Intracranial Subdural Haemophilic Pseudotumor: Case Report
Micaela Uberti1*, Matías Burroni1, Lucas Capo1, Alejandra I Baques2, Patricia R Do scimento2, Silvio Grisendi3, María S Serrano3 and Javier E Salazar1
1Department of Neurosurgery, Milstein Hospital, Argentina
2Department of Haemophilia, Milstein Hospital, Argentina
3Department of Pathology, Milstein Hospital, Argentina
Submission: November 24, 2016; Published: January 31, 2017
*Corresponding author: Micaela Uberti, Department of Neurosurgery, Milstein Hospital, Argentina, 104-108 Curtain Road, Flat 12. EC2A 3AH, London, UK, Tel:(0044)7538488570, Email:micauberti@gmail.com
How to cite this article: Micaela U, Matías B, Lucas C, Alejandra I B, Patricia R D s, et al. Intracranial Subdural Haemophilic Pseudotumor: Case Report. 002 Open Access J Neurol Neurosurg. 2017; 2(3): 555590. DOI: 10.19080/OAJNN.2017.02.555590
Abstract
Hemophilia is an autosomal recessive disease linked to the X chromosome. It runs with Factor VIII deficiency (Type A, more frequent), and Factor IX deficiency (Type B). A hemophilic pseudotumor is an infrequent complication of this disease, mainly in severe cases. Starker was the first to report a case in a 14 year old boy, in 1918. The estimated incidence is of 1-2% in severe hemophiliacs, although some pseudotumors have been reported in moderate cases. This kind of tumor is generally seen in long bones such as femur and humerus, pelvis, and small bones of hands and feet. Cases have also been reported in the cranium, orbit and facial bones, and only one previously similar to this case report. We present a case of an intracranial subdural hemophilic pseudo tumor in a patient with type A severe hemophilia.
Keywords: Pseudotumor; Hemophilia; Intracranial; Subdural
Introduction
Hemophilia is an autosomal recessive disease linked to the X chromosome. Type A is the most frequent one and is caused by Factor VIII deficiency [1,2]. Type B has Factor IX deficiency, and is less common. Hemophilic pseudotumors are an infrequent complication of this disease. Starker was the first to report a case in a 14 year old boy, in 1918 [3]. In 1965, Fernandez de Valderrama and Matthews described the condition as a “chronic cystic inflammation of the muscle, caused by recurrent bleedings, and associated with radiological evidence of compromised bone structure” [4,5]. Based on the scarce published information, the estimated incidence is of 1-2% in severe hemophiliacs, although some pseudotumors have been reported in moderate cases [3,4,6-9]. This kind of tumor can be more frequently found in long bones such as femur and humerus, pelvis, and small bones of hands and feet [3,4]. Cases have been reported in the cranium, orbit and facial bones, but always characteristically included bone structures [10,11]. There is only one intracranial case reported in 2009. We present a case of an intracranial subdural hemophilic pseudotumor in a patient with severe factor VIII deficiency.
Case Report
A 45 year old male with severe Factor VIII deficiency was referred from another institution with weakness in the right arm that had progressed for 2 months, and had worsened the previous week the hospital admission. He had also an urinary infection at the time of admission. His past medical history included Hepatitis C, epilepsy, and knee replacement secondary to hemarthrosis in 2013. He had also suffered a traumatic brain injury when he was 4 years old, and later on was diagnosed with intracranial hemophilic pseudotumor by an hematology service of another institution. No surgical treatment was done at this stage, and the patient was followed with serial CT scans along the years. 40 years ago in Argentina there wasn’t a good access to the treatment known as anti-haemophilic prophylaxis, which basically consists of intravenous Factor VIII three times a week, to prevent spontaneous bleeding. The only available treatment was poor quality Factor VIII that was administrated only in bleeding episodes. However, the patient did eventually gain full access to prophylactic treatment, but he did not self-administer factors on a regular basis, as he was taught to do by his former doctors. He was thus always treated on demand, and factors were administered only on bleeding episodes.The haemophilic pseudotumor was probably a consequence of poor treatment and low adherence to it.
