The Role of Psychosocial Rehabilitation Within the Biopsychosocial Model
Christina Crawford G1,6*, Stanley Crawford L2,3, Prasad Padala R1,2, Benjamin Wright C2,4, Aparna Das5
1Geriatric Research Education and Clinical Center (GRECC), Central Arkansas Veterans Healthcare System (CAVHS), Little Rock, AR, USA
2Department of Psychiatry, University of Arkansas for Medical Sciences (UAMS), Little Rock, AR, USA
3Department of Geriatrics, UAMS, Little Rock, AR, USA
4Community-Based Outpatient Clinic Mental Health Medical Director, Veterans Health Administration
5Department of Psychiatry, Advent Health Orlando
6University of Arkansas at Little Rock Rehabilitation Counseling program
Submission: May 21, 2024; Published: June 06, 2024
*Corresponding author: Christina G. Crawford, Geriatric Research Education, and Clinical Center (GRECC), Central Arkansas Veterans Healthcare System (CAVHS) and of Rehabilitation Counseling, University of Arkansas, Little Rock, AR, USA
How to cite this article: Christina Crawford G*, Stanley Crawford L, Prasad Padala R, Benjamin Wright C, Aparna Das. The Role of Psychosocial Rehabilitation Within the Biopsychosocial Model. OAJ Gerontol & Geriatric Med. 2024; 8(2): 555734. DOI: 10.19080/OAJGGM.2024.08.555734
Abstract
Psychosocial Rehabilitation focuses on social and psychological factors related to a person’s rehabilitation experience and the outcome of overall treatment. This paper aims to promote psychosocial intervention and assessment through our own clinical demonstration project report and literature review of positive psychosocial attributes such as self-worth, adaptability, optimism, self-efficacy, coping skills, communication, interpersonal skills, and diverse therapy interventions designed to help a person overcome anxiety, distress, depression, and trauma. A person’s environment can be positive when filled with support but negative when they have become isolated and lack interpersonal relationships and support.
Negative psychosocial responses such as anxiety, distress, social withdrawal, aggression, substance use, and impulsive behaviors such as gambling, and depression have the potential to hold people back from levels of attainable recovery. A search was conducted online on PubMed/MEDLINE for information on this topic using the keywords psychosocial, biopsychosocial, disability, and pain. Articles reviewed were published within the last 10 years and had a focus on areas labeled as psychosocial including but not limited to trauma, pain, coping skills, self-efficacy, adaptability, self-worth, optimism, communication, interpersonal skills, anxiety, distress, depression, environment, and expectations.
Results of the articles indicate the prioritizing of psychosocial interventions as helping people with chronic pain and disability to reframe negative thoughts and to become more optimistic, productive, and promote healing. In addition, our clinical demonstration project concluded Psychosocial intervention further mediates a healthier outlook on life and may lead to a better psychological and social experience, encouraging participation in an activity, therapies, and pharmacological treatment.
Keywords: Psychosocial; Biopsychosocial; Disability; Pain; Pain Catastrophizing Scale
Abbreviations: FAM: Fear Avoidance Model; CBT: Cognitive Behavioral Therapy; AEM: Avoidance Endurance Model; LOT: Life Orientation Test; PCS: Pain Catastrophizing Scale; VAS: Visual Analogue Scale; FEX: Future Expectations questionnaire; CPT: Cognitive Processing Therapy; WHO-ICF: World Health Organization International Classification of Functioning, Disability, and Health; GRECC: Geriatric Research Clinical and Education Center; BRCS: Brief Resilient Coping Scale; AGS: American Geriatric Society; JHR: Journal of Humanities in Rehabilitation; ACTION: Addiction Clinical Trial Translations, Innovations, Opportunities, and Networks; APS: American Pain Society; PTSD: Posttraumatic Stress Disorder; RA: Rheumatoid Arthritis
Introduction
Maybe you are not a Star Wars fan like I am dating back to the original Star Wars in 1977. Since then, they’ve come out with multiple sequels and prequels to Star Wars and I have watched them all, at least once. Recently, when watching “Star Wars, The Rise of Skywalker” a line spoken by Prince Leia stood out to me. The general was giving her a report of the battle against the empire and things were looking bleak for the resistance. She looked at the general and said, “Do me a favor, be optimistic”. Even in some of the most difficult of circumstances, and in life’s disappointments, our attitude of optimism and willingness to work on things, may make a difference.
