Hypomelanosis of Ito with Partial Motor Seizure and Hemimegaloencephaly: Case Report
Amal Y. Kentab*
Department of Pediatric Neurology Division, King Khalid University Hospital, Saudi Arabia
Submission: November 12, 2016; Published: January 23, 2017
*Corresponding author: Amal Y. Kentab, Assistant Professor & Consultant Pediatric Neurologist, Department of Pediatric, Neurology Division , King Khalid University Hospital , College of Medicine ,King Saud University, Riyadh, Saudi Arabia, Fax: +966(1)469-1512; Email: amkentab@hotmail.com/akentab@ksu.edu.sa
How to cite this article: Amal Y. K. Hypomelanosis of Ito with Partial Motor Seizure and Hemimegaloencephaly: Case Report. Open Access J Neurol Neurosurg. 2017; 2(2): 555585. DOI: 10.19080/OAJNN.2017.02.555585
Abstract
The term hypomelanosis of Ito [HI] is applied to individuals with skin hypopigmentation along the lines of Blaschko. Even though originally described as a purely cutaneous disease, subsequent reports have included a 33% to 94% association with multiple extracutaneous manifestations mostly of the central nervous and musculoskeletal systems leading to frequent characterization as a neurocutaneous disorder. A boy with constellation of multiple congenital anomalies including facial dysmorphism, skin hypopigmentation, musculoskeletal, and nervous system abnormalities in the form of hypotonia and mild mental retardation suggestive of [HI] presented with partial motor seizures and found to have hemimegalencephaly [HME] on MRI of the brain.
Keywords: Hypomelanosis ito (HI); Cortical dysplasia; Neurocutaneous syndrome; Cerebral malformation.
Introduction
Hypomelanosis of I to [HI] or Incontinentia pigmenti achromians [OMIM no. 146150]. Ito first introduced the syndrome 1951 [1]. It is a rare neurocutaneous syndrome that involves mainly skin and nervous system symptoms in 75 % of cases and may be associated with multiple organ systems involvement including the head and face, eyes (microphthalmia, cataracts, optic atrophy, and retinal detachment), teeth, cleft lip and palate, heart (tetralogy of Fallot), kidneys, musculoskeletal (hemihypertrophy), and reproductive systems (precocious puberty) [2-4]. The incidence and prevalence of [HI] has been reported to be1/7540 births and 1/82,000 individuals, respectively [4]. McKusick`s catalogue of inherited diseases lists HI as an autosomal dominant disorder, although evidence for this mode of inheritance, or indeed for any genetic etiology, is inconclusive [2]. Frequency is equal among males and females. It is caused by Nonheritable mutation, and it have been reported frequently in association of various chromosomal abnormalities, including mosaicism for aneuploidy or unblanaced translocations, mosaic trisomy 18, ring chromosome 22, and translocations involving the X chromosome. There is no clear genotype - phenotype correlation [2]. Only a few cases of HI have been reported with partial motor seizures in association with hemimegalencephaly [HME]. In order to highlight on this rare neurocutaneous disorder, this report describes such association in a 10 year old boy with skin hypopigmentation, craniofacial and musculosketetal abnormalities.
Case Report
A 10 -year-old male, left handed, 6th grade student was evaluated in our tertiary care neurology clinic for afebrile complex partial motor seizure with 2nd generalization, started one month prior to presentation. He had frequent episodes of sudden left-sided eye deviation and facial twitching with secondary left-sided unilateral and generalized tonic-clonic seizures. Each episodes last for less than 3 minutes, preceded by dizziness, pain in the right eye with blurred vision and headache, end spontaneously after an episode of vomiting , headache , and postictal sleep without loss of sphincter control . Seizures were controlled with levetiracetam (Keppra). He was a product uneventful pregnancy delivered by spontaneous vaginal delivery at 36 weeks gestational age, readmitted on 2nd day, and operated for intestinal intussusception. Past history included a slower cognitive and language development in comparison to other siblings, skin hypopigmentation noted at 6 months of age, bronchial asthma, abnormal dentation with frequent dental caries, and tonsillectoy-adenectomy operation for frequent tonsillitis.
