Neurofibromatosis1 with Carcinoma Breast: A Surgical Conundrum
Era Yadav, Nilesh Taneja, Megha Tandon* and Ashwani Gupta
Department of Surgery, VMMC and Safdarjung Hospital, New Delhi
Submission:August 04, 2021; Published:August 12, 2021
*Corresponding author: Dr Megha Tandon, Associate Professor, Department of Surgery, VMMC and Safdarjung Hospital, New Delhi.
How to cite this article: Era Y, Nilesh T, Megha T, Ashwani G. Neurofibromatosis1 with Carcinoma Breast: A Surgical Conundrum. Open Access J Surg. 2021; 13(3): 555864 DOI: 10.19080/OAJS.2021.13.555864.
Introduction
Neurofibromatosis-I (NF-1) is an autosomal dominant multi system genetic disorder, due to mutation of NF-1 gene (Neurofibromin) that predisposes to myriad of neoplasms - both malignant and non-malignant, predominantly affecting skin and nervous system. However other organ systems can be involved as well [1]. The association of breast cancer with NF-1 is very rare and has recently been elucidated. There is a moderately elevated risk of early breast cancer in women with NF-1, under the age of 50 years [2]. The presence of neurofibromas may poses certain amount of diagnostic dilemma and sometimes, even therapeutic challenges in breast cancer patient especially during radiotherapy due to fear of increased risk of angio-sarcoma in such patients after radiotherapy. The aim to publish this case report is to increase awareness regarding this association and to highlight the difficulties that may be encountered during management of such patients.
Case Report
A 38-year-old premenopausal lady presented to our Outpatient Department with complains of lump in left breast for last 5 months. The lump in breast, was noticed by the lady as a new lump while bathing and was initially of size of around 2x2 cms. She did not pay much head to it. However, when the size increased gradually to around 4x5 cm, she became concerned and contacted her local practitioner from where she was referred to our OPD. There was no complain of pain, fever or nipple discharge. There was no history of trauma, radiation exposure or any hormonal treatments. She had multiple nodular skin lesions and coffee-colored spots over face, arms, trunk and back, both increasing in number and size since her childhood. Her mother had died of unknown cancer involving spine 20 years ago and father had similar skin lesions all over body and died of natural causes 25 years ago. On breast examination, a 4x6 cm well defined irregular lump with variegated consistency, nodular surface and restricted mobility was palpable from 10 o’clock to 2 o’clock position in the left breast. It was non tender, and no signs of local inflammation were present. There was a 3x2 cm matted lymph node mass in left axilla. C/L breast and axilla were normal and no supra/infra clavicular nodes were palpable.
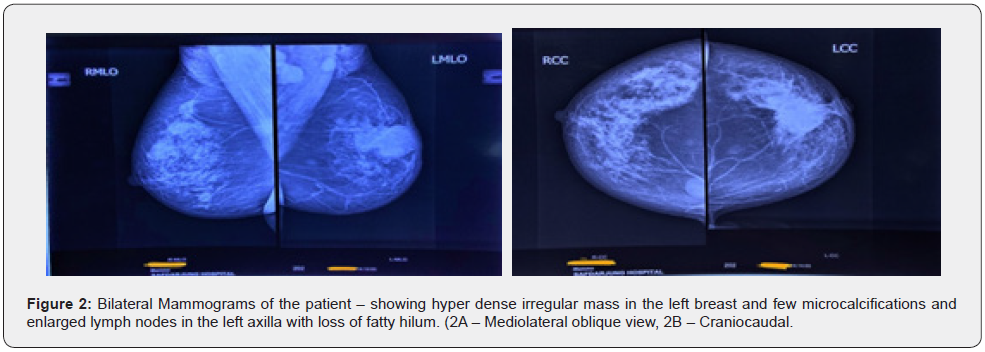
She underwent triple assessment. Bilateral mammogram revealed hyper dense irregular mass in the left breast with speculated margins and few microcalcifications in the left breast with multiple enlarged lymph nodes in the left axilla with loss of fatty hilum (BIRADS V). USG correlation confirmed the findings. Core needle biopsy confirmed Grade II Triple Negative Infiltrating Ductal Carcinoma left breast. Ophthalmological and CNS assessment were normal. CECT chest, abdomen and pelvis revealed no distant metastasis, or any abdominal tumors related to NF-1. The patient was discussed in MDT and was planned for neo-adjuvant chemotherapy with concurrent assessment of response followed by surgery (Modified Radical Mastectomy).
