Gastric Cancer after H. Pylori Eradication therapy develops in the Intermediate Zone. Relationship to Spasmolytic Polypeptide-Expressing Metaplasia
Kazuyoshi Yagi1, Ikuo Nagayama1, Takahiro Hoshi1, Satoshi Abe1, Shinichi Morita1, Tsuyoshi Suda1, Yu ichi Sato2 and Shuji Terai3
1Department of Gastroenterology and Hepatology, Niigata University Medical and Dental Hospital, Japan
2Department of Internal Medicine, Japan
3University Graduate School of Medical and Dental Sciences, Japan
Submission: April 12, 2018; Published: April 30, 2018
*Corresponding author: Kazuyoshi Yagi, Department of Gastroenterology and Hepatology, Uonuma Institute of Community Medicine, Niigata University Medical and Dental Hospital, Japan, Fax: ; Email: yagikazu@popl2.odn.ne.jp
How to cite this article: Kazuyoshi Y, Ikuo N, Takahiro H, Satoshi A, Shinichi M, et.al. Gastric Cancer after H. Pylori Eradication therapy develops in the Intermediate Zone. Relationship to Spasmolytic Polypeptide-Expressing Metaplasia. Open Access J Surg. 2018; 9(1): 555751. DOI: 10.19080/OAJS.2018.09.555751
Introduction
The relationship between H. pylori infection and gastric cancer has been acknowledged for almost 20 years [1]. Some studies have demonstrated that H. pylori eradication reduces the incidence of gastric cancer [2], and consequently the health insurance system in Japan has approved eradication therapy for patients with H. pylori gastritis. However, even after successful H. pylori eradication therapy, some patients still develop gastric cancer. Furthermore, the endoscopic appearance of gastric cancer after eradication therapy is reported to resemble gastritis, making it difficult to diagnose the extent of the cancer [3-5]. Saka et al. [5] have clarified the characteristic endoscopic features and histological characteristics of gastric cancer after eradication therapy, thus facilitating more accurate diagnosis. Nawata et al. [6] have reported the characteristic endoscopic features of the stomach that tend to be predictive of gastric cancer development after eradication.
