Giant Presacral Schwannoma Presenting With Acute Urinary Retention: A Case Report
Abdul Rasak1*, Ashok Kumar1 and Mohammad Azfar2
1Department of General Surgery, LLH Hospital Musaffah, VPS Healthcare, UAE
2Department of General Surgery Al Bustan Speciality Hospital, UAE
Submission: February 13, 2017; Published: February 20, 2017
*Corresponding author: Abdul Rasak, Department of General Surgery, LLH Hospital Musaffah, VPS Healthcare, P O Box 92313, Musaffah, Abu Dhabi, UAE, Tel:+97125557711; Email: dr.abdulrasak@llhmusaffah.ae
How to cite this article: Abdul R, Ashok K, Mohammad A. Giant Presacral Schwannoma Presenting With Acute Urinary Retention: A Case Report. Open Access J Surg. 2017; 2(3): 555586.DOI: 10.19080/OAJS.2017.02.555586
Abstract
Schwannomas are rare tumours originating from the Schwann sheath of peripheral and cranial nerves. They are usually benign in nature and most commonly the origin is from peripheral nerves. Their occurrence rare in the pelvis or retro-peritoneum.We report a case of46-year old male with a giant pelvic retroperitoneal Schwannoma.
Keywords: Pelvis; Retro peritoneum; Schwannoma
Introduction
Schwannoma is an extremely rare tumour that is composed of Schwann cells of the peripheral nerve sheath, predominantly in the head and neck regions or flexor surfaces of the extremities. Most Schwannoma are benign tumour, although malignant cases are known to occur, especially when there is association of Von Recklinghausen’s disease which occurs in 5-18% of all Schwannomas [1-3] Involvement of other sites like testes, penis, spermatic cord and tunica vaginalis has been previously reported [4,5] Retroperitoneal Schwannoma are usually larger than those at other sites and have greater tendency to undergo spontaneous degeneration and haemorrhage. Presenting symptoms are vague and uncharacteristic. We, here in, describe a case of retroperitoneal giant Schwannoma with extensive mucoid degeneration presenting as acute urinary retention and briefly review the existing literature.
Case Report
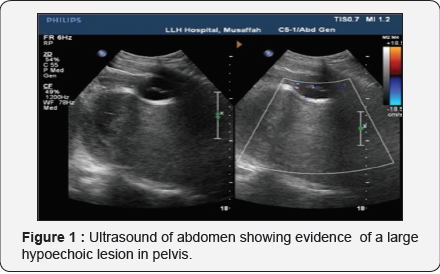
A 46 year old male patient with two months history of lower abdominal pain, urinary disturbance and difficulty in evacuation of bowelspresented with acute urinary retention. He was a known case of Type II diabetes mellitus, on oral hypoglycaemic. He denied any significant past medical or surgical history. His physical and general examination did not reveal any abnormality except acute urinary retention; abdominal examination after urinary catheterization did not reveal any palpable mass. Digital rectal examination revealed fullness of posterior rectal wall with a mass effect. His laboratory investigations were withinnormal limits. Ultrasound of abdomen showed evidence of a large hypoechoic lesion in pelvis posterior to urinary bladder measuring approximately 15 x 10 x 13 cm (Figure 1).
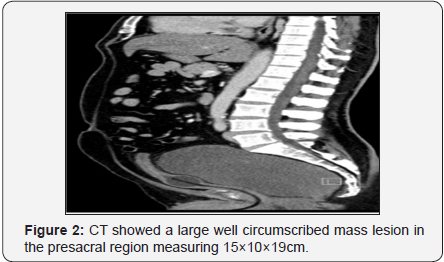
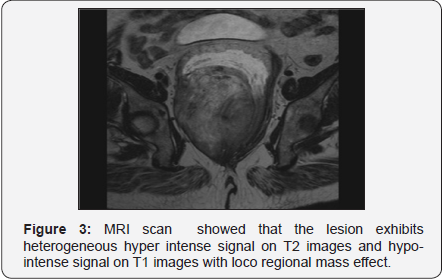
Contrast enhanced CT showed a large well circumscribed heterogeneous density predominantly iso to hypo dense mass lesion in the pre-sacral region measuring 15×10×19cm. It did not show anyenhancement on post contrast study (Figure 2). It was extending from the level of anal canal on right side and pushing the rectum left anteriorly and urinary bladder and prostate anteriorly causing bladder neck kinking. MRIscan showed that the lesion exhibitsheterogeneoushyper intense signal on T2 images and hypo-intense signal on T1 images with loco regional mass effect (Figure 3).
Exploratory laparotomy was performed with a lower midline incision. A large pre-sacral mass was completely excised which was occupying the entire pelvis,obliterating and shifting the rectum, urinary bladder and prostate,without posterior infiltration to the sacral bone. Subsequent histological examination showed pelvic Schwannoma with extensive mucoid degeneration without any evidence of necrosis, mitotic figures or cellular atypia. Immunobiologicalfindings revealed spindle cells positive for vimentin and S-108, CD-34 positive fibroblasts, the cells are negative for CK, Desmin and CD-68 (Figure 4). On his recent follow up after a year of surgery, hewasasymptomatic. His laboratories were unremarkable. Ultrasound of abdomen and pelvis was alsonormal without any evidence of recurrence.

Discussion
Schwannoma (Neurilemmoma) are nerve sheaths tumours of benign nature. Common sites are head, neck and flexor surfaces of extremities but rareto find in retro peritoneum (incidence of less than 1%of all benign Schwannoma) [3]. They usually affect adult patients aged 20 to 50 years predominantly in males. The rarity [6] of this tumour and lack of clinical manifestations make a pre-surgical diagnosis very difficult. These tumours are slowly growing and clinical signs and symptoms manifest themselves only by compression or infiltration of adjacent structures, detection is often accidental [1].