His parents were consanguineous and there was a history of seizure disorder in two sons of paternal uncle from twin pregnancy. Microophthalmia in two sisters of paternal ante. Reported multiple infantile deaths of both parental, and maternal side with obscured reasons. His mother had cafe`-au lit spot and hypopigmentation on her thighs. On examination, he had macrocephaly, short stature, dysmorphic features in the form of high prominent forehead, low set and posteriorly rotated prominent ears, orbital hypertelorism, epicanthal fold, depressed nasal bridge, anteverted nostrils, high arched palate, tooth spacing with abnormality in size and shape, micrognathia, broad fingers with archanodactyly, mild clinodatyly of 5th finger, broad nails, a gap between big toe and the second one, syndactly between the 2nd and the 3rd toes on the right foot, mild scoliosis (deviation to the left) with prominent lordosis, joint hyperlaxity and bilateral pes plans , with mild hemi hypertrophy of the right side of the body , involving mainly the face and upper extremity.
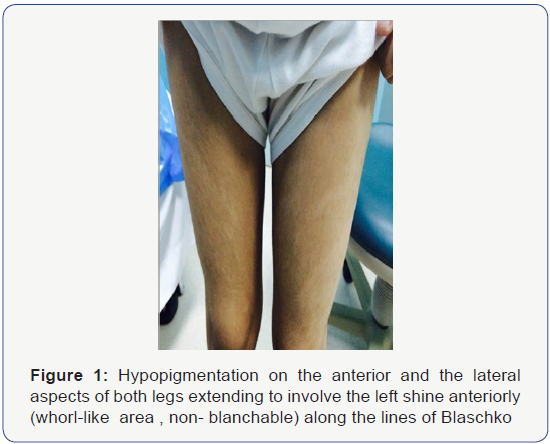
Hypopigmented areas (whorl-like and streaks) noted on the anterior and the lateral aspects of both legs extending to involve the left shine anteriorly and another similar one but with small size seen at the right shoulder (Figure 1). His neurological examination revealed poor short-term memory and cognitive delay, especially in terms of general knowledge, the ability to read and mathematical concepts and mild right hemiparesis. His initial basic laboratory work-up was normal apart from mild anemia, and low vitamin D 62 nmol/l (NR 75-120). Full metabolic screen thyroid function test, full chromosomal analysis, microarray CGH showed and Cardiac evaluation by electrocardiogram (ECG), echocardiogram (Echo) and Abdominal ultrasound were unrevealing. Ophthalmological evaluation showed mild sclerocornea, pigmented iris, and bilateral flat retinal astrocytoma with retinal pigmentary changes. Skeletal survey revealed mild osteoporosis and mildscoliosis.
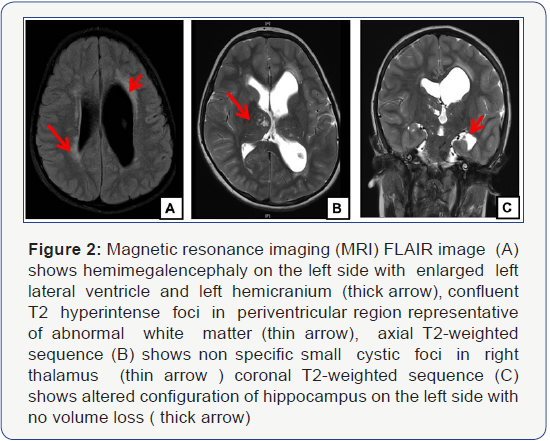
Electroencephalogram (EEG) showed background asymmetry with slow theta wave activity noted on the left hemisphere with occasional sharp waves seen predominately on the left hemisphere. Computed tomographic (CT) scan of the brain showed no space occupying lesion, but left hemimegaloencephaly with dilated left ventricle. Magnetic resonance imaging scan of the brain (MRI) revealed similar findings with small arachnoid cyst at left middle fossa with no evidence of neuronal migration disorders or cortical dysplasia (Figure 2). Magnetic resonance angiography (MRA) was normal with no evidence of vessel stenosis or picture similar to moyamoya disease.
