Acute Porto-Mesenteric Venous Thrombosis after Sleeve Gastrectomy
Freund A*, Elshafei M, Aktas S and Weiner S
Departement of Obesity and Metabolic Surgery, Nordwest Hospital in Frankfurt, Germany
Submission:February 13, 2022; Published:February 22, 2022
*Corresponding author: Freund A, Departement of Obesity and Metabolic Surgery, Nordwest Hospital in Frankfurt, Germany
How to cite this article: Freund A, Elshafei M, Aktas S, Weiner S. Acute Porto-Mesenteric Venous Thrombosis after Sleeve Gastrectomy. Open Access J Surg. 2022; 13(5): 555872 DOI: 10.19080/OAJS.2022.13.555872.
Introduction
Acute Portal Vein Thrombosis (PVT) is defined as a recent formation of a thrombus within the portal vein trunk and/or right or left intrahepatic branches. The thrombus may extend into the mesenteric or splenic veins; occlusion may be complete or partial [1]. The underlying pathophysiology is the Virchow’s triad which includes endothelial damage, stasis, and hypercoagulability. PVT most often occurs in patients suffering from a liver pathology (e.g., cirrhosis) or due to a vessel damage during a surgical procedure. PVT can occur in combination with mesenteric thrombosis as well. Few cases of Portal Mesenteric Vein Thrombosis (PMVT) have been described in the literature [2]. The Pathogenesis of PMVT remains unclear and the conditions is described after different laparoscopic surgeries. The intraabdominal pressure during laparoscopy has an inverse relation with the blood flow within the portal vein, the release of Vasopressin during the surgery and the anti-Trendelenburg position might be contributing factors [3]. Therefore, a reduced flow in the portal vein can lead to a PVT. Different hematological condition such as hereditary thrombophilia can increase the risk of PVT by being a hypercoagulable state [4]. Multiple risk factors have been mentioned in literature [5]. Due to the different clinical pictures (acute and chronic) the symptoms of a PVMT might range from acute abdominal pain to the complete absence of symptoms, which makes the diagnosis challenging. The most frequently observed symptoms include acute abdominal pain, nausea, vomiting, and/or melena. A systemic inflammatory response syndrome is present in 85% of patients diagnosed with acute portal vein thrombosis which contrasts with local or systemic infection being present in only 20% of these patients. Blood tests of the liver generally show no, or only mildly and transient abnormalities. Ascites is present in 50% of patients [1,6]. Acute obstruction of the superior mesenteric vein and mesenteric arches can lead to intestinal ischemia, and life-threatening infarction. Following acute complete occlusion of the portal vein there is intense compensatory hepatic arterial vasodilatation (“arterial rescue”) that stabilizes liver function [7]. A definitive diagnosis of PVT can be established with Computed Tomography (CT) scanning, which shows the filling defect [8].
Case Presentation
Our patient is a 52-year-old male with a history of Vitamin D and Float deficiency as well as severe obstructive sleep apnea presented with relevant respiratory insufficiency on our obesity center. Due to his super-obesity with a BMI of 69,6 kg/m2 he was hospitalized and underwent a 3-week conditioning with Stier-Schema (Liraglutid injections, AminoHepar and low-calorie diet) leading to a weight losss of 12 kg. Prophylaxis for thromboembolism was given twice a day 60mg Enoxaparine. During the usual preoperative tests (ECG, gastroscopy and lung function, as well as sleeping laboratory) a C-PAP mask was administered during the night to increase his lung ventilation. Finally, he underwent a laparoscopic sleeve gastrectomy. The postoperative course including laboratory blood results, ultrasound and oral intake of liquids was normal, and the patient was discharged as planned on the 4th postoperative day under thromboembolic prophylaxis with Clexane 40mg 1x per day for the following 3 weeks and well as Protone Pump Inhibitors (PPI) for 6 months. On postoperative day 8, the patient consulted the emergency department with a two-day history of postprandial abdominal epigastric pain, nausea, and vomiting. Physical examination showed a painless, soft and non-distended abdomen with normal bowel sounds. In the laboratory we found elevated infection parameter (CRP 171mg/l and a leukocytosis of 12,69/nl). No elevated lactate acid. A Computer Tomography (CT) scan of the abdomen and pelvis with intravenous contrast revealed an extended thrombosis of the portal vein with occlusion and thrombosis of the entire superior mesenteric vein and their branches as well as inferior mesenteric vein. A small thrombus was found in the lineal vein, which had normal perfusion. No edematous changes of the jejunum or ileum were detected (Figure 1-3). Due to the ongoing COVID-19 pandemic an admission to the intensive care unit was not possible in our hospital nor the surrounding hospitals up to 100km distance. Therefore, the patient was hospitalized on a standard surgical ward. Intravenous administration of antibiotic prophylaxis was administered, and full heparinization PTT monitoring was applied for the management of superior mesenterial thrombosis and portal vein thrombosis. A lysis therapy was discussed with the colleagues of the vascular surgery, angiology, and interventional radiology department. Local lysis as well as systematic lysis was estimated as too risky with the stable patient, thrombectomy at a BMI of still 62 kg/ m² was considered as too invasive management with the stable patient, too. As the patient remained throughout asymptomatic, we continued the treatment with heparin und frequent laboratory studies testing the infection signs, lactic acid and PTT.
