Video-Assisted Laparoscopic Bile Duct Exploration with Choledochoscope for Large Element Choledocholithiasis: Case Report
Fernando Carballar Mejía*, Sergio Maldonado Mares, Ana Sofía González Izaguirre, Maria Fernanda González Castillo, Pablo De Jesús Díaz Cruz, and Alondra Gabriela Mercado Mendiola
Department of Surgery at Hospital Regional León, ISSSTE. León, México, USA
Submission: October 18, 2023; Published: October 30, 2023
*Corresponding author: First name: Fernando Carballar Mejía, Department of Surgery at Hospital Regional León, ISSSTE. León, México. USA, Email: fcarballar@hotmail.com
How to cite this article: Fernando C M, Sergio M M, Ana S G I, Maria F G C, Pablo De J D C, et al. Video-Assisted Laparoscopic Bile Duct Exploration with Choledochoscope for Large Element Choledocholithiasis: Case Report. Open Access J Surg. 2023; 15(1): 555903. DOI: 10.19080/OAJS.2023.15.555903.
Abstract
Choledocholithiasis is defined by the presence of stones in the main bile duct. The prevalence of choledocholithiasis in patients with calculous cholecystitis according to the American Society for Gastrointestinal Endoscopy (ASGE) and European Society for Gastrointestinal Endoscopy (ESGE) guidelines is 8% to 18%. LCBDE offers effective single-stage treatment with a stone clearance rate similar to ERCP. This method of intervention has positioned itself as an effective and safe alternative in the treatment of patients with large element choledocholithiasis or patients with failed ERCP.
Keywords: Choledocholithiasis; LCBDE; choledochoscope; European Society of Gastrointestinal Endoscopy (ESGE); American Society of Gastrointestinal Endoscopy (ASGE)
Introduction
Choledocholithiasis is defined by the presence of stones in the main bile duct. It is classified as primary (85%) or secondary, depending on the etiology of the stone [1]. Primary stones are those that form directly in the bile ducts, while secondary stones form in the gallbladder and migrate through the cystic duct to the common bile duct [2,3]. Secondary stones are usually made of cholesterol, while primary stones are made of brown pigment. Causes of bile stasis that lead to the development of primary stones include biliary stricture, papillary stricture, tumors, or other (secondary) stones [4]. The clinical manifestations of common bile duct stones can be silent and are often discovered incidentally. They can cause obstruction, complete or incomplete, or manifest as gallstone cholangitis or pancreatitis. The prevalence of choledocholithiasis in patients with stone cholecystitis reported in the American Society of Gastrointestinal Endoscopy (ASGE) and European Society of Gastrointestinal Endoscopy (ESGE) guidelines is 8% to 18% [5,6]. In Mexico, the proportion is 5% to 10%, of these10-20% have giant choledocholithiasis, that is, the presence of stones larger than 15 mm, increasing morbidity and mortality due to complications [5,7]. Giant stones are a challenging problem and ERCP is very useful in resolving them through its different modalities. Most common bile duct stones can be removed without problems with sphincterotomy. Removal of these stones can sometimes be difficult or unsuccessful due to large stones. In these cases, the combination of Endoscopic Sphincterotomy with Endoscopic Papillary Dilation with Large Balloon (EPDBG) can be useful [2,8-10].
