Complex Odontoma: Clinical Case
Francesco Briguglio*
Adjunt Professor, University of Messina, Italy
Submission:December 20, 2021; Published:December 29, 2021
*Corresponding author: Francesco Briguglio, Adjunt Professor, University of Messina, Italy
How to cite this article: Francesco B. Complex Odontoma: Clinical Case. Open Access J Surg. 2021; 13(4): 555870 DOI: 10.19080/OAJS.2021.13.555870.
Abstract
The term odontoma refers to a benign neoformation of the jaws, belonging to tumor lesions of odontogenic origin which, manifesting as self-limiting lesions, are also counted among the hamartomatous lesions. Although the exact etiology is not yet known, several possible causes have been proposed: local trauma, infections, genetic mutations. Most of these lesions appear to be an occasional finding during radiographic examinations performed for other purposes and can remain asymptomatic even for years. The therapy is surgical and consists in the removal of the neoformation; they do not tend to relapse. Here, a case of intraosseous compound odontoma is reported.
Keywords: Complex Odontoma; Odontogenic Tumor; Hamartoma
Introduction
Odontomas are lesions classified as benign odontogenic tumors, although in reality, as they do not present the typical proliferative aspect of tumors, they should be considered hamartomas. They appear as masses of completely calcified tissue, made up of enamel, dentin, and cement in a more or less disorganized manner [1]. The pathology represents 30% of odontogenic tumors and affects males more frequently (59%) than females (41%) between the second and fourth decade of life. From an etiological point of view, the causes of the onset of odontomas are fundamentally still unknown: mechanical, traumatic, or inflammatory factors would be the cause of these proliferations. The pressures exerted on developing dental germs resulting from the presence of supernumerary teeth, possible macrodontics or underdevelopment of the jaws with space reduction could also be important. There is a greater localization in the upper maxilla than in the mandible. Generally, the lesion is small, asymptomatic and the diagnosis is often occasional, in conjunction with radiological examinations performed routinely, or due to lack of dental eruption or due to anomalies in the position of the elements in the arch. Odontoma can manifest itself clinically in the advanced stages with ulceration of the mucosa due to trauma due to the superficializing of the lesion or to chronic osteitis following a secondary infection of the cavity. The patient’s attention is usually attracted by the swelling of the maxilla caused by the odontoma and covered by mucosa of normal appearance, of hard consistency, of various sizes and shapes, with an irregular surface, with fairly clear limits and generally not painful; there is no satellite lymphadenopathy.
Radiographically, the odontomas appear as a circumscribed, calcified formation with a fairly homogeneous appearance; this formation is clearly delineated by the surrounding bone which corresponds to the connective envelope that usually surrounds the neoformation [2]. According to the histological picture under the microscope, odontomas have been classified into:
Compound odontomas
Radiologically appear as irregular radiopaque masses attributable to small more or less developed dental structures surrounded by a radiolucent border and prefer the jaw in the anterior region. It is hypothesized that the onset of compound odontomas is due either to an overproduction of dental germs by the dental lamina or to the fragmentation of a single dental germ. The elective seat of the compound odontoma is the incisor-canine region [3]. The macroscopic aspect shows a mass delimited by a fibrous capsule and constituted by fibrous tissue containing bone trabeculae and an agglomeration of teeth or dental sketches of various numbers.
Complex odontomas
They appear as a single radiopacity with irregular margins and also in this case surrounded by a radiolucent border. They are most frequently located in the posterior region of the mandible. The macroscopic appearance is that of a rounded mass, often bumpy, no larger than a tooth (diameter about 1 cm) and therefore hardly causes jaw deformations; the outer surface is smooth and very thin. Microscopically, the lesion has a fibrous capsule that envelops a mass consisting of enamel, dentin and cement scattered irregularly. The presence of these lesions is not usually associated with agenesis of dental elements.
This work presents the case of an asymptomatic intraosseous compound odontoma.