The differential diagnoses for a retroperitoneal schwannoma include, epithelial cyst, abscess, plexiform malignant peripheral nerve sheath tumour (MPNST), sacral meningioma, ependymoma, chordoma, chondrosarcoma, giant cell tumour, aneurysmal bony cyst, osteoblastoma, sacrococcygealteratoma, lymphoma, and the malignant transformation of a benign tumour. These disease categories can be distinguished from Schwannoma by clinical symptoms, age, the radiologic image, subcutaneous paracentesis, and chromosomal study. Ganglioneuroma is a neurogenic tumour which should be considered in the differential diagnosis,it is more commonly found in the retro peritoneum than schwannoma and has similar findings on CT and MRI [7].
Schwannoma typically appears as a solitary, encapsulated and smooth-surfaced round mass. In large tumours (>8-10 cm), a degenerative pattern is commonly found that identifies the “ancient” variant [4]. Histologically a typical schwannoma is composed of inter mixed Antoni A components (highly cellular) and Antoni B areas (loose microcystic tissue adjacent to Antoni A regions). Schwannomas show uniform and intense staining for S- 100 protein 8 [5,8].
CT and MRI are imaging modalitiesof choice in evaluation of retroperitoneal soft tissue tumours. The MRI characteristics of presacral Schwannomas are homogenous or heterogeneous cystic appearance with well-defined margins and iso/iso intensity, iso/high intensity on T1/T2 images respectively [9]. CT scan accurately detects bony destruction. However preoperative diagnosis of schwannomas is not easy due to difficulty in finding imaging features that differentiates schwannomas from other soft tissue tumours (fibrosarcoma or liposarcoma) and benign forms from malignant [10]. Schwannomas can frequently be misdiagnosed. The radiological imaging is helpful in therapeutic planning, as it gives information about the tumour size, location, and possible invasion of other structures. Fine-needle aspiration biopsy may be useful if Schwann cells are found in the sample, but the tissue specimen collected for diagnosis could be insufficient or misleading because of cellular pleomorphism in degenerated areas.
Abdominal or pelvic schwannomas, tend to have a smooth well defined border, ovoid or spherical shape and location inthe pre-sacral region or lower retro peritoneum at the pelvic brim [10]. Evidence of degeneration was common. The cystic schwannomas tend to be larger, with a mean diameter of 10.5cm. Total tumour excision is the treatment of choice for presacral Schwannoma [4,11], as malignant schwannomas are insensitive to chemotherapy and radiation, resulting in poor prognosis [12]. Generally anterior trans-abdominal or retroperitoneal approach for presacral Schwannoma to gain control of vascular plexus and protection of intrapelvic organs. Some authors believe that complete resection is ideal and sacrificing of vital structures may be necessaryto achieve negative margins [11]. In patients who underwent partial resection, some investigators have even reported recurrence rates of up to 10-20% even in benign circumstances, thus emphasizing the importance of a complete resection [7].
Conclusion
Pre-SacralGiant Schwannoma is a benign encapsulating neoplasm with an overall low incidence. It is extremely slow growing tumour and usually presents late with pressure symptoms like abdominal pain, urinary symptoms or constipation. CT and MRI is the preoperative diagnostic imaging modality in demonstrating tissue heterogeneity and anatomic location of the tumour. Surgery is the treatment of choice for patients as it is associated with functional improvement. Although benign, an incompletely excised lesion is capable of recurrence. Malignant change is exceedingly rare.
Acknowledgement
The authors are highly indebted and thankful to Mr. Mohammed Mudassir Anwar Ali for his secretarial assistance in preparation of this article.
References
- Singh V, Kapoor R (2005) Atypical presentation of benign retroperitoneal schwannoma: Report of three cases with review of literature. Int Urol and Nephrol 37(3): 547-549.
- Parfitt Jr HG, Hamonnd ME, Midletton AW (1982) Perirenal malignant schwannoma: a case report and review of literature. J Urol 128(6): 1299-1301.
- José Cury, Rafael Ferreira Coelho, Miguel Srougi (2007) Clinics. 62(3):359-362.
- Girgin C, Ozkan U, Sezer A, Yan NT (2003) Large pelvic schawannomacausing bilateral hydronephrosis. International Journal of Urology 10(11): 616-618.
- Ng KJ, Sherif A, McClinton S, Ewen SW (1993) Giant ancient schwannoma of the urinary bladder presenting as a pelvic mass. Br J Urol 72(4): 513-514.
- Sharma SK, Koleski FC, Husain AN, Albala DM, Turk TM (2002) Retroperitoneal schwannoma mimicking an adrenal lesion. World J Urol 20(4): 232-233.
- Tortorelli AP, Rosa F, Papa V, Rotondi F, Sanchez AM, et al. (2007) Retroperitoneal schwannomas: diagnostic and therapeutic implications. Tumori 93(3): 312-315.
- Tan G, Vitellas K, Morrison C, Frankel WL (2003) Cystic schwannoma of the pancreas. Ann Diagn Pathol 7(5): 285-291.
- Ferrozzi F, Bova D, Garlaschi G (1995) Pancreatic schwannoma: report of three cases. Clin Radiol 50(7): 492-495.
- Hughes MJ, Thomas JM, Fisher C, Moskovic EC (2005) Imaging features of retroperitoneal and pelvic schwannomas. Clin Radiol 60(8): 886- 893.
- Gu L, Liu W, Xu Q, Wu ZY (2008) Retroperitoneal schwannoma mimicking hepatic tumor. Chin Med J 121(17): 1751-1752.
- Li Q, Gao C, Juzi JT, Hao X (2007) Analysis of 82 cases of retroperitoneal schwannoma. ANZ J Surg 77(4): 237-240.






