Case Report
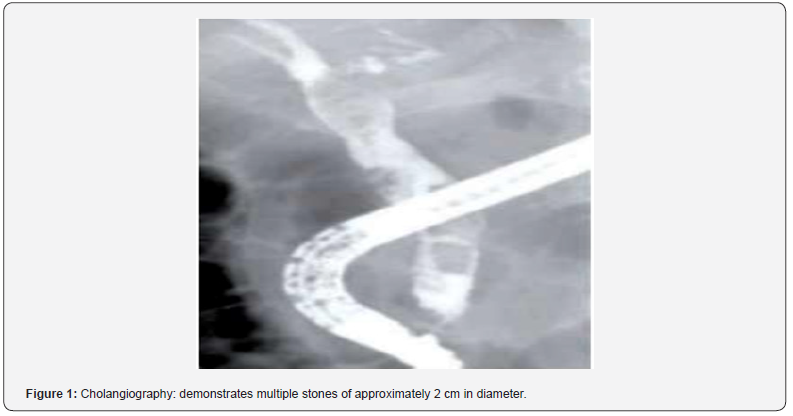
A 41-year-old female patient, originally and resident of León, Guanajuato, México denies chronic degenerative diseases. Surgical history of bilateral tubal occlusion in 2017. She began suffering from it 3 days before her admission to hospital presenting abdominal pain in the radiated epigastrium, hypochondrium and right flank, acute of sudden onset, transfictional character and colic type, jaundice, nausea without reaching vomiting and fever 38.3°C as accompanying symptoms. On physical examination, patient is conscious, oriented, integuments with jaundice +++/++++, cardiopulmonary without apparent ventilatory compromise, ballooning abdomen, distended with pain on mid-palpation in the epigastrium and in the right upper quadrant, negative Murphy’s sign, without evidence of peritoneal irritation, peristalsis present, extremities with adequate distal capillary filling. Laboratories report upon admission: Complete blood cell count: Leukocytes 16,000, Hemoglobin 13.7 g / dl, Hct 40%, Platelets 184,000. Liver and Pancreatic Function Tests: BT: 7.3 mg / dl, BD: 6.2 mg / dl, BI: 1.1 mg / dl, FA: 458 U / L, GGT: 313 U/L, AST: 40 U / L, ALT: 47 U / L. Cholangiography reports: demonstrates multiple stones of approximately 2 cm in diameter (Figure 1).
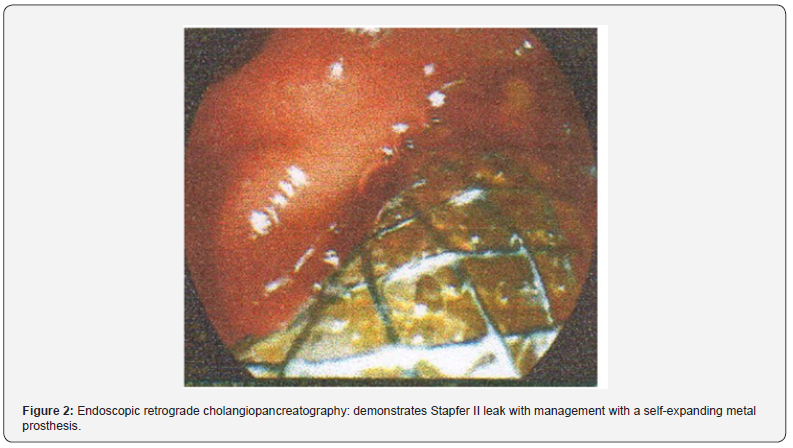

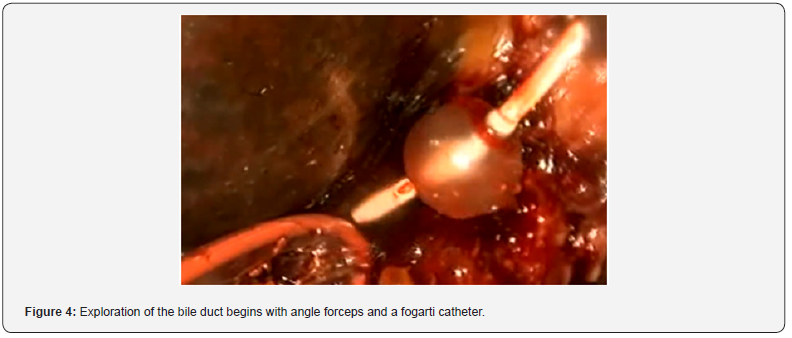
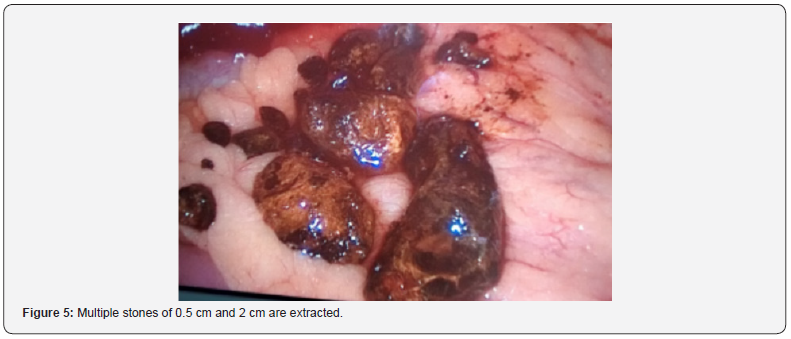
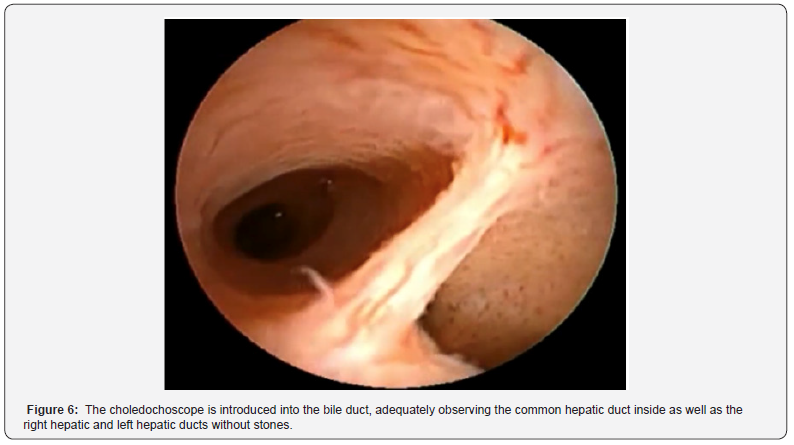
Endoscopic retrograde cholangiopancreatography reports: Unresolved choledocholithiasis of large elements, sphincterotomy and sphincteroplasty, Stapfer II leak with management with a self-expanding metal prosthesis (Figure 2). Because it was not possible to resolve the biliary obstruction using ERCP, antibiotic management was started with ertapenem and it was decided to perform Video-assisted laparoscopic bile duct exploration with choledochoscope, a preoperative evaluation was carried out by the internal medicine service, granting surgical risk of ASA 1, Goldman 1, Lee 1. The patient is placed in a supine position under balanced general anesthesia after asepsis and antisepsis of the