Small Bowel Perforations- Indian Experience
Keshav Jindal1*, Manmohan Bhardwaj1, Sanjay Gupta2 and Attri AK2
1 Senior Resident, Department of Surgery, Government medical college, Chandigarh, India
2 Professor, Department of Surgery, Government medical college, Chandigarh, India
Submission:May 02, 2023; Published: May 12, 2023
*Corresponding author: Keshav Jindal, Department of surgery, Government medical college, Chandigarh, India, Email id: keshav.jindal.19@gmail.com
How to cite this article: Keshav Jindal, Manmohan Bhardwaj, Sanjay Gupta, Attri AK. Small Bowel Perforations- Indian Experience. Open Access J 002 Surg. 2023; 14(3): 555886. DOI: 10.19080/OAJS.2023.14.555886.
Abstract
Background: Very few studies are available in English literature that has evaluated the outcome following small bowel perforations (SBP) in developing countries like India. The present study aims to know the latest trend in aetiology of SBP and to identify the risk factors that are associated with worse outcome.
Methods: Data of 100 patients with SBP was maintained prospectively. Specific investigations like Widal, blood culture, urine culture, histological examination of margins of perforation or enlarged lymph nodes were done to identify the cause of SBP. Based on Clavein- Dindo classificationof post-operative complications, patients with Grade III and above complications were compared with patients having no or < Grade III complications, to identify the factors that can predict outcome following SBP.
Results: In 53% of the cases no specific aetiology could be found, and these were labelled as ‘non-specific’; enteric fever was diagnosed in 34% and tuberculosis was found in 10% of patients. Overall mortality was 14% and morbidity was 34%. Combination of serum lactate (>2meq/l), respiratory rate (>20/min) and serum potassium levels (>5.5meq/l) with sensitivity of 93.94%, was found to be better predictor of severe complications as compared others parameters like aetiology, operative procedure and commonly used prognostic scoring system -Mannheim Peritonitis Index (MPI).
Conclusion: ‘Non-specific’ perforations account for majority of SBP. However, these should preferably be managed like enteric as diagnostic yield of various tests for enteric fever is low. Hyperlactemia in presence of hyperkalaemia and hyperventilation reliably predicts prognosis in patients with peritonitis secondary to SBP.
Keywords: Small bowel; Perforation; Enteric; Hyperlactemia
Introduction
Intestinal perforation is one of the common emergencies encountered by surgeons world over. There is regional bias in the frequency and incidence of intestinal perforations, with small bowel perforations (SBP) being encountered more frequently in the developing countries, and colonic perforations in the developed nations [1]. The etiological spectrum of non-traumatic SBP in the developing world is also different from the western world. Ileal perforation secondary to enteric fever or tuberculosis is common in developing countries whereas in western countries causes include malignancy, trauma, radiation enteritis, adhesions, ischemic enteritis, systemic lupus erythematosus (SLE), Crohn’s disease and very rarely, intestinal tuberculosis [1,2]. In developing countries like India, enteric fever being endemic is considered as the leading cause of SBP. But there are studies found that large number of these perforations are in fact ‘non-specific’ in nature which occur secondary to sub-mucus vascular embolism, chronic ischemia due to atheromatous vascular disease or arteritis, or drugs such as enteric coated potassium tablets [3,4]. Tuberculosis of small bowel is another common cause of small bowel perforation. Most common site of tubercular perforation is ileum (50 – 80 %), which is usually seen proximal to stricture site. Other causes rare include diverticular perforation, perforation secondary to hernia or foreign body ingestion [1,5].
Despite advances in management strategies, the morbidity and mortality associated with small bowel perforation is significantly high. Morbidity rate varies between 50-80% and mortality is quoted to be as high as 40% [6,7]. The prognosis and outcome in these patients depend on the complex interaction of various factors i.e., patient related, disease related, and intervention related. Early risk assessment of these patients by accurate and reliable methods can improve clinical outcome and reduce treatment costs. Limited studies are available in the English literature which have evaluated the role various risk factors and scoring systems in peritonitis secondary to SBP. The present study was therefore, designed to know the latest trend in aetiology of SBP and to identify risk factors that can accurately predict disease severity.