The medical humanities are composed of many academic disciplines that contribute to our understanding of the personal, cultural, and social factors of care. The relevance of these factors is reflected in the current International Classification of Disease model that includes two psychosocial domains – personal and social. These domains have gained greater relevance than in the past as research emerges that shows the connection and cause and effect of these dimensions on rehabilitation interventions and outcomes.
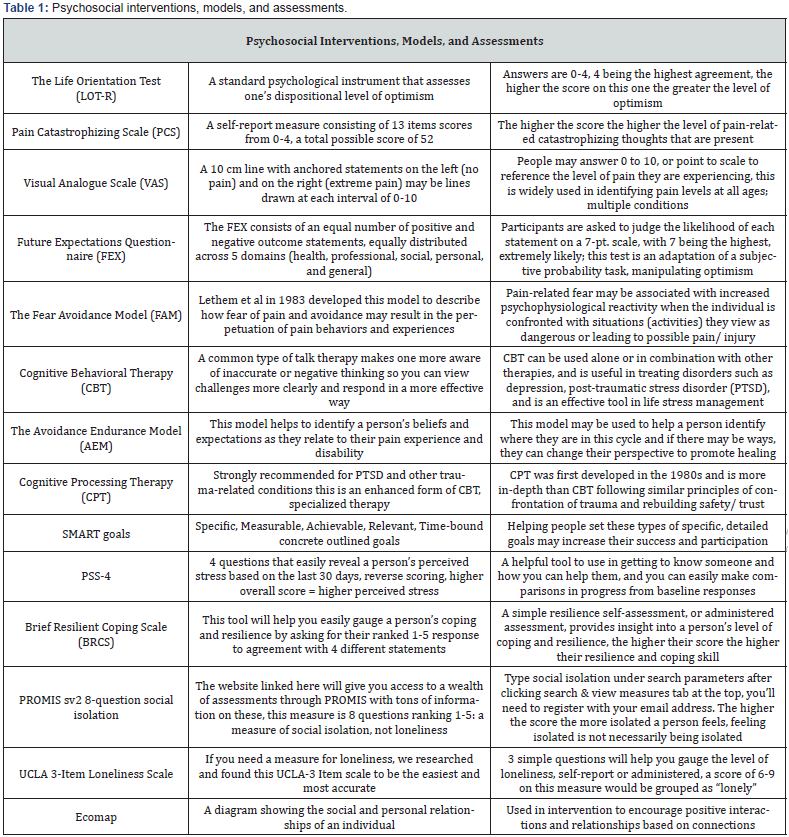
Psychosocial interventions, treatments, assessments, and methodology in rehabilitation focus on the human and social dimensions of care related to overall outcomes in a person’s rehabilitation experience and success. Certain treatments using the psychosocial recovery model, within the biopsychosocial framework, focus on reframing a person’s attitude and psychological response to their physical condition. The psychosocial assessments and interventions, that can be used as interventions, we reviewed are as follows: The Fear Avoidance Model (FAM) [1,2], Cognitive Behavioral Therapy (CBT), The Avoidance Endurance Model (AEM) [3], The Life Orientation Test (LOT-R), Pain Catastrophizing Scale (PCS), Visual Analogue Scale (VAS), Future Expectations questionnaire (FEX) and Cognitive Processing Therapy (CPT) [4] (Table 1). Often assessments for intervention must be validated by research to be considered usable in therapy and in this case in their use for efficacy in psychosocial intervention. Brief Cognitive Behavioral Therapy is one of the simplest evidence-based treatments to set specific goals. These goals are often practical in nature and this type of approach is emulated in our Connection Plan goals sheet.
