared conventional physical therapy with manual lymphatic drainage applied three times a week for four weeks in 41 patients with lymphedema and a pain scale score of 3 or higher [29]. They found significant improvements in functional and symptomatic aspects, shoulder flexor muscle strength assessed by the DASH (disabilities of the arm, shoulder, and hand) score, and pain levels measured by the NRS (numeric rating scale). Moreover, they noted a more significant difference in the group receiving combined conventional physical therapy and manual lymph drainage compared to those receiving conventional physical therapy alone, which is consistent with the results of this study.
MLD techniques enhance the movement of lymphatic fluid in the interstitial space, contributing to the removal of interstitial fluid. This drainage into the venous system improves venous return, reduces systemic vascular resistance, and facilitates oxygen delivery to cells. In other words, the improved blood circulation after the intervention is believed to facilitate the muscle cell oxygenation, consequently alleviating pressure on the muscles and, thus, contributing to the reduction in muscle tone [30]. Continuous light stimulation during moderate pressure massage activates Aβ fibers, stimulating the substantia gelatinosa in the spinal dorsal horn and inhibiting pain transmission [31]. Additionally, oxytocin’s activation of the endogenous pain control system induces analgesic effects [32,33]. This study suggests that the press-release rhythmic stimulation effectively reduced pain in patients with breast cancer.
Research suggested post-surgical exercises for patients with breast cancer to reduce complications and improve physical function, including flexibility exercises to smooth joint range of motion, muscle strength exercises, and exercises to strengthen cardiorespiratory function and increase stamina. [34] A similar study compared the effectiveness of MLD and complete decongestive therapy (CDT); this physical therapy regimen includes compression bandaging in moving fluid and reducing limb volume in 13 patients with lymphedema of the lower extremities. The study found that the volume of the leg and the amount of intracellular and extracellular fluid decreased when using the physical therapy regimen compared to CDT [35]. Orthopedic manual lymphatic physiotherapy integrated with MLD influences the body through various mechanisms. It has been reported to reduce excessive sympathetic nervous system activity due to stress or other factors and enhance parasympathetic nervous activity, promoting relaxation. Additionally, it increases the activity of alpha waves, associated with relaxation and calmness, and decreases gamma waves, activated during extreme arousal and excitement [36]. This study suggests that the press-release rhythmic stimulation used in orthopedic manual lymphatic physiotherapy, akin to functional massage, facilitates muscle relaxation and joint mobility as well as optimally applies lymphatic treatment. This approach improved the range of motion and reduced pain in the shoulder joint, as evidenced by the study’s results.
However, this study has certain limitations stemming from the number of local participants and the control of external variables. Future research should involve a larger sample size and more controlled measurement of various variables.
Conclusion
This study investigated the effectiveness of orthopedic manual lymphatic physical therapy using the press-release technique in improving upper extremity swelling, shoulder joint range of motion, and pain in patients after breast cancer surgery.
The volume of the upper arm and forearm of the experimental group decreased significantly from pre-treatment to post-treatment. In the control group, the decrease was significant for the upper arm but not for the forearm (p<0.05).
Changes in pre-post treatment range of motion of the shoulder joint between the experimental and control groups There were statistically significant differences in the pre-post treatment range of motion of the shoulder joint between the experimental and control groups for flexion, abduction, and external rotation, and only for abduction in the control group (p<0.05).
The changes in pain sensation of the experimental group and control group according to the intervention are as follows (Table 4). The pain sensation before and after the intervention for each group was compared by paired sample t-test, and there was a statistically significant difference after the intervention in the experimental group (p<.05).
Orthopedic manual lymphatic physiotherapy with pressrelease techniques in manual lymph drainage was effective in improving upper extremity edema, shoulder joint range of motion, and pain in a post-breast cancer surgery patient.
Acknowledgements
The authors would like to thank the study participants for their collaboration.
Conflict of Interest
The authors declare no conflict of interest.
References
- Bray F, Ferlay J, Soerjomataram I, Isabelle S, Rebecca LS, et al. (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6): 394-424.
- Shih YC, Xu Y, Cormier JN, Janice NC, Sharon G, et al. (2009) Incidence, treatment costs, and complications of lymphedema after breast cancer among women of working age: a 2-year follow-up study. J Clin Oncol 27(12): 2007-2014.
- De Vries M, Vonkeman WG, van Ginkel RJ, Hoekstra HJ (2006) Morbidity after inguinal sentinel lymph node biopsy and completion lymph node dissection in patients with cutaneous melanoma. Eur J Surg Oncol 32(7): 785-789.
- Lee BB, Kim YW, Kim DI, Hwang JH, Laredo J, et al. (2008) Supplemental surgical treatment to end stage (stage IV-V) of chronic lymphedema. Int Angiol 27(5): 389-395.
- Warren LE, Miller CL, Horick N (201) The impact of radiation therapy on the risk of lymphedema after treatment for breast cancer: a prospective cohort study. Int J Radiat Oncol Biol Phys 88(3): 565-571.
- Jemal A, Center MM, DeSantis C, Ward EM (2010) Global patterns of cancer incidence and mortality rates and trends. Cancer Epidemiol Biomarkers Prev 19(8): 1893-1907.
- Martin ML, Hernandez MA, Avendano C, Rodriguez F, Martinez H (2011) Manual lymphatic drainage therapy in patients with breast cancer related lymphoedema. BMC Cancer 11: 94.
- Didem K, Ufuk YS, Serdar S, Zumre A (2005) The comparison of two different physiotherapy methods in treatment of lymphedema after breast surgery. Breast Cancer Res Treat 93(1): 49-54.
- Johansson K, Albertsson M, Ingvar C, Ekdahl C (1999) Effects of compression bandaging with or without manual lymph drainage treatment in patients with postoperative arm lymphedema. Lymphology 32(3): 103-110.