Methodology
After institutional ethical committee approval, this prospective observational study was conducted on 100 patients of SBP admitted to tertiary health care institute of North India from November 2018 to August 2020. The sample size was calculated based on 5% level of significance and 90% power with an alpha error of 0.05 taking into consideration sensitivity of MPI as 92%. All adult patients (>18 years) who consented to participate and operated for SBP were only included. Patients with SBP secondary to trauma and patients who had pre-existing condition that can alter CRP levels like rheumatoid arthritis, inflammatory bowel disease or lupus were excluded. Patient particulars, symptoms and clinical features on admission, pre-operative investigations, operative findings, and post-operative course was recorded. Based on preoperative investigations and operative findings, Mannheim Peritonitis Index (MPI) was calculated and MPI of > 26 was taken as indicator of severe disease [8].
Specific investigations like Widal, blood culture, histopathology of margins of perforation and enlarged lymph nodes were done to confirm the aetiology of SBP. Perforation of ileum in the background of any one of the criteria was labelled as ‘enteric’- (i) acute onset of fever for more than 7 days of duration; (ii) positive Widal test (TO antigen titre > 1:160) and; (iii) positive blood or urine culture positive for S.typhi. In absence of these criteria or any specific finding on histological examination, the perforations were labelled as ‘non-specific’. As per our institute policy ‘non-specific’ perforations were presumed to be enteric in nature and were treated similarly. All patients before surgery patients were resuscitated and were given broad spectrum parenteral antibiotics. During surgery, the site of perforation was confirmed, and the extent and type of contamination was recorded. Type of procedure (ileostomy, primary repair, or resection anastomosis) was left to surgeons’ discretion. Post-operatively these patients were given third generation cephalosporin (Ceftriaxone 2gm intravenous BD or Cefixime 400mg orally BD). This was continued for 14 days in patients found to have enteric or ‘non-specific’ perforation.
During post-operative course, major complications including mortality occurring within one month of surgery were stratified according to the Clavein- Dindo classification [9]. Grade III and above complications were considered as severe and were compared with patients having no or < Grade III complications, to identify the factors that can predict severity of peritonitis following SBP. The Collected data was analysed using SPSS software (Chicago, IL). Categorical variables were expressed as numbers and percentages. Comparison among groups (mild/severe peritonitis) were made with the Pearson’ chi-squared test or Fisher’s exact test. Continuous data was expressed as mean ± standard deviation or median and inter-quartile range. For multivariate analysis, logistic regression model was applied. Receiver operating characteristic curves were used to find cut off with highest sensitivity and specificity. P –value of <0.05 was taken as significant.
Results
Of 100 patients who presented with SBP, there were 69 males and 31 females. The mean age was 34.12 SD 14.66 years. Most common type of perforation was ‘non- specific’ in 53 patients followed by enteric perforation in 34 patients; 10 patients had tubercular perforation and 1 each had ascariasis, duodenal hypertrophy, and intestinal endometriosis on histological examination. Among patients with enteric perforation, 16 had acute onset fever of more than 7 days; 14 were Widal positive and 4 had both, positive Widal and fever. In none of the patient blood and urine culture was positive for S.typhi. Loop or end ileostomy was done in most of the patients (82%) followed by primary repair (13%) and resection anastomosis (5%). Post operatively 34 patients had Grade III or more complication (64 in total including 14 mortalities). Most common complication was related to respiratory tract (22; 34.37%) followed by wound dehiscence (31.2%), intraabdominal abscess (15.6%), leak from anastomotic or repair site (9.3%) and others. Overall mortality was 14%; 08 died from multi organ failure (71.4%) whereas 5 (35.7%) died from respiratory complications and 1(7.1%) from cardiac event.