abdominal region, sterile fields are placed, the first 12 mm right paraumbilical trocar is placed with the open Hasson technique, and the laparoscope and 4 more trocars are placed under direct vision supraumbilical, right subcostal, right flank and left paraumbilical. The peritoneal leaf of the bile duct is released, properly identifying the common bile duct, a longitudinal choledochotomy is performed with a number 11 scalpel, obtaining purulent material outflow (Figure 3), it is drained, and exploration of the bile duct begins with angle forceps and a fogarti catheter (Figure 4), multiple stones of 0.5 cm and 2 cm are extracted (Figure 5). The choledochoscope is introduced into the bile duct, adequately observing the common hepatic duct inside as well as the right hepatic and left hepatic ducts without stones (Figure 6).
The choledochoscope is directed inferiorly, locating a stone of approximately 1 cm which is fractured with forceps and removed from the bile duct. Biliary, choledochoscope is introduced again, observing bile duct without stones, metal prosthesis is found in duodenum, cholecystectomy is continued, releasing anterior and posterior walls with monopolar energy without achieving critical safety vision, so it is decided to perform restorative subtotal cholecystectomy, gallbladder´s walls are closed with 2-0 vicryl, the body and bottom of the gallbladder are removed, a 10fr x 12cm plastic endoprosthesis is placed. Its adequate position is confirmed with a choledochoscope, the choledochotomy is closed with a surget with 4-0 monocryl, a penrose 3/8 is placed. The surgical procedure was terminated without complications or incidents, bleeding 150 cc. On the second post-surgical day, control laboratory studies are requested; Complete blood cell count: Leukocytes 11,000, Hemoglobin 13.1 g/dl, Hct 39%, Platelets 192,000. Liver and Pancreatic Function Tests: BT: 3.0 mg/dl, BD: 2.0 mg/dl, BI: 1.0 mg/dl, FA: 340 U/L, GGT: 275 U/L, AST: 42 U/L, ALT: 40 U / L. The patient clearly shows improvement in the decrease in Leukocytes, bilirubin’s, alkaline phosphatase and jaundice, which reflects the resolution of bile duct obstruction.