Discussion
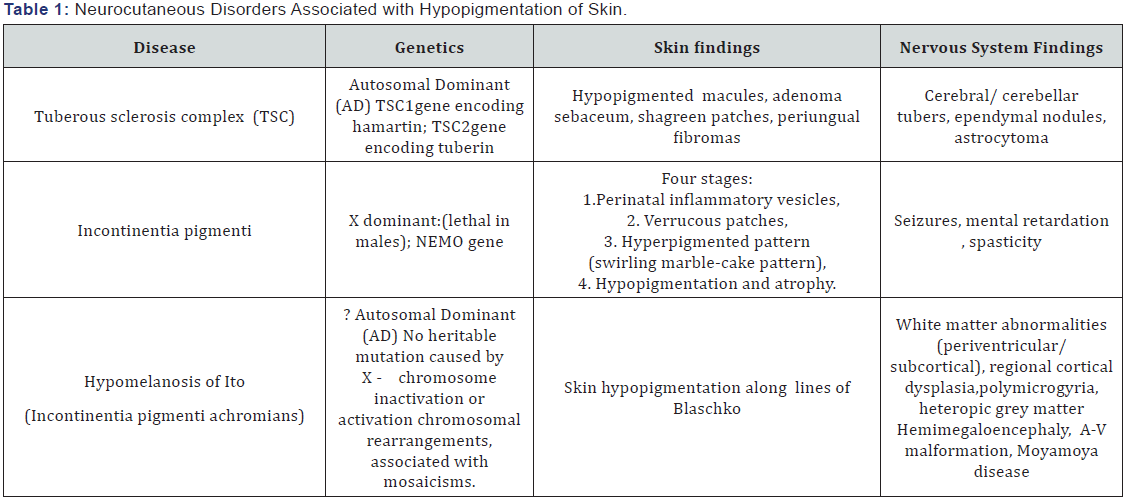
The cutaneous features of HI include multiple hypopigmented streaks or patches that found in 100% of affected individuals and are either present at birth or emerge in infancy. These lesions follow Blaschko lines (skin lines that form specific patterns over the trunk and extremities, such as a V shape over the back and linear lines over the limbs and are best detected under ultraviolet light in light - skinned children. In contrary to incontinentiapigmenti, these lesions, are not preceded by inflammatory or degenerative changes. (Table 1) The extent of the skin lesions do not correlate strongly with neurologic involvement. An important differential diagnosis is Tuberus Sclerosis Complex, where the hypopigmented patch (ash leave spot which is usually oval in shape with regular border) appears during the 1st year of life mainly on trunk or extremities, and as the child approaching puberty other skin manifestations appear like adenoma sebaceum, on the face, shagreen patch on the back and periungual fibroma [3,4].
(Table 1) Neurologic manifestations include intellectual impairment with mild to severe mental deficiency (IQ<70) that is usually seen in 57% while only 20% of patients have an IQ above 85% with reported poor school performance in (40-60%). Seizures that include generalized tonic or tonic-clonic, complex partial, myoclonic seizures or infantile spasm with onset early in the first year of life, with variable response to anticonvulsant drugs . Behavior disorders that include autism, Asperger`s syndrome, self-injurious behavior and severe sleep problems especially in the first 3-5 years of age [3,4]. Macrocephaly or microcephaly may be seen, with the former being more common. Other associated findings include, a non-progressive speech delay, muscular hypotonia or hypertonia, hyperkinesias, nystagmus, ataxia, and neurosensory deafness. MRI in more than half of patients may show either cerebral or cerebellar hypoplasia and various other malformations of cortical development including hemimegalencephaly, lissencephaly, pachygyria, and heterotopia. White matter abnormalities of either cystic like lesions or delayed myelination. Other brain abnormalities include, focal or generalized brain atrophy, basal ganglia lesion, or intracranial vascular abnormalities such as A-V malformation, Moyamoya disease, leptomeningeal angioma [2]. The patient in this report had clinical picture suggestive of HI (skin hypopigmentation, facial dysmorphism, eye and dental abnormalities, joint hypermobility, skeletal abnormalities ie. short stature, scoliosis, osteoporosis, mild learning disability, partial motor seizures), mild right hemiparesis and HME with no other associated neuronal migration disorder on brain MRI which has been previously reported [5-9].