Dr. George Engel and Dr. John Romano are credited with developing the biopsychosocial model in the 1970s to address the behavioral, thought, and emotional influences that affect a person’s health and wellness [5,6]. The biopsychosocial model of care has been used for the understanding and treatment of chronic pain and disability for many years [3]. The World Health Organization International Classification of Functioning, Disability, and Health (WHO-ICF) defines disability as stemming from different, mutually related bio-psychosocial factors. However, disability is defined by the ADA as “a person with a disability as a person who has a physical or mental impairment that substantially limits one or more major life activities. This includes people who have a record of such an impairment, even if they do not currently have a disability. It also includes individuals who do not have a disability but are regarded as having a disability” [7].
Within the biopsychosocial model, psychosocial factors and variables are often secondarily viewed by many service providers as a reaction to the pain [2]. However, the process of psychosocial intervention focuses on improving psychological responses and underlying vulnerabilities as a means to better manage pain, not just responding to physical limitations with an automatic cognitive reaction such as becoming agitated, irritable, aggressive, apathetic, anxious, fearful, and depressed. [3]. The idea of any type of intervention is to be proactive, not reactive to disability and chronic conditions with hopes to shift the paradigm to response versus reactionary.
For the past 3 years, the Geriatric Research Clinical and Education Center (GRECC) has conducted ongoing psychosocial interventions reaching out to veterans post-COVID-19. Through these interventions, we encourage participants to set goals in the areas of body, mind, and social connectedness. In speaking with over 100 geriatric candidates who are suffering from limited mobility, chronic pain, chronic disease, diagnosed disability, and various health problems, we have found success through psychosocial intervention and assessment outcomes. These are people often isolated by their physical limitations. By brainstorming with them about their interests, many continue to practice their set goals and psychosocial activities long after the 8-week intervention, and we keep in touch with them. While their condition, pain, or disability status remain unchanged, our results indicated they increased in confidence, resilience, and perceived stress was reduced. There are many unique stories and experiences to share from our Connection Plans program. Early on in our Connection Plans program people were still isolated due to COVID. I had one Veteran who set a goal to walk 3 times per week at a local park. The goal enabled him to walk regularly while adding socialization. Part of his specific goal was to say hi to several people while walking. More currently, I had a participant who is 90 years old and completed 5, 500 or 1000-piece jigsaw puzzles. I send (one at a time of course) he sent me a picture of the completed puzzles on many occasions. I have one Veteran who wrote and blogged poetry, and another who chose adult coloring books, and journaling. Still another Veteran who enjoyed fixing jewelry, sewing buttons, and making repairs on clothing by hand for his family. He had children and grandchildren who depended on him for sewing repairs. His legs are not as strong as in the past, but he is finding fulfillment in what he can do through a positive perspective, using his upper body.
Within our GRECC clinical demonstration project, we conducted multiple assessments including the PSS-4, Brief Resilient Coping Scale (BRCS), and PROMIS sv2 8-question social isolation questionnaire (Table 1). These assessments were provided at a baseline initial visit and then results were measured in comparison after 8 weeks of ongoing intervention. We measured the difference after a person became engaged in 8-10 weeks of physical activity, social connectedness, and/ or reframing thoughts, and practicing mental exercises, as part of their goals. This progress was noted using VA REDCap assessments at baseline and follow-up. This allowed the interventionists to instantly use a data comparison tool and share with the Veteran the scores from their initial visit to the final visit. A significant number of participants showed an increase in coping, confidence, and cognition. The increase in physical activity plays a role in the increase of these psychosocial areas and the positive cyclical pattern results in a greater participation in health initiatives including but not limited to physical therapy and occupational therapy treatment.
Results. The results (Table 2) of our Geriatric Research Education and Clinical Center (GRECC) clinical demonstration indicates a significant positive effect after a person completes the 8-12-week psychosocial intervention.

The decrease in social isolation and loneliness resulted in increased coping and confidence. In addition to brainstorming with an individual and getting to know them, their goals, likes, dislikes, daily patterns, and some of their relationship connections, we provided resources to them to pursue success. Resources included ongoing VA program information from our whole health and wellness along with sending puzzles, art sets, calendars, whiteboards, puzzle books, printed word searches, athome seated exercise printouts, at-home seated stretching from NIH, VA crisis line information, PTSD application information, sleep hygiene referrals, and referrals to peer support. When our focus turned to meeting needs from a whole health perspective, psychosocial avenues of care were a natural result and are meant to enhance formal treatment and care for which there is no replacement. A poster presentation for the connection plans clinical demonstration is accepted by the 2023 & 2024 American Geriatric Society (AGS) annual meeting [8].
