Diagnostic and Therapeutic Management of Brain Tumors of Child in Dakar CHU
Thiongane A1*, Ndongo AA1, Boiro D2, Ba ID1, Thiam AB4 , Basse I5, Kane A1 , Kei'ta Y3, Niang B1, Sow A1, Faye PM1, Ba A1, Fall Al1, Sylla A3, Diouf S1 and Ndiaye O1
1Albert Royer Children's Hospital, Dakar
2Department of Pediatrics, Abass Ndao Hospital, Dakar
3Department of Pediatrics, Le Dantec Hospital, Dakar
4Department of Neurosurgery, CHU Fann, Dakar
5Department of Pediatrics, Children's Hospital of Diamniadio, Dakar
Submission: February 06, 2017; Published: March 06, 2017
*Corresponding author: Aliou Thiongane, Chef de Clinique Assistant, Albert Royer Children’s Hospital, Dakar Fann, BP 25755, Dakar Fann, Dakar, Tel: 00221770469488; Email: draliou@gmail.com
How to cite this article: Thiongane A, Ndongo A, Boiro D, Ba I, Thiam A et.al. Diagnostic and Therapeutic Management of Brain Tumors of Child in Dakar CHU. Open Access J Neurol Neurosurg. 2017; 2(5): 555596. DOI: 10.19080/OAJNN.2017.02.555596
Abstract
Introduction: Brain tumors constitute a set of intracranial neoplasms. Their symptomatology associates an intracranial hypertension syndrome (HTIC) and focal neurological syndrome. The objective of our work was to study diagnostic and therapeutic management of brain tumors in children hospitalized at the National Hospital for Children Albert Royer (CHNEAR) in Dakar.
Materials and methods: This was a retrospective study of brain tumors (1st January 2005 to 31st December 2014). Data were collected from patients and hospital records.
Results: Of the 30 patients with brain tumors, only 16 cases were included in our study. The incidence was 0.07%, the age ranged from 3 years to 14 years with an average age of 7.6 ± 3.7 years. The majority of children were under 10 years of age in 75% of the cases. The sex ratio is 2.2 (68% boys and 32% girls). All children were presented with headache, vomiting in 56.3% of cases and visual impairment in 37.5% of cases. Other clinical signs are disorders of alertness, amblyopia and convulsions. Neurological examination found papillary edema in 4 patients, hypertonia in 38%, pyramidal syndrome in 31% of cases, cerebellar syndrome in 37.5% of cases, and meningeal syndrome in 25% of cases. There were 69% of infra tentorial location and 31% in the fourth ventricle. The histological types suspected on cerebral tomodensitometry are ependymoma (18.75%), medulloblastoma (12.5%), astrocytoma (12.5%), Glioblastoma (12.5%) and craniopharyngioma (6.25%). Some patients required preoperative medical treatment (analgesic and neuro-resuscitation). The surgical treatment consisted of a ventriculo-peritoneal derivation in 4 cases, a tumoral excision in 2 cases. Mortality was high in 10 cases (62.5%).
Conclusion: Cerebral tumors of the child are relatively frequent. Mortality however remains high.
Keywords: Child; Brain tumor; Neuro-resuscitation; Ventriculo-peritoneal derivation
Introduction
Brain tumors constitute a set of intracranial neoplasms with an intra- or extra-axial origin [1]. They are the leading cause of cancer deaths [2] in children. Worldwide, their incidence is estimated at 2.5 cases / 100 000 inhabitants / year [3,4]. In developed countries, they are the second leading cause of cancer after leukemia [1, 3]. In sub-Saharan Africa, their incidence remains unknown, particularly in Senegal, where few studies have been carried out. They can be seen at any age with prevalence between 4 and 8 years [5] and represent 16 to 25% of tumors before 16 years. They are the most frequent pediatric solid tumors [6-8]. The symptomatology is non-specific characterized by the association of an intracranial hypertension syndrome and a focal syndrome. Brain computed tomography and nuclear magnetic resonance imaging are essential for the confirmation of topographic diagnosis [9]. Confirmation of the histology of the tumor is obtained by antomo-pathological examination. In developing countries, especially Senegal, the problem is two-fold, diagnostic and therapeutic [6,10]. The objective of our work was to study diagnostic and therapeutic management of brain tumors in children hospitalized at the National Hospital for Children Albert Royer (CHNEAR) in Dakar.