Hemimegalencephaly is a major, but rare congenital hamartomatous malformation of the brain [10], characterized by enlargement of all or parts of a cerebral hemisphere and frequently associated with cortical focal or diffuse neuronal migration defects, such as polymicrogyria, pachygyria, or heterotopias. HEM affects all ethnic groups and both genders equally.
Its etiology remains unknown. It has been suggested that it results from some type of acquired unilateral hemispheric insult in the mid to late second trimester of pregnancy [11] that affect the genetically programmed process that establishes symmetry as well as the development of neuroepithelial lineage and cellular growth occurring at an earlier stage of neuroblast migration [12]. It does not follow a Mendelian pattern of inheritance and usually occurs sporadically. It is widely believed that a single or multiple gene mutations contribute to this process.
It typically presents with a triad of intractable epilepsy, psychomotor delay and hemiparesis. Some patients show entire brain asymmetry, hemifacial hypertrophy, or hemicorporal hypertrophy. Other associated features may include macrocephaly with cranial asymmetry, and behavioral disabilities. Epilepsy is usually of early onset and intractable. Those with later-onset epilepsy are more likely to have mild motor deficit like the patient in this report, or normal motor function. The EEG is abnormal in all cases of HME. In the neonatal period, suppression burst pattern, followed by hypsarrhythmia and later, focal seizure activity may be seen. Functional or anatomical hemispherectomyis recommended for early - onset pharmacoresistant epilepsy as improvement of either the motor function level or intellectual development was seen in most patients post-surgery [13,14].
It is often an isolated disorder, but may be syndromic associated with several diseases or neurocutaneous syndromes, such as epidermal nevus syndrome, tuberous sclerosis complex (TSC), linear sebaceous nevus syndrome, Klippel - Trenaunay syndrome (KTS), Proteus syndrome (PS), hypomelanosis of ito (HI), neurofibromatosis , Sotos syndrome and Alexander [10,15]. It is worthy to mentioned that usually there is no differences in clinical symptoms in regards to the laterality (Right or left) or the type (isolated or syndromic) of hemimegalencephaly [16].
MR Imaging is the investigation of choice for diagnosis, though ultrasound and CT will show the abnormalities. As in our patient, increased size and altered shape of the ventricle is usual. The cortex is broader (dysplastic) than normal, neuroblast migratory anomalies are frequently seen, the most common being heterotopias. [11], as well as white-matter abnormalities (high signal intensity in T2W image) [17]. Since the disease does not follow a Mendelian pattern of inheritance, chances of recurrence are rare and there is usually no family history of other affected individuals. Prenatal diagnosis may be suspected on the basis of fetal ultrasound [18] or MRI (diffusion - weighted images) [19].
Conclusion
Combination of a triad of intractable epilepsy, psychomotor delay and hemiparesis in the presence of macrocephaly and / or skin hypopigmentation should prompt consideration of HEM . MRI is the imaging of choice for diagnosis of HEM. HEM should prompt a search for other syndromic diagnosis such as HI.
Acknowledgment
This work was supported by the College of Medicine Research Center, Deanship of Scientific Research, King Saud University.