Ms. L, a veteran we have regular contact with through the intervention program, has experienced chronic pain due to fibromyalgia for over 20 years. She says the diagnosis was newer and less accepted when she received it. This led to some providers being harsh and less compassionate. I asked her what helped her to overcome the negative effects of the chronic pain, which at one point caused her to think of suicide. She attests to having a change of attitude leading to a determination on her part, precipitated by the compassionate care her healthcare provider gave. In asking for specific advice on helping she simply answered, “Listening, it really helps when people just listen to you.” Ms. L walks with a cane or rollator on most days to stay as active as possible, with the intent to increase mobility, balance, posture, and stamina.
This meta-analysis of psychosocial interventions highlights how a focus on the area of psychosocial well-being, encourages the positive, along with reframing negative thoughts using psychosocial intervention methods may impact physical and psychiatric responses of people who are struggling with chronic pain or disability. Cognitive therapy interventions may include reframing negative thought patterns such as cognitive behavioral therapy (CBT) (Table 1) into each day to counteract apathetic responses to therapy. Highlighting how a person’s outlook may apply to their treatment and long-term prognosis, there is evidence to support engagement in regular physical activity, positive social connections, and encouraging communication will result in improved coping outcomes. A search was conducted online on PubMed, MEDLINE, and The Journal of Humanities in Rehabilitation (JHR).
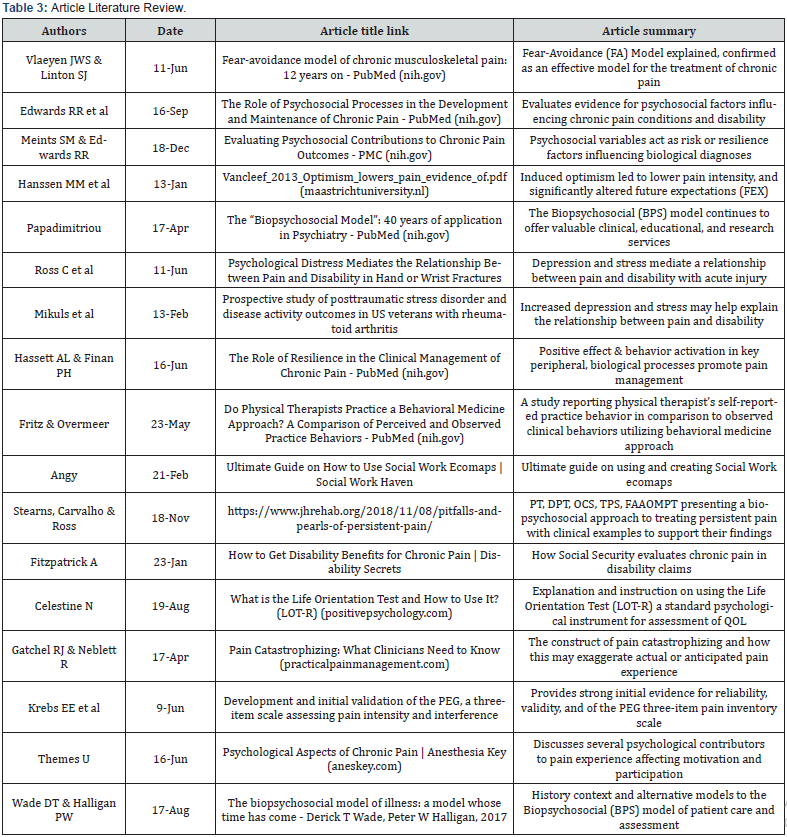
In our review of online information on this topic we used the keywords psychosocial, biopsychosocial, disability, and pain. The author and co-authors reviewed articles published with a focus on differing areas labeled as psychosocial including but not limited to trauma, pain, coping skills, self-efficacy, adaptability, self-worth, optimism, communication, interpersonal skills, anxiety, distress, depression, environment, and expectations. The articles with summaries were included in this overview (Table 3). Articles include holistic health care relating to a person’s overall dayto- day experience and show a significant correlation between optimism, psychosocial intervention, reduced pain, wellness, as well as positive coping outcomes for those with long-term diagnoses.
