Airway Obstruction Following External Jugular Vein Cannulation in A Bilateral Cleft Lip and Palate Patient-Case Report
shaza BM Mahjoub, Sulafa M Elhassan, Talal Murtada and Amel Eltayeb*
Assistant Professor of Oral and Maxillofacial Surgery-Nile university-Sudan
Submission:April 30, 2021; Published:June 09, 2021
*Corresponding author: Amel eltayeb, Assistant Professor of Oral and Maxillofacial Surgery-Nile university-Sudan
How to cite this article: Shaza Majoub B, sulafa Elhassan M, Talal M, Amel E. Airway Obstruction Following External Jugular Vein Cannulation in A Bilateral Cleft Lip and Palate Patient-Case Report. Open Access J Surg. 2021; 13(2): 555857 DOI: 10.19080/OAJS.2021.13.555857.
Abstract
Introduction: Airway obstruction is a rare fatal complication that may occur following external jugular vein cannulation.
Case presentation: A patients with cleft lip and palate was intubated orotracheally and external jugular vein cannulated after multiple failure of finding a peripheral intravenous line. Rupture of external jugular vein after extubation happened and airway was obstructed, immediate neck incisions were done to decompress the swollen neck. Patient recovered completely after 48 hours and discharged in good condition
Conclusion: Good care and adequate precautions in patients with external jugular venous cannulation in the Operation rooms, intensive care unit or wards to prevent such serious iatrogenic complications and early diagnosis and intervention if complications occurred.
Keywords: Airway obstruction; External jugular vein EJV; Cleft lip and palate; Cannulation
Abbreviations: (EJV) External Jugular Vein; (CLP) Cleft Lip and Palate; (ICU) Intensive Care Unit
Introduction
Cleft lip and/or palate (CLP) is the most common congenital malformation with an incidence of approximately 1 in 700 live births worldwide. This rate varies significantly across geographical regions [1]. Airway obstruction secondary to cervical haematoma commonly occurs after anterior neck surgery, especially carotid endarterectomy [2]. and thyroidectomy. It has also been described following internal jugular vein cannulation [3].
A number of well recognized complications are associated with internal jugular vein catheterization including bleeding, pneumo and hemothorax, chylothorax, air embolism, pericardial tamponade, infections, hematoma, nerve injuries and Horner’s syndrome [4,5]. However significant complications related to external jugular vein catheterization are uncommon. Yadav et.al reported a case of massive infusion hydrothorax following insertion of an external jugular vein catheter necessitating immediate drainage via a pigtail catheter insertion and mechanical ventilation [6].
Case presentation
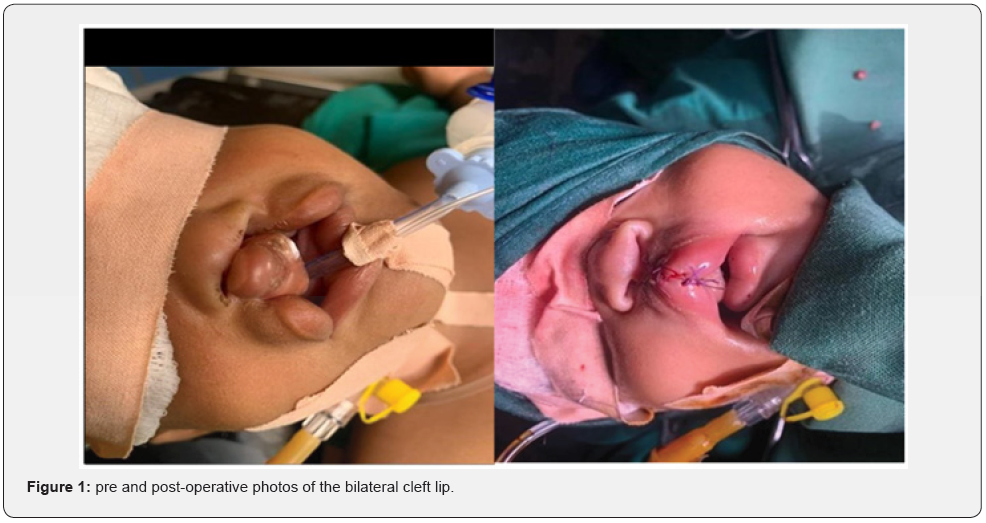
An 18-months-old male with bilateral cleft lip and palate was presented to the cleft clinic at Haj al-safi teaching hospital for cleft lip repair under general anaesthesia. His past medical history revealed an ICU admission after birth for three days and nasogastric tube insertion for feeding for up to 5 months. Also, multiple admissions due to recurrent chest infection which affected his general condition. On physical examination, he was underweight (7 kg) with noticeable developmental delay. He had frontal bossing, hypertelorism, medial squint in both eyes, saddle nose and low positioned ears. Pre-operative assessment was done, patient was examined by paediatric cardiologist and paediatrician and clearance was given for the operation under general anaesthesia. In the operation room the aesthesia team couldn’t find a proper peripheral I.V line, a line in the right external jugular vein was then inserted (size 18). Oro-tracheal intubation followed and general anaesthesia was obtained. Cheiloplasty for the bilateral cleft lip was done and the patient was extubated uneventfully and transferred to the ward in a stable condition (Figure 1).