Examination
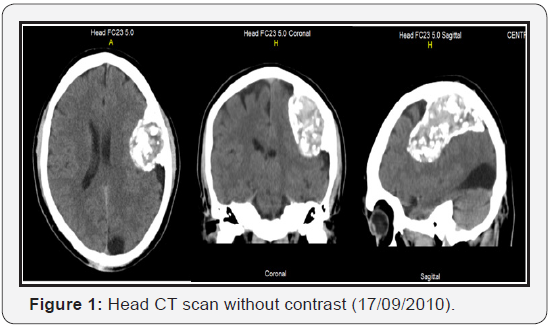
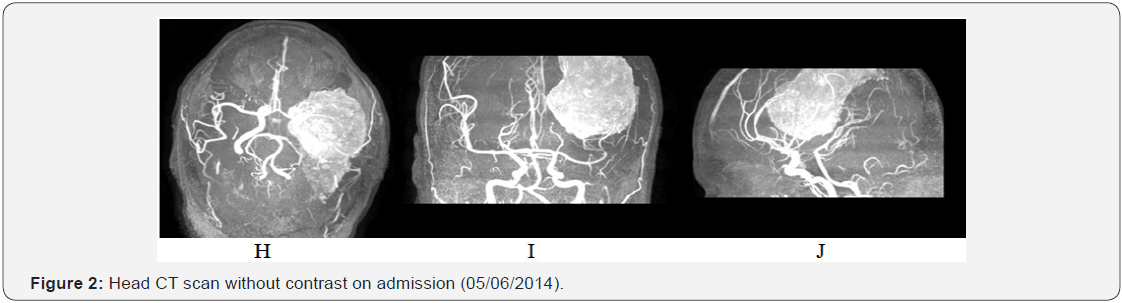
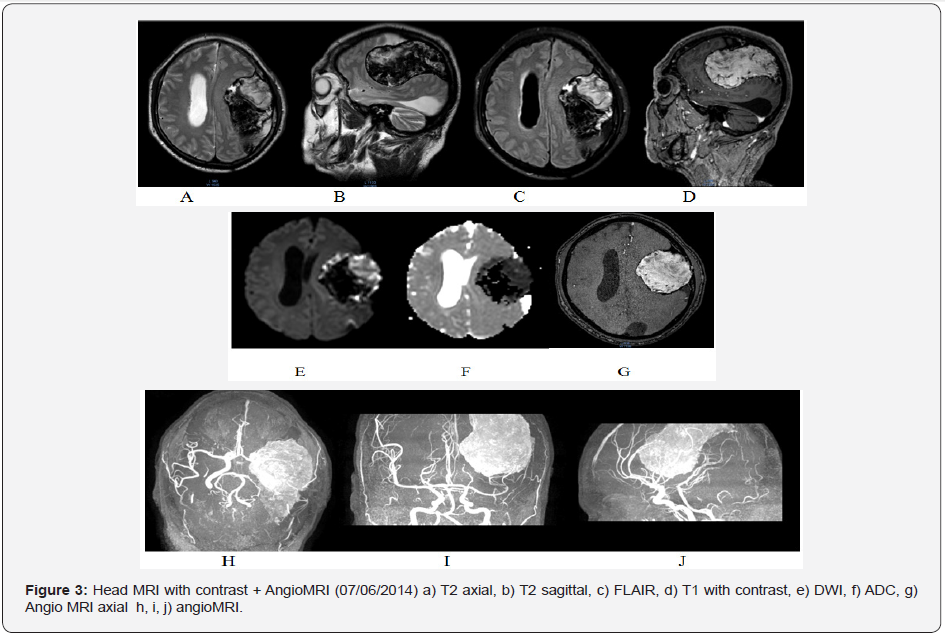
On admission, the patient presented with right homonymous hemianopsia, mild right hemiparesia, generalized hyperreflexia and hypoesthesia in right arm and leg. Hebrought with him a CT head scan from September of 2010 which showed an heterogeneous left fronto-parietal lesion, with calcification areas, in contact with the meninges, and slight mass effect over the parenchyma, with no surrounding edema (Figure 1). A new CT head scan showed a largerheterogeneous fronto-parietal mass, with calcification areas and severe mass effect over the parenchyma, with no surrounding edema (Figure 2). It was decided to do an MRI with contrast to further characterise the lesion, and anMRA, to rule out a vascular malformation, given the repetitive bleeding episodes (Figure 3). The patient was treatedwith ceftriaxone for the urinary infection, and he was also given an intravenous bolus of 4000 IU of Factor VIII.
