Tachyarrhythmia, Sharp Hemodynamic Instability During Surgery of Pheochromocytoma in a Child with Important of Preoperative Preparation : A Systemic Review and Case Report
Elamin YE Alamelhuda1*, Alsadig AA Corina1, Awatif O Mohamed1, Maram OE Mabyoue2, Kamal E Elsiddig2
1Sudan Medical Specialization Board, Sudan
2Faculty of Medicine, University of Khartoum, Sudan
Submission:May 31, 2021; Published:June 04, 2021
*Corresponding author: Elamin YE Alamelhuda, MBBS, MRCSED, MD SMSB. General Surgery department at Letterkenny University Hospital co. Donegal, Ireland.
How to cite this article: Elamin YE A, Alsadig AA C, Awatif O M, Maram OE M, Kamal E E. Tachyarrhythmia and Sharp Hemodynamic Instability During Surgery and Important of Preoperative Preparation of Pheochromocytoma in a Child: A Systemic Review and Case Report. Open Access J Surg. 2021; 13(1): 555855.. DOI: 10.19080/OAJS.2021.13.555855.
Abstract
Introduction: Pheochromocytomas are the most common tumors originating from the adrenal medulla, they secret catecholamine in their active form. The hallmark is hypertension with sympathetic hyperactivity that occur in a very small percentage of the pediatric population. Tachyarrhythmia and severe hemodynamic instability can complicate their surgery.
Case report: A 14-year-old boy presented to Khartoum Teaching Hospital complaining of symptoms and signs of sympathetic hyperactivity. He was investigated for pheochromocytoma which came positive, specially metanephrine and VMA in 24hours urine collections; moreover, ultrasound and CT scan confirmed right suprarenal swelling. He was planned for surgery, during induction of anesthesia he developed tachyarrhythmia and shooting blood pressure, therefore, the operation was postponed. Alpha blocker (Doxazocin) was prescribed for one month then his general condition improved, and he gained weight. Adrenalectomy was performed without intraoperative or postoperative complications. Follow up for 6 months passed uneventfully.
Discussion: Pheochromocytoma is a serious disease with a high mortality rate, intraoperative hemodynamic instability and arrhythmias. Additionally, cardiac complications were also reported. The occurrence of hypertensive crises, arrhythmias and hypotensive crises during surgery in pheochromocytoma can be prevented both preoperatively and intraoperatively by adequate alpha-adrenergic blockade and volume replacement.
Conclusion: Pheochromocytoma is one of the few causes of hypertension that can be treated surgically. Intraoperative complications are common with symptomatic variant of the disease which mandate preoperative use of alpha blocker. There is no significant difference in outcome between using selective or nonselective alpha blocker.
Keywords: Pheochromocytoma, Child, Hemodynamic instability, Systemic review, Case report
Abbreviations: VMA= Vanilmandelic acid, CT scan= Computed tomograph
Introduction
Pheochromocytomas are the most common tumors originating from the adrenal medulla (80 – 90%), secreting catecholamine in their active type, there is also a nonsecreting type [1]. The hallmark is hypertension with sympathetic hyperactivity that occur in only 0.1% of the pediatric population [2]. Moreover, tachyarrhythmia and sharp hemodynamic instability can occur during surgery [1,2]. This kind of hypertension can be treated surgically by removing the adrenal tumor [3]. Blockage of the alpha-adrenergic receptors during the preoperative phase is necessary to improve the general fitness of the patient and prevent intraoperative cardiac and hemodynamic instability [4]. Beta blockers are also required if tachyarrhythmia developed, this should not be introduced until the patient is on alpha blocker for a long time, because unopposed alpha-adrenergic receptor stimulation can precipitate hypertensive crisis. Either cardio-selective or non-selective beta-blockers can be used [5]. Pheochromocytoma has been classified as a "10% tumor" because various studies have shown that each of the characteristics mentioned below occur with a frequency of approximately 10%: bilateral, extra-adrenal, multiple, malignant, familial, recurrent, discovered incidentally and occurring in children [1].
