Acute Mesenteric Ischemia Due to COVID-19: A Case Report
Fakhar Shahid1, Syed Muhammad Ali1,2*, Sana Saleem3, Umair Shahid3, Nadia Karim4, Ejaz Latif1, Ahmed Zarour1
1Department of Acute Care Surgery, Hamad Medical Corporation, Qatar
2Weill-Cornell Medicine, Qatar
3Anesthesia and SICU, Hamad Medical Corporation, Qatar
4Internal Medicine, Hamad Medical Corporation, Qatar
Submission:September 24, 2020; Published:October 12, 2020
*Corresponding author:Syed Muhammad Ali, Department of Acute Care Surgery, Hamad Medical Corporation, Doha 3050, Qatar
How to cite this article:Fakhar S, Syed Muhammad A, Sana S, Umair S, Nadia K. Acute Mesenteric Ischemia Due to COVID-19: A Case Report. 002 Open Access J Surg. 2020; 12(2): 555831. DOI: 10.19080/OAJS.2020.12.555832.
Abstract
Introduction: Recent evidence has shown that a key feature of severe COVID –19 is that it may predispose to both venous and arterial thromboembolic diseases leading to adverse outcomes. Case Presentation: We report a case of an elderly lady who presented with acute abdomen and diagnosed to have acute mesenteric ischemia (AMI). She was tested positive for COVID – 19 and underwent surgical intervention but could not survive her post-operative course. Conclusion: There remains much interest, and an urgent clinical need, to precisely delineate the mechanisms by which SARS CoV-2 infection causes thrombotic complications in the hope that new insights into this process will yield novel therapeutic approaches where early diagnosis and prompt effective treatment could have improved the clinical outcome.
Keywords:Acute Abdomen; Covid-19; Mesenteric ischemia; Mortality.
Abbreviations: XR: X-ray; AMI: Acute mesenteric ischemia
Introduction
Since the disclosure of the SARS-CoV-2, emerging in Wuhan China, which causes COVID-19, a huge number of cases have been analyzed overall bringing about countless deaths. In the United States, there are approximately 2.9 million reported cases with over 100,000 deaths as of 1st week of July 2020 [1]. Although the unfavorable impacts of COVID-19 were at first considered to influence the respiratory tract by causing pneumonia and respiratory distress syndrome (ARDS), it has now become clear that COVID-19 may be related to thromboembolic complications [2]. Apart from deep venous thrombosis and pulmonary embolism (PE), acute mesenteric ischemia (AMI) has also been reported in severe COVID-19 patients [3]. Acute mesenteric ischemia is a potentially fatal vascular emergency, with an overall mortality of 60-80% [4] requiring prompt diagnosis and treatment. This report will detail the clinical findings of the prothrombotic status of a patient experiencing AMI while testing positive for COVID-19.
Case Presentation
71-year-old female known to have diabetes mellitus type 2, hypertension, atrial fibrillation on warfarin, presented to the emergency department with epigastric pain of one-day duration, sudden onset, severe in nature, postprandial, non- radiating associated with vomiting containing food particles and with a sense of impending doom. She was uncomfortable, afebrile with tachycardia (136) and blood pressure of 169/82 and maintaining 95% O2 saturation on room air. Her abdominal examination showed out of proportion tenderness in the periumbilical region without rigidity but guarding. Her WBC count was high (23.7 x 103/ ul) with an increased neutrophil count and increased inflammatory markers, CRP was 5.2mg/dl and lactic acid = 6.9 mmol/L and also had high Troponin T levels (23-24 ng/L) (Table 1).
