Operative Strategy for the Prevention of Common Bile Duct Injuries during Laparoscopic Cholecystectomy
Nadjet Azzi1, Becherki Yakoubi2* and Radia Ait Chaalal3
1Department of Surgery, Hospital University of Bab El Oued Algiers, Algeria
2Department of Neurosurgery, Hospital University of Bab El Oued Algiers, Algeria
3 Department of Radiologic, Hospital University of Bab El Oued Algiers, Algeria
Submission:May 01, 2020; Published: June 09, 2020
*Corresponding author:Becherki Yakoubi, Department of Neurosurgery, BEO University Hospital, Algiers, Algeria
How to cite this article:Nadjet A, Becherki Y, Radia Ait C. Operative Strategy for the Prevention of Common Bile Duct Injuries during Laparoscopic Cholecystectomy. Open Access J Surg. 2020; 11(4): 555819. DOI:10.19080/OAJS.2020.11.555819.
Summary
Introduction: laparoscopic cholecystectomy appeared more attractive by its multiple advantages; aesthetic, early rising, less pain and above all a shorter stay, but this requires a learning curve compared to the technical means available in laparoscopy, like a limited two-dimensional but magnifying vision, innovative instruments represented by appropriate forceps allowing dissection. This is how the laparoscopic approach was decisive in the dissection of the elements of the Calot’s triangle, moreover several teams opted for various approaches; however, the incidence of bile injury by this route is higher than that which occurred during a laparotomy. These biliary injuries caused by laparoscopy are considered more serious than in laparotomy
Patients and Methods: This is a retrospective mono-centric study over a period extending from 2003-2017, it totals 2685 cases of cholecystectomies distributed by gender in 2243 female (83.5%) and 442 male (16.4%), and whose average age is 57 years with extremes (18 to 92 years). The same operator has produced this series for over a decade.
Conclusion: Biliary injury during laparoscopic cholecystectomy unfortunately remain a topical subject. Our experience has highlighted the effectiveness of an operative approach based on the choice of laparoscopic instruments minimizing electrocoagulation and allowing elective and a traumatic dissection biliary and vascular elements, knowing that the respect of the rules concerning a good exposure of the Calot’s triangle guarantees the safety of the surgical act as well as the prevention of biliary injuries.
Keywords:Laparoscopic cholecystectomy; Biliary injury; Prevention
Introduction
Laparoscopic cholecystectomy was performed for the first time in France by Philipe Mouret in 1987, and in the USA in 1988. It became a gold standard [1], which allowed its worldwide development, knowing that the open approach at that time entailed its hazards and risks like the biliary injury described above; and whose management has been known for several decades [1-5]. This is how the laparoscopic approach was decisive in the dissection of the elements of the Calot’s triangle, moreover several teams opted for various approaches; however the incidence of biliary injuries by this route is 0.1- 0.9% depending on the series, they are higher than those which occurred during a laparotomy. These biliary injuries caused by laparoscopy are considered more serious than by the laparotomy elsewhere described by CHaudhary et al. [6].
Objectives
The aim of our study is to demonstrate through our experience the advantage of a laparoscopic approach based essentially on the choice of instruments used in the dissection of the Calot’s triangle which has proven itself in the prevention of biliary injury during cholecystectomy laparoscopic.
Patients and Methods
This is a retrospective mono-centric study over a period extending from 2003 - 2017, it totals 2685 cases of cholecystectomies distributed by gender in 2243 female (83.5%) and 442 male (16.4%), and whose average age is 57 years with extremes (18 to 92 years), we collected 2353 (87.6%) uncomplicated cholecystectomy and 332 (12.3%) acute cholecystitis and chronicles. The same operator has produced this series for over a decade.
Technique
Description of the laparoscopic cholecystectomy technique
i. Installation Figure 1: French position.
ii. The pneumoperitoneum is created using a de Veress needle introduced through a supra- umbilical fascial incision and peritoneal. (Insufflation takes place at a pressure of 10-12mmHg).