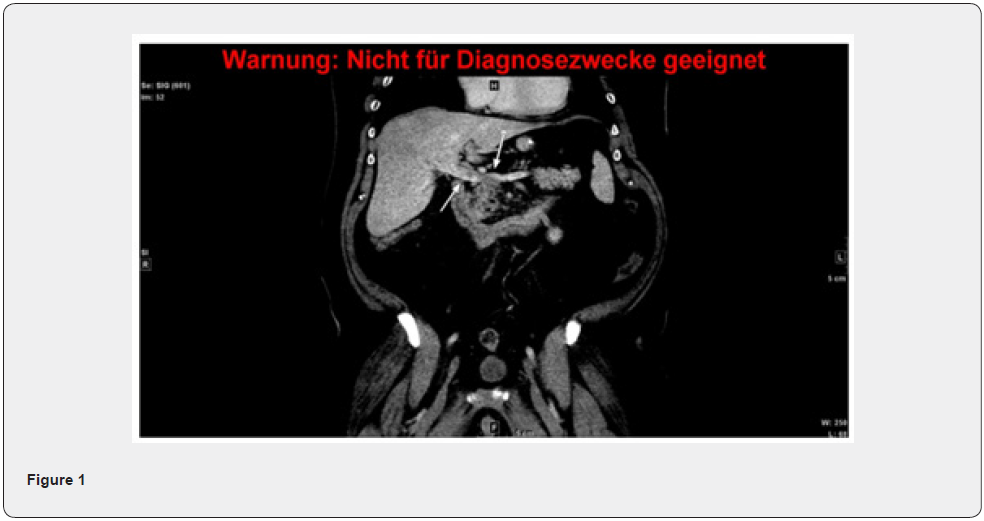
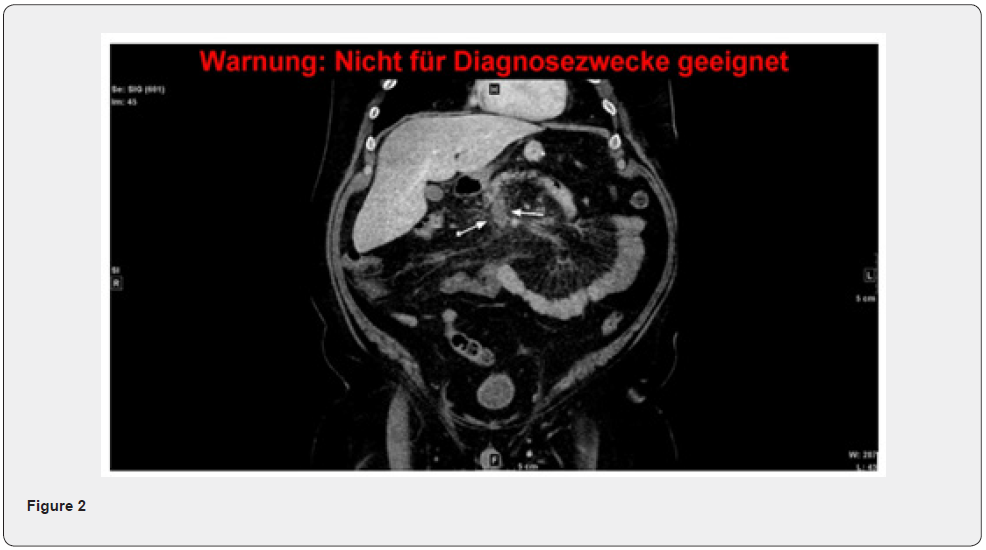
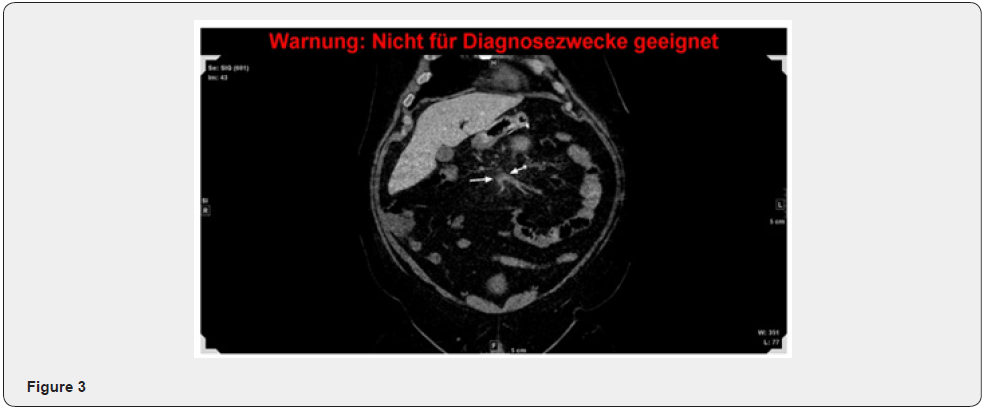
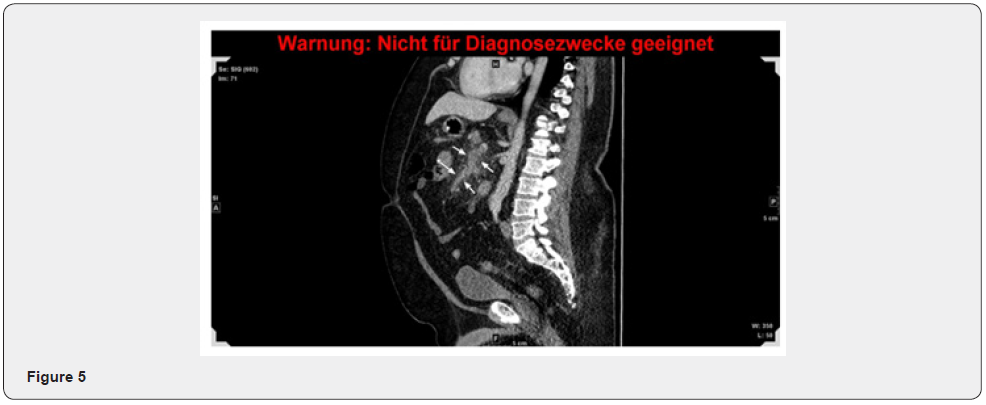
The further hospital stay showed no further symptoms; therefore, a fluid diet was restarted. After 10 days the intravenous antibiotic therapy was stopped and the anticoagulation therapy with Xarelto was started, initially 30mg per day and after 3 weeks 20mg per day under PPI therapy. The anticoagulation therapy will be continued for 6 to 12 months. Our patient was discharged after 10 days in stable and asymptomatic condition. Two weeks after discharge, the patient was re-evaluated in our outpatient clinic, including a CT scan of the abdomen. The scan showed a very small reduction of the thrombosis of the portal vein, as well as the superior mesenterial vein and lineal vein. The laboratory parameters were all at normal range. (Figure 4,5). Subsequent tests for inherited thrombophilia will be done in 3-month time, as well as a MRT follow up of the thrombosis.
