Bilateral Identical Ethmoidal Dural Arteriovenous Fistula, Extremely Rare Case
Abolghasem Mortazavi1*, Seyedsina Ahmadiabhari1, Ebrahim mahmoudi1, Peyman Gookizadeh1, Fatemeh Ghazizadeh Hashemi2 and Mohammad Ghorbani3
1Department of Neurosurgery, Sina Hospital, Tehran University of Medical Sciences, Tehran, Iran
2Psychiatry and Psychology Research Center, Roozbeh Hospital, Tehran University of Medical Sciences, Tehran, Iran
3Department of Neurosurgery, Division of Vascular and Endovascular Neurosurgery, Firoozgar Hospital, Iran University of Medical Sciences, Tehran, Iran
Submission: April 22, 2024; Published: May 03, 2024
*Corresponding author: Abolghasem Mortazavi, Department of Neurosurgery, Sina Hospital, Tehran University of Medical Sciences, Tehran, Iran
How to cite this article: Abolghasem Mortazavi*, Seyedsina Ahmadiabhari, Ebrahim mahmoudi, Peyman Gookizadeh, Fatemeh Ghazizadeh Hashemi and Mohammad Ghorbani. Bilateral Identical Ethmoidal Dural Arteriovenous Fistula, Extremely Rare Case. OAJ Gerontol & Geriatric Med. 2024; 8(2): 555731. DOI: 10.19080/OAJGGM.2024.08.555731
Abstract
A dural arteriovenous fistula (DAVF) is an arteriovenous shunt located in the dural wall of the venous sinus or the expanded layer of the dura mater. Dural arteriovenous fistulas (DAVFs) account for approximately 10%-15% of intracranial vascular malformations. The primary goal in treating DAVFs is the complete obliteration of the arteriovenous shunt. Currently, option for treatments of Ethmoidal DAVFs include surgical resection, endovascular treatment (EVT) and stereotactic radiosurgery. In this paper we report cases of bilateral ethmoidal AVF treated endovascularly and review their clinical presentation, history of treatment options, and recent advances in endovascular management.
Keywords: Ethmoidal DAVFs; Tortuous Conjunctival Vessels; Retinal Thrombosis; Systemic Heparinization; Angioarchitecture
Introduction
A dural arteriovenous fistula (DAVF) is an arteriovenous shunt located in the dural wall of the venous sinus or the expanded layer of the dura mater [1]. Dural arteriovenous fistulas (DAVFs) account for approximately 10%-15% of intracranial vascular malformations [2]. Anterior ethmoid DAVFs are included in about 10% of DAVFs [3]. Patients may be asymptomatic or experience symptoms ranging from headaches to fatal hemorrhage [4]. The venous drainage pattern has been reported as the main factor determining the DAVFs clinical presentation [5-7]. The primary goal in treating DAVFs is the complete obliteration of the arteriovenous shunt [8,9]. Currently, option for treatments of Ethmoidal DAVFs include surgical resection, endovascular treatment (EVT) and stereotactic radiosurgery [10,11].
Traditionally Open surgical treatment was the main treatment for ACF DAVFs, but endovascular treatment using recently available microcatheters and liquid embolic materials is also becoming a safe and effective treatment [10-12]. In this paper we report cases of bilateral ethmoidal AVF treated endovascularly and review their clinical presentation, history of treatment options, and recent advances in endovascular management. We report the third case of bilateral ethmoidal DAVF and review the literature on this regard.
Case Presentation
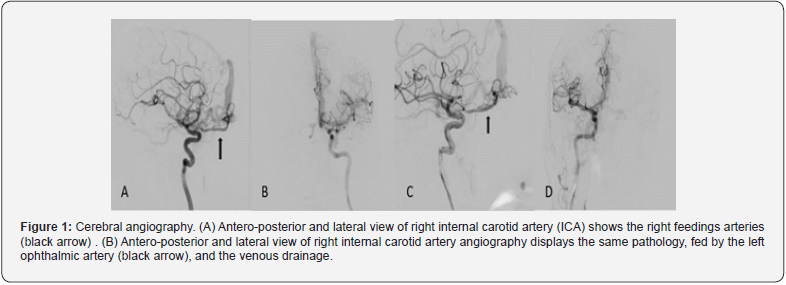
A 41-year-old man presented with severe headache, visual decline for 2 years. The symptoms were preceded by sneezing. There was no history of trauma or family history of vascular abnormalities. Ocular exam revealed a visual acuity of 20/70 OD and 20/30 OS. There was no restricted eye movement. she had mild periorbital edema, dilated and tortuous conjunctival vessels. Digital subtraction angiogram revealed bilateral ethmoidal arteriovenous fistula supplied by the bilateral OA and draining into the SSS via ectatic cortical veins (Figure 1). The ectatic cortical veins which was grossly dilated and tortuous drained anteriorly into several small tributaries with slow outflow. No nidus and no communication into the cavernous sinus were observed. Transarterial Onyx18 embolization was performed via the OA.