Discussion
Pre-operative ERCP followed by LC is the most commonly protocol of treatment modality for management of choledocholithiasis. However ERCP carries a high rate of morbidity and mortality mostly due to post-procedure pancreatitis, risk of duodenal perforation and bleeding, as well as sphincter of oddi injury. LCBDE offers a one stage and effective treatment with similar or better stone clearance rate and with a shorter hospital stay, with the advantage of keeping the integrity of sphincter of oddi. After the procedure, stone clearance during LCBDE can be confirmed by IOC (Intraoperative cholangiography) or choledochoscopy. Intra-operative choledochoscopy shows better results than IOC for determining ductal clearance after TD LCBDE and is less time-consuming. Both TC (transcystic) and TD (transcholedochal) approaches seem to be safe and effective. Except that TD stone extraction is associated with an increased risk of bile leaks and requires more expertise and choledochoscopy.
There is lack of randomized trial comparing primary closure with biliary stent. The bile leak rates associated with both forms of LCBDE approaches have been significantly reduced from the last few years, probably explained by the accumulative experience of laparoscopic surgeons. In our case, the excellent and immediately improvement of biochemical markers of obstructive hyperbilirrubinemia as well as deacrease of symptoms in the patient shows the success of this one stage managment for choledocholithiasis. In favor of minimal access surgery mainly because of all the advantages over the open approches, many centers in the world incluiding ours, have started offering one stage management of choledocholithiasis by LC with laparoscopic CBD exploration (LCBDE).
Conclusion
The LCBDE has demonstrated significant efficacy in patients with choledocholithiasis. Its indications include scenarios such as choledocholithiasis of large elements, or patients with a history of failed ERCP. This method of intervention has positioned itself as an effective and safe alternative in the management of these patients, in addition to avoiding complications of typical endoscopic procedures, such as post-ERCP pancreatitis, hemorrhage or duodenal perforation. The importance of monitoring through bilirubin markers and inflammatory response markers, as well as the patient’s symptomatology, is emphasized. More tests are required to establish and standardize the methods of bile duct exploration in the future.
Conflicts Of Interests
The authors declare no conflict of interest.
Acknowledgement
Fernando Carballar Mejía
Sergio Maldonado Mares
References
- Zamorano m, cárcamo c, cares j, fermer o, gabrielini m (2008) Coledocolitiasis gigante. Manejo actual. Cuadernos decirugía 22: 18-24.
- Neuhaus h, zillinger c, born p, et al. (1998) randomized study of intracorporeal laser lithotripsy versus extracorporeal shock-wave lithotripsy for difficult bile duct stones 47 (5): 327-334.
- Cáceres h, ortiz a, orué c, melgarejo o, morinigo r, samaniego c (2013) Litiasis residual versus litiasis primaria de la víabiliar principal: a propósito de un caso controversial. Cirugía paraguaya 37(1): 36-37.
- Narváez-rivera r, gonzález g j, monreal r r, garcía c d, paz d j, garza g a, et al (2016) Accuracy of asge criteria for the prediction of choledocholithiasis. Rev Esp Enferm Dig 108(6): 309-314.
- Asge pancreatic and biliary stent (2013) Status evaluation report. Gastrointestinal endoscopy 77(3).
- Lauri a, horton r, davidson b, burroughs a k, dooley j (1993) Endoscopic extraction of bile duct stones: management related to stone size. Gut 34(12): 1718-1721
- Paik w, ryu j, park j, song b, kim j, park j, et al. (2014) Which is the better treatment for the removal of large biliary stones? Endoscopic papillary large balloon dilation versus endoscopic sphincterotomy. Gut liver 8(4): 438-444.
- Madhoun mf, wani s, hong s, tierney w n, maple jt (2014) Endoscopic papillary large balloon dilation reduces the need for mechanical lithotripsy in patients with large bile duct stones: a systematic review and meta-analysis. Diagnostic and therapeutic endoscopy 2014:309618.
- Draganov p, evans w, fazel a, forsmark c (2009) Large size balloon dilation of the ampulla after biliary sphincterotomy can facilitate endoscopic extraction of difficult bile duct stones. Journal clinic of gastroenterology. 43(8): 782-786.
- Sackmann m, holl j, sauter gh, J Pauletzki, C von Ritter, G Paumgartner et al. (2001) extracorporeal shock wave lithotripsy for clearance of bile duct stones resistant to endoscopic extraction. Gastrointest Endosc 53(1): 27-32.






