A recent study by Fritz & Overmeer focused on incorporating a biopsychosocial view and behavior change techniques in physical therapy and determined the need for therapists to focus on psychosocial rehabilitation in their clinical practice. This study observed patient interactions on video of 23 physical therapists within 139 patient consultations. There was only a small extent devoted to the psychosocial or behavioral aspects affecting the patient’s participation and therapeutic outcomes during these consultations [9].
Positive Appraisal May Counter Pain-Specific Negative Appraisal
The results of our literature review support the idea of addressing psychological or psychosocial aspects within a person’s rehabilitation treatment plan and suggest these may have a positive impact on overall health outcomes. The effects of optimism on pain tolerance study results indicated “dispositional optimism significantly correlates to both positive and negative future expectations as measured with the Future Expectation Assessment, FEX” [4] (Table 1) These revealed general positive appraisals can counter pain-specific negative appraisal and indicates the value of positive interventions providing useful alternatives in reducing pain catastrophizing and a focus on psychosocial intervention as highly relevant [4]. A cross-sectional study by Ross et al demonstrates a significant relationship (p<0.001) between pain, disability, and symptoms of depression, anxiety, and stress. This cross-sectional study collected selfreport data from 594 patients with acute/ hand/ wrist fractures, including variables such as depression and stress, but not anxiety. The conclusion of this study indicated psychosocial factors as contributing to the mediated relationship between pain and a person with a physically limiting disability [10]. Edwards et al based their evaluation of psychosocial factors influencing diagnoses and the trajectory of chronic pain disorders on the Addiction Clinical Trial Translations, Innovations, Opportunities, and Networks (ACTION) American Pain Society (APS) chronic pain, Pain Taxonomy (AAPT) evidence-based, multidimensional, chronic pain classification system, and concluded, “There is ample evidence to support the biopsychosocial model of care as it relates to caring for individuals who are faced with chronic pain and physical limitations due to disability” [2].
Mikuls et al. studied 1,522 US Veterans in a longitudinal observational study of posttraumatic stress disorder (PTSD) as it relates to the occurrence and severity of symptoms of Veterans with Rheumatoid Arthritis (RA). In comparison to those within the group who did not have a psychiatric diagnosis, those with PTSD or an anxiety/depression diagnosis experienced more frequent comorbid illnesses, and those patients without a psychiatric diagnosis reported lower pain values than those diagnosed with PTSD [11]. Results of this research found an association between those with a PTSD diagnosis correlating with higher values of self-reported pain, in comparison to patients with no psychiatric diagnosis. Conclusions of patient-reported outcomes of those with RA disease, findings were like those with anxiety and depression diagnoses, as well as participants diagnosed with PTSD [11]. The aim of the Mikuls et al study is to determine if the distress caused by psychological symptoms such as depression, anxiety, and/or stress may mediate a relationship between pain and disability.
The Meints, Hanssen, and Hassett study evaluated participants meeting clinical research criteria focusing on psychological distress as it relates to chronic pain. Results indicated the relationship between pain, and disability, and symptoms of depression, anxiety, and stress, were statistically significant (P <0.001) [11]. They referenced psychosocial contributions of pain and disability highlighting the positive effects of optimism as likely to decrease pain and improve functioning while negative affect was associated with increased pain and dysfunction, according to their evaluation and research on the contributions of psychosocial factors to the experience of chronic pain [3,4,12].