Pheochromocytoma can occur sporadically or familial, such as in syndrome of multiple endocrine neoplasia MEN IIA and IIB, neurofibromatosis (von Recklinghausen's disease), von Hippel-Lindau's disease, Sturge-Weber's syndrome and tuberous sclerosis. Cases in familial usually occur at a younger age and are mostly bilateral and carry an aggressive biological behavior [6]. Diagnosis is established by vanilmandelic acid (VMA) detection in 24-hour urine collection, it confirms the diagnosis in 95% of cases [1]. Fractionated catecholamines and metanephrines are also helpful in the diagnosis. CT abdomen (with contrast) is 95% accurate in localizing the tumor, but prior alpha-blockers should be given to prevent the sudden rise in blood pressure [1]. Surgical excision of the tumor is the only way for a successful treatment [3].
Case report
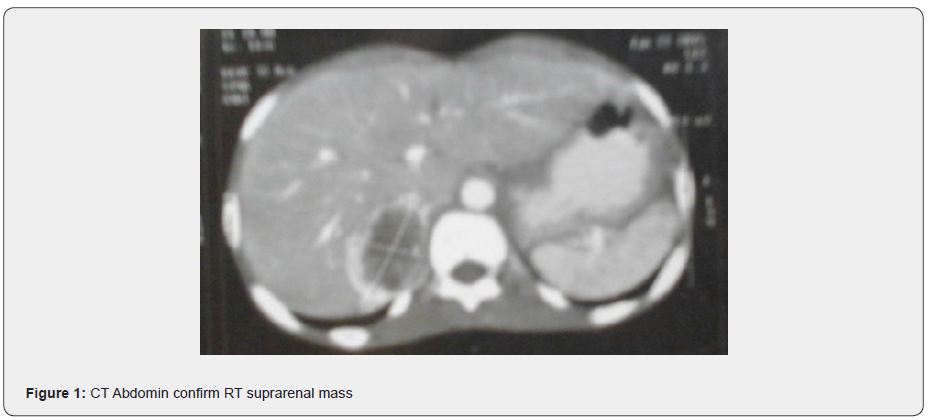
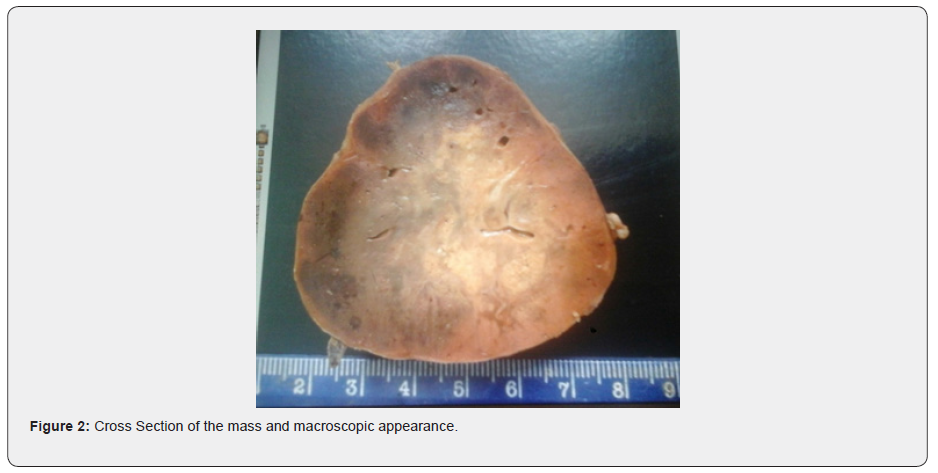
A 14-year-old boy presented to Khartoum Teaching Hospital complaining of progressive loss of weight despite normal appetite, fatigability, heat intolerance, profuse sweating, generalized joint pain, high-grade intermittent fever with a change in urine color to red, and polyuria for 9 months. Moreover, he complained of chest pain, palpitation, shortness of breath, paroxysmal nocturnal dyspnea, orthopnea with neurological symptoms such as irritability, headache, tremor, nervousness and blurring of vision. On physical examination, the patient looked ill, emaciated, pale, his respiratory rate was 24b/m, blood pressure 135/110, pulse rate 120 b/m and temperature 37° C. Nevertheless, he had active pericardium and a soft diastolic murmur in mitral area. Funduscopic Examination revealed bilateral hypertensive maculopathy and retinopathy. General laboratory tests were in the normal range. VMA per 24 hrs urine collection was 13mg/day (normal up to 13.6mg/day), metanephrines per 24hrs urine collection was 8785 mg/24hrs (normal range up to 100mg/24hrs).