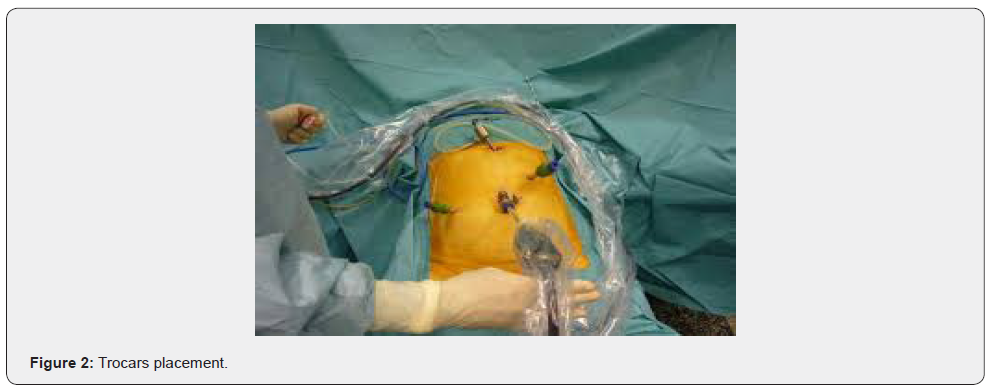
Trocars placement (Figure 2)
i. Trocar 10mm extra umbilical: camera (30-degree optics.)
ii. Trocar 5mm right hypochondrium.
iii. Trocar 5mm epigastrium (to the right of the round ligament) liver retractor.
iv. Trocar 10mm left hypochondrium: operator
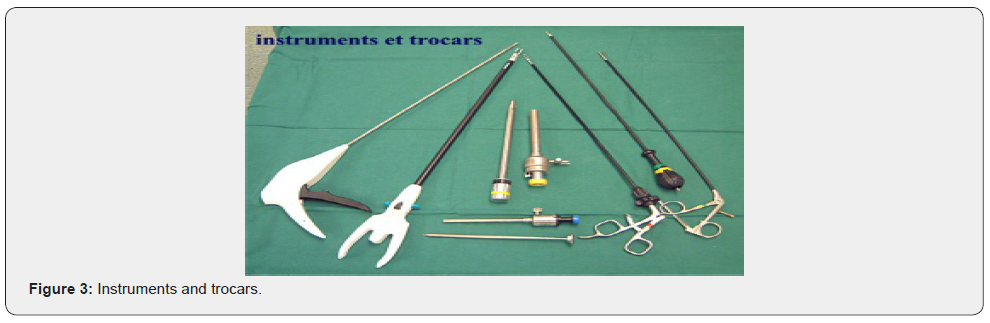
Instruments (Figure 3)
i. Window grip forceps. (5mm left hypochondrium trocar).
ii. Curved dissector forceps Figure 4. (10mm trocar right hypochondrium).
iii. Coagulator hook. (10mm right hypochondrium trocar).
iv. Scissors. (10mm right hypochondrium trocar).
v. Vacuum and retractor. (5mm epigastric trocar).
vi. Clip holder (10mm trocar left hypochondrium).
vii. 30-degree optics. (umbilical trocar).
Exposure of the calot’s triangle after horizontal traction of the crop towards the right makes it possible to highlight the cystic pedicle Figure 5.