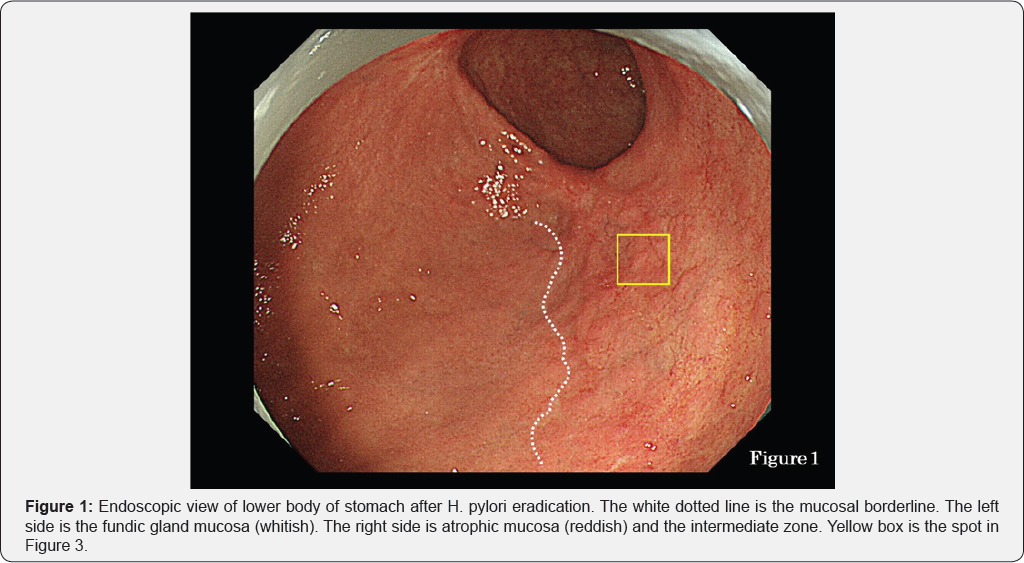
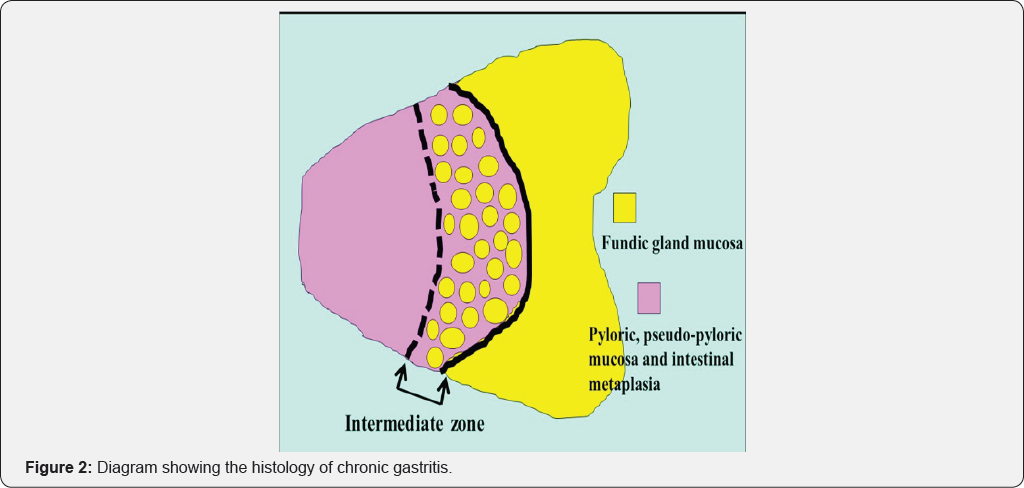
This has been termed the "reversal phenomenon" on the mucosal borderline [6]. In chronic active gastritis due to H. pylori, inflammation activity is more marked in the fundic gland mucosa than in atrophic mucosa including intestinal metaplasia. Therefore, in chronic active gastritis, the fundic gland mucosa appears reddish and atrophic mucosa appears whitish [7]. After eradication, inflammation activity disappears from the fundic gland mucosa and its color changes from reddish to whitish. This means that the color of the atrophic mucosa has a relatively reddish hue when observed by endoscopy. This color change corresponds to the "reversal phenomenon" (Figure 1). In the atrophic mucosa, a whitish elevated area is evident within the reddish part (Figure 1). This area is termed the intermediate zone [8,9]. In chronic gastritis, the intermediate zone is the area in which fundic glands, pseudo-pyloric glands and intestinal metaplasia coexist, representing the border between adjacent atrophic mucosa and fundic gland mucosa (Figure 2). Endoscopically, the whitish elevated part in the intermediate zone is fundic gland mucosa and the reddish part is intestinal metaplasia (Figure 1).
Using endoscopy, we studied 43 lesions of gastric cancer after eradication therapy and found that 19 of them were located in the intermediate zone (Table 1). Furthermore, histological examination revealed that 29 lesions were located in the intermediate zone (Table 1). Figure 1 shows a case of gastric cancer after eradication therapy. The yellow box in the figure shows a lesion suspected to be cancerous because of its slightly whitish hue. This suspected cancerous lesion was located in the intermediate zone containing a mixture of whitish elevated areas and reddish areas. NBI (narrow-band imaging) endoscopy at lower magnification revealed an unclear white zone [10] pattern and an irregular vascular pattern, suggestive of cancer (Figure 3, white arrows).