In Hanssen et al results regarding optimism, there were 79 participants between the ages of 18 and 35 years old. Participants were recruited for participation in a study examining the influence of visualization on pain during Cognitive Processing Therapy (CPT) [4]. Cognitive Processing Therapy or CPT (Table 1) is a specific cognitive behavioral mode of therapy that enables patients to learn how to modify and challenge their thought life to reframe unhelpful beliefs or negative thoughts related to trauma. There were several questionnaires (Table 1) used to measure the effects of optimism versus negativity in response to pain: The Life Orientation Test (LOT-R), Pain Catastrophizing Scale (PCS), Visual Analogue Scale (VAS) and the Future Expectations questionnaire (FEX). This was of substantial theoretical and clinical importance as it aimed to support the causal status of optimism as it relates to pain 4. In many cases, chronic pain is considered a disability depending on the duration and limitations of functioning related to persistent pain [13]. The Life Orientation Test is a psychological instrument, self-administered in most cases, that indicates the level of optimism in a person and provides meaningful insight into how clients may replace harmful thought patterns with more constructive thought patterns [14]. The Pain Catastrophizing Scale measures the extent of catastrophic thinking in three major categories: pain-rumination, magnification, and helplessness [15]. A visual analog scale measures pain intensity on a line continuum scale such as choosing a pain level from 1-10. The PEG- 3: pain screening tool is a good example of a visual analog scale for pain [16]. The Future Expectations questionnaire is an adaptation of the Subjective Probability Task and determines negative and positive future outcomes across 5 domains: health, professional, social, personal, and general. The results of the Hanssen et al. study concluded a significant correlation between optimism and lowering of pain intensity, and better psychological and physical well-being were indicated in the study [4].
Discussion
The results indicate many psychosocial factors that influence rehabilitation outcomes [17]. Some psychosocial constructs are pain-specific such as altered central nervous system pathways, catastrophizing, coping, expectations, and self-efficacy [3]. There is a wealth of evidence delineating that psychosocial factors such as depression, anxiety, and other types of emotional stress may contribute to a greater degree than physical limitations regarding key long-term outcomes of persistent pain management [3].
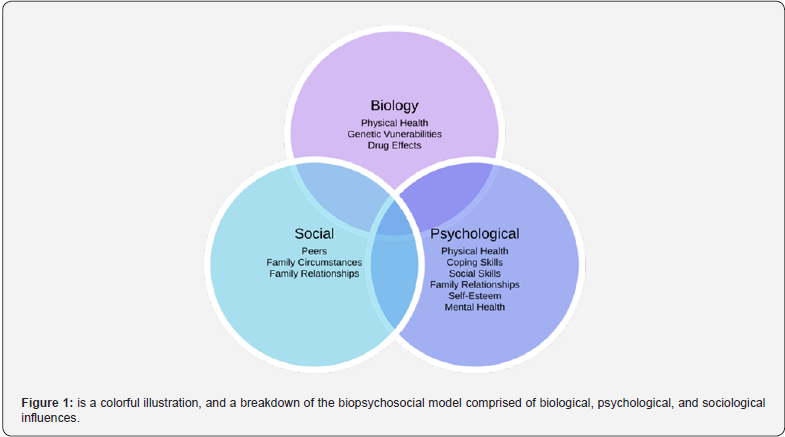
Figure 1, illustrates a breakdown of the biopsychosocial model of care into each of its three respective parts. The extending details of the image outline support the psychosocial domain by including psychological (thoughts, emotions, and behaviors such as psychological distress, fear/avoidance beliefs, current coping methods, and attribution) and sociological (socio-economical, socio-environmental, and cultural factors such as work issues, family circumstances, and benefits/economics) focused pieces to this puzzle which interconnect with the biological (physiological pathology) aspect of a person’s individualized experience [18]. Using this model as a guideline, an Ecomap could be drawn for a client to aid in determining their needs in each area of the biopsychosocial model [19].
Implications for Rehabilitation as it Relates to Pain and Disability
One example found in the Hanssen et al study concluded an attitude of optimism was indicated on more than one occasion as linked to better psychological well-being, especially during times when one could choose to focus on adverse circumstances yet choose to remain positive [4]. The effect of this cycle becomes clear as a continuum of the negative psychosocial variables as they relate to pain and disability. In a study by Ross et al., “mediation analyses were conducted to determine the role of depression, anxiety, and stress in the relationships between pain and disability, controlling for relevant demographic variables.” The conclusions of this study indicated both depression and stress as significantly related to the mediating relationship between pain and disability [10] which supports focused psychosocial impact on a relationship between biological rehabilitative factors.
