Cavernous Lymphangioma Mimicking Hydatid Cyst
Gaurav Singhal, Tanvi Kanungo, Dipesh Goel, Iti Bhardwaj and Sathish, Prateek Sharda*
Maharishi Markandeshwar university, Sarada hospital, Thana Road, Meham ditrict-rohtak, Haryana, India
Submission: June 14, 2023; Published: July 10, 2023
*Corresponding author: Prateek Sharda, Institute of MMIMSR, Mullana, Ambala, Maharishi Markandeshwar university, sarada hospital, thana road, meham ditrict-rohtak, Haryana, india, E-mail: prateeksharda2006@gmail.com
How to cite this article: Gaurav S, Tanvi K, Dipesh G, Iti Bhardwaj, Sathish, Prateek S. Cavernous Lymphangioma Mimicking Hydatid Cyst. Open Access J Surg. 2023; 14(3): 555889. DOI: 10.19080/OAJS.2023.14.555889.
Abstract
Lymphangioma is a benign vascular lesion with characteristics of sub epithelial tumour which can proliferate in the lymphatic system. Lymphangioma of the retroperitoneal area is rare. We recently experienced a case of Cavernous Lymphangioma in a 51yr old male who was misdiagnosed as having a Hydatid Cyst. The final diagnosis was confirmed by pathologic examination of the specimen that was obtained by exploratory laparotomy. Herein we report a very rare case of retroperitoneal cavernous Lymphangioma.
Keywords: Lymphangioma; Chronic inflammatory cells; Retroperitoneal cystic lesion; Host tissue; Laparoscopy
Introduction
Lymphatic system neoplasm known as lymphangiomas affect the skin and subcutaneous tissues. Lymphangiomas can be divided into three types: Lymphangioma simplex, cavernous Lymphangioma and cystic Lymphangioma [1]. Cavernous Lymphangioma is also known as cystic Lymphangioma, cystic hygroma or Lymphangioma cavernosum, is a benign tumour characterised by large dilated lymphatic channels with an attenuated endothelial lining which could be in some cases surrounded by an irregular discontinuous smooth muscle layer [2]. The etiology of cavernous lymphangioma is regarded as a developmental malformation in which obstruction or agenesis of lymphatic tissue results in lymphangiectasia, secondary to lack of normal communication of the lymphatic system, which are particularly frequent in Turner’s and other malformative syndromes [3].
Case Presentation
A 51-year-old male was apparently well 2years back when he developed swelling in the left iliac region which was gradual in onset and progressively increased in size. The swelling was aggravated on sitting and got relieved on applying pressure. Since, the past two months the patient has started experiencing multiple episodes of non-radiating, shooting pain, on and off around the day in left lower limb, which was relieved on rest and medication. The patient has no significant past medical or surgical history with no such episodes in family too. His physical examination revealed a single globular swelling 8 to 10 cms in diameter extending from umbilical to left iliac region, non-tender, non-fluctuant, non-reducing, not moving with respiration and neither any fixation to skin. The swelling had a dull note on percussion and size can’t be commented due to large size. Concerning the symptoms and involved organs, analysis of blood biochemical parameters was prescribed for the patient. Lab investigations seem to be normal. USG whole abdomen suggestive of large well defined cystic lesion with septations and echogenic content within it. CECT whole abdomen suggestive of large multiloculated, multiseptated seen in the left iliac region measuring 15x11cm in cross section and approximately 15cm in cranio-caudal, likely retroperitoneal, query hydatid cyst. Gasoline report was negative. Patient was planned for exploratory laparotomy; tumour was excised in toto and sent for histopathology examination. Post -operatively patient was managed by IV antibiotics and analgesic. Daily aseptic dressings were done. HPE revealed Cavernous Lymphangioma, spaces lined by flattened endothelium, fibrous septa containing chronic inflammatory cells, congested blood vessels and multifocal hemosiderin deposition. No evidence of malignancy noted in sections (Figures 1-4).
Discussion
Initial differential diagnosis for this case included a hydatid cyst, abscess and cavernous Lymphangioma. To differentiate this diagnosis, and we obtained a CT scan. CT demonstrated large multiloculated, multiseptated lesion in the left iliac region measuring 15X11cm in cross-section and approximately 15cm in cranio-caudal. Imaging was not consistent with typical appearance of abscess, simple cyst or hydatid cyst. It clearly demonstrates the hydatid sand, floating membranes, daughter cysts, and vesicles inside the cyst. Additionally, hydatid cyst is most often found within the liver [4]. When a lymphangioma is confined to fairly dense tissue, it presents as a cavernous lymphangioma, but when it develops in the relatively loose fascia of the neck, a cystic lesion occurs. Cystic hygromas, however, account for approximately 90% of the lymphangiomas in the head and neck region. Other common sites, outside the head and neck, include the axilla, shoulder, chest wall, mediastinum, abdominal wall, and thigh [5].