Materials and Methods
This was a retrospective study on brain tumors in children hospitalized from 1 January 2005 to 31 December 2014; 10 years. All children aged 0 to 15 admitted for brain tumors were included in the study. The diagnosis was evoked on the clinical aspects and confirmed by CT scans. We excluded all suspected cases of brain tumors not confirmed by CT and all unusable or incomplete records. The data was entered and analyzed using the Epi Info software version 3.3.2.
Results
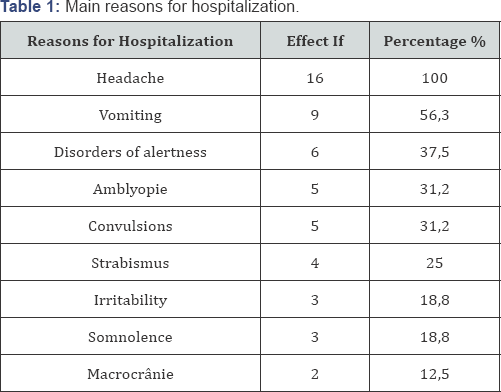
During the study period from 1 January 2005 to 31 December 2014, 44,988 children aged 0-15 years were hospitalized. Of these, 30 (0.07%) children had a cerebral tumor. Of the 30 patients, only 16 cases were included in our study. The 14 excluded files included 10 children lost to follow-up and 4 non- exploitable cases. The mean age of the patients was 7.6 ± 3.7 years with extremes of 3 to 14 years. The age groups of [0-5 years] and [6-10 years] were predominant with 37.5% whereas the age group [11-15 years] represented only 25%. The majority of patients were boys (68%) versus 5 girls (31.2%). The sex ratio was 2:2. The majority of patients came from urban areas in 62.5% of cases. Headache was the most common reason for consultation in all patients. Other symptoms include vomiting, alertness, amblyopia, and convulsions (Table 1). Neurological signs are represented by disorders of consciousness, motor deficits, sensory, hypertonia, respectively in 19%, 31%, 6%, 38%. The rest of the neurological examination showed pyramid syndrome, cerebellar syndrome and meningeal syndrome in (31%), (37.5%), (25%) cases. A child came blind with a torticollis.
Computerized tomography (CT) was performed in all patients and confirmed diagnosis of brain tumor, topography and suspects its histological type. Sub-tentorial localization predominated with 11 cases (68.75%), including 5 cases in the 4th ventricle. The sampling location represents only 31.25%. The diagnosis of ependymoma in three cases, medulloblastoma in two cases, astrocytoma in two cases, glioblastoma in two cases, and craniopharyngioma in one case, were diagnosed histologically. According to sex, there were 7 boys with two medulloblastomas, two glioblastoma, one ependymoma, one astrocytoma and one craniopharyngioma. Three girls had two ependymomas and one astrocytoma. According to the age of the children the 3 ependymomas were found in the age groups (0-5 years), (6-10 years) and (11-15 years), the two astrocytomas in the age groups of both (0-5 years) and (11-15 years), both medulloblastoma and craniopharyngioma in the age group (610 years), the two glioblastomas in the age group (11-15 years).
Pathological examination performed in six children was concluded that in 3 patients, there are 2 medulloblastomas and 1 craniopharyngioma. Patients were treated with anti-convulsant and anti-oedematous drugs in 31% and 63% of cases respectively. Half of the patients were under antibiotics. All patients had analgesic treatment. Corticosteroids were prescribed in 47% of patients. Three patients were put under oxygen therapy, and one patient on a ventilator.Surgical treatment consisted of biopsy resection in one case, total resection in another case. Four patients underwent ventriculo-peritoneal diversion, one with external drainage.
Of the 16 cases included in our series, the progression was favorable in 2 patients (12.5%). We found complications in 14 patients (87.5%). These complications were mainly hydrocephalus in 11 cases, nosocomial infection in 8 cases, metabolic complications in 3 cases and hemorrhagic in 1 case. Four children were lost to follow-up and ten were deceased (62.5%).
Discussion
The incidence was low in our study (0.07%) over the 10 years of study. In Europe, the incidence of brain tumors was lower in the order of 0.003% but with an average increase of 1.7% per year between 1978 and 1997, partially explained by improved diagnostic capabilities without any variation in risk factors being excluded [11]. Nevertheless, a study carried out in Cameroon on central nervous system tumors showed that the pediatric population represented 15% of the population [12,13].
