The Atypical Clarification -Trichilemmal Carcinoma
Anubha Bajaj*
Consultant Histopathologist, Panjab University, India
Submission:February 21, 2020; Published: March 13, 2020
*Corresponding author:Anubha Bajaj, Consultant Histopathologist, Panjab University, India
How to cite this article:Anubha Bajaj. The Atypical Clarification -Trichilemmal Carcinoma. Open Access J Surg. 2020; 11(4): 555816. DOI:10.19080/OAJS.2020.11.555816.
Preface
Trichilemmal carcinoma is an exceptional, malignant cutaneous adnexal neoplasm derived from extraneous root sheath of the hair follicle. The external hair follicular root sheath is comprised of clear cells with vacuolated cytoplasm and abundant intracellular glycogen. Trichilemmal carcinoma was initially scripted by Headington as a “historically invasive, atypical clear cell neoplasm of adnexal keratinocytes contiguous with superimposed epidermis and/or follicular epithelium” [1]. Trichilemmal carcinoma is discerned upon cogent histopathological examination with complementary and confirmatory immune histochemical reactions [1,2].
Keywords:Trichilemmal carcinoma; Hair follicular; Adnexal keratinocytes; Histochemical Reactions; Lesions; Tuberculosis; Biological behaviour; Inferior prognosis; Epithelial membrane Antigen; Cisplatin
Disease Characteristics
As a malignant version of trichilemmoma, trichilemmal carcinoma demonstrates a predilection for sun exposed, hair bearing cutaneous surfaces. Trichilemmal carcinoma as a cutaneous adnexal tumour exemplifies a lesion distribution within zones of sunlight exposure or a concomitant appendageal origin and occurs predominantly upon the head and neck region [1,2]. Apart from distribution of lesions upon regions of sunlight exposure, trichilemmal carcinoma appears in burn scars or elderly subjects subjected to radiography for discernment of pulmonary lesions such as tuberculosis. Nevertheless, pathogenesis of trichilemmal carcinoma remains poorly explained [1,2]. A recent, abrupt stage of tumour growth is encountered within a phase of delayed tumour progression. Despite an aggressive pattern of tumour evolution, trichilemmal carcinoma delineates an indolent clinical course, which is primarily indicative of a benign neoplastic process, amenable to comprehensive surgical excision [2,3]. Trichilemmal carcinoma demonstrates a minimal metastatic potential, deep-seated tumour infiltration and occasional localized reoccurrence of the tumefaction, although the neoplasm is devoid of distant metastasis. Localized cervical or regional lymph node metastasis and distant metastasis are infrequently encountered in trichilemmal carcinoma. As investigative modalities for discerning trichilemmal carcinoma are inadequately denominated, biological behaviour and prognostic outcomes are challenging to predict [3]. Metastatic trichilemmal carcinoma is associated with an inferior prognosis. Possible emergence of tumour reoccurrence and lymph node metastasis can be proportionate to aforesaid manifestations of squamous cell carcinoma. Median follow up of trichilemmal carcinoma usually is 63.8 months and varies from one month to 147 months. On account of exceptional nature of the neoplasm, significant data is unavailable [3,4].
Clinical Elucidation
Trichilemmal carcinoma arises as a solitary, indolent neoplasm although multiple lesion can emerge upon non-exposed cutaneous surfaces. Trichilemmal carcinoma is a gradually progressive neoplasm cogitated within an elderly population, appearing as a pale, tan or reddish papule, indurated plaque or a nodule. The lesion is generally discerned upon scalp, forehead, face, neck, trunk, upper extremities, temporal or occipital region, nape or lower lip and demonstrates a varying magnitude betwixt 0.4 centimetre to 8 centimetres with a mean dimension of 2.8 centimetres. Majority (80%) of lesions demonstrate a clear, tumour-free margin. Prior to appropriate detection, the tumefaction can occur from 2 months to up to 50 years, followed by rapid tumour progression [3,4]. As trichilemmal carcinoma can be frequently misinterpreted as a benign lesion, a clinical demarcation is necessitated from neoplasms such a squamous cell carcinoma, basal cell carcinoma, nodular variant of malignant melanoma or a kerato-acanthoma [4].