At the ward, after a failed trial of inserting IV fluids the nurse noticed the ruptured canula and escaping of fluids into the neck spaces compressing on the trachea and compromising the airway. Immediate decompression started by placing two neck incisions (Figure 2) and placing a nasopharyngeal tube at same time, slowly the fluids started to drain from neck spaces, the swelling started to reduce, and his oxygen saturation was raised back to 100%, two drains were inserted in the incisions and patient was kept on close monitoring for the following 24 hours. The next day the patient was extubated, and the drains were removed, 48 hours later he was discharged in a good condition.

Discussion
External jugular vein has an impressive safety profile due to its superficial position and distance from vital structures, thus decreasing the risk of major complications which are commonly associated with central venous lines. External jugular venous (EJV) cannulation is being increasingly used in emergencies patients for fluid and inotrope administration. As central venous access is potentially lifesaving, there are no absolute contraindications to performing the procedure [7], however, knowing which device is most appropriate for each situation might improve patient outcomes. Aside from emergent placement of central lines, the indications for central catheters include the following; administration of IV fluids, medications, or blood products, either in large quantities or over a prolonged period of time, administration of medications that are harmful to peripheral veins (eg, chemotherapy), and poor or inaccessible peripheral venous access [8,9].
There are several complications associated with central line use, regardless of the site of insertion. Past research has demonstrated that ultrasound guidance has been shown to decrease the risk of complications at all central line access sites [10,11]. Complications that occur during or closely following a central line insertion are called immediate complications which can be categorized into the following; cardiac, vascular, pulmonary, and catheter placement complications [12]. The delayed complications of a central line insertion include infection and device dysfunction. These complications are much more gradual in onset and can occur in the weeks to months after a central line insertion [12]. In this case, an early complication occurred due to ruptured of the external jugular vein with blockage and escaping of fluids into the neck spaces. Manipulation of the operative site may have caused the disconnection, careful per procedural care and monitoring should always be conducted.
Conclusion
Good care and adequate precautions in patients with external jugular venous cannulation in the operation rooms, intensive care unit or wards is mandatory to prevent such serious iatrogenic complications. Early diagnosis and intervention if complications occurred is also of such importance.
Conflict of interest
The authors declare no conflict of interest.
References
- Bender PL (2000) Genetics of cleft lip and palate. J Pediat Nurs 15(4): 242-249.
- O’Sullivan JC, Wells DG, Wells GR (1986) Difficult airway management with neck swelling after carotid endarterectomy. Anaesthesia and Intensive Care 14(4): 460-464.
- Kua JSW, Tan IKS (1997) Airway obstruction following internal jugular vein cannulation. Anaesthesia 52(8): 776-785.
- Hoffmann W, Weidmann B, Jansen W, Tauchert M (1988) Infusion hydrothorax as a sequel of malposition of an internal jugular vein catheter. Med Klin 83(15): 496-498.
- Van Haeften TW, Van Pampus EC, Boot H, Strack van Schijndel RJ, Thijs LG (1988) Cardiac tamponade from misplaced central venous line in pericardiophrenic vein. Arch Intern Med 148(7): 1649-1650.
- Manoj Kumar Jangid, Yadav SK (2014) Rare Case of Massive Hydrothorax following external Jugular vein Cannulation. Pediatric Oncall Journal 11(2): 46-47.
- Taylor RW, Palagiri AV (2007) Central venous catheterization Crit Care Med 35(5): 1390-1396.
- Moureau N, Poole S, Murdock MA, Gray SM, Semba CP (2002) Central venous catheters in home infusion care: outcomes analysis in 50,470 patients. J Vasc Interv Radiol 13(10): 1009-1016.
- Ng PK, Ault MJ, Ellrodt AG, Maldonado L (1997) Peripherally inserted central catheters in general medicine. Mayo Clin Proc 72(3): 225-233.
- Bannon MP, Heller SF, Rivera M (2011) Anatomic considerations for central venous cannulation. Risk Manag Healthc Policy 4: 27-39.
- Vascular Access 2006 Work Group (2006) Clinical practice guidelines for vascular access. Am J Kidney Dis Supl(1): S176-S247.
- Kornbau C, Lee KC, Hughes GD, Firstenberg MS (2015) Central line complications. Int J Crit Illn Inj Sci 5(3):170-178.






