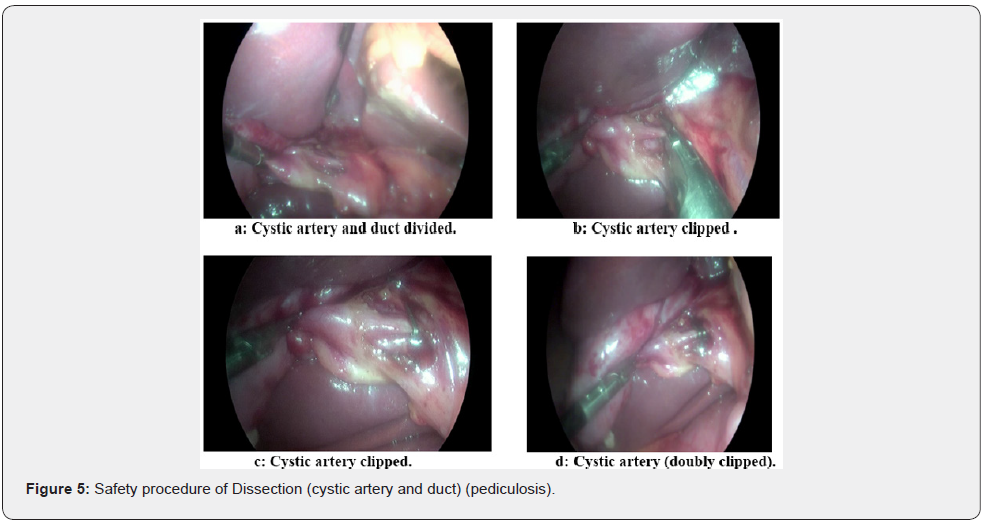
Dissection and identification of cystic pedicle (Figure 5)
Cystic pedicle horizontalized by traction; allows a rather anterior and lateral approach of the cystic elements on their free thimble; abutted at the level of the collar, the dissection is carried out using an a traumatic-curved forceps; minimizing the effect of electrocoagulation, followed by a posterior dissection requiring the verticalization of the cystic pedicle. This elective individualization allows the recognition of the main bile duct as well as the vascular and biliary anatomical varieties before even clipping or cutting, especially in case of cholecystitis (pediculitis, fibrosis, bleeding), this step requires excellent visibility
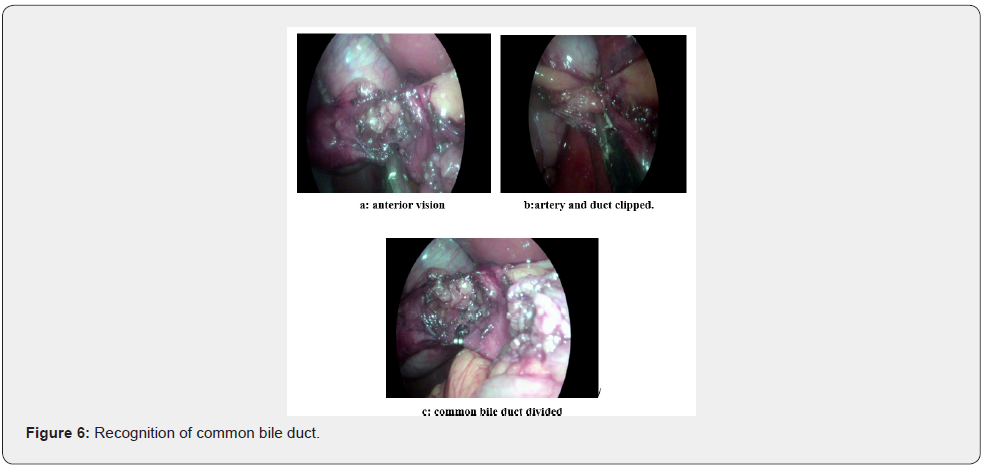
Installation of clips (Figure 6)
The installation of the clips requires the horizontalization of the cystic elements, allowing to have a cystic duct axis perpendicular to the common biliary duct.
i. Set up of two clips on the cystic elements (artery and canal).
ii. Section of cystic elements with scissors Figure 7.