Clinical Case
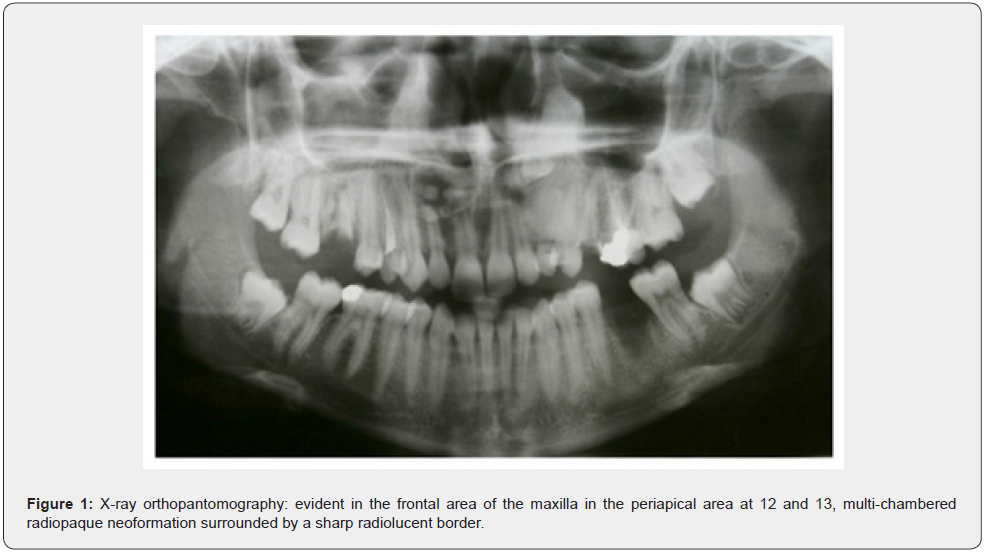
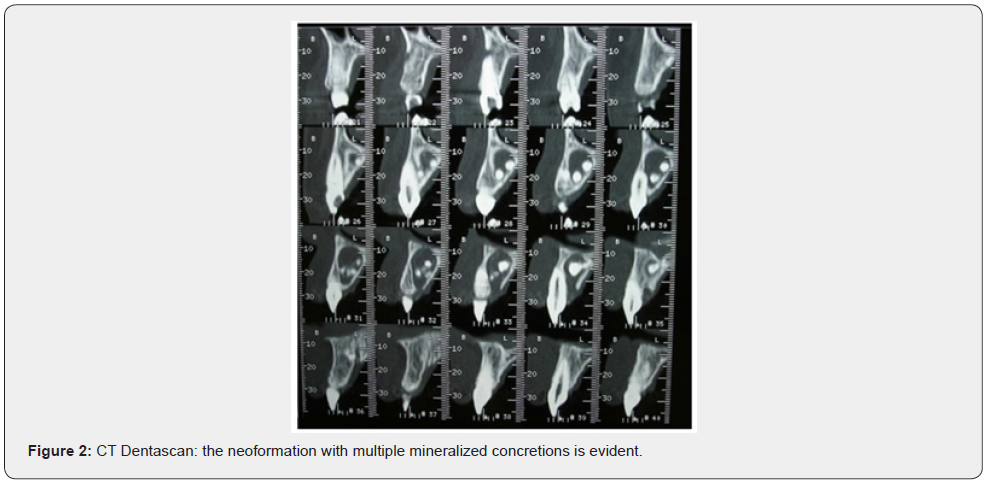
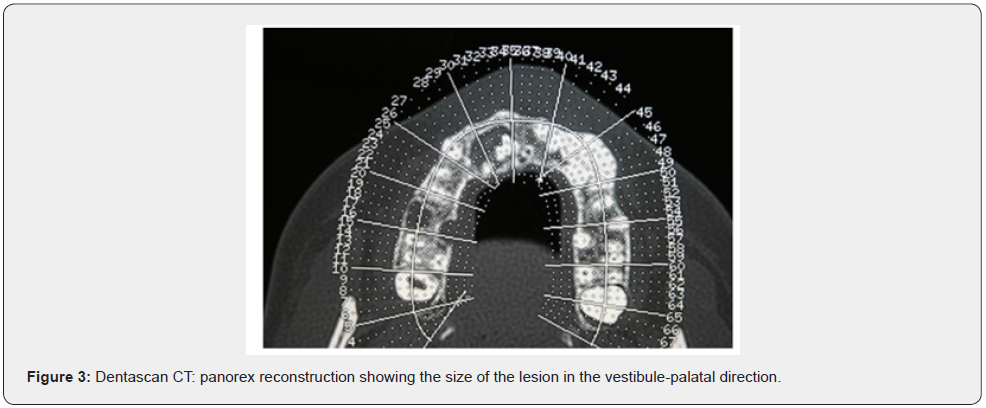
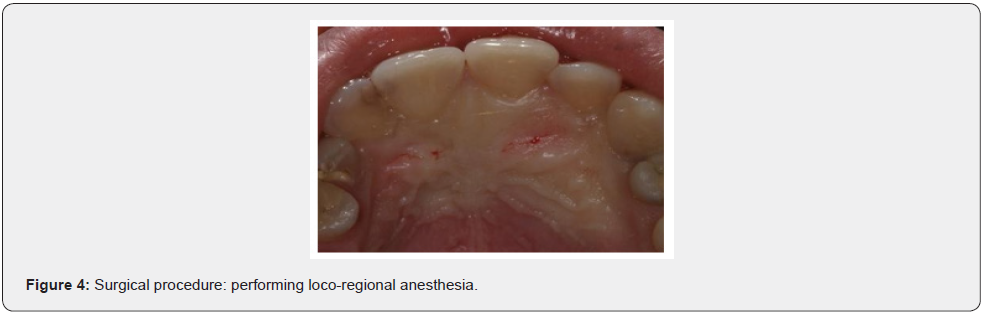
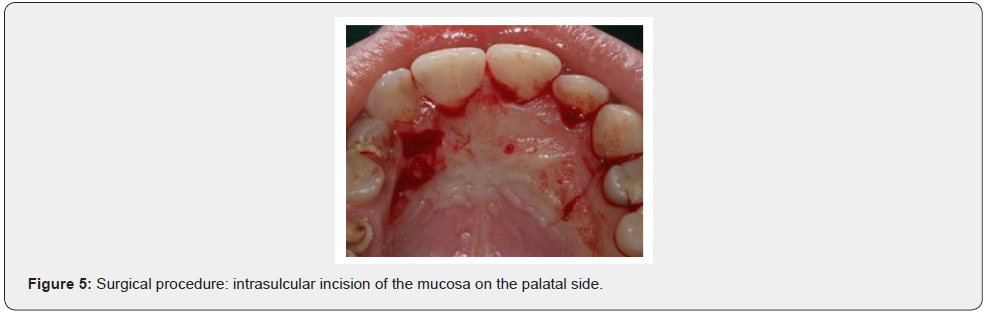
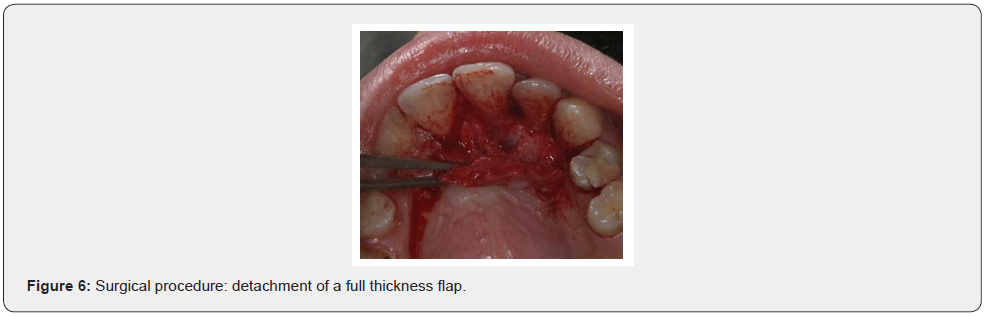
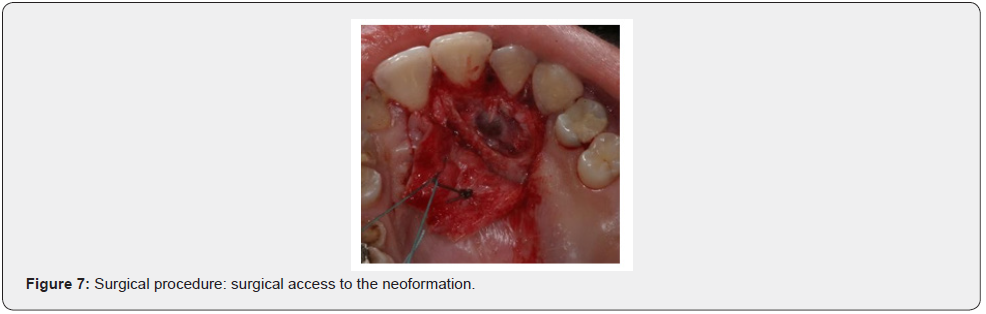
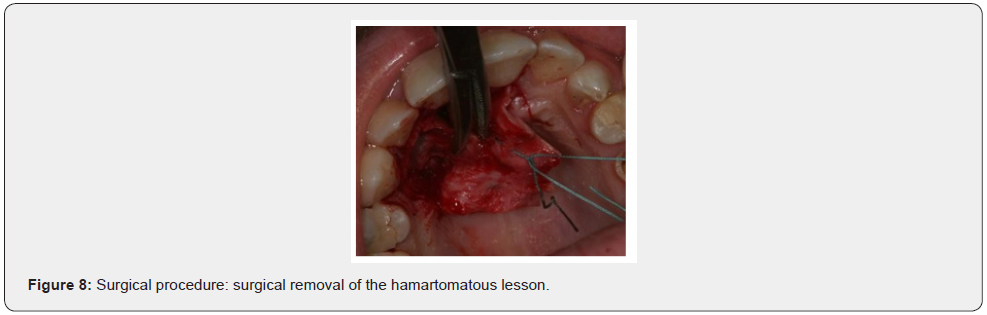
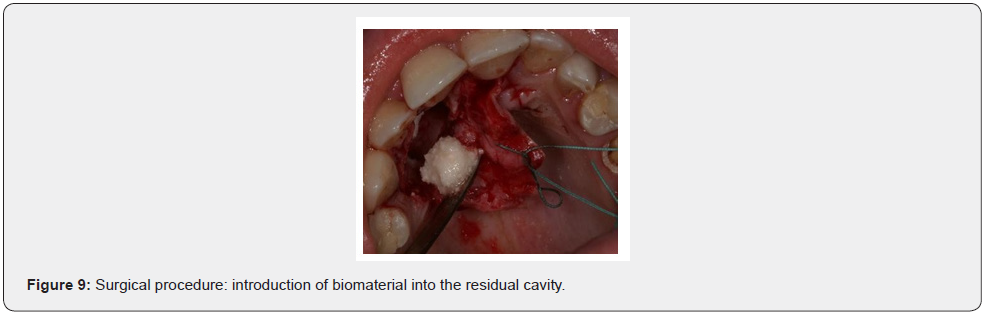
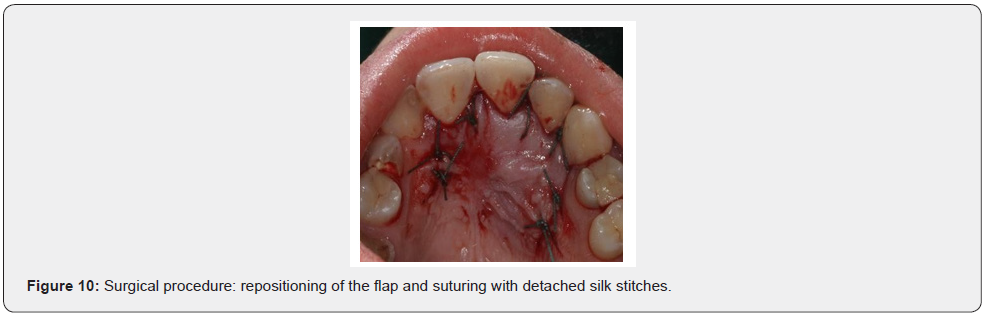
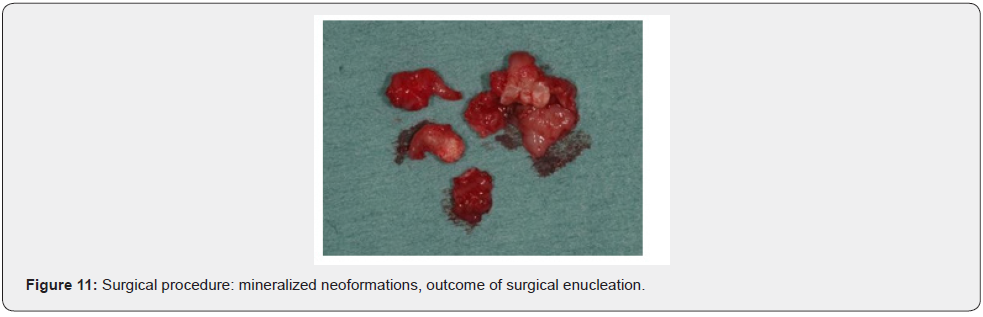
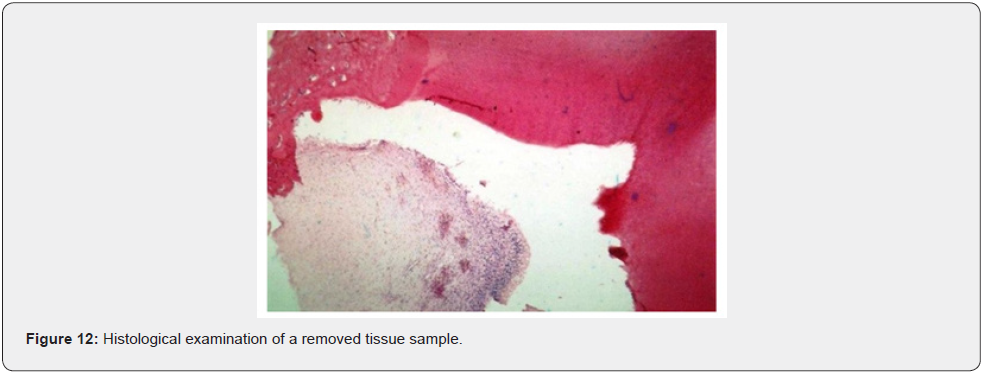
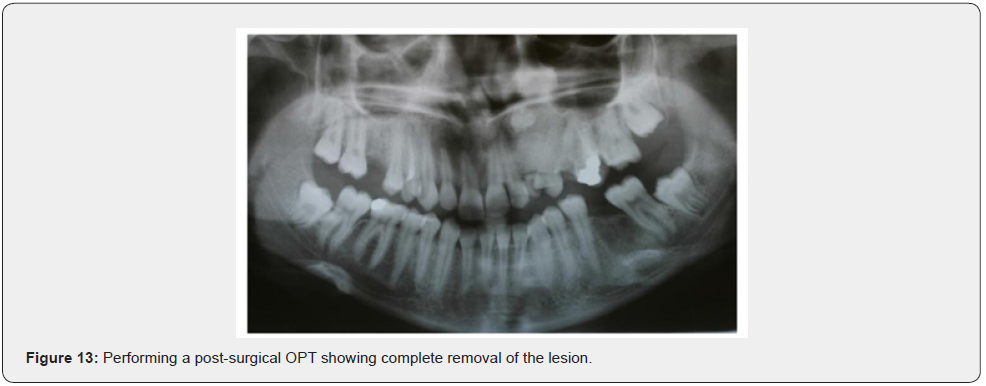