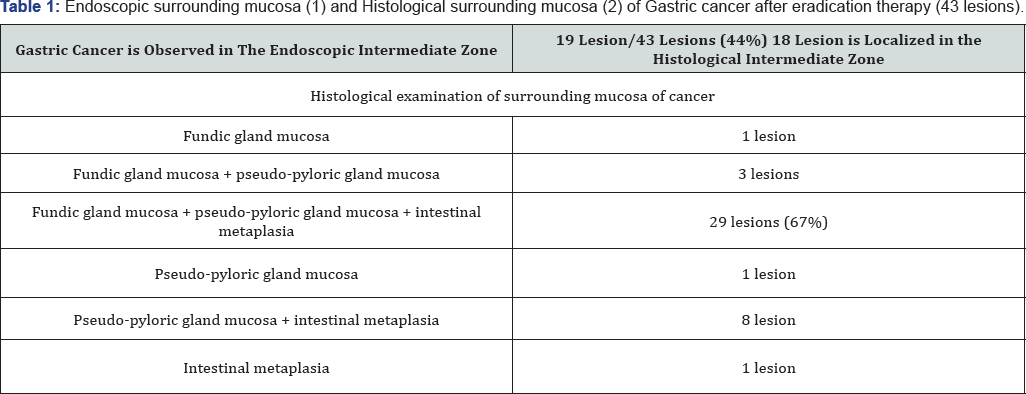

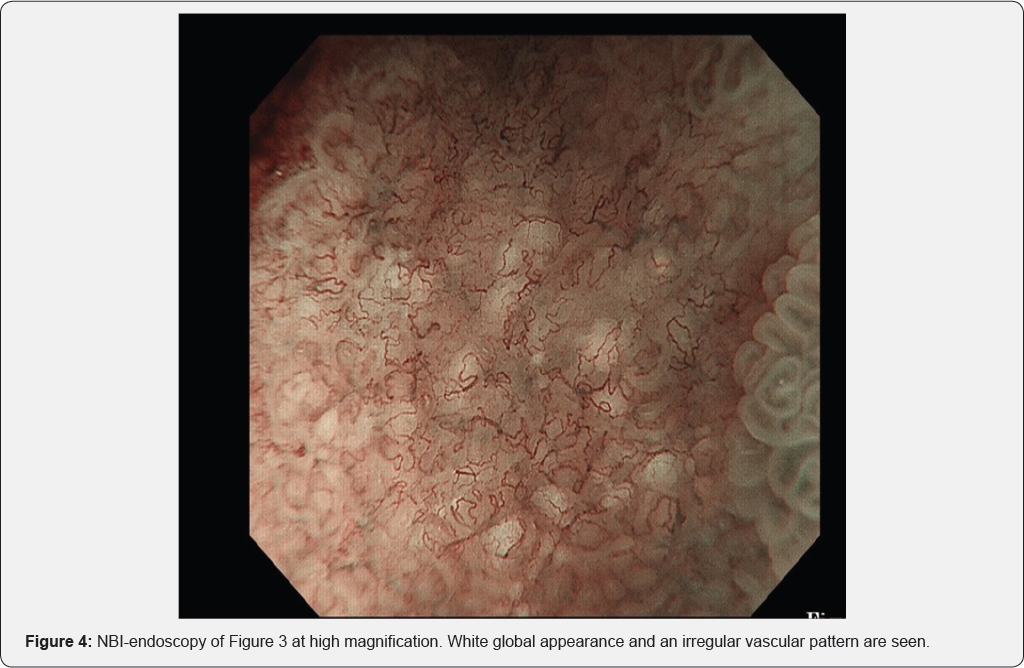
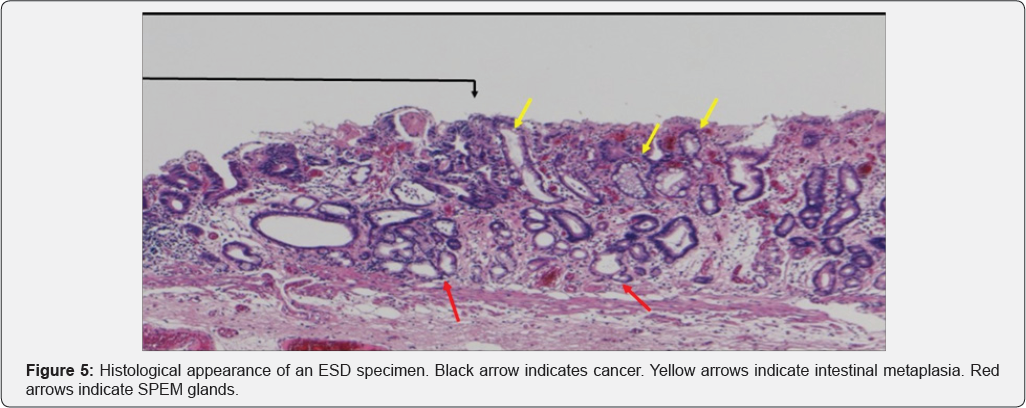
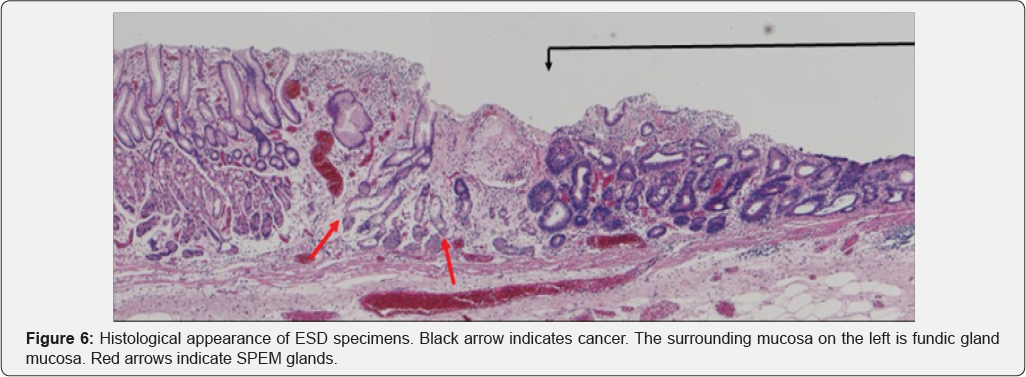
In Figure 3, area A shows round pits indicating fundic gland mucosa and area B shows a tubular pattern indicating atrophic mucosa or intestinal metaplasia [11,12], thus corresponding to the intermediate zone. NBI-endoscopy at high magnification demonstrated a white global appearance [13] with an irregular vascular pattern (Figure 4). A biopsy specimen was diagnosed as differentiated adenocarcinoma, and endoscopic submucosal dissection (ESD) was performed. The ESD specimen showed mucosal differentiated adenocarcinoma (Figure 5 & 6 black arrows). In addition, intestinal metaplasia (Figure 5 yellow arrows) and fundic glands (Figure 6) were seen in the surrounding mucosa, thus corresponding to the intermediate zone.
Many articles have suggested that development of gastric cancer is related to intestinal metaplasia [14,15] and that gastric cancer occurring after H. pylori eradication therapy also has a relationship with intestinal metaplasia [16]. However, we recognized that gastric cancer after eradication therapy developed more frequently in the intermediate zone than in areas of intestinal metaplasia. No previous reports have suggested that fundic glands and pseudo-pyloric glands are related to the development of gastric cancer. Our results suggest that the process of metaplasia from fundic glands to pseudo- pyloric glands and intestinal metaplasia may be related to development of gastric cancer. This process is evident in the case of spasmolytic polypeptide-expressing metaplasia (SPEM) [17-19].
In SPEM, loss of parietal cells disrupts the proper differentiation of other lineages such as chief cells [18,20], and metaplasia from chief cells to mucus cells forming glands with dilatation occurs [17-19]. These glands are similar to Brunner glands or antral pyloric glands [17-19]. This process of SPEM occurs as a result of inflammation due to H. pylori [17-19] or administration of drugs [21]. These mucus cell glands are referred to as SPEM glands [17-19], and