Predictors of Severity
<Various factors were analysed that can predict severity of complications. Univariate analysis revealed increased incidence of severe complications in patients who had high arterial lactate (AL) on admission (>2mmol/l), increased respiratory rate (RR)(>20/min), abnormal serum potassium(K+) (>5.5 meq/l) and in those who had MPI >26 (Table 1). This difference was also found to be significant on multivariate regression analysis. Other factors like age, gender, duration of symptoms, blood pressure, heart rate, blood urea, serum creatinine, serum bilirubin, etiology of perforation and type of surgery do not contribute significantly to severe complications. Receiver operating characteristic curve was constructed for significant variables to identify best cut off, sensitivity, specificity, positive predictive value, negative predictive value, and accuracy (Table 2; Figure 1 & 2). MPI (>28.5) had highest sensitivity of 73.53% with an area under curve (AUC) of 0.329, in predicting severe form of peritonitis as compared to others. On further analysis, it was found that sensitivity of combined AL, RR and K+ (AUC- 0.783) was significantly more as compared to MPI (93.94 %vs 73.53%), with an accuracy of 79%.
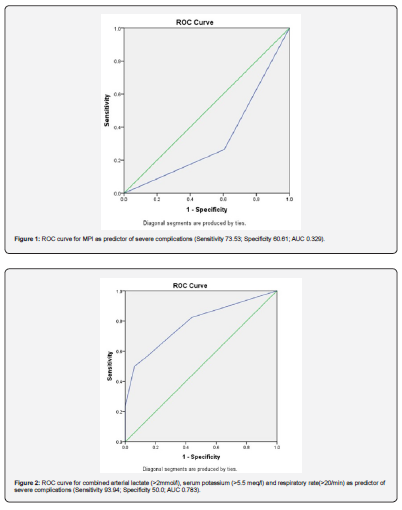
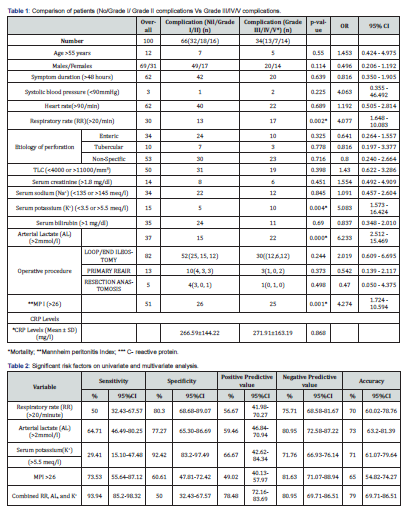
Discussion
SBP secondary to enteric fever is considered as one of leading cause of SBP in developing nations. Though enteric fever is endemic in developing nations like India (incidence 493.5 cases per 100000 per year of all ages) its diagnosis poses a significant challenge to treating physicians [10]. The clinical presentation of enteric fever is highly non-specific and available diagnostic tests have low sensitivity. Isolation of S. typhi and S. Paratyhpi from blood, urine bone marrow, stools or intestinal secretions is considered as diagnostic but sensitivity of this ranges from 40-80% because of high rate of self-antibiotic use [11]. The Widal and other new generation serological test like typhidot and tubex have also been found to be unreliable. Typhoid-paratypoid assay that detects IgA, is only test that is found to be promising and has sensitivity of 100%, but this is usually not available in emergency setting [10]. Due to these reasons, it is usually difficult to make diagnosis of enteric fever as a cause of SBP and these perforations can erroneously be labelled as ‘non-specific’ in absence of any specific cause. It is probably because of this reason few authors have reported high incidence ‘non-specific’ SBP as compared to enteric perforations [3,4].