Patient of Caucasic race, male sex and age of 38 years comes to our observation for a bump in palatal side. The history was negative. On the extra-oral clinical examination, the face was symmetrical with non- palpable lymph nodes. The intra-oral clinical examination did not reveal anything particular for diagnostic purposes. An orthopantomography was performed which revealed the presence, in the frontal area of the upper jaw in the periapical region at 11 and 12, of an inhomogeneous multichambered radiopaque lesion well delimited by an osteosclerotic border (Figure 1). Computed tomography performed using a multidetector spiral technique, according to axial acquisition and subsequent panorex and parasagittal reconstructions, was very useful in the diagnosis and in the operative phase, which made it possible to carry out a complete and detailed evaluation of the extension and morphology of the neoformation and therefore a correct planning. intervention (Figures 2 and 3). Surgical removal of the odontoma was performed under loco-regional anesthesia (Figure 4). An intrasulcular incision of the mucosa was made on the palatal side (Figure 5) with subsequent detachment and elevation of a full-thickness flap which allowed to uncover the cortical bone (Figures 6 and 7). Once the bone breach was created that guaranteed direct access to the lesion, the latter was carefully removed by also carrying out careful curettage in order to remove it completely and thus avoid possible recurrence (Figure 8). In order, then, to promote complete wound healing, biomaterial was inserted into the residual cavity (Figure 9). Finally, the flap was repositioned, and a detached suture was performed (Figure 10). The numerous neoformations removed (Figure 11) were subjected to histopathological examination which confirmed the initial diagnosis (Figure 12). Upon completion of the surgery, a control orthopantomography was performed to ensure complete removal of the lesion (Figure 13).