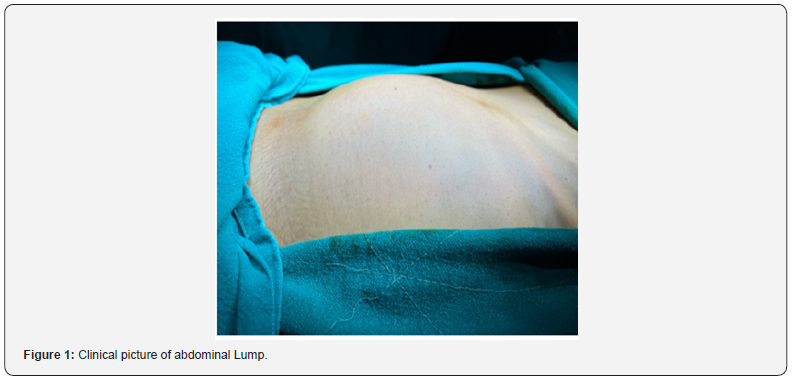

Pre-operative diagnosis of retroperitoneal lymphangioma, in general, is challenging and rare, prior to laparotomy or laparoscopy. The diagnosis of lymphangioma, based on the radiographic modalities, is generally one of many potential differentials for a multiloculated cystic mass arising retroperitoneally [6]. Surgical resection remains the best treatment for lymphangiomas; other treatment options, such as sclerotherapy have been proposed as an alternative to reduce the impact and complications of surgery [7]. T Harashima et al. concluded in their study that if Nd: YAG laser therapy is used for reducing the tumour size as a primary treatment, the operation becomes easy, and the recurrence may be less than with the conventional treatment [8]. Riitta Rautio et al. showed that treatment of lymphangiomas with OK-432 was safe and effective [9].
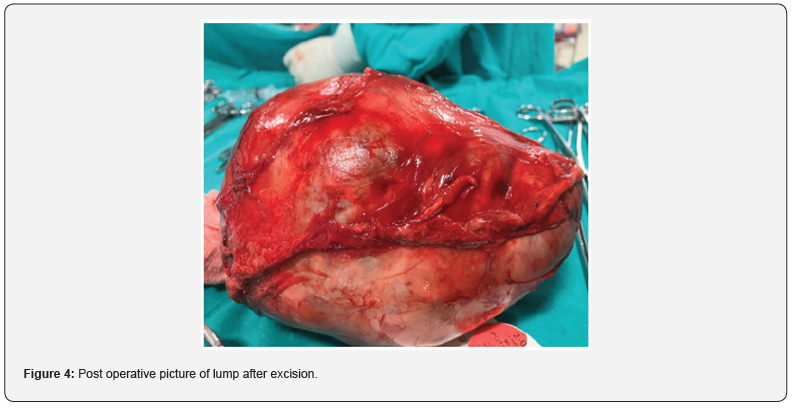
Patient was taken up for excision. On direct visualisation of the cyst, it appeared translucent with cystic fluid. In contrast, hydatid cyst would appear round or ovoid with opaque walls within a fibrous peri cyst formed from host tissue. The diagnosis of macrocytic Lymphangioma was confirmed on final pathology. In conclusion, lymphangioma, should be considered among the many different possible diagnoses of a retroperitoneal cystic lesion.
References
- Rathan JJ, Vardhan BG, Muthu MS, Venkatachalapathy, Saraswathy K, Sivakumar N et al. (2005) Oral lymphangioma: A case report. J Indian Soc Pedod Prev Dent 23(4): 185-189.
- Beham A (2002) Lymphangioma. Pathology and Genetics. Tumours of Soft Tissue and Bone, CDM Fletcher, KK Unni, F Mertens. IARC Press, Lyon pp. 162-163.
- Beham A (2002) Lymphangioma. In: Fletcher CDM, Unni KK, Mertens F, editors. Pathology and Genetics. Tumours of Soft Tissue and Bone. Lyon: IARC Press pp. 162-163.
- Mehta P, Prakash M, Khandelwal N (2016) Radiological manifestations of hydatid disease and its complications. Trop Parasitol 6(2): 103-112.
- Ward FE, Hendrick JW, Chambers RG (1950) Cystic hygroma of the neck. West J Surg Obstet Gynecol 58: 41-47.
- Hauser H, Mischinger HJ, Beham A, Berger A, Cerwenka H, et al. (1997) Cystic retroperitoneal lymphangiomas in adults. Eur J Surg Oncol 23: 322-326.
- Grasso DL, Pelizzo G, Zocconi E, Schleef J (2008) Lymphangiomas of the head and neck in children. Acta Otorhinolaryngol Ital 28(1): 17-20.
- Harashima T, Hossain M, Walverde DA, Yamada Y, Matsumoto K (2001) Treatment of lymphangioma with Nd: YAG laser irradiation: a case report. J Clin Laser Med Surg 19(4): 189-191.
- Rautio R, Keski-Nisula L, Laranne J, Laasonen E (2003) Treatment of lymphangiomas with OK-432 (Picibanil). Cardiovasc Intervent Radiol 26(1): 31-36.






