In present series, we also had similar observation. Non-specific perforations (51%) were found to be more as compared to enteric perforations (36%). But as diagnostic tests for enteric are unreliable, all ‘non-specific’ perforations were presumed to be enteric and treated accordingly. Intestinal tuberculosis (ITB) is another common cause of SBP. Though it is usually seen in developing nations, increased incidence is reported from western world because of human immunodeficiency virus (HIV) prevalence. ITB usually affects ileo-caecal region because of abundance of lymphatic tissue and increased stasis of contents in this area. Incidence of SBP secondary to intestinal tuberculosis varies from 1-11% and majority these perforations occur secondary to over distension of bowel caused by distal stricture. True or ‘Free’ perforation of tubercular ulcer is rare phenomenon and only few cases have been reported in literature [12]. In present cohort, 10 patients were diagnosed with tuberculosis of small bowel on histological examination. Of these, five had free perforation of ileum in the absence of any other gross pathological feature. This strongly advocates the need for biopsy of margin of all SBP to avoid misdiagnosis. Other rare causes of SBP reported in the literature includes radiation enteritis, hernia, foreign body ingestion and to add to this list we found one case each of duodenal hypertrophy, intestinal endometriosis, and ascariasis.
There is no consensus on type of procedure to be done for SBP.
Simple closure, wedge excision or segmental resection and anastomosis, ileostomy, and even, side to side ileo-transverse anastomosis after primary repair of the perforation have been described in the literature. In this series ileostomy was fashioned in 82 patients. In our experience, we found that these patients have bowel oedema which makes it difficult for sutures to hold and therefore, exteriorization of the perforated segment as a 'loop' ileostomy should be preferred approach. Closure of this loop ileostomy can be done after 6 to 8 weeks. A primary anastomosis or simple closure should only be done when the patient presents early, and the bowel is healthy. Despite advancement in peri-operative care, peritonitis due to SBP is associated with significant morbidity and mortality. To improve outcome further, various authors attempted to identify risk factors and scoring systems that can reliably prognosticate the disease at time of admission. Of these, the Mannheim Peritonitis Index, which was specifically designed for peritonitis, is found to be most reliable marker for assessing severity and prognosis [8,13,14].
It takes into consideration both preoperative and operative factors to identify high risk patients. In present study, MPI>26 was found to reliably predict grade III and more complications (including mortality) in 73.5% of the patients. Apart from MPI, significant number of patients in severe complication group had increased serum lactate, hyperkalaemia and increased respiratory rate. Although, the sensitivity of these parameters when compared individually to MPI was low, the combined sensitivity was however, found to be higher (93.94% Vs 73.53%). Lactate levels as a tool to represent tissue hypoxia was first described by Broder and Weil in 1964 [15]. Lactate, a product of anaerobic glycolysis, is overproduced in patients with tissue hypoxia. Liver (60%) followed by kidney (30%) are major organs responsible for lactate clearance from the body. In presence of sepsis, decreased perfusion associated kidney and liver dysfunction can lead to increased lactate levels because of overproduction and decreased clearance [16]. Increased lactate level can lead to metabolic acidosis in presence of sepsis. To compensate for this, hyperventilation occurs to decrease levels of arterial pCO2 [17]. Complex alterations occur in potassium levels in response to sepsis. Hyperkalaemia can result because of reduced kidney function, presence of metabolic acidosis and increased cell turnover in septic patients [18]. Thus, Hyperlactemia associated with peritonitis can also result in hyperkalaemia and hyperventilation.
Several studies have found lactate level of >2mmol/l, as an independent predictor of survival in patients with mortality [19,20]. Based on data obtained from present study hyperlactemia alone was found to have low sensitivity as compared to MPI (64.71% Vs 73.53%). However, in presence of associated abnormalities like hyperventilation and hyperkalaemia its sensitivity is more than MPI. Therefore, combination of hyperlactemia, hyperkalaemia and hyperventilation can be considered as a better tool in predicting severe complications following SBP. Apart from sensitivity, MPI is also cumbersome to use as it relies on number of preoperative and intraoperative findings. Based on above observations, we recommend combined use of arterial lactate, serum potassium and respiratory rate as predictor of outcome in patients with SBP. But this study has its own limitations. The number of patients with abnormal potassium levels (>5.5 meq/l) and increased respiratory rate(>20/min) were very less. Therefore, large multicentric studies on similar group of patients is required before contribution of these parameters in predicting severe complications can be established.