Operation
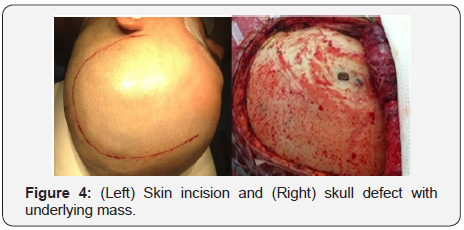
Given that the patient was symptomatic, we decided for surgical resection of the lesion. He was first treated with 3000 IU of Factor VIII every day until the surgery. The patient was given 9000 IU of Factor VIII intraoperatively (100IU/kg). A left frontoparietal incision was performed. When the bone was reached, there was a visible defect on it, which suggested that the lesion had eroded through (Figure 4). After the craniotomy was done, a large mass resembling an organized clot was encountered, which was beneath the dura mater, had several calcified areas, and was directly contacting the cerebral parenchyma, but not infiltrating it (Figure 5). The lesion was fully extracted (Figure 6) and was sent for histology. This showed signs linked to an encapsulated chronic hematoma (Figure 7).
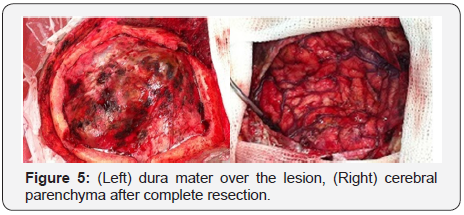
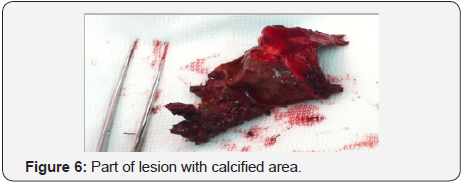
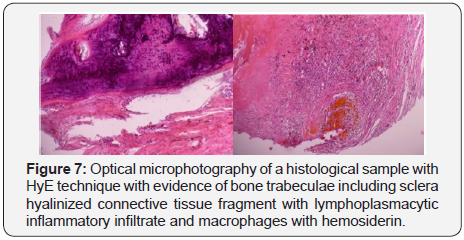
Postoperative course
The patient remained with intraoperative doses of Factor VIII for four more days, and then this was weaned to three weekly prophylaxis of 2000 IU of IV Factor VIII, which is his present treatment. Ten days after surgery the wound began to leak CSF, but resolved with suturing, antibiotics, and acetazolamide. A CT scan at that point showed good evacuation of the pseudotumor, with minimal postoperative effusion. He was discharged approximately 2 weeks after the surgery, CT and MRI control images done two months after the operation showed no recurrence of the lesion (Figure 8&9). The patient had a favorable evolution and recovered total motor function after one week (Figure 10). Afterwards the patient was followed with head CT and head MRI scans at 2, 6 and 12 mounths that showed no recurrence of the lesion.
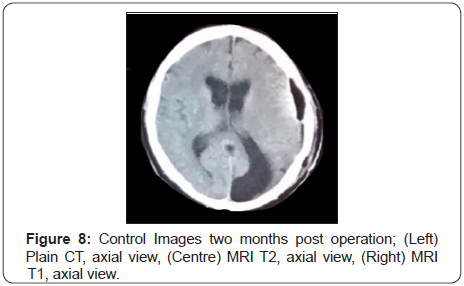
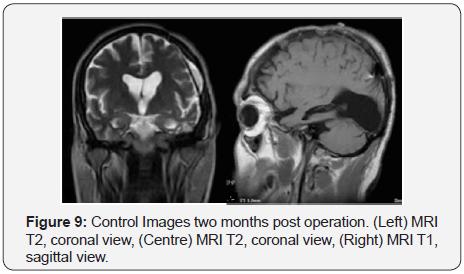

Discussion
The natural history of this disease is of a slow growing clot that may or may not be product of a banal trauma [10], perpetuated by small internal haemorrhages that gradually increase its size [3,7]. Although they are avascular, they develop a capsule that is well irrigated. This rich vascular supply causes the repeated haemorrhages, which result in the expansion of the mass [12]. These lesions can compress and erode adjacent structures like bones and neurovascular structures, causing pathological fractures, neurological symptoms, skin necrosis and infections [11,12].