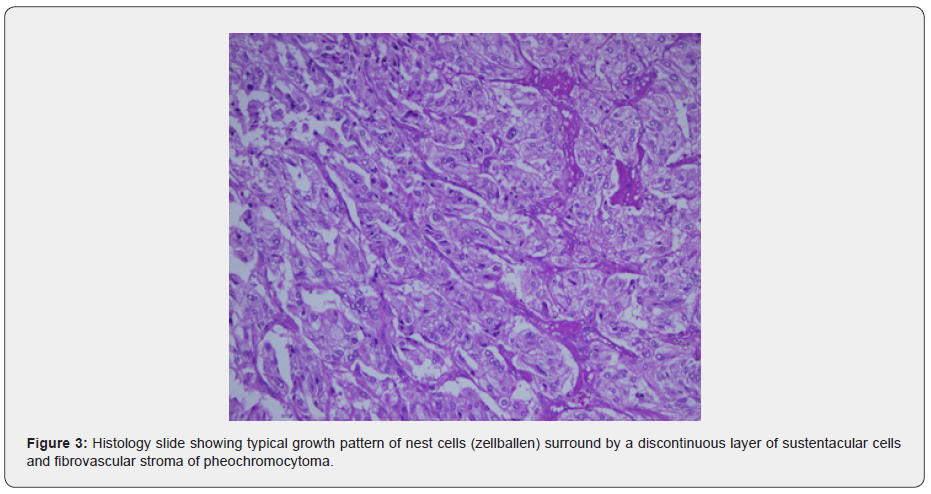
Echocardiography showed ejection fracture 60%, small membranous ventricular septal defect with left to right shunt and hypertrophic non-obstructive cardiomyopathy. An abdominal ultrasound scan showed evidence of isoechoic mass seen in the right retroperitoneal region adjacent to the upper pole of the right kidney measured about 4.5*4.4 cm diameter with normal right kidney. Doppler examination showed normal flow signal and normal peak systolic velocity of the main renal artery. Computed tomography scan of the abdomen showed a hypodense mass seen in the right suprarenal region. The mass exhibit heterogeneous enhancement after contrast and cannot be separated from the upper pole of the right kidney.
Treatment was started with nifedipine 100mg per day divided dose in the acute stage, which controlled the blood pressure, then, the patient was sent to surgery after one week of the anti-hypertensive treatment. During induction of anesthesia, the patient blood pressure readings increased up to 240/125 with tachyarrhythmia and sharp hemodynamic instability, so the operation was post-ponded to control his blood pressure and improve anesthetic fitness. Patient received medications as follows; Amlodipine 10mg, Atenolol 100mg, Doxazocin 4mg and Hydrochlorothiazide 25mg, along with nutritional support for one month. The features of sympathetic over activity disappeared and his weight improved. He was planned for right adrenalectomy, which run uneventfully with use of trinitrate infusion to control the blood pressure and volume expansion to avoid postoperative hypotension. Postoperative period passed without hypotension or persistent hypertension. Histopathology report confirmed the diagnosis of pheochromocytoma. Postoperative follow up for 6 months passed safely.