References
- Ito M (1952) Studies on melanin XI. Incontinentia pigmentiachromians. A single case of nevus depigmentosus systematic usbilaterlis. Tohoku J Exp Med Suppl 55: 57-104.
- Amal Y Kentab, Hamdy H Hassan, Mudathir HA Hamad, Ahmed Alhumidi (2014) The Neurologic aspects of hypomelanosis of Ito: Case report and review of the literature. Sudan J Paediatr 14(2): 61-70.
- Pscual-Castroviejo I, Roche C, Martinez-Bermejo A, Arcas J, Lopez- Martin V et al. (1998) Hypomelanosis of Ito. A study of 76 infantile cases. Brain Dev 20(1): 36-43.
- Ruggieri M, Pavone L (2000) Hypomelanosis of Ito: Clinicalsyndrome or just phenotype? J Child Neurol 15(10): 635-644.
- Okanari K, Miyahara H, Itoh M, Takahashi A, Aizaki K, et al. (2014) Hemimegalencephaly in a patient with coexisting trisomy 21 and hypomelanosis of Ito. J Child Neurol 29(3): 415-420.
- Sharma S, Sankhyan N, Kabra M, Kumar A (2009) Hypomelanosis of Ito with hemimegalencephaly. Dermatol online J 15(11): 12.
- Chapman K, Cardenas JF (2008) Hemimegalencephaly in a patient with a neurocutaneous syndrome . Semin Pediatr Neurol 15(4): 190-193.
- Iype M, Iype T, Geetha S, Retnakumar J (2007) Hypomelanosis of Itowith cerebral malformation. Indian J Pediatr 74(11): 1044-1045.
- Tagawa T, Futagi Y, Arai H, Mushiake S, Nakayama M et al. (1997) Hypomelanosis of Ito associated with hemimegalencephaly: a clinicopathological study. Pediatr Neurol 17(2): 180-184.
- Flores-Sarnat L (2002) Hemimegalencephaly Part 1. Genetic, clinical, and imaging aspects. J Child Neurol 17(5): 373-384.
- Barkovich AJ, Chuang SH (1990) Unilateral megalencephaly. Correlates of MR imaging and pathological characteristics. AJNR Am J Neuroradiol 11: 523-531.
- Flores-Sarnat L, Sarnat HB, Davila-Gutierrez G, Alvarez A (2003) Hemimegalencephaly: Part 2. Neuropathology suggests a disorder of cellular lineage. J Child Neurol 18(11): 776-785.
- Battalgia D, Di Rocco C, Iuvone L, Acquafondata C, Iannelli A, et al. (1999) Neuro-cognitive development and epilepsy in children with surgically treated hemimegalencephaly. Neuropediatrics 30(6): 307- 313.
- Luders H, Schuele SU (2006) Epilepsy surgery in patients with malformations of cortical development. Curr Opin Neurol 19(2): 169- 174.
- Tinkle BT, Schorry EK, Franz DN, Crone KR, Saal HM (2005) Epidemiology of hemimegalencephaly: a case series and review. AM J Med Genet A 139(3): 204-211.
- Sasaki M, Hashimoto T, Furushima W, Okada M, Kinoshita S, et al. (2005) Clinical aspects of hemimegalencephaly by means of a nationwide survey . J Child Neurol 20(4): 337-341.
- Di Rocco C, Battalgia D, Pietrini D, Piastra M, Massimi L (2006) Hemimegalencephaly: clinical implications and surgical treatment. Childs Nerv Syst 22(8): 852-866.
- Hung PC, Wang HS (2005) Hemimegalencephaly: cranial sonographic findings in neonates. J Clin Ultrasound 33(5): 243-247.
- Agid R, Lieberman S, Nadjari M, Gomori JM (2006) Prenatal MR diffusion - weighted in a fetus with hemimeglencephaly. Pediatr Radiol 36(2): 138-140.






























