Use Of Personal Voice Assistants by Older Adults and Its Implication for Geriatric Care
Guoqing Chen*, Ryan Spaulding, Shawna Wright and Shelley Bhattacharya
University of Kansas Medical Center, Kansas City, KS USA
Submission: September 26, 2023; Published: October 13, 2023
*Corresponding author: Guoqing Chen, University of Kansas Medical Center, Kansas City, KS USA
How to cite this article: Guoqing Chen*, Ryan Spaulding, Shawna Wright and Shelley Bhattacharya. Use Of Personal Voice Assistants by Older Adults and Its Implication for Geriatric Care. OAJ Gerontol & Geriatric Med. 2023; 7(4): 555719. DOI: 10.19080/OAJGGM.2023.07.555719
Abstract
Background: The growing use of personal voice assistant (PVA) in the population has sparked significant interest in their potential to revolutionize self-management of chronic diseases and geriatric care. However, there are few evidence-based findings available about effectiveness of using PVA currently.
Objective: This mini review aims to examine how off-the-shelf PVA was being used by older adults and their experience.
Method: This review used keywords and text terms, searching three databases: PubMed, CINHAL and Web of Science, and the search was limited to the published journal articles between the years 2013 and 2023.
Results: The final review included ten articles directly related to actual use of PVA. The review found older adults had positive perceptions and experience in the use of PVA in the initial phase. All studies were descriptive except one that used a randomized controlled trial design and with a small sample size. Despite the perceived usefulness of using PVA, there was no complete assessment of the effectiveness of use of PVA on outcomes of older adults. The review finds gaps in the literature and suggests intervention-based randomized controlled trials with sufficient statistical power to assess the effectiveness and cost-effectiveness of these voice-activated technologies.
Keywords: Chronic Diseases; Geriatric Care; Aging; Cognitive
Keywords: PVA: Personal Voice Assistant, RCT: Randomized Controlled Trial, HC: Healthy Control, MCI: Mild Cognitive Impairment, PACE: Program for All-Inclusive Care of the Elderly
Introduction
The rapid advancement of voice-activated technology has profoundly impacted various aspects of our daily lives, including aging and healthcare. A main innovation in recent years is the personal voice assistant (PVA), which continues to grow, and more people use these smart devices. PVA is defined as “hardware devices or software agents that are powered by artificial intelligence and assist people with information searches, decision-making efforts or executing certain tasks using natural language in a spoken format.”[1] The popularity of the voice-assistants is because of their ability to facilitate human–computer interactions naturally and intuitively, similar to the conversations between human beings. In the United States, the older population has significantly grown since 2010 and is expected to increase to 81 million in 2040 and 95 million in 2060 [2].
Smart devices such as Amazon’s Alexa, Google’s Nest, and Apple’s Home Pod can connect to the Internet by speaking instead of typing, and voice commands are improving increased access to intelligent technologies among disabled adults and the rapidly increasing aging population. [3,4] Conventional user interfaces, such as computers and smartphones, are often difficult for older adults with visual, fine motor, or cognitive impairment to operate easily. Smart devices incorporate artificial intelligence, which uses algorithms that emulate human cognitive and behavioral processes. The software apps of various platforms allow older adults to connect to the internet and knowledge bases [5]. The voice-activated personal assistants’ platform can automatically process and respond to human voice and language. Through natural language processing and machine learning, PVAs interpret voice prompts and respond with voice messages using a simulated human tone [6].
Older adults who are sixty or over represent a significant portion of the general population. These technologies offer a unique set of beneficial possibilities and challenges. While personal voice assistants help set reminders, look up information, and check weather updates, their full potential in this population is far from realized [7]. Despite the PVAs growing popularity, older adults’ adoption and usability of these technologies are not straightforward. The evidence-based findings of integrating these technologies in geriatric care remain unknown. In this mini-review, we aimed to explore how off-shelf PVAs such as Amazon Alexa, Google Nest, and Apple Home Pod were used and the published findings, discuss potential risks associated with PVA use in older adults, identify gaps in the current research, and suggest avenues for future studies. We limited it to three brands because their PVA dominates in the US market, is low cost, and easy to set up.