Discussion
Pheochromocytoma is a disease with a high mortality rate and intraoperative hemodynamic instability and arrhythmias which can be reduce by adequate perioperative treatment [3,5]. Additionally, cardiac complications also reported by many authors which mandate the use of Beta blocker after long use of alpha blocker for 14 days [5]. The occurrence of hypertensive crises, arrhythmias and hypotensive crises during surgery in pheochromocytoma can be prevented both preoperatively and intraoperatively by adequate alpha-adrenergic blockade and volume replacement. Only in few cases addition of beta-adrenergic blockade is necessary [7]. Multiple studies are compliant with our case findings during surgery, like shooting blood pressure and cardiac complications. Identification of preoperative risk factors for intraoperative hemodynamic instability discussed by this study, predicts that a high plasma noradrenaline concentration, larger tumor size, more profound postural blood pressure falls after alpha-blockade and mean arterial pressure levels above 100 mmHg (130/85 mmHg) collectively increase the risk of intraoperative complications [8]. Comparably, other studies predicted that open adernalectomy and the type of alpha blockade are considered as risk factors for intraoperative hemodynamic instability [9].
According to the function of pheochromocytoma, it is safe and efficient to use different preoperative preparations. Grading the patients according to the perioperative blood pressure and severity of hypertension can predict the severity of intraoperative complications. As the perioperative blood pressure of Functionary Grade 0 had no fluctuation intraoperatively, the blood pressure of therapeutic group of Functionary Grade 1 had small range fluctuation (< 20 mm Hg), the hemodynamics of Functionary Grade 2 and Grade 3 recovered within 24 hours postoperatively and no complications occurred [10].
On the other hand, one large cohort study argued the importance of perioperative treatment to avoid hemodynamic instability during surgery, it revealed no mortality and low global and cardiovascular morbidity rates. Showing that pheochromocytoma surgery without systematic perioperative preparation and even without preoperative antihypertensive is feasible and safe for selected patients [11]. Moreover, postoperative complications are encountered such as hypotension, due to the use of phenoxybenzamine or loss of effect of catecholamine hormone (noradrenaline and dopamine secreting tumor), when the tumor was removed, which were treated by fluid expanders. In addition, the persistent hypertension usually occurs in noradrenergic tumors type. Also, recurrence of the malignance is anticipated [4,12]. Blockage of the alpha-adrenergic receptors during the preoperative phase is necessary to prevent cardiovascular complications and perioperative mortality after resection of catecholamine-producing tumors. Phenoxybenzamine is the commonly used alpha-adrenergic blocking agent. Therapy begins with low doses and is increased stepwise up to 250 mg daily [5].
Despite the adverse side effects of phenoxybenzamine, it has been widely used for the preoperative management of patients with pheochromocytoma. Doxazocin, a selective alpha 1-adrenoceptor antagonist, has a pharmacologic profile more suited to controlling blood pressure in such patients. Doxazocin provides safe, efficacious pre- and perioperative control of arterial pressure. In patients with predominantly norepinephrine-secreting tumors (in line with our case management) [14]. Nevertheless, one study concluded that there was no significant difference in the operative and postoperative blood pressure and plasma volume control among the nonselective (phenoxybenzamine) and selective (doxazocin, prazocin) [14,15]. Perioperative haemodynamics seem to be slightly better controlled with phenoxybenzamine, at the cost of more pronounced postoperative hypotension. Side effects occurred less often in the doxazocin use [15]. The use of alpha blocker has no benefit in maintaining intraoperative hemodynamic stability in patients with normotensive pheochromocytoma (nonsecretory tumors). It may increase the use of vasoactive drugs and colloid infusion [10,13].
Conclusion
Pheochromocytoma is one of the few causes of hypertension that can be treated surgically. Although it is the causative factor of hypertension in about 0.1% to 0.6% of the hypertensive population, its detection is mandatory, not only for the potential cure of hypertension but also to avoid the lethal effect of the unrecognized tumor. Intraoperative complications are common with symptomatic variant of pheochromocytoma which mandate preoperative use of alpha blocker. There is no significant difference in outcome between using selective or nonselective alpha blocker.