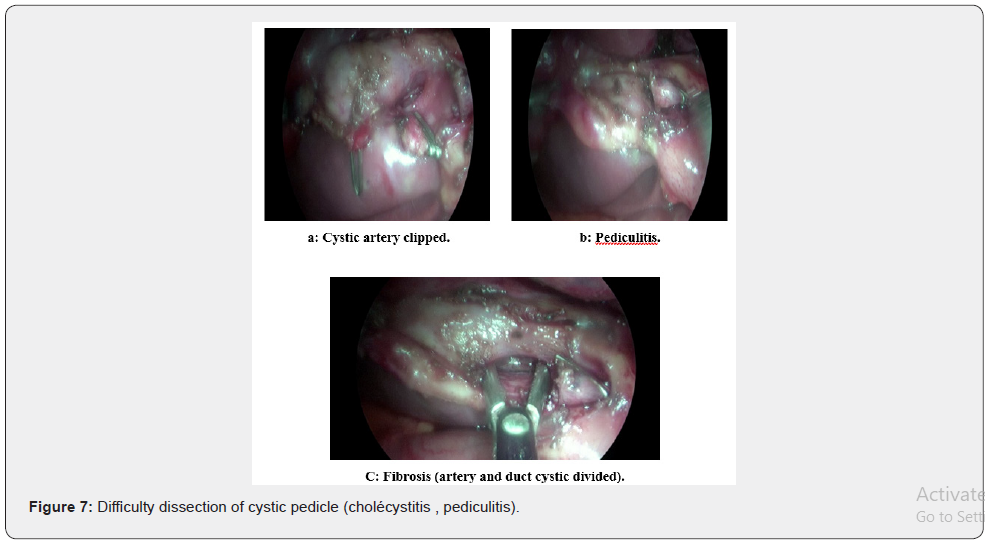
Cholecystectomy
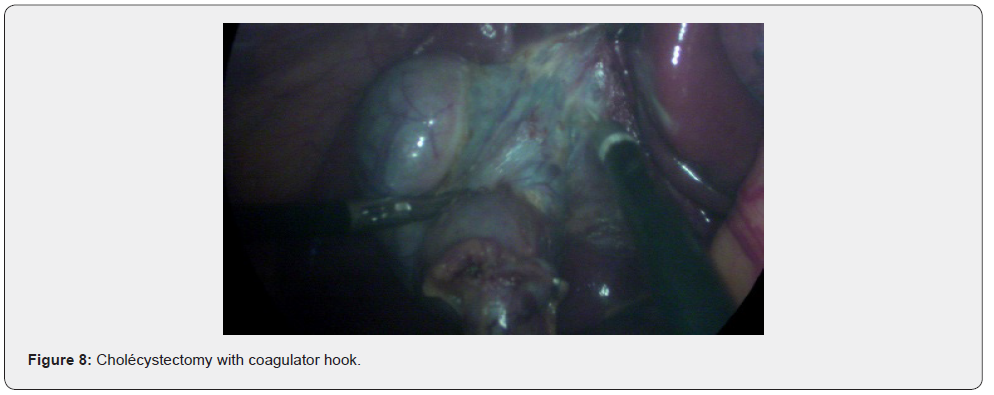
Cholecystectomy is performed with the coagulator hook Figure 8, retrograde or anterograde depending on the difficulties.
Results
Our centre did not collect any biliary injury during or after laparoscopic cholecystectomies.
Rates of the bile injury ducts: 0%
In addition, complications that occurred during the surgical procedure (Table 1) were noted; as haemorrhages in 12 patients related to the cystic artery; at the introduction of the trocar the latter was a source of colonic and vascular injuries in 2 patients, difficulties were observed during acute and chronic cholecystitis (n = 74) which represents 22% of cases, so we have collected 2 cases of biliary fistula. Other reasons for conversion such as the discovery of a gastric stromal tumor, and for hemodynamic instability for an undetermined reason.
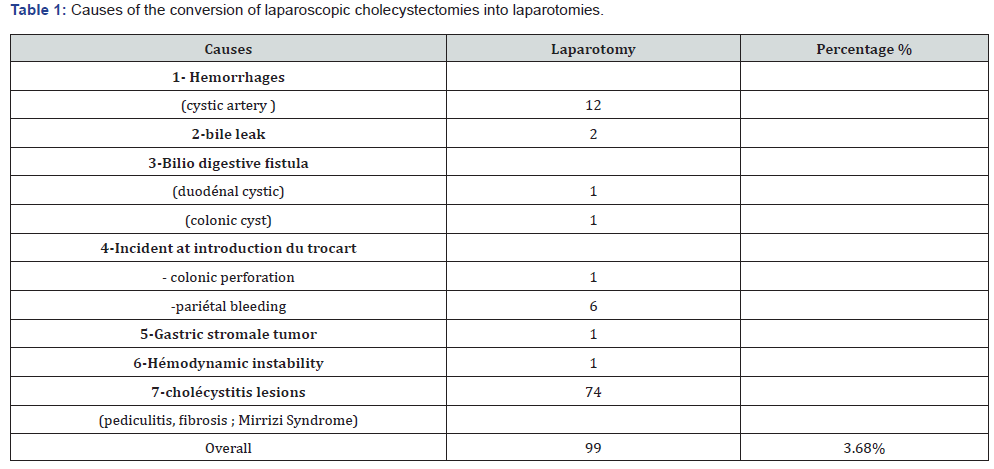
We converted 99 patients to laparotomy, a rate of around 4%.