correspond to pseudo- pyloric glands pathologically. Furthermore, goblet cells appear in SPEM glands, marking the onset of intestinal metaplasia [19]. Yoshizawa et al. [19] have reported that H. pylori infected Mongolian gerbils developed SPEM initially in the intermediate zone along the lesser curvature, and that this subsequently spread out towards the greater curvature, goblet cell intestinal metaplasia developing only at a late stage of infection. They concluded that SPEM develops early in H. pylori infection in this model, and that alterations in gland morphology arise from SPEM glands during the course of gastric infection, goblet cell intestinal metaplasia developing subsequent to SPEM [19]. We recognized that the histological findings described by Yoshizawa et al. correspond to the histological features in the surrounding mucosa of the gastric cancers we observed after eradication therapy. SPEM glands are evident in Figures 5 & 6 (red arrows). Goldenring et al. have also stated that gastric cancer develops from SPEM glands, and not from intestinal metaplasia [17,18].
SPEM is thought to be most active in the intermediate zone, and accordingly gastric cancer is thought to develop there. The fact that 29 of 43 (67%) gastric cancer lesions we observed were located in the intermediate zone appears to support this. Therefore it appears that more attention should be paid to alterations in gland morphology from chief cells to SPEM, and subsequently to intestinal metaplasia, to clarify the development of gastric cancer, including analysis of genetic variation. Our present results suggest a paradigm shift when considering the development of gastric cancer.
References
- Uemura N, Okamoto S, Yamamoto S, Matsumura N, Yamaguchi S, et al. (2001) Helicobacter pylori infection and the development of gastric cancer. N Engl J Med 345(11): 784-789.
- Fukase K, Kato M, Kikuchi S, Inoue K, Uemura N, et al. (2008) Effect of eradication of Helicobacter pylori on incidence of metachronous gastric carcinoma after endoscopic resection of early gastric cancer: an open-label, randomized controlled trial. Lancet 372(9636): 392-397.