Discussion
Neurofibromatosis is a fairly common genetic disorder, with the birth incidence of 1 in 2500 and prevalence of 1 in 5000 [3-4]. It occurs due to mutation or deletion of the NF-1 gene (a tumor suppressor gene) which is located in the peri-centromeric region of the long arm of chromosome 17 (which also houses the BRCA1 gene) which has 100% penetrance but highly variable phenotypic presentation. Only 50% cases are familial, rest occur due to sporadic mutations in NF-1 gene [5].
NF1 is a clinical diagnosis based on the official diagnostic criteria that was developed at a National Institutes of Health Consensus Conference 1987, molecular genetic testing is seldom needed [1]. Based on these criteria, a person who has at least 2 of the following features is considered to have NF1:
1. 6 or more café-au-lait spots. These spots must be more than 5 millimeters (mm) in diameter in young children and more than 15 mm in diameter after puberty.
2. 2 or more neurofibromas or 1 plexiform neurofibroma
3. Freckling around the armpits or groin
4. Optic glioma, which is a tumor on the optic nerve in the brain that effects vision
5. 2 or more Lisch nodules, which are tumors on the iris of the eye
6. Specific bone changes, including sphenoid dysplasia, which is an abnormality of 1 of the bones forming the skull, or thinning of the long bones
7. A parent, sibling (brother or sister), or child with NF1 A person with family history of NF1, is suspected of having NF1 if any features present.
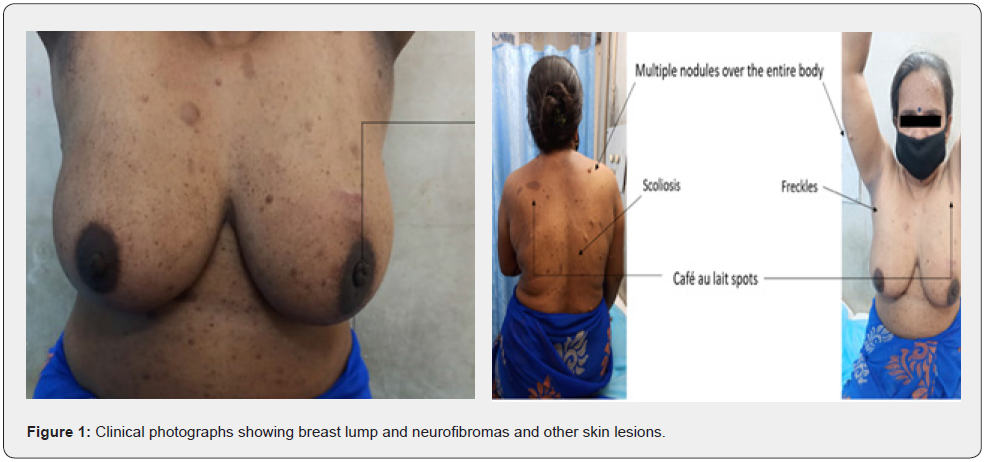
All affected individuals will have neurocutaneous featuresnone of which are life threatening (in form of neurofibromasbenign tumors of nerves) however it can also involve eye, brain, adrenal glands, spine and muscle [6-7] They are particularly at an increased risk of CNS Tumours (gliomas) and MPNST (malignant peripheral nerve sheath tumors) [8-9]. In addition to these they are also at an increased risk of GIST, Rhabdomyosarcomas and Phaeochromocytomas [10]. Their association with breast cancers has been debated over years and only recently been established [10]. Those with the mutation are at a fourfold increased risk of breast cancer compared to the general population [11]. The first case of a female patient with NF-1 and breast cancer was reported in 1933 by Arthur Jackson [12]. Since then, 286 reported cases have been analysed in a meta-analysis published by Lorena P. et al in 2019 and they noted that breast cancers in NF-1 were diagnosed at median age of 46 years [13]. Cases of male breast cancer with NF-1 have also been recently reported [14]. Furthermore, both the overall mortality and breast cancer-specific mortality appears to be higher among women with NF1 according to a Finnish population study [15]. These patients also appear to have a more aggressive presentation with 4 to 11-fold higher risk of contralateral breast cancer [16]. Murayama et al. reported most of the cases were diagnosed at an advanced stage owing to the presence of fibromatas on the trunk, the author also noted that most of these women had invasive ductal carcinoma [10]. The risk of a woman having breast cancer in her lifetime in NF-1 is 17.6% according to a survey conducted in neurofibromatosis clinics across USA. These tumours appear to result in worsened survival in comparison to the sporadic counterparts [17].