Haemophilia can be classified based on the quantity of factor present in blood, as mild (coagulation factor more than 5% of normal value), moderate (1%-5% of normal value), or severe (less than 1% of normal value) [13]. Apart from ours, fourteen cases have been reported of hemophilic pseudotumors in the cranium (Table 1). Seven of those cases occurred in moderate hemophiliacs and five in severe ones (two were not specified). This marks a difference with the rest of the areas in which this disease is generally seen (for example long bones), as the latter present themselves mainly in severe cases. Almost all cranial cases affected bone structures, with extension to the epidural space, but never passed, o were born under, the dura mater. Only one case in 2009 was subdural. Differential diagnoses include Ewing sarcoma, giant-cell tumor, condrosarcoma, osteomyelitis, tuberculosis and, in this case, meningioma, plasmocitoma, and epidural or subdural calcified hematoma [3,5,8,14].
Most published cases had a history of trauma. The interval from the traumatic incident and symptom presentation and diagnosis can vary between months and years [5]. This is why it is of the utmost importance to keep a thorough track of traumatic episodes, so as to alert the physician of possible pseudotumors in the future.
Simple x-rays and CT scans are useful to evaluate bone extension and calcifications, given that these cases generally take years to develop [6]. CT with contrast might show a capsule if present. However, the imaging of choice is MRI [3,9]. Chronic haemorrhage is hypointense in T1 and T2 because of the hemosiderine; and the capsule´s hypointensity is better visualized in T2 than T1, because of fibrous organisation. The heterogeneous signal of the haemophilic pseudotumor in both CT and MRI is caused by the different evolution of blood products [8,9,14].
Several possible treatments have been described, but none have proved as effective as surgery. Small and asymptomatic pseudotumors could be managed conservatively with coagulation factors and immobilisation [4,6]. The possibility of aspirating via puncture was mentioned in other cases (not in the cranium), but that predisposed to recurrence, fistulas and infections [3,4,7,10,15,16]. Radiation treatment has been proposed as a treatment but its mechanism of action is unknown [3,9,15] and at least in cranial cases it would represent unnecessary brain exposure to radiation. Nevertheless, this method could be useful in cases where there is a Factor VIII inhibitor, in which factor replacement and thus surgery are not an option [3,6,16].
There are no cranial cases that have been treated with radiotherapy. Lastly, embolization could be used given that the capsule is vascularised, generally by more than one artery. It has a temporary effect, due to arterial recanalisation after some weeks. It could be a helpful pre-operative tool, and has been tried in pseudotumors outside the cranium [6,11,12]. Surgery is used in those cases that do not respond to conservative treatment, in symptomatic patients, evidence of neurovascular compression, large masses, or to confirm the diagnosis [3,9,13]. With all this said, because of the infrequent nature of this pathology, there are no treatment protocols, and management is mainly based on the individual case and previous reports. Correct pre- and postoperative factor replacement by hematologists is a key factor, given the increased risk of postoperative haemorrhages and infections in these patients [17-19].
Conclusion
The life expectancy and treatment quality of haemophilic patients has increased with the development of factor replacement treatment, and so pseudotumors should likely become less frequent. Still, it is important to know of their existence, mainly to implement the corresponding prevention techniques. It is precisely the lack of medical awareness that permits growth of these tumours until they cause symptoms, some of which may be irreversible. Surgery has proved to be a good choice of treatment, without recurrence. We nonetheless believe that the key to tackling this high morbidity complication is close cooperation with haematology team, with correct followup and control of the patient and his disease.