The average age was 7.6 years (3 and 14 years). In Ivory Coast Broalet had recovered an average age close to our age of 8 years [1]. The age groups (0-5 years) and (6-10 years) were predominant 37.5%. The majority of patients had an age less than or equal to 10 years in 75% of the cases. This is comparable to the literature in which the age of the majority of patients was between 4 and 11 years [4]. Elie in Cameroon found a majority in the age group 8 and 13 [6].The male was predominant with 68.8% of cases, the sex ratio was 2.2. Delhemmes reported a male predominance [14]. On the other hand, Yaounde Elie had regained a female predominance with a sex ratio of 0.9 [6].
Intracranial Hypertension Syndrome (HTIC) was found in all patients. In the literature, these results were superimposable [14-17]. It consisted mainly of constant headaches (100%), vomiting (56.3%) and visual disturbances (37.5%). Hamza had recorded 93% of cases of headache and 66.6% of vomiting [10]. Elie had found super imposable results with a frequency of 85% for headache and 45% for vomiting [6]. Lower rates of headache were noted by Wilne 56% [18], Broallet 50.87% of cases [1]. Other clinical signs were tone disorders (75%), amblyopia (31.2%), strabismus (25%), somnolence, irritability and macrocrania (18.8%), respectively. General condition was good in five patients (31%), poor in 11 patients (69%). The majority of patients were hospitalized at an advanced stage of the disease, one with a coma. Infectious syndrome was found in 8 patients (50%).
Six patients (37.5%) had cerebellar syndrome. Elie had found the same frequency in his study [6]. Higher frequencies were found by Boujlal and Kanaan with 51% and 65%, respectively [18,19]. On the other hand Broalet had found a lower frequency with 26% [1]. We found a stiff neck in 1 patient as Hamza in his series [10] while Kanaan [19] had reported more cases. It is a highly evocative sign of posterior fossa tumor. We noted 5 children (31%) with pyramid syndrome. In the literature lower frequencies were reported, Wilne and Hamza noted 27% [20,10], Boujlal 22% [18]. Twenty five per cent of children presented with meningeal syndrome same as Hamza who had found 26.7% of the cases [10]. Boujlal, in his series, had not found any case of meningeal syndrome [18].
The Brain scans (CT) have revolutionized diagnostic and therapeutic management of brain tumors. All our patients had a cerebral computed tomography (CT) scan despite the high cost and unavailability in all hospital facilities. However, although it is non-invasive, it is not an innocuous examination indeed; it has a strong irradiation power in contrast to magnetic resonance imaging (MRI). Cerebral tumors of the child are frequent at the sub-tentorial level (69%). Elie in Cameroon had recovered 55%, [6] Hamza in Senegal had reported 53% [10]. On the other hand, some authors had noted a predominance at the supranational level. Broalet in Côte d'Ivoire found 54% [1] as did Wong.
The CT scan allows in most cases a histological diagnosis of presumption. The results of CT scans in various intracranial tumors were strongly correlated with histopathological abnormalities [21-23]. In our study, the histological type was specified on CT scans in 10 patients. These were 3 ependymomas, 2 medulloblastomas, 2 astrocytomas, 2 glioblastomas and 1 craniopharyngioma. Kamaan found 70% of the cases [18], Hamza [10] and Behat [24] found 50% of the cases, Elie 32% [1].
The majority of our patients received anti-edematous treatment with corticosteroids (47% of cases). The same treatment was used by Kanaan [18,19] in 90% of the cases. Hamza [10] had 30% of patients with corticosteroids and 53.3% with anti-edematous patients. Anti-comitial treatment was administered in 31% of cases (phenobarbital, diazepam). Analgesics were prescribed in all patients. Three patients were on oxygen and a ventilator.Six patients were operated on 30% of cases including total excision and partial excision. Four ventriculo-peritoneal derivations.
The evolution and prognosis of pediatric brain tumors were very dark with heavy mortality 62.5% of cases including six children even before surgical management. This high mortality could be explained by a delay in diagnostic and therapeutic management. Broalet had regained a favorable rate of change of 15% [1]. Higher rates were reported in the literature, 26% for BEHAT [24], 30% for Hamza and 48% for Kanaan [18].
Conclusion
Cerebral tumors of the child are relatively frequent. The diagnosis of brain tumors is based primarily on histological analysis. Management is multidisciplinary.