Conclusion
Combination of hyperlactemia, hyperkalaemia and hyperventilation are an effective tool in predicting severe complications in patients of secondary peritonitis following SBP. Large multicentric studies are however, needed to further validate this before it can be routinely used to predict outcome.
References
- Gupta S, Kaushik R (2006) Peritonitis - the Eastern experience. World J Emerg Surg 1: 13.
- Freeman HJ (2014) Spontaneous free perforation of the small intestine in adults. World J Gastroenterol 29 : 9990-9997.
- Verma H, Pandey S, Sheoran KD, Marwah S (2015) Surgical Audit of Patients with Ileal Perforations Requiring Ileostomy in a Tertiary Care Hospital in India. Surgery Research and Practice 351548.
- Nekarakanti P, Elamurugan TP, Kate V (2014) Spectrum of small bowel perforation in a tertiary care hospital of south India: Predictors of morbidity and mortality. Indian J Gastroenterol 33(6): 575–577.
- Chaterjee H, Jagdish S, Pai D, Satish N, Jyadev D, et al. (2003) Pattern of nontyphoid ileal perforation over three decades in Pondicherry. Trop Gastroenterol 24: 144-147.
- Tan KK, Bang SL, Sim R (2010) Surgery for small bowel perforation in an Asian population: predictors of morbidity and mortality. J Gastrointest Surg 3: 493-499.
- Gedik E, Girgin S, Taçyildiz IH, Akgün Y (2008) Risk factors affecting morbidity in typhoid enteric perforation. Langenbecks Arch Surg 393(6): 973-977.
- Billing A, Fröhlich D, Schildberg FW (1994) Prediction of outcome using the Mannheim peritonitis index in 2003 patients. Peritonitis Study Group. Br J Surg 81(2): 209-213.
- Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, et al. (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2): 187-96.
- Wain J, Hendriksen RS, Mikoleit ML, Keddy KH, Ochiai RL (2015) Typhoid fever. Lancet 21: 1136-45.
- Mogasale, V Ramani E, Mogasale, VV et al. (2016) What proportion of Salmonella Typhi cases are detected by blood culture? A systematic literature review. Ann Clin Microbiol Antimicrob 15(1): 32.
- Gupta S, Jayant M, Kaushik R. Free tubercular perforation of the ileum. World J Emerg Med 4(3): 235-236.
- Budzyński P, Dworak J, Natkaniec M, Pędziwiatr M, Major P, et al. (2015) The usefulness of the Mannheim Peritonitis Index score in assessing the condition of patients treated for peritonitis. Pol Przegl Chir 7 (6): 301-306.
- Sharma R, Ranjan V, Jain S, Joshi T, Tyagi A, et al. (2015) A prospective study evaluating utility of Mannheim peritonitis index in predicting prognosis of perforation peritonitis. J Nat Sci Biol Med 6: S49-52.
- Broder G, Weil Mh (1964) Excess lactate: an index of reversibility of shock in human patients. Science 43(3613): 1457-1459.
- Jeppesen JB, Mortensen C, Bendtsen F, Søren Møller (2013) Lactate metabolism in chronic liver disease. Scand J Clin Lab Invest 73: 293-299.
- Ganesh K, Sharma RN, Varghese J, Pillai MG (2016) A profile of metabolic acidosis in patients with sepsis in an Intensive Care Unit setting. Int J Crit Illn Inj Sci (4): 178-181.
- Tongyoo S, Viarasilpa T, Permpikul C (2018) Serum potassium levels and outcomes in critically ill patients in the medical intensive care unit. J Int Med Res 46(3): 1254-1262.
- Lee SM, An WS (2016) New clinical criteria for septic shock: serum lactate level as new emerging vital sign. J Thorac Dis 8(7): 1388-1390.
- Shankar-Hari M, Phillips GS, Levy ML, Seymour CW, Liu VX, et al. (2016) Sepsis Definitions Task Force. Developing a New Definition and Assessing New Clinical Criteria for Septic Shock: For the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 23: 775-787.






