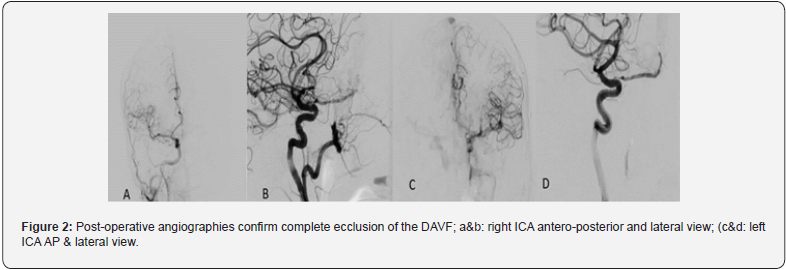
Endovascular procedure was performed on the patient under general anesthesia. A Marathon microcatheter (ev3 Neurovascular, Irvine, California) was advanced into one of the proper feeders arising from the distal OphA, and distal to the origin of a common trunk of central retinal artery. Angiography immediately after the procedure showed complete occlusion of the AVF. Systemic heparinization was continued for 1 week after the procedure to prevent retinal thrombosis. The postoperative course was favorable, with clinical improvement occurring immediately after the operation. At discharge, visual acuity was improved and headache was decreased. After three months, the lesion on the opposite side was treated in the same way as mentioned. Cerebral angiography performed 1 year after embolization revealed the complete disappearance of the lesions (Figure 2).

Discussion
DAVFs of the anterior cranial base, also called “ethmoidal fistulas” or “cribriform plate fistulas,” are extremely uncommon lesions [8]. In ACF DAVFs, the main feeding arteries are the AEA of the OA. however, feeders from MMA , ethmoidal branch (sphenopalatine artery) of the internal maxillary artery (IMA), the pial branches of the ACA and MCA, the angular branch of the facial artery and even the persistent primitive olfactory artery can be involved in ACF DAVF [13-15]. The fistula point of an ACF DAVF is usually located at the level of the cribriform plate in the lateral epidural space, which includes the lamina cribrosa and the orbital roofs [11]. The venous drainage routes of ACF DAVFs include drainage to the frontal veins and then secondarily into the SSS [16].
Understanding the angioarchitecture of the DAVF is important for successful treatment. The treatment of the lesion can be divided into endovascular or surgical methods based on the anatomical structure of the lesion. In ACF DAVFs, EVT should be considered only in patients with favorable angiographic anatomy. However, in appropriate patients, EVT is effective and associated with a high obliteration rate [13]. The therapeutic goal of EVT is for the embolic agents to penetrate through the trans osseous shunt to obliterate in trans arterial approach it is important to ensure that the central retinal artery(CRA) is not occluded. In TVE approach the path from the puncture point to the DAVF is longer and difficult to navigate, so that TVE is more time taking [5].
TAE is the first selection in patients with good trans arterial access (e.g., large and easily navigable OA with limited proximal vessel tortuosity) that allows distal microcatheterization in close proximity to the fistulous point and a less degree of reflux [17]. Additionally, TVE is preferred in DAVF with easily navigable draining vein and short cortical distance [8]. In EVT, although complications may occur, AVF DAVFs have an acceptable prognosis in appropriately selected patients. Surgery has proved the highest healing rate and three surgical approaches are used for ethmoidal DAVFs anterior interhemispheric approach, orbitozygomatic approach and bilateral sub frontal approach is the most common approach for ethmoidal DAVFs. Although the surgical treatment of ethmoidal DAVFs is an effective approach, it exposes patients to peri- and postoperative risks associated with craniotomy and major surgery [11]. Over the years, there are a progressive shift in the treatment of dural AVFs with endovascular treatment considered the first line of therapy in the majority of case [14].
Advancement in technique and instrument along with improvement in the embolic agents available leads endovascular both safer and more effective in selected patients with e-dAVFs. It seems that according to the cosmetic issues and the level of invasiveness, if the artery has a suitable size for microcatheterization or if there is possible venous access, endovascular treatment is the choice. As shown in the figure 3 [18], in trans arterial treatment, it is very important to determine the origin of the retinal artery and inject the distal onyx into this artery. Retinal artery occlusion causes blindness.
In general, surgery is considered for ethmoidal DAVFs with intracranial hemorrhage or after failed EVT or radiosurgery, actually ethmoidal DAVFs with fine or tortuous arterial feeders, and when the main artery of the ethmoidal DAVF has many branches into adjacent structures of brain parenchyma [9,12,19,20].
Conclusion
Bilateral ethmoidal DAVFs are a rare disease. The present study describes the safe and complete obliteration of the fistula by trans arterial endovascular treatment through the ophthalmic artery. Careful angiographic evaluation of ethmoidal DAVFs and appropriate treatment option are required to achieve excellent outcomes.