Duration of operation
i. start 190mn and 45 minutes average
ii. Minimum 12 minutes.
iii. Maximum 180 minutes.
Discussion
Surgical expertise
The learning curve remains the key factor contributing to the high rate of main bile duct injuries at the start of the experiment, thus demonstrating that the risk of main bile duct injuries was 1.7% during the first cholecystectomy and 0.57% when the surgeon had already performed 50 procedures (Graph 1). A surgical group [7] showed that 90% of biliary tract wounds in a series of 8839 laparoscopic cholecystectomies occurred mainly before the first 30 cases in the surgeon’s experience.
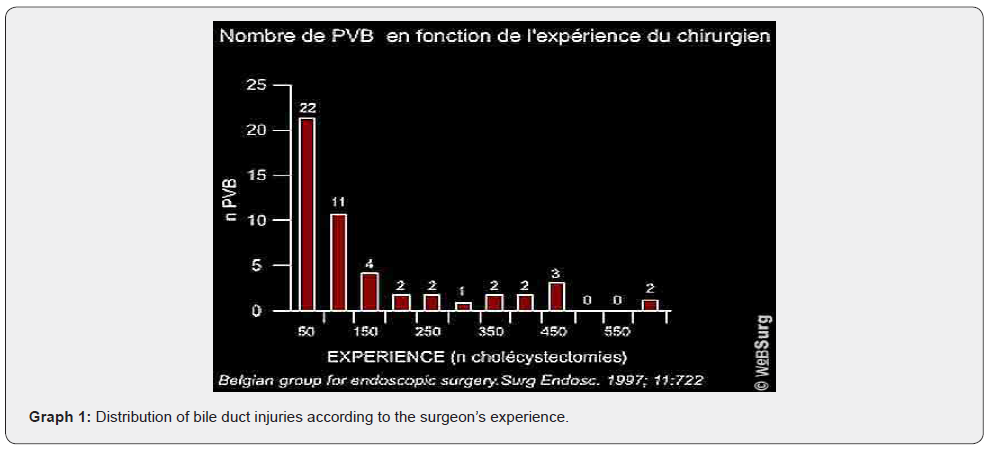
Instruments
The rate of biliary injury during Laparoscopic Cholecystectomy (Table 2) remains higher than in laparotomy (rate: 0.3 to 0.8%) they are particularly more complex, and above all very serious, because they generally result from a technical or instrumental fault. Indeed, the specific mechanism of biliary injury during the laparoscopic approach is twofold: technical (section, clipping, tearing, shredding) or thermal, the latter generated by the coagulating hook causing burns that can be extended and even source of biliary necrosis early or late bile stenosis depending on the extent of the thermal attack; moreover, monopolar electrocoagulation has been clearly implicated in this complication, justifying its sparing use during the dissection of Calot’s triangle [8,9].

Risk factors
The risk factors must be taken into account in the genesis of the biliary injuries, they are linked above all to the patient (advanced age; the male obesity), and to the local factors linked to the gallbladder, besides the rate of wounds gallbladder is high (cholecystitis: 5.5%) [10]. (Inflammation: cholecystitis, fibrosis, Difficulties related to excessive bleeding; anatomical varieties). There are other factors to consider, inherent in the laparoscopic approach; since it only offers. Only a two-dimensional vision of the operating field, which is insufficient since it combines the absence of palpation of the hepatic pedicle and a tangential or lower dissection on contact with the main bile duct. The instrumental means used in laparoscopy (hook coagulator) are also incriminated and increases the risk of injury to the bile ducts adding the surgeon’s inexperience with all of the other risk factors (patient, local).