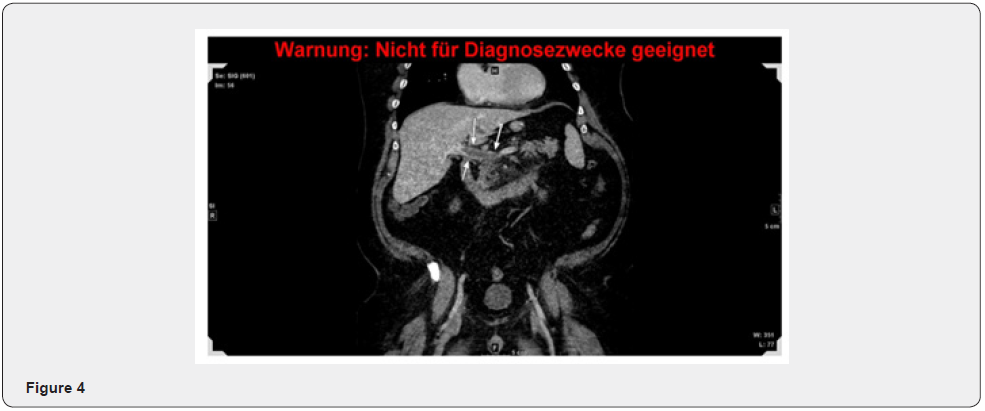
Discussion
Acute obstruction of the portal vein, superior mesenteric vein and mesenteric arches can lead to intestinal ischemia, and lifethreatening infarction and is therefore a vascular emergency [7]. As in our patient the thrombosis extended into the mediastinal veins a thrombolysis was discussed with the colleagues of the vascular surgery, angiology, and interventional radiology department. In the literature review, the experience of local thrombolysis, either venous or arterial, has been reported in no more than 100 patients, mainly as case reports. The transhepatic route or transjugular routes have been used. The reported re-canalization rates have been similar to those achieved with anticoagulation alone. However, 50% of treated patients developed procedure-related bleeding, with a fatal outcome in some [1,9-11]. The trans jugular approach for thrombolysis appears to be associated with reduced complications but the data remains limited to less than 30 treated patients [1,12,13]. surgical thrombectomy and re-canalization is achieved in only 30% of the patients. It is associated with a high recurrence rate, when performed >30 days from onset [1,14]. As the long-term outcome of patients with chronic PVT is generally good (five-year survival rate above 70%) and mostly related to the associated conditions, the risk to benefit ratio of such invasive procedures has to be considered [1,15]. The mortality rate for AMVT approaches 50% and therefore, anticoagulation therapy should be administered even in the presence of active bleeding [8]. Venous Thromboembolism is known as relevant complication after bariatric surgery. In registries the rate of deep venous thrombosis is described with 0.3%, whereas thromboembolic events had the highest impact of the rate of re-admissions and mortality (MBSAQIP registry). The incidence of portomesenteric vein thrombosis is only described in case reports and rarely investigated. Whereas the general risk of a thromboembolic event can be evaluated based on age, BMI, sex and history of previous events, as well as long operating times and late mobilization (BAriClot Modell), the incidence of portomesenteric vein thrombosis might be related to the procedure. Interestingly Thereaux et al have reported a higher rate in thromboembolic events (0,34%) in patients after sleeve gastrectomy, which occured with 30 days after surgery [16]. Therefore, prolonged medical thromboembolic with low-molecular heparine is to be recommended. The mounting applications of laparoscopic sleeve gastrectomy’s for patients with morbid obesity should urge health care professionals to investigate post-operative complications. Deep venous thrombosis, pulmonary embolism, hemorrhage, and anastomotic leakage are commonly reported complications in the postoperative course of laparoscopic sleeve gastrectomy [17- 20]. Porto-Mesenteric Vein Thrombosis (PMVT) is a potentially fatal complication after bariatric surgery; however, this has been rarely reported in literature and mostly as case reports. There are several reports on PMVT after sleeve, but only one after gastric bypass (in 3 cases) [21-25]. Moreover, the recommendation of medical prophylaxis of thromboembolism remains unclear in the guidelines. Many studies suggest the weight adjusted administration and a prolonged prophylaxis up to 30 days.
Conclusion
PMVT is a rare postoperative complication after Sleeve Gastrectomy, which can be life-threatening. Subsequent perioperative medical prophylaxis for thromboembolism should be administered but cannot prevent this condition in any case. Especially in high BMI patients the pneumoperitoneum itself, the anti-Trendelburg positioning and the extensive manipulation on the vessels, as well as pressure with liver retractor can influence the risk. Therefore, subsequent liver fasting preoperative might be supportive as well as low pressure laparoscopy. The management should be adapted on the overall condition of the patient, to decide for a therapeutic anticoagulation therapy instead of lysis therapy. PMVT is an emergency condition that requires continuous supervision and should be excluded in any patient presenting with unspecific symptoms within 30 days after bariatric surgery. So far there are no guidelines considering postoperative anticoagulation in high BMI patients, prospective studies are still needed to get clear consensus.
References
- (2015) EASL Clinical Practice Guidelines Vascular diseases of the liver. J Hepatol.
- Kerem Karaman (2018) Porto mesenteric venous thrombosis after laparoscopic sleeve gastrectomy A case report and systematic review of the 104 cases. Obes Res Clin Pract.
- U Haglund, K Norlen, I Rasmussen, JL Flowers (1995) Complications Related toPneumoperitoneum.
- Haris M, Thachil J (2017) Portal vein thrombosis a primer for the general physician. Clin Med (Lond) 17(3): 212-219.
- Harnik IG, Bradt LJ (2010) Mesenteric venous thrombosis. Vasc Med 15: 407.