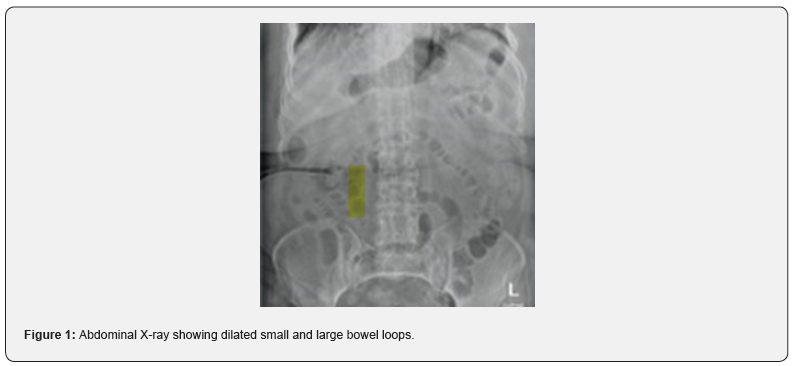
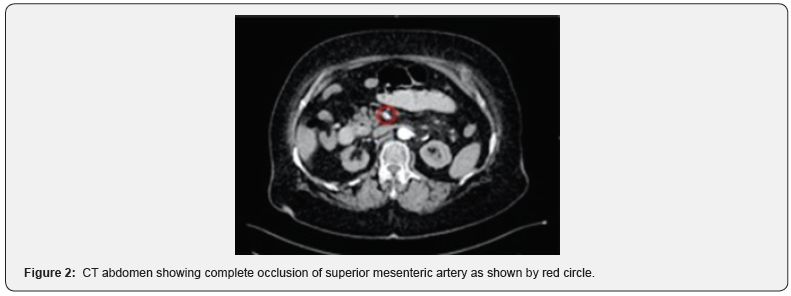
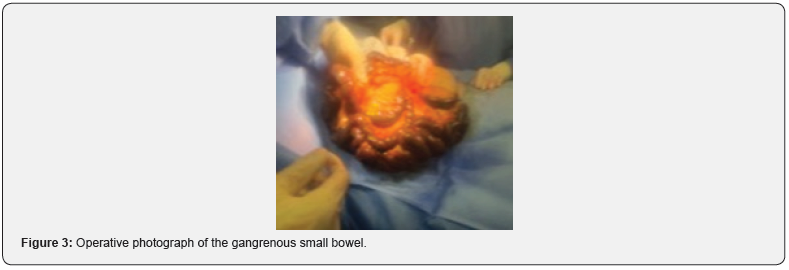
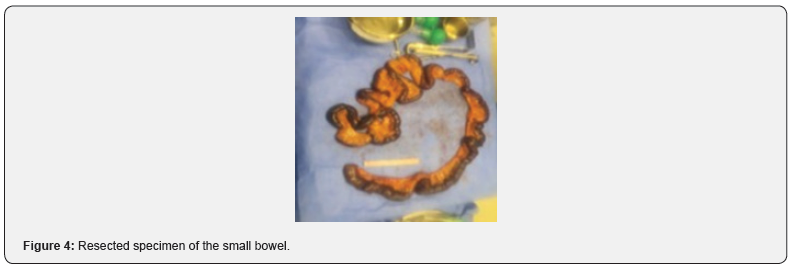
The patient initially underwent an abdominal XR (Figure 1) which displayed non-specific bowel pattern, and no abnormal air-fluid levels. Her CT Abdomen (Figure 2) revealed complete occlusion of the superior mesenteric artery, with mild dilatation of the proximal small intestinal loops showing suspicious pneumatosis intestinalis and poor post-contrast enhancement of the distal ileal loops features concerning for bowel ischemia. The patient was immediately shifted to operating theatre for midline laparotomy. There was foul-smelling serosanguinous peritoneal fluid along with complete gangrene of the small bowel, colon was healthy and other organs were unremarkable. Damage control surgery with resection of the gangrenous bowel was carried out except 30 cm distal to the duodeno-jejunal junction and 15 cm proximal to the ileocaecal valve (Figures 3 and 4).

The patient was transferred to surgical ICU post-operatively for ventilator and hemodynamic support. She was confirmed to be infected with COVID-19 by PCR nasal swab. She was unstable during her recovery and developed metabolic acidosis with respiratory acidosis resulting in increasing difficulty to maintain her oxygenation despite full mechanical ventilator support and 100% Fio2. On second day hemodialysis was started despite which patient continued to deteriorate and developed mixed acidosis, multiple organ failure, and refractory septic shock secondary to abdominal sepsis and viral infection (COVID19) all that led to increasing lactic acid level and liver failure. On 3rd post-operative day, the patient developed cardiac arrest with asystole and expired.
Discussion
The novel coronavirus belongs to a group of severe acute respiratory syndrome-related corona viruses [5]. It originated in Wuhan, Hubei Province, China, in December 2019 and was declared a pandemic by WHO on 11 March 2020 [6]. Severe SARS-CoV-2 infection is more commonly observed in patients with specific comorbidities, yet the mechanism of this relationship is unclear. Advanced age, hypertension, diabetes, smoking, and coronary artery disease are risk factors for severe COVID-19, conditions which are all associated with vascular endothelial dysfunction. Vascular complications are increasingly being reported [7] in COVID patients. Apart from venous thromboembolism, acute mesenteric ischemia (AMI) has been reported in severe COVID-19 patients. Acute mesenteric ischemia is a life-threatening emergency; the delay in diagnosis of which contributes to the continued high mortality rate.