Method
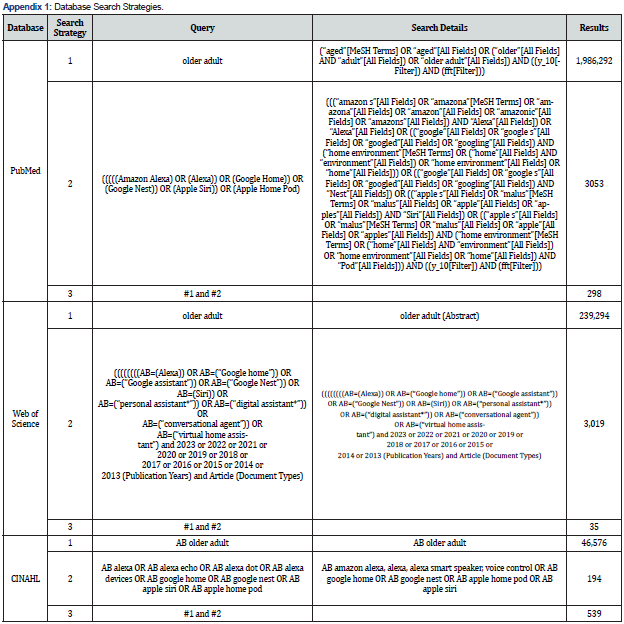
We conducted a literature search across multiple databases, including PubMed, CINAHL, and Web of Science. An array of terms and keywords were employed in the database search to ensure comprehensive coverage of the relevant studies. The search incorporated keywords including “personal voice assistants,” “voice assistant,” “Alexa,” “Google Nest,” “Google Home,” “Apple Siri,” “Apple Home Pod”, “older adult,” and “senior.” Boolean operators such as “AND” “OR” and “NOT” were used to refine the search strategy and outcomes. The initial screen was based on the titles and abstracts for relevance to the topics of use of personal voice assistants and older adults. For this review, we selected peer-reviewed publications in English and included only studies that use these voice assistants in older adults. After the screening and reviewing, ten studies were selected for this review.
Results
Study Characteristics
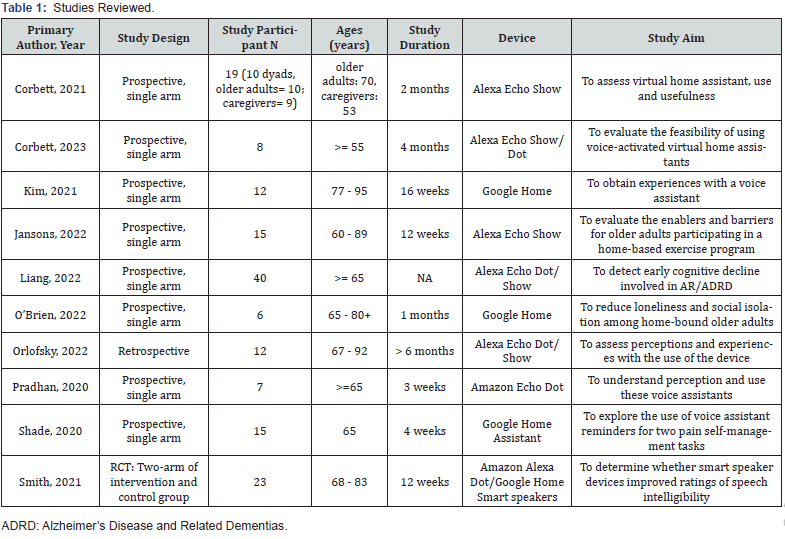
Study designs of these ten studies included in this mini-review were descriptive. All were used convenience samples except for one study. [8] Of the eleven studies, eight used single-arm prospective approaches [9-16] one was retrospective analyses [17]. There was only one study using a design of randomized controlled trial (RCT) [8] (Table 1). The findings of six prospective and one retrospective study were based on qualitative content analysis, the sample size range of study participants from 6 to 19. One of Corbett’s studies used a dyad as a study unit that included older adults (n = 10) and their respective caregivers (n = 9). [10] Liang et al. reported findings upon 40 participants who were either Healthy Control (HC) participants or Mild Cognitive Impairment (MCI) on the differential cognition status through machine-learning models. [13] Corbett used a dyad as a unit to recruit older adults, including ten and their respective caregivers (n = 9). [10] The duration of studies ranged from 3 weeks to 6 months. Amazon devices were used in eight studies, and Google devices in five.