Cognitive Behavior Therapy (CBT) has been used to help people reframe negative automatic cognitions by encouraging the role of positive cognitive responses to their circumstances. In addition, physical activity therapies can play a positive role in improving individual pain outcomes. In these examples, we see the psychosocial aspects of treatment and other aspects such as physical activity working together within the biopsychosocial model of care to help improve the patient’s response to the negative impacts of chronic pain as well as long-term disability [3].
The Fear Avoidance Model (FAM) outlines the concept of fear as a factor in the psychological response of people with a disability and those people who may experience persistent and chronic pain. This model developed over 20 years ago has been widely used to describe the process of psychosocial aspects as it relates to pain-related outcomes. Edwards et al described the multidimensional factors of interacting forces that contribute to chronic pain [2]. The Fear Avoidance Model is used to describe psychosocial variables such as pain-related catastrophizing in contrast with pain-related coping, and self-efficacy for managing pain and other aspects of long-term disability [3].
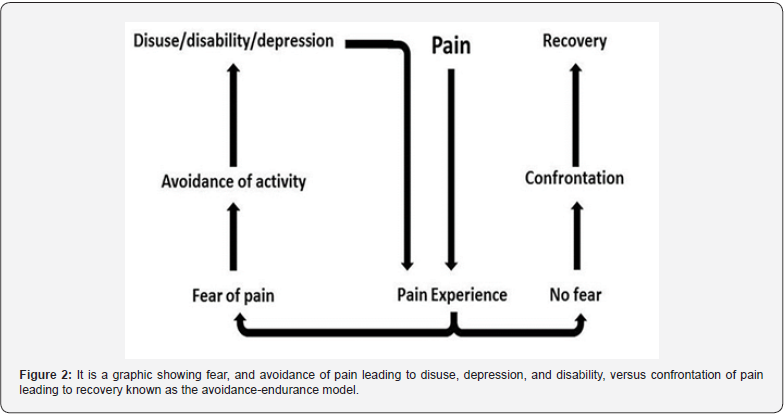
The avoidance-endurance model (AEM) in Figure 2 above outlines confrontation as a part of recovery and demonstrates the role of psychosocial rehabilitation in the process of recovery within the biopsychosocial model. Confronting pain or physical limitation versus making attempts to avoid it leading to adverse emotional responses is more productive and key to positive long-term outcomes of recovery from the experience of pain and disability [20].
In addition to other physical and occupational therapies, modalities of treatment such as a TENS unit, or medications often prescribed to help with adverse anxieties, distress, and physical pain experienced by an individual, psychosocial rehabilitation such as these interventions, models, and assessments are all part of holistic treatment [3]. There is often the opportunity for clinicians and practitioners in pain management and rehabilitation services such as Physical Therapists to address the psychosocial needs of a patient while they are in biologic treatment [21]. These specialties are often star quarterbacks (and head cheerleaders) in a person’s rehabilitation and recovery. However, any clinician can make a mindful effort towards building a person up.
Conclusions
While the biomedical model remains a prominent illness model in public awareness, the biopsychosocial model has become an established alternative and widely used model [22]. The biopsychosocial model is geared towards recognizing the impact of psychological as well as sociological factors as they impact a person’s disability and are associated with chronic or acute pain. This reminds practitioners and clinicians of the significant association of the psychosocial aspect of care including psychological and sociological contributors to a person’s overall experience and encourages holistic patient care. Incorporating the psychosocial aspect in rehabilitation has proven effective for rehabilitation recovery outcomes and the reduction of pain.
Self-assessment and discussion can be productive means of communication about personal thought patterns and may lead to an opportunity for psychosocial rehabilitation to become part of the larger rehabilitation process. Clinicians are in a unique position to help people who may be experiencing psychosocial difficulties with their disability and chronic pain by employing techniques such as Cognitive Behavioral Therapy (CBT), the Avoidance Endurance Model (AEM), the Fear Avoidance Model (FAM), self-report and measured psychosocial assessments referenced here (Table 1). They may also have additional resources to provide to their clients which will help them experience success in these areas. Increased listening by the practitioner translates to participation in therapy.