Discussion
The term odontoma is reserved for those calcified odontogenic tumors in which epithelial and mesenchymal cells show complete differentiation, with the result that ameloblasts and odontoblasts form enamel and dentin. In accordance with the WHO, a compound odontoma is defined as “that malformation in which all dental tissues are represented in a more or less ordered way than the complex odontoma, forming more dental-like structures. Many of these structures do not morphologically resemble the teeth of the physiological dentition; however, enamel, dentin, cement and pulp are present “[1]. Their etiology still remains virtually unknown. These lesions are usually asymptomatic, and their discovery is accidental following the execution of a routine orthopantomography. In some cases, however, they can prevent the correct eruption of some dental elements or can cause infectious complications, caused by perforation of the cortical bone and communication with the oral cavity. Usually, compound odontomas appear as a set of tooth-like structures surrounded by a radiolucent zone [4]. Therefore, they can often be confused with any other similar entity, such as supernumerary teeth. In our case, the diagnosis was confirmed with the help of histopathological examination. The differential radiographic diagnosis must also be made with osteomas, with respect to which odontomas have a clearer demarcation with the surrounding bone and have a denser and more compact radiopacity; osteomas, in fact, have less clear peripheral limits and show a radiopacity more similar to that of bone. An early excision is recommended due to the possible evolution in a cystic or ameloblastic sense and due to the possibility of displacement and resorption of the adjacent teeth [5,6]. Removal of the lesion is usually simple due to the presence of an easily identifiable cleavage plane; the only difficulty can be represented by an unfavorable location that makes the lesion difficult to reach or proximity to anatomical structures at risk. Remember that a subperiosteal cleavage always reduces bleeding and the chances of accidental sections of nerve branches.
Conclusion
Compound odontomas must be surgically removed, in order to prevent their possible evolution into cysts or their possible transformation into odonto-ameloblastoma. Furthermore, since these, macroscopically and radiographically, are very similar to odonto-ameloblastoma and ameloblastic fibro-odontoma, histopathological examination is always necessary for definitive diagnostic confirmation. Surgical treatment of enucleation of compound odontomas is successful and reduces the risk of recurrence.
References
- Philipsen, Richart PA (2002) Revision of the 1992 edition of the WHO histological typing of odontogenic tumors A suggestion. J Oral Pathol Med 31: 253-258.
- Neville, Damm, Allen (2002) Bouquet Odontogenic cysts and tumors. (2nd ed), Oral and Maxillofacial Pathology, pp. 631-632.
- Owens BM, Sachuman NJ, Mineer H, Turner JE, Oliver FM (1997) Dental odontomas A retrospective study of 104 cases. Clin Pediat Dent 21: 261-264.
- Cuesta S Amado, Albiol J Gargallo, Aytés L Berini, Escoda C Gay (2003) Review of 61 cases of odontoma Presentation of an erupted complex odontoma. Med Oral 8(5): 366-373.
- Shafer, Hine, Levy (2006) Shafer's Textbook of Oral Pathology. In: Rajendran R, Sivapathasundharam B (editors.), Cysts and tumors of odontogenic origin. (6th ed), Elsevier, New Delh, pp. 404-407.
- Syed MR, Meghana SM, Ahmedmujib BR (2006) Bilateral complex odontomas in mandible. J Oral Maxillofac Pathol 10: 89-91.






