References
- Neha Vapiwala, John P Updated by J Taylor Whaley (2011) Medulloblastoma: Overview.
- Tobey MacDonald, Roger J Packer, Kathleen M Sakamoto, Mary L Windle, Steven K Bergstorm, et al. (2012) Pediatric Medulloblastoma. Medscape Reference, Drug Diseases and Procedures.
- Bloom HJ, Glees J, Bell J, Ashley SE, Gorman C, et al. (1990) The Treatment and long term prognosis of children with intracranial tumors: a study of 610 cases.1950-1981. Intl J radiate Oncol Biol Phys. 8(4): 723-745.
- Rutka JT (1997) Medulloblastoma. Clin Neurosurg 44: 571-585.
- David KM, Casey AT, Hayward RD, Harkness WF, Phipps K, et al. (1997) Medulloblastoma; is the-5 year survival rate improving ? A review of 80 cases from a single institution. J Neurosurg 86(1): 13-21.
- Zee CS, Segall HD, Nelson M (1993) Infratentorial Tumours in Childern. Neuro imaging Clinics of North Am 3(4): 705-714.
- Menon G, Nair S, Muthurethinam T, Krishna kumar K, battacharya RN (2006) Medulloblastoma in Childern: Prognostic Factors and Predictors of outcome. J Pediatr Neurosci 1(1): 16-20.
- Park TS, Hoffman HJ, Hedrick EB, Humphreys RP, Becker LE (1983) Medulloblastoma: Clinical Presentation and Management. Experience at the hospital for sick children, toronto, 1950-1980. J Neurosurg 58(4): 543-552.
- Yazigi-Rivard L, Masserot C, Lachenaud J, Diebold-Pressac I, Aprahamian A, et al. (2008) [Childhood medulloblastoma]. Arch Pediatr 15(12): 1794-1804.
- John Mealey, Jr MD, Peter V Hall (1977) Medulloblastoma in Childern, Survival and Treatment. Journal of Neurosurgery 46(1): 56-64.
- Packer RJ, Vezina G (2008) Management of and Prognosis with Medulloblastoma: Therapy at a Crossroads. Arch Neurol 65(11): 1419- 1424.
- Harisiadis L, Chang CH (1977) Medulloblastoma in Childern: A correlation between staging and results of treatment. Intl J of Rad Oncl Biol Phys 2(9): 833-841.
- Bloom HJ, Wallace EN, Henk JM (1969) The Treatment and Prognosis of Medulloblastoma in Childern. A Study of 82 Varified Cases. Am J Roentgenol Radium Ther Nucl Med 105(1): 43-62.
- Awasthy BS, Das Gupta C, Patel AK, Julka Pk (1997) Medulloblastoma- A Retrospective Analysis. Indian J Pediatr 64(5): 693-697.
- Jenkin D, Goddard K, Armstrong D, Becker L, Berry M, et al. (1990) Posterior Fossa Medulloblastoma In Childhood:Treatment results and a Proposal for a new staging system. Int J Radiate Oncol Biol Phys 19(2): 265-274.
- Khalil EM (2008) Treatment results of adults and children with Medulloblastoma NCI, Cairo University experience. J Egypt Natl Canc Inst 20(2): 175-186.
- Djamil Fertikh, Michael L Brooks, Chi-Shing Zee, Bernard D Coombs, Douglas Phillips, et al. (2013) Medulloblastoma Imaging. Medscape References, Drug Diseases & Procedures.
- Thapar K, Laws ED (1995) Tumours of central nervous system. In: Clinical Oncology. Am Cancer So, pp. 396-397.
- Prados MD, Wara W, Edwards MS, Aterr J, Rabbit J, et al. (1996) Treatment of high risk medulloblastoma and other primitive neuroectodermal tumors with reduced dose craniospinal radiothtion therapy and multi agent nitrouria based chemotherapy. Pediatr Neurosurg 25(4):174-181.






