- Ito M, Tanaka S, Takata S, Oka S, Imagawa S, et al. (2005) Morphological changes in human gastric tumors after eradication thrapy of Helicobacter pylori in a short-term follow-up. Aliment Pharmacol Ther 21(5): 559-566.
- Kobayashi M, Hashimoto S, Nishikura K, Mizuno K, Takeuchi M, et al. (2013) Magnifying narrow-band imaging of surface maturation in early differentiated-type gastric cancers after Helicobacter pylori eradication. J Gastroenterol 48(12): 1332-1342.
- Saka A, Yagi A, Nimura S (2016) Endoscopic and histological features of gastric cancers after successful Helicobacter pylori eradication therapy Gastric Cancer 19(2): 524-530.
- Yoshitaka Nawata, Kazuyoshi Yagi, Megumi Tanaka, Atsuo Nakamura (2017) Reversal phenomenon on the mucosal borderline related to development of gastric cancer after successful eradication of H. pylori. Journal of Gastroenterology and Hepatology Research 6(12): 1-6.
- Yagi K, Nakamura A, Sekine A (2002) Magnifying endoscopy of the gastric body: a comparison of the findings before and after eradication of Helicobacter pylori Digestive Endoscopy 14(1): S76-S82.
- Yagi K, Ajioka Y (2016) Endoscopic diagnosis of gastric cancer after H. pylori eradication therapy. Igakuchoin, Tokyo, Japan.
- Iida Y (1979) Morphological and functional studies on endoscopic atrophic border, mainly intermediate zone. Gastroenterol Endosc 21: 155-169.
- Yagi K, Nozawa Y, Endou S, Nakamura A (2012) Diagnosis of early gastric cancer by magnifying endoscopy with NBI from view point of histological imaging: Mucosal patterning in terms of white zone visibility and its relationship to histology. Diagn Ther Endosc 2012: 954809.
- Yagi K, Nakamura A, Sekine A (2002) Comparison between magnifying endoscopy and histological, culture and urease test findings from the gastric mucosa of the corpus. Endoscopy 34(5): 376-381.
- Saka A, Yagi K, Nimura S (2015) OLGA- and OLGIM- based staging of gastritis using narrow-band imaging magnifying endoscopy. Dig Endosc 27(7): 734-741.
- Doyama H, Yoshida N, Tsuyama S, Ota R, Takeda Y, et al. (2015) The white global appearance (WGA): a novel marker for a correct diagnosis of early gastric cancer by magnifying endoscopy with narrow-band imaging (M-NBI). Endosc Int Open 3(2): E120-124.
- Correa P (1988) A human model of gastric carcinogenesis. Cancer Res 48(13): 3554-3560.
- Filipe MI, Muñoz N, Matko I, Kato I, Pompe Kirn V, et al. (1994) Intestinal metaplasia types and the risk of gastric cancer: a cohort study in Slovenia. Int J Cancer 57(3): 324-329.
- Moribata K, Iguchi JK, Nakachi K, Maeda Y, Shingaki N, et al. (2015) Endoscopic features associated with development of metachronous gastric cancer in patients who underwent endoscopic resection followed by Helicobacter pylori eradication. Dig Endosc 28: 434-442.
- Goldenring JR, Nam KT, Wang TC, Mills JC, Wright NA (2010) Spasmolytic polypeptide-expressing metaplasia and intestinal metaplasia: time for reevaluation of metaplasia and the origins of gastric cancer. Gastroenterology 138(7): 2207-2210.
- Weis VG, Goldenring JR (2009) Current understanding of SPEM and its standing in the preneoplastic process. Gastric Cancer 12(4): 189-197.
- Yoshizawa N, Takenaka Y, Yamaguchi H, Tetsuya T, Tanaka H, et al. (2007) Emergence of spasmolytic polypeptide-expressing metaplasia in Mongolian gerbils infected with Helicobacter pylori. Lab Invest 87(12):1265-1276.
- Li Q, Karam SM, Gordon JI (1996) Diphtheria toxin-mediated ablation of parietal cells in the stomach of transgenic mice. J Biol Chem 271(7): 3671-3676.
- Goldenring JR1, Ray GS, Coffey RJ, Meunier PC, Haley PJ, et al. (2000) Reversible drug-induced oxiyntic atrophy in rats. Gastroenterology 118(6):1080-1093.






