Technique
The technical stages of cholecystectomy by laparotomy are similar to those by laparoscopy, however the difficulties encountered differ, they are linked to a poor adaptation of the operator to a two-dimensional visual field, as well as to the instrumental means whose choice remains questionable. In addition, some authors have described the principles to prevent biliary injuries; by paying close attention to the undeniable contribution of the laparoscopic route during cholecystectomy, Biliary injuries are prevented by a careful operative technique [11-15].
These steps are as follows:
i. Perfect exposure of the operating field with tensioning of the hepatic pedicle.
ii. Pulling up the liver.
iii. Pulling down the abdominal viscera through the proclive position.
iv. Perfect vision of the pedicle structures is essential; it must be like that of laparotomy, for this an optic (an angle of 30 degrees) can be used [15-18].
v. The exposure of the Calot’s triangle hence the importance of the lateral traction of the cystic infundibulum to open the triangle (cystic channel is 90 degrees from the common bile duct) [11-13].
vi. American technique (gallbladder is pushed upwards) [15,18].
vii. anterior and posterior during the dissection of the Calot’s triangle [19].
viii. Dissection begins at the level of the collar (identification of the cystic-common bile junction).
ix. Exact identification of the cystic duct and common bile duct. [14,20-22].
x. Careful use of coagulation is necessary during the dissection of the Calot’s triangle.
xi. The use of intraoperative cholangiography must be carried out in case of doubt after complete dissection before any ligature or section.
xii. Liberation of the gallbladder can be done completely in contact with it.
xiii. If unidentified canal structures; conversion to laparotomy is an attitude of safety.
Our experience
Has demonstrated the advantage of a laparoscopic approach which is essentially based on:
i. The choice of instrumentation (30° optics, fine and curved forceps).
ii. The exposure of the calot’s triangle which consists:
a) Retraction of the liver (exposure of the sub hepatic region).
b) Gripping the infundibular area of the gallbladder in the horizontal axis for anterior and vertical vision for a double lateral and posterior vision of the cystic pedicle.
iii. An elective atraumatic dissection minimizing electrocoagulation of the ductal elements:
a) Dissection beginning at the level of the vesicular neck.
iv. Identification and detection of bile and vascular elements in relation to the common bile duct and the lower hepatic border.
Apart from the anatomical varieties. We encountered difficulties mainly related to the confinement of large stones in addition to the inflammatory and haemorrhagic lesions caused by acute cholecystitis, which cause a shortening of the cystic elements adhering to the lateral edge of the common bile duct. In these cases we have always recommended the initiation of dissection without coagulation, using the tip of the curved forceps, with its branches opening in the horizontal direction and parallel to the duct which allows to widen this passage to the lateral edge of the common bile duct. This dissection gesture is atraumatic and makes it possible to avoid the thermal effect of electrocoagulation near the biliary duct. This dissection is valid for inflammatory tissues and even for fibrosis.
After individualization and recognition of the cystic pedicle, these are doubly clipped (artery). The coagulating hook usually performs cholecystectomy, it is retrograde unless ignorance or difficulties during individualization of the canal becomes anterograde and allows control of the cystic pedicle. Biliary injury during laparoscopic cholecystectomy unfortunately remain a topical subject. Our experience has highlighted the effectiveness of an operative approach based on the choice of laparoscopic instruments minimizing electrocoagulation and allowing elective and atraumatic dissection biliary and vascular canal elements, knowing that the respect of the rules concerning a good exposure of the calot’s triangle guarantees the safety of the surgical act as well as the prevention of biliary injuries. Our study demonstrated the value of surgical expertise, which comes above all from respect for the known principles of open surgery combining it with the laparoscopic approach.
Conclusion
A good dissection allows recognition of the biliary and vascular elements in an atmosphere of inflammation or fibrosis and even in the case of anatomical varieties; except that it is based on a judicious choice of the instrumental means offered by laparoscopy. Only for a better introduction to laparoscopic cholecystectomy, it is necessary to consider the technical imperatives in order to prevent iatrogenic injury of the bile ducts, and especially to convert to laparotomy in the event of major difficulties, dead ends or doubts. The laparoscopic approach is only one-way, it requires expertise, and it should not contribute to the genesis of a lesion which at the start is minimal and whose aggravation can become irreversible.