The exact mechanism underlying the complication of AMI in COVID-19 patients is still unknown at present. However, a few mechanisms, independently or in combination could be responsible for this complication. Firstly, the SARS-CoV-2 enters the cell via the angiotensin-converting enzyme 2 (ACE2) receptor present in the alveoli. The severe form of the infection is characterized by an intense immune-inflammatory response, evidenced by the presence of neutrophils, lymphocytes, monocytes, and macrophage [8]. High serum levels of proinflammatory cytokines (interleukins 1 and 6, tumor necrosis factor and interferon-g), known as “cytokine storm”, have been reported in those patients [9]. Evidence has shown a bidirectional relationship between inflammation and coagulation, in which inflammation activates coagulation, and coagulation heightens inflammatory activity [10]. However, the evidence available at present has not conclusively demonstrated large mesenteric vessel (arterial or venous) thrombosis. Preliminary pathological evidence has shown bowel necrosis with small vessel thrombosis involving the submucosal arterioles, thereby pointing to an in-situ thrombosis of small mesenteric vessels rather than an embolic event [3].
The expression of angiotensin-converting enzyme (ACE 2) on enterocytes of the small bowel, the target site for SARS-COV 2 also may point to damage leading to cause mesenteric ischemia which seems more plausible cause in our patient as her atrial fibrillation was well controlled. However, there may be a possibility that thrombus originated from heart and aggravated by the concurrent COVID-19 infection. Lastly, the hemodynamic instability in the form of hypotension, associated with COVID-19 pneumonia might also play a role in causing nonocclusive mesenteric ischemia [11].
Conclusion
Understanding the relationship between COVID-19 and the occurrence of AMI needs to be further studied as it will be imperative in setting appropriate diagnostic testing as well as developing new therapeutic targets. The growing awareness and understanding of thrombotic complications in patients with SARS-CoV-2 infection will contribute to a more rigorous approach resulting in the earlier detection of such events and reducing the mortality rate associated with the disorder.
Ethical Approval
Waiver of Consent was received as the Patient expired and no Relatives or Next of Kin were found for Consent. Approval received by Medical Research committee of Hamad Medical Corporation reference number (MRC-04-20-664).
Informed consent
We have a waiver of consent as the patient expired in the hospital. The relatives or next of Kin could not be traced. Patient identity information is not shared in this article.
Funding:
No funding applied.
Conflict of Interest:
All authors have declared no conflict of interest.
References
- Centers for Disease Control and Prevention (CDC): Cases in the USA. 2020.
- Lodigiani C, Iapichino G, Carenzo L,Maurizio C, Paola F, et al. (2020) Venous and arterial thromboembolic complications in COVID-19 patients admitted to an academic hospital in Milan, Italy. Thromb Res191:9-14.
- Bhayana R, Som A, Li MD, Denston E C, Mark A A, et al. (2020) Abdominal Imaging Findings in COVID-19: Preliminary Observations.Radiology. 297(1):E207-E215.
- Florian A, Jurcut R, Lupescu I, Grasu M, Croitoru M, et al. (2010) Mesenteric ischemia--a complex disease requiring an interdisciplinary approach. A review of the current literature. Rom J Intern Med48(3):207-222.
- Gorbalenya A, Baker S, Barik R (2020) The species severe acute respiratory syndrome related coronavirus: classifying 2019-nCoV and naming it SARS-CoV-2. Nat Microbiology 5:536-544.
- int. WHO Director-General’s opening remarks at the media briefing on COVID-19- 11 March 2020 [Internet], 2020.
- Cui S, Chen S, Li X, Liu S, Wang F (2020) Prevalence of venous thromboembolism in patients with severe novel coronavirus pneumonia. J ThrombHaemost18(6):1421-1424.
- Fletcher-Sandersjöö A, Bellander BM (2020) Is COVID-19 associated thrombosis caused by overactivation of the complement cascade? A literature review. Thromb Res194:36-41.
- Levi M, van der Poll T, Büller HR (2004) Bidirectional relation between inflammation and coagulation. Circulation109(22):2698-2704.
- Nascimento JHP, Gomes BFO, Carmo Júnior PRD, et al. (2020) COVID-19 and Hypercoagulable State: A New Therapeutic Perspective. COVID-19 e Estado de Hipercoagulabilidade: Uma Nova PerspectivaTerapêutica. Arq Bras Cardiol114(5):829-833.
- Parry AH, Wani AH, Yaseen M (2020) Acute Mesenteric Ischemia in Severe Coronavirus-19 (COVID-19): Possible Mechanisms and Diagnostic Pathway. Acad Radiol27(8):1190.






