Utilizing and prioritizing psychosocial interventions may help people with chronic pain or disability to reframe negative thought patterns and become more optimistic, active, productive, and reduce suffering. These interventions may further mediate a healthier outlook on life leading to a better psychological and social experience, enhancing overall physical and mental wellness, and encouraging participation in their physical therapies, and compliance with medication regimens. Psychosocial rehabilitation doesn’t ask what a person can do but instead asks what they would like to do, and seeks to help them set goals to attain the highest level of function in this area. This open-ended question can lead to a discussion about positive interests, activities, possibilities, and fan the force of optimism, despite a person’s circumstances which may include pain or disability.
References
- Vlaeyen JWS, Linton SJ (2012) Fear-avoidance model of chronic musculoskeletal pain: 12 years on. Pain 153(6): 1144-1147.
- Edwards RR, Robert HD, Mark DS, Dennis CT, Ajay DW (2016) The Role of Psychosocial Processes in the Development and Maintenance of Chronic Pain. J Pain 17(9 Suppl): T70-92.
- Meints SM, Edwards RR (2018) Evaluating psychosocial contributions to chronic pain outcomes. Prog Neuropsychopharmacol Biol Psychiatry 87(Pt B): 168-182.
- Hanssen MM, Madelon LP, Johan WSV, Yvo MCM, Linda MGV(2013) Optimism lowers pain: evidence of the causal status and underlying mechanisms. Pain 154(1): 53-58.
- Papadimitriou G (2017) The Biopsychosocial Model: 40 years of application in Psychiatry. Psychiatriki 28(2): 107-110.
- Marschall A, PsyD (2023) Understanding the Biopsychosocial Model of Health and Wellness.
- Network AN (2024) What is the definition of disability under the ADA?
- Korrapati C, Choksi MSU, Crawford C, Gauss, CH, Mendiratta P, et al. (2023) Improving Social Interaction, Resilience, and Loneliness In Cognitively Impaired Older Adults. American Geriatric Society.
- Fritz J, Overmeer T (2023) Do Physical Therapists Practice a Behavioral Medicine Approach? A Comparison of Perceived and Observed Practice Behaviors. Phys Ther 103(5): pzad025.
- Ross C, Ilona J, Hopin L, Luke P, Tasha RS, et al. (2015) Psychological Distress Mediates the Relationship Between Pain and Disability in Hand or Wrist Fractures. J Pain 16(9): 836-843.
- Mikuls TR, Prasad RP, Harlan RS, Fang Yu, Kaleb M, et al. (2013) Prospective study of posttraumatic stress disorder and disease activity outcomes in US veterans with rheumatoid arthritis. Arthritis Care Res (Hoboken) 65(2): 227-234.
- Hassett AL, Finan PH (2016) The Role of Resilience in the Clinical Management of Chronic Pain. Curr Pain Headache Rep 20(6): 39.
- Fitzpatrick A (2021) How Social Security Evaluates Chronic Paid in Disability Claims. Disability Secrets.
- Celestine N (2021) What is the Life Orientation Test and How To Use It.
- Gatchel RJN, Pain R (2017) Catastophizing: What Clinicians Need to Know. Practical Pain Management 15(6).
- Krebs EE, Karl AL, Matthew JB, Teresa MD, Jingwei W, et al. (2009) Development and initial validation of the PEG, a three-item scale assessing pain intensity and interference. J Gen Intern Med 24(6): 733-738.
- Rubin SE, Roessler RT, Rumrille PD (2016) Foundations of the Rehabilitation Process. (7th edn). 2016, Indianapolis, IN: Pro Ed.
- Karina C, Jackson K, Lowe R, Hampton L, Bell J, et al. (2020) Biopsychosocial Model. Physiopedia.
- Angy S (2021) Struggling with completing Ecomaps. Ultimate Guide on How to use Social Work Ecomaps.
- Themes U (2016) Psychological Aspects of Chronic Pain.
- Stearns ZR, Carvalho ML, Ross MA (2018) Pitfalls and Pearls of Persistent Pain. J Humanities Rehabilitation (JHR).
- Wade DT, Halligan PW (2017) The biopsychosocial model of illness: a model whose time has come. Clin Rehabil 31(8): 995-1004.






