References
- Broalet E, Haidara A, Zunon-Kipre Y, D N'dri Oka, H N'Da, et al. (2007) Approche diagnostique des tumeurs cérébrales chez l'enfant. Afr J Neurological sciences 26(2): 27-38.
- Reddy AT (2001) Advances in biology and treatment of childhood brain tumors. Curr Neurol Neurosci Rep 1(2): 137-143.
- Philippon J (2004) Tumeurs cérébrales. Paris: Masson. Plantaz D, Tumeur de la fosse cérébrale postérieure de l'enfant. Corpus Médical, Faculté de Médecine de Grenoble, pp. 218.
- Lachassinne E, Durquet-Perelman C (1996) La Pédiatrie au quotidien. Paris : Maloine (2nd edn), Paris, France.
- Elie M, Christian L S, Vincent DPB (2011) Aspects cliniques, scanographiques et histologiques des tumeurs cérébrales de l'enfant à Yaoundé, Caméroun. Schweizer Archiv Für Neurologie Und Psychiatrie 162(7): 284-287.
- M haded H (1996) Le cancer chez l'enfant, Sanofi-Espoir.
- Borha A (1998) Tumeurs cérébrales et médullaires chez les enfants. Service de Neurochirurgie CHU de Caen, Dhakar fann, Dhakar.
- Fattet S, Rillet B, Vernet O (2007) Tumeurs cérébrales de l'enfant : diagnostic et traitement. Rev Med Suisse 3(109): 1131-1138.
- Hamza El Hamzaoui (2012) Tumeurs cerebrales de l'enfant. A Propos de 30 cas. Thése Med. Dakar.
- Peris-bonet R, Martinez-Garcia C, Lacour B et al. (2006) (Childhood central system tumours-incidence and survival in Europe: report from Automated Chilhood Cancer Information System Project. Eur J Cancer 42(13): 2064-2080.
- E yenga vc, Eloundou Ngah J, Atangana R (2008) Les tumeurs du système nerveux central au Cameroun: Histopathologie, démographie. Cahiers Santé 18(1): 39-42.
- Zerah M, Rougault T (2004) Tumeurs cérébrales de l'enfant dans: Tumeurs cérébrales : Du diagnostic au traitement. Paris : Masson, pp. 233-252.
- Delhemmes P, Hladky JP (1995) Tumeurs sus tentorielles de l'enfant. In: Decq P, Kéravel Y, Ellipses AUPELF/UREF. Neurochirurgie, pp. 230238.
- Girard PL, Dumas M, Collomb H (1973) Processus expansifs intracrâniens chez l'enfant au Sénégal. Afr J Med Sci 4(2): 161-169.
- Pollack IF, Finkelstein SD, Burnham J (2001) Age and TP53 mutation frequency in childhood malignant gliomas: results in a multi- institutional cohort. Cancer Res 61(20): 7404-7407.
- Pollack IF, Hamilton RL, James CD (2006) Rarity of PTEN deletions and EGFR amplification in malignant gliomas of childhood: results from the Children's Cancer Group 945 cohort. J Neurosurg 105(5): 418-424.
- Boujlal A (1994) Tumeurs cérébrales de l'enfant, à propos de 64 cas. Thèse Med, Casablanca.
- Kanaan A Tumeurs (2005) cérébrales de l'enfant à propos de 240 cas. Thèse Med,Casablanca.
- Wilne SH, Ferris RC, Nathwani A (2006) The presenting features of brain tumors: a review of 200 cases. Arch Dis Child 91(6): 502-506.
- Haqet MZ, Karim ME, Al-Azad, Rôle de la tomodensitométrie au Bangladesh. PMID : 21548545.
- Lacour B, Desandes E, Mallol N (2005) Le registre lorrain des cancers de l'enfant: incidence, survie 1983-1999. Arch Pediatr 12(11): 15771586.
- Chiu JK, Woo SY, Ater J (1992) Intracranial ependymoma in children: analysis of prognostic factors. J Neurooncol 13(3): 283-290.
- Behat M (2009) Tumeurs cérébrales de l'enfant à propos de 34 cas. Thèse Med, Dakar.
- Schweigsguth O (1991) Les tumeurs cérébrales de l'enfant: l'expérience passée. Entretien avec Odile Schweisguth par T. Philip. Pediatr 46(1):121-124.






