References
- Guo Y, Yu J, Zhao Y, Yu J (2018) Progress in research on intracranial multiple dural arteriovenous fistulas. Biomed Rep 8(1): 17-25.
- Brown Jr RD, Flemming KD, Meyer FB, Cloft HJ, Pollock BE, et al. (2005) Natural history, evaluation, and management of intracranial vascular malformations. Mayo Clinic Proc 80(2): 269-281.
- Jamous MA, Satoh K, Satomi J, Matsubara S, Nakajima N, et al. (2004) Detection of enlarged cortical vein by magnetic resonance imaging contributes to early diagnosis and better outcome for patients with anterior cranial fossa dural arteriovenous fistula. Neurol Med Chir 44(10): 516-521.
- Chung SJ, Kim JS, Kim JC, Lee SK, Kwon SU, et al. (2002) Intracranial dural arteriovenous fistulas: analysis of 60 patients. Cerebrovasc Dis 13(2): 79-88.
- Van Dijk JMC, terBrugge KG, Willinsky RA, Wallace MC (2002) Clinical course of cranial dural arteriovenous fistulas with long-term persistent cortical venous reflux. Stroke 33(5): 1233-1236.
- Van Dijk JMC, TerBrugge KG, Willinsky RA, Wallace MC (2002) Multiplicity of dural arteriovenous fistulas. J Neurosurg 96(1): 76-78.
- Van Dijk JMC, TerBrugge KG, Willinsky RA, Wallace MC (2004) Selective disconnection of cortical venous reflux as treatment for cranial dural arteriovenous fistulas. J Neurosurg 101(1): 31-35.
- Robert T, Blanc R, Smajda S, Ciccio G, Redjem H, et al. (2016) Endovascular treatment of cribriform plate dural arteriovenous fistulas: technical difficulties and complications avoidance. J Neurointerv Surg 8(9): 954-958.
- Grady C, Benjamin CG, Kondziolka D (2017) Radiosurgery for dural arteriovenous malformations. Handb Clin Neurol 143: 125-131.
- Agid R, TerBrugge K, Rodesch G, Andersson T, Söderman M (2009) Management strategies for anterior cranial fossa (ethmoidal) dural arteriovenous fistulas with an emphasis on endovascular treatment. J Neurosurg 110(1): 79-84.
- Defreyne L, Vanlangenhove P, Vandekerckhove T, Deschrijver I, Sieben G, et al. (2000) Transvenous embolization of a dural arteriovenous fistula of the anterior cranial fossa: preliminary results. Am J Neuroradiol 21(4): 761-765.
- Chen CJ, Lee CC, Ding D, Starke RM, Chivukula S, et al. (2015) Stereotactic radiosurgery for intracranial dural arteriovenous fistulas: a systematic review. J Neurosurg 122(2): 353-362.
- Deng JP, Li J, Zhang T, Yu J, Zhao ZW, et al. (2014) Embolization of dural arteriovenous fistula of the anterior cranial fossa through the middle meningeal artery with Onyx. Clin Neurol Neurosurg 117: 1-5.
- Cannizzaro D, Peschillo S, Cenzato M, Pero G, Resta M, et al. (2018) Endovascular and surgical approaches of ethmoidal dural fistulas: a multicenter experience and a literature review. Neurosurg Rev 41(2): 391-398.
- Tsutsumi S, Shimizu Y, Nonaka Y, Abe Y, Yasumoto Y, et al. (2009) Arteriovenous Fistula Arising from the Persistent Primitive Olfactory Artery With Dual Supply From the Bilateral Anterior Ethmoidal Arteries. Case Report. Neurol Med Chir 49(9): 407-409.
- Lawton MT, Chun J, Wilson CB, Halbach VV (1999) Ethmoidal dural arteriovenous fistulae: an assessment of surgical and endovascular management. Neurosurgery 45(4): 805-810.
- Matsumaru Y, Alvarez H, Rodesch G, Lasjaunias P (1997) Embolisation of branches of the ophthalmic artery. Interv Neuroradiol 3(3): 239-245.
- Prada D, Harris A, Guidoboni G, Rowe L, Verticchio-Vercellin AC, et al. (2019) Vascular anatomy and physiology of the eye. Ocular Fluid Dynamics p. 23-45.
- Pradilla G, Coon AL, Huang J, Tamargo RJ (2012) Surgical treatment of cranial arteriovenous malformations and dural arteriovenous fistulas. Neurosurgery Clin 23(1): 105-122.
- Park SH, Park KS, Kang DH, Hwang JH, Hwang SK (2017) Stereotactic radiosurgery for intracranial dural arteriovenous fistulas: its clinical and angiographic perspectives. Acta Neurochirurgica 159(6): 1093-1103.






