References
- Shea JA, Healey MJ, Berlin JA, Clarke JR, Malet PF, et al. (1996) Mortality and complications associated with laparoscopic cholecystectomy, a meta-analysis. Ann Surg 224: 609-620.
- Bismuth H, Lazorthes F (1981) Les traumatismes opératoires de la voie biliaire principale. Masson, Paris, France.
- Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomyJ. Am Coll Surg 180: 101-125.
- Fletcher DR, Hobbs MST, Phil D, Tan P, Valinski LJ, et al. (1999) Complications of cholecystectomy : risks of the laparoscopic approach and protective effects of operative cholangiography. A population-based study. Ann Surg 229 : 449-457.
- EM Marco C, Balagué C, Rodriguez J, Cugat E, Hoyuela, et al. (1998) How, when, and why bile duct injury occurs Surg. Endosc 12: 322-326.
- Chaudhary A, Manisegran M, Chandra A, Agarwal AK, Sachdev AK (2001) How do bile duct injuries sustained during laparoscopic cholecystectomy differ from those during open cholecystectomy? J Laparoendosc Adv Surg Tech A 11 : 187-189.
- A prospective analysis of 1518 laparoscopic cholecystectomies - The Southern Surgeons Club (1991) N Engl J Med 324: 1073-1078.
- Gigot, Jean-François (2007) Les plaies biliaires des cholécystectomies par laparoscopie : [Bile duct injury during laparoscopic cholecystectomy]. Journal de Chirurgie 144(5): 383-384.
- Chirurgie des voies biliaires, par J- F .Gigot (2005) Collection Techniques Chirurgicales. Masson, Paris, France 148.
- C K Kum, P M Goh, J R Isaac, Y Tekant, S S Ngoi (1994) Laparoscopic cholecystectomy for acute cholecystis Br J Surg 81: 1651-1654.
- Jacques Perissat (1993) Laparoscopic cholecystectomy :The European experience. AMJ Surg 165(4) : 444-449.
- J Perissat, D Collet, M Edye, E Magne, R Belliard, et al. (1992) Laparoscopic cholecystectomy : An analysis of 777 cases. 6(4) : 727-742
- F Dubois (1995) Laparoscopic cholecystectomy : The French Technique. Operative Strategies in Laparoscopic Surgery, Springer, pp.30-33.
- G Branum, C Schmitt, J Baillie, P Suhocki, M Baker, et al. (1993) Management of Major Biliary complication after Laparoscopic cholecystectomy Ann Surg 217(5): 532-541.
- Hunter JG (1991) Avoidance of bile duct injury during laparoscopic cholecystectomy. Am J Surg 162: 71-76.
- J G Hunter (1993) Exposure, dissection, and laser versus electrosurgery in laparoscopic cholecystectomy. Am J Surg 165(4): 492-496.
- Hunter J (1997) Advanced laparoscopic surgery. American Journal of Surgery 173(1): 14-20.
- KD Horvath (1993) Strategies for the prevention of laparoscopic common bile duct injuries. Surg Endosc 7(5): 439-444.
- Soper NJ, Stockmann PT, Deanna DL, Ashley SW (1992) Laparoscopic Cholecystectomy The New 'Gold Standard . Arch Surg 127(8): 917-923.
- Davidhoff AM, Pappas TN, Murray EA, DJ Hilleren, RD Johnson, et al. (1992) Mechanisms of major biliary injury during laparoscopic cholecystectomy. Ann Surg 215: 196-202.
- Olsen DO, Asbun HJ, Reddick EJ, Spaw AT (1991) Laparoscopic cholecystectomy for acute cholecystitis. Prob Gen Surg 8: 426.
- AM Ress, MG Sarr, DM Nagorney, MB Farnell, JH Donohue, et al. (1993) Spectrum and management of major complications of laparoscopic cholecystectomy 165(6): 655-652.






