Ethical Approval
Ethical clearance was obtained from the Department of Pediatric Surgery, Khartoum teaching Hospital, Khartoum state, Sudan.
Informed Consent
Written consent was obtained from the patient and his parents to write and publish his case as a report with accompanying radiological images.
Conflicts of Interest
Authors declare that there are no conflicts of interest regarding the publication of this paper.
Authors’ Contributions
Authors contributed equally and significantly to the concept and design, drafting, critical revision and final approval of the report.
References
- Prys Roberts C, Farndon JR (2002) Efficacy and safety of doxazosin for perioperative management of patients with pheochromocytoma. World J Surg 26(8): 1037-1042.
- Bissada NK, Safwat AS, Seyam RM, Al Sobhi S, Hanash KA, et al., (2008) Pheochromocytoma in children and adolescents: a clinical spectrum. J Pediatr Surg 43(3): 540-543.
- Jovanović K, Romić P, Kovacević S, Popadić A (2002) Pheochromocytoma as a challenge for the anesthesiologist. Srp Arh Celok Lek 130: 25-30.
- Conzo G, Musella M, Corcione F, Depalma M, Stanzione F, et al., (2013) Role of preoperative adrenergic blockade with doxazosin on hemodynamic control during the surgical treatment of pheochromocytoma: a retrospective study of 48 cases. Am Surg 79(11): 1196-1202.
- Lam KY, Chan AC, Wong WM, Lam KS (1993) A review of clinicopathologic features of pheochromocytomas in Hong Kong Chinese. Eur J Surg Oncol 19(5): 421-427.
- Tatić S, Havelka M, Paunović I, Bozić V, Diklic A, et al., (2002) Pheochromocytoma--pathohistologic and immunohistochemical aspects. Srp Arh Celok Lek 130: 7-13.
- Schmucki O (1979) Medical support in surgery for pheochromocytoma. Helv Chir Acta 46(3): 287-290.
- Bruynzeel H, Feelders RA, Groenland TH, Van Den Meiracker AH, Van Eijck CH, et al., (2010). Risk factors for hemodynamic instability during surgery for pheochromocytoma. J Clin Endocrinol Metab 95(2): 678-685.
- Kiernan CM, Du L, Chen X, Broome JT, Shi C, et al., (2014) Predictors of hemodynamic instability during surgery for pheochromocytoma. Ann Surg Oncol 21(12): 3865-3871.
- Pan DL, Li HZ, Zeng ZP (2004) The discussion of standards for clinical functional gradation and preoperative preparation of pheochromocytoma. Zhonghua Wai Ke Za Zhi 42(18): 1089-1092.
- Buisset C, Guerin C, Cungi PJ, Gardette M, Paladino NC, Taïeb D, et al., (2020) Pheochromocytoma surgery without systematic preoperative pharmacological preparation: insights from a referral tertiary center experience. Surg Endosc 18: 1-8.
- Furnica RM, Dusoruth MM, Persu A, Gruson D, Mourad M, et al., (2020) Influence of secretory phenotype and preoperative preparation on surgical outcome in pheochromocytoma. Endocr Connect 10(1): 92-101.
- Shao Y, Chen R, Shen ZJ, Teng Y, Huang P, et al., (2011) Preoperative alpha blockade for normotensive pheochromocytoma: is it necessary? J Hypertens 29(12): 2429-2432.
- Prys Roberts C, Farndon JR (2002) Efficacy and safety of doxazosin for perioperative management of patients with pheochromocytoma. World J Surg 26(8): 1037-1042.
- Kocak S, Aydintug S, Canakci N (2002) Alpha blockade in preoperative preparation of patients with pheochromocytomas. Int Surg 87(3): 191-194.






