- Dominik Jakob, Swantje Heidtmann (2017) Akute Mesenterialvenenthrombose. SCHWEIZERISCHES MEDIZIN FORUM 17(23): 500-504.
- Damian J Harding, M Thamara PR Perera, Frederick Chen, Simon Olliff, Dhiraj Tripathi Portal vein thrombosis in cirrhosis: Controversies and latest developments
- Mohamed Elnaggar, Jagmohan S Jandu, Bryce D Beutler, Sally Leong, Robert McCain Superior Mesenteric Vein Thrombosis in the Setting of Ileitis: Case Report and Literature Review.
- Smalberg JH, Spaander MV, Jie KS, Pattynama PM, Van Buuren HR (2008) Risks and benefits of transcatheter thrombolytic therapy in patients with splanchnic venous thrombosis. Thromb Haemost 100: 1084-1088.
- Ferro C, Rossi UG, Bovio G, Dahamane M, Centanaro M (2007) Transjugular intrahepatic portosystemic shunt, mechanical aspiration thrombectomy, and direct thrombolysis in the treatment of acute portal and superior mesenteric vein thrombosis. Cardiovasc Intervent Radiol 30: 1070-1074.
- Hollingshead M, Burke CT, Mauro MA, Weeks SM, Dixon RG, et al. (2005) Transcatheter thrombolytic therapy for acute mesenteric and portal vein thrombosis. J Vasc Interv Radiol 16: 651-661.
- Liu FY, Wang MQ, Duan F, Wang ZJ, Song P (2010) Interventional therapy for symptomatic-benign portal vein occlusion. Hepato gastroenterology 57: 1367-1374.
- Wang MQ, Liu FY, Duan F, Wang ZJ, Song P (2011) Acute symptomatic mesenteric venous thrombosis: treatment by catheter-directed thrombolysis with transjugular intrahepatic route. Abdom Imaging 36: 390-398.
- Malkowski P, Pawlak J, Michalowicz B, Szczerban J, Wroblewski T, et al. (2003) Thrombolytic treatment of portal thrombosis. Hepatogastroenterology 50: 2098-2100.
- Condat B, Valla D (2006) Non malignant portal vein thrombosis. Nat Clin Pract Gastroenterol Hepatol 3: 505-515.
- Plessier A, Darwish MS, Hernandez Guerra M, Consigny Y, Fabris F, et al. (2010) Acute portal vein thrombosis unrelated to cirrhosis: a prospective multicenter follow-up study. Hepatology 51: 210-218.
- D Fuks, P Verhaeghe, O Brehant, C Sabbagh, F Dumont, et al. (2009) Results of laparoscopic sleeve gastrectomy a prospective study in 135 patients with morbid obesity. Surgery 145(1): 106-113.
- F Caruso, G Cesana, L Lomaglio, S Cioffi, F Ciccarese, et al. (2017) Is portomesenteric vein thrombosis after laparoscopic sleeve gastrectomy related to short-course prophylaxis of thromboembolism? A monocentric retrospective analysis about an infrequent but not rare complication and review of the literature. J Laparoendosc Adv Surg Tech 27(10): 987-996.
- S Parikh, R Shah, P Kapoor (2010) Portal vein thrombosis. Am J Med 123 (2): 111-119.
- AA Gumbs, M Gagner, G Dakin, A Pomp (2007) Sleeve gastrectomy for morbidobesity. Obes Surg 17(7): 962-969.
- A W James, C Rabl, A C Westphalen (2009) Portomesenteric venousthrombosis after laparoscopic surgery a systematic literature review. Arch Surg 144(6): 520-526.
- L Belnap, G M Rodgers, D Cottam (2016) Portal vein thrombosis afterlaparoscopic sleeve gastrectomy presentation and management. Surg Obes Relat Dis 12(10): 1787-1794.
- J M Rosenberg, M Tedesco, D C Yao, D Eisenberg (2012) Portal vein thrombosisfollowing laparoscopic sleeve gastrectomy for morbid obesity. JSLS 16(4): 639.
- Naif Alenazi (2019) Porto-Mesenteric vein Thrombosis following laparsocopic sleeve gastrectomy for morbid obesity: Case series and literature review. International Journal of Surgery Case Reports 63: 59-64.
- Daniel E Swartz, Edward L Felix (2004) Acute Mesenteric Venous Thrombosis following laparoscopic RNYGB. JSLS 8: 165-169.






