Conclusion
Although the number of reported cases of breast cancer in NF-1 are rare, rarer still in Indian scenario, the association between breast cancer and NF-1 is common but frequently overlooked. The presentation of these cancers is also delayed due to difficulty in identifying the sinister breast cancer lump amidst multiple cutaneous lesions. The radiological interpretation of mammograms can be challenging. Radiotherapy decision should be with caution. Awareness about the condition and this association of NF-1 with breast cancer is way forward in early diagnosis and management of such cases.
References
- (1987) Neurofibromatosis. NIH Consensus statement.
- Sharif S, Moran A, Huson S, Iddenden R, Shenton A, et al. (2007) Women with neurofibromatosis 1 are at a moderately increased risk of developing breast cancer and should be considered for early screening. Journal of Medical Genetics 44(8): 481-484.
- Kallionpää R, Uusitalo E, Leppävirta J, Pöyhönen M, Peltonen S, et al. (2017) Prevalence of neurofibromatosis type 1 in the Finnish population. Genetics in Medicine 20(9): 1082-1086.
- Evans D, Howard E, Giblin C, Clancy T, Spencer H, et al. (2010) Birth incidence and prevalence of tumor-prone syndromes: Estimates from a UK family genetic register service. American Journal of Medical Genetics Part A 152A(2): 327-332.
- Griffiths S, Thompson P, Frayling I, Upadhyaya M (2006) Molecular diagnosis of neurofibromatosis type 1: 2 years experience. Familial Cancer 6(1): 21-34.
- Friedman J (2021 ) Neurofibromatosis 1.
- (2021) Neurofibromatosis Type 1.
- Evans D (2016) What Is the Malignancy Risk in Neurofibromatosis Type 1?. Journal of Clinical Oncology 34(17): 1967-1969.
- Uusitalo E, Rantanen M, Kallionpää R, Pöyhönen M, Leppävirta J, et al. (2016) Distinctive Cancer Associations in Patients With Neurofibromatosis Type 1. Journal of Clinical Oncology 34(17): 1978-1986.
- Murayama Y, Yamamoto Y, Shimojima N, Takahara T, Kikuchi K, et al. (1999) Ti Breast cancer associated with Von Recklinghausen's Neurofibromatosis. Breast Cancer 6(3): 227-230.
- Airewele GE, Sigurdson AJ, Wiley KJ, Frieden BE, Caldarera LW, et al. (2001) Neoplasms in neurofibromatosis 1 are related to gender but not to family history of cancer. Genet Epidemiol 20: 75.
- JACKSON A (1933) THREE CASES OF MULTIPLE NEUROFIBROMATOSIS WITH MALIGNANT DEGENERATION. The Journal of Nervous and Mental Disease 78(6): 581-596.
- Suarez Kelly L, Yu L, Kline D, Schneider E, Agnese D, et al. (2019) Increased breast cancer risk in women with neurofibromatosis type 1: a meta-analysis and systematic review of the literature. Hereditary Cancer in Clinical Practice 17(1).
- Tandon M, Panwar P, Garg P, Chintamani, Siraj F (2015) Neurofibromatosis with male breast cancer-risk factor or co-incidence? Report of two rare cases. Breast Disease 35(1): 29-32.
- Uusitalo E, Kallionpää R, Kurki S, Rantanen M, Pitkäniemi J, et al. (2016) Breast cancer in neurofibromatosis type 1: overrepresentation of unfavourable prognostic factors. British Journal of Cancer 116(2): 211-217.
- Evans D, Kallionpää R, Clementi M, Trevisson E, Mautner V, et al. (2019) Correction: Breast cancer in neurofibromatosis 1: survival and risk of contralateral breast cancer in a five country cohort study. Genetics in Medicine 22(1): 242-242.
- Wang X, Teer J, Tousignant R, Levin A, Boulware D, et al. (2017) Breast cancer risk and germline genomic profiling of women with neurofibromatosis type 1 who developed breast cancer. Genes Chromosomes and Cancer 57(1): 19-27.






