Histological Elucidation
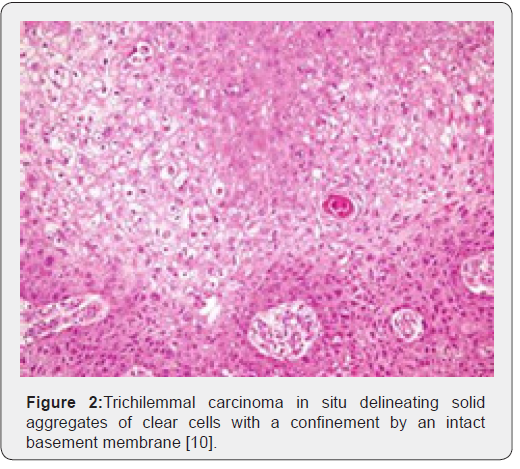
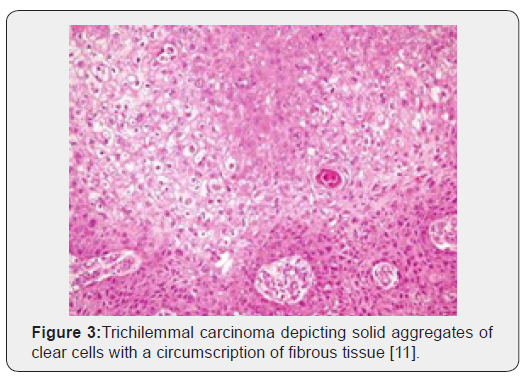
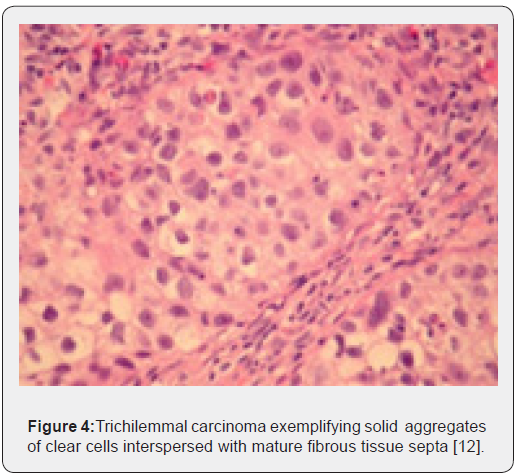
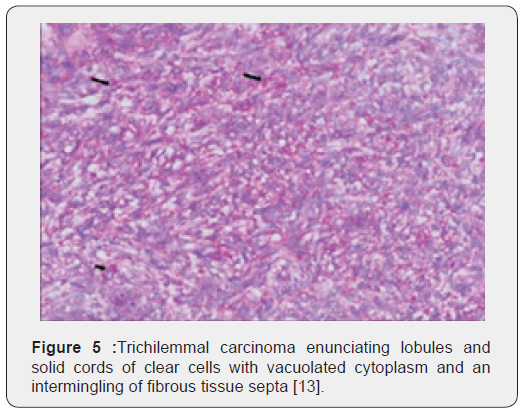
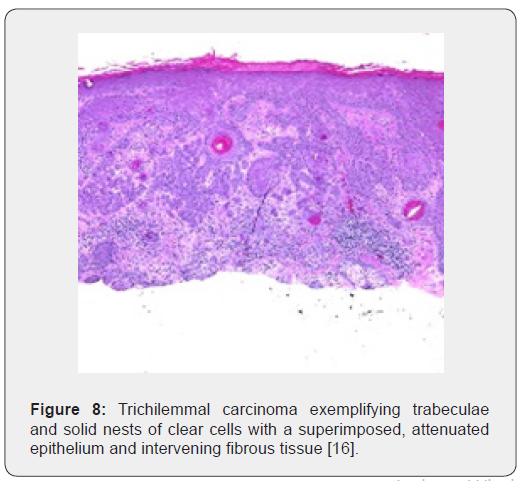
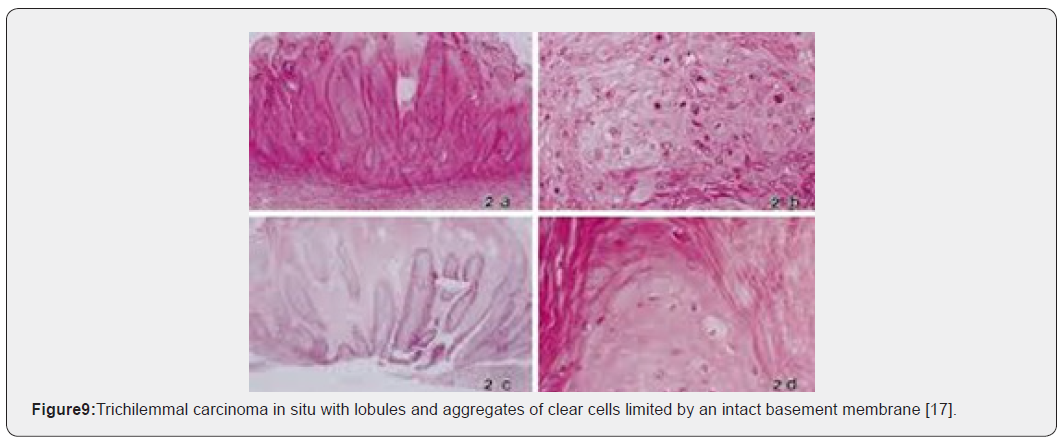
Trichilemmal carcinoma is an exceptional, malignant neoplasm delineating histological features of an intermediate to high grade malignancy. Grossly, the lesions are polypoid, exophytic, ulcerated, nodular or haemorrhagic [4,5]. On microscopy, trichilemmal carcinoma demonstrates diverse configurations such as solid, lobular or a trabecular pattern of growth. Sharply defined, infiltrative tumour lobules depict a pushing tumour perimeter and a hyaline membranous envelop which can be highlighted by a periodic acid Schiff’s (PAS) stain. Cellular constituents configuring the lobules are enlarged tumour cells impacted with clear or pale-staining, eosinophilic cytoplasm which is reactive to periodic acid Schiff’s (PAS) stain with diastase sensitivity and non-reactive to mucin stains. Peripheral palisading of cells, subnuclear vacuolization and numerous mitotic figures are observed. Foci of pilar subtype of keratinization and few dyskeratotic cells are discerned. Zones of actinic damage demonstrate superficial cutaneous ulceration. The tumour delineates a pagetoid form of dissemination or infiltration into the deep-seated dermis can be enunciated [4,5]. Immune reactivity to cytokeratin along with immune non-reactive carcinoembryonic antigen (CEA) and epithelial membrane antigen (EMA) are exemplified [5].
Differential Diagnosis
Trichilemmal carcinoma requires a segregation from various clear cell carcinomas arising from the cutaneous surfaces. Trichilemmoma and clear cell hidradenoma are benign tumours which lack an infiltrative pattern of tumour growth and cytological atypical [6]. Trichilemmal carcinoma and malignant proliferating trichilemmal tumour are described as two distinct entities wherein malignant proliferating trichilemmal tumour is engendered from a pre-existing trichilemmal cyst and is accompanied by a distinct metastatic potential [6].