- Boris M, Weindorf S, Lasinkski S (1997) Persistence of lymphedema reduction after noninvasive complex lymphedema therapy. Oncology (Williston Park) 11(1): 99-109.
- Williams AF, Vadgama A, Franks PJ, Mortimer PS (2002) A randomized controlled crossover study of manual lymphatic drainage therapy in women with breast cancer-related lymphoedema. Eur J Cancer Care (Engl) 11(4): 254-261.
- Taylor R, Jayasinghe UW, Koelmeyer L, Ung O, Boyages J (2006) Reliability and validity of arm volume measurements for assessment of lymphedema. Phys Ther 86(2): 205-214.
- Rietman JS, Dijkstra PU, Geertzen JH, et al. (2003) Short-term morbidity of the upper limb after sentinel lymph node biopsy or axillary lymph node dissection for Stage I or II breast carcinoma. Cancer 98(4): 690-696.
- Grafton KV, Foster NE, Wright CC (2005) Test-retest reliability of the Short-Form McGill Pain Questionnaire: assessment of intraclass correlation coefficients and limits of agreement in patients with osteoarthritis. Clin J Pain 21(1): 73-82.
- Hawker GA, Mian S, Kendzerska T, French M (2011) Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP). Arthritis Care Res (Hoboken) 63(11): 240-252.
- Song SH, Park JS, Song KY et al. (2023) A Study on the Validity and Test-retest Reliability of the Measurement of the Head Tilt Angle of the Smart Phone Application ‘KPIMT Torticollis Protractor’. J Kor Phys 35(6): 177-184.
- Emery C (1994) The determinants of treatment duration for congenital muscular torticollis. Phys Ther 74(10): 921-929.
- Kaltenborn FM (1993) Orthopedic manual therapy for physical therapists Nordic system: OMT Kaltenborn-Evjenth concept. J Manual & Manipulative Therapy 1(2): 47-51.
- McDowell JM, Johnson GM, Hetherington BH (2014) Mulligan Concept manual therapy: standardizing annotation. Man Ther. 19(5): 499-503.
- Hopkins A (2008) A community nursing guide: multilayer lymphoedema bandaging. Br J Community Nurs 13(4): 18-20.
- Shin HR, Jung KW, Won YJ, Jae-Gahb P (2004) 2002 annual report of the Korea Central Cancer Registry: based on registered data from 139 hospitals. Cancer Res Treat 36(2): 103-114.
- Youn HS, Kang SH, Kang SS (2004) Nationwide Korean breast cancer data of 2002. J Korean Breast Cancer Soc 7(2): 72-83.
- Lee JS, Bae YT (2004) Clinical analysis of breast cancer patients treated with surgery. J Korean Breast Cancer Soc 7(3): 174-179.
- DeSantis C, Ma J, Bryan L, Jemal A (2014) Breast cancer statistics, 2013. CA Cancer J Clin 64(1): 52-62.
- Siotos C, McColl M, Psoter K, Richard CG, Mohamad ES, et al. (2018) Tumor Site and Breast Cancer Prognosis. Clin Breast Cancer 18(5): 1045-1052.
- Choi JH, Kim SW, Kim JH, et al. (2003) Clinical features and pathological characteristics of ductal calcinoma in situ of the breast mastectomy and breast conservative surgery. J Korean Surg Soc 65(2): 101.
- Secker GA, Harvey NL (2015) VEGFR signaling during lymphatic vascular development: From progenitor cells to functional vessels. Dev Dyn 244(3): 323-331.
- Tunay VB, Akbayrak T (2012) The effect of multidimensional physiotherapy program on shoulder function, pain, and lymphedema after surgery in elderly breast cancer patients. J Geri Reh 28(4): 281-286.
- Cho Y, Do J, Jung S, Kwon O, Jeon JY (2016) Effects of a physical therapy program combined with manual lymphatic drainage on shoulder function, quality of life, lymphedema incidence, and pain in breast cancer patients with axillary web syndrome following axillary dissection. Support Care Cancer 24(5): 2047-2057.
- Ramos PDS, Cunha IRMM, Rachel MC, Pacca PSS, Ferreira AP, et al. (2015) Acute cardiovascular responses to a session of Manual Lymphatic Drainage. Fisioterapia em Movimento 28: 41-48.
- McMahon C, Barley JP, Edgar HW, et al. (2013) Anthelmintic resistance in Northern Ireland. II: Variations in nematode control practices between lowland and upland sheep flocks. Vet Parasitol 192(1-3): 173-182.
- Breton JD, Veinante P, Uhl-Bronner S (2008) Oxytocin-induced antinociception in the spinal cord is mediated by a subpopulation of glutamatergic neurons in lamina I-II which amplify GABAergic inhibition. Mol Pain 4: 19.
- Lund I, Ge Y, Yu LC, Kerstin UM, Jing W, et al. (2002) Repeated massage-like stimulation induces long-term effects on nociception: contribution of oxytocinergic mechanisms. Eur J Neurosci 16(2): 330-338.
- Eom AY (2006) Development and application of early rehabilitation program using yang-style tai chi exercise for breast cancer patients after mastectomy. Dissertation of Doctorate Degree Seoul University.
- Brix B, Apich G, Roessler A, Andreas R, Christian U, et al. (2020) Fluid Shifts Induced by Physical Therapy in Lower Limb Lymphedema Patients. J Clin Med 9(11): 3678.
- Shim JM, Yeun YR, Kim HY, Kim SJ (2017) Effects of manual lymph drainage for abdomen on the brain activity of subjects with psychological stress. J Phys Ther Sci 29(3): 491-494.






