Therapeutic Options
Trichilemmal carcinoma is amenable to a comprehensive surgical extermination with a broad perimeter of uninvolved, circumscribing soft tissue. As the appropriate therapeutic management is a complete surgical eradication of the neoplasm with a clear, tumour free surgical margin, a subsequent, periodic surveillance is advantageous, especially in the absence of cogent adjuvant therapy [7]. Histologically tumour free surgical perimeter is critical for assessing features such as localized tumour infiltration or a potential, localized tumour reoccurrence. Localized tissue reconstruction with rotation flap and skin grafting can be adopted following adequate surgical eradication of the neoplasm. Regardless of a comprehensive surgical excision with a tumour free margin, tumour reoccurrence can appear within an estimated 8% instances [7,8]. Adequate surgical extermination of the neoplasm with satisfactory eradication of the surgical border is a safe, cost-effective and an efficacious methodology of treating trichilemmal carcinoma. Post- operative follows up is mandated to facilitate a preliminary discernment of disease reoccurrence and distant metastasis [7,8]. Optimal treatment of trichilemmal carcinoma with metastasis lacks consensus and an established chemotherapeutic or adjunctive treatment regimens are absent. Regional lymph node and distant metastasis are accompanied by a mortality rate of roughly (8%) following a surgical extermination and cogent chemotherapy with cisplatin and vindesine is recommended. Combination therapy with cisplatin and cyclophosphamide can induce with a partial remission as it controls the tumour progression although alleviation of the tumefaction is absent [8]. Concurrence of 5- fluouracil with cisplatin is accompanied by an inferior prognosis. Moreover, administration of cisplatin with adriamycin and vindesine (CAV treatment) recapitulates the therapeutic regimen of high grade, advanced squamous cell carcinoma. Reoccurring lesions of trichilemmal carcinoma associated with distant metastasis are generally refractory to therapy. Administration of cogent chemotherapy can curb tumour progression. Following adequate surgical of the neoplasm, tumour reoccurrence is usually absent for a period of few months. Definitive, discernible distant metastasis is optimally treated with systemic chemotherapy comprised of a combination of cisplatin and vindesine or cisplatin with cyclophosphamide [7,8] (Figures 1-9).



References
- Reis JP, Tellechea O, Cunha A, Poiares Baptista (1993) Trichilemmal carcinoma: review of 8 cases. J Cutan Pathol 20(1): 44-49.
- Xu DB, Wang T, Liao Z (2018) Surgical treatment of trichilemmal carcinoma. World J Oncol 9(5-6): 141-144.
- Boscaino A, Luigi Maria Terracciano, Vittoria Donofrio, Gerardo Ferrara, Gaetano De Rosa (1992) Trichilemmal carcinoma: a study of seven cases J Cutan Pathol 19(2): 94-99.
- Swanson PE, Marrogi AJ (1992) Trichilemmal carcinoma: a clinico-pathologic study of 10 cases. J Cutan Pathol 19(2): 100-109.
- Maize JC, Snider RL (1995) Non melanoma skin cancers in association with seborrheic keratosis: Clinico-pathologic correlations. Dermatol Surg 21(11): 960-962.
- Garrett AB, Azmi FH (2004) Trichilemmal carcinoma: a rare cutaneous malignancy: a report of two cases. Dermatol Surg 30(1): 113-115.
- Yi HS, Sym SJ, Park J, Cho EK, Ha SY, et al. (2010) Recurrent and metastatic trichilemmal carcinoma of the skin over the thigh: a case report. Cancer Res Treat 42(3): 176-179.
- Miguel Roismann, Rosyane Rena de Freitas, Leandro Carvalho RibeiroII, Marcos Flávio Montenegro, Luciano José Biasi, et al (2011) Trichilemmal carcinoma: case report. Am Bras Dermatol 86(5): 991-994.
- Image 1 Courtesy: Scielo Br.
- Image 2 Courtesy: LWW Journal.
- Image 3 Courtesy: Springer Link.
- Image 4 Courtesy: Dermnet NZ.
- Image 5 Courtesy: Indian J Dermatol Venereol Leprol.
- Image 6 and 7 Courtesy: Research Gate.
- Image 8 Courtesy: Dermatology advisor.
- Image 9 Courtesy: Medical Journals.






