User Acceptance and Usability
Corbet’s dyad study demonstrated that the most frequent PVA uses were listening to music, requesting information, obtaining weather forecasts and news, and enjoying entertainment e.g., jokes and podcasts [10]. Older adults used PVA to listen to music more often than caregivers. The caregivers used PVA to gain information more often than older adults. The users were more active in using the device in the first week, then decreased over time in all categories, i.e., getting information, obtaining weather or news, or making calls. The feature of reminder was not actively used. The study found that some participants felt Alexa provided companionship and security; reminders were helpful for what they should do daily. However, some participants experienced difficulties figuring out the capabilities of the devices they owned and understanding those that did and did not work together. The manual was difficult to understand for them.
In Corbett’s other study [9], she examined how older adults in the Program for All-Inclusive Care of the Elderly (PACE) used Alexa PVA. The study participants used the intelligent features of Alexa on voice-activated lighting and getting information. These older adults infrequently used Alexa’s skills that could promote physical exercise or cognitive games, e.g., chair yoga and word recall games. Orlofsky et al. examined Amazon’s Alexa potential for older adults to successfully age in place, including smart home technology to support social engagement, health, wellness, and daily functioning at home [17]. To understand about their perceptions and experiences with the use of the device, Orlofsky et al. interviewed twelve home-dwelling older adults aged 65 and older who had used the Alexa devices of Echo Show or Dot for at least six months to gain insights into how this technology had shaped their aging experience. They found no significant differences in the senior responses based upon or attributed to age, education, race/ethnicity, marital status, health status, or level of social engagement. They identified several barriers to using the Alexa devices. Their findings show that older adults with little initial and ongoing support did not fully utilize the Alexa device’s full spectrum of functionality and features. The older adults enjoying the use of the Alexa device for selective nonessential features and centain functions which were convenient to use on the Alexa device, but they did not see the use of the Alexa device as essential to their successful aging in place.
Jansons et al. utilized Alexa Echo Show to evaluate the feasibility of remotely delivering an individually tailored, homebased exercise program to older adults living independently and alone [11]. They found all 15 older participants aged 60 to 89 (with a mean age of 70.3 years) had 100% retention; adherence to the exercise program was over the targets. There were no adverse events reported to be related to the intervention, while the usability scored as above average (75/100). Other outcomes, such as health-related quality of life, did not significantly change across the 12-week follow-up. They concluded it is feasible and safe to prescribe a home-based exercise program delivered and monitored remotely by an exercise physiologist using an Alexa device. In their qualitative study [18], older adults reported that using voice interactions to engage in the Alexa exercise program was user-friendly, convenient to access the program from home, simple to use and enjoyable; and the conversation style and reminder function of the Alexa provided motivation and social engagement to them adherence the exercise program. Some participants reported technical issues, i.e., poor internet connectivity and inaccuracy of voice recognition, as barriers to maintaining them in the Alexa home-based exercise program.
Other barriers included inadequate feedback or attention to patient goals in an asynchronous digital health approach, and privacy concerns. Similar issues were also reported by Pradhan, et al. [15] In the study, they conducted a 3-week field deployment of the Amazon Echo Dot seven older adults living at home to know how older adults who use technology infrequently perceive and use these voice assistants. They observed consistent usage for finding online information, while other types of actual usage dropped over the three weeks, such as playing music, setting timers, and reminders. Kim et al. examined the effects of gender, age, and individual belief on using Google Home devices. [12] They found there were no individual differences in young adults.
There was variation within the older adult group, but the variations were not statistically different. They observed that results in the usage of Alexa devices. They also found that female participants showed no difference in perception of human likeness for movements produced by a virtual robot and a digital human. However, in the same study, males did show a distinction by rating the digital human movements as more human-like than the robot. They found that older adults had several challenges that evolved from unfamiliarity with a voice assistant in their first interactions to coping with the devices’ technical and functional errors. O’Brien, K. et al. explore the utilities of Google Home devices to reduce loneliness and social isolation among home-bound older adults [14]. They recruit older adults and geriatric experts to participate in their homes for four weeks and then provide feedback. The investigators received 288 comments from these participants. They identified eight domains of PVA in reducing loneliness: administrative support, companionship, home control, education, emergency communication, entertainment, health and well-being, and reminders. Their study findings showed that PVA can be useful across multiple domains and potentially provide physical, social, and cognitive stimulation to home-bound older adults. PVA can offer many functional benefits, focus on common geriatric syndromes, and help reduce social isolation and loneliness. However, some participants faced challenges related to effectively using PVA. The learning curve involved in phrasing commands and questions properly for the device was an issue. Shade et al. explored using PVA’s reminders for selfmanagement of community-dwelling older adults with chronic pain while assisting them for independence [16]. They enrolled fifteen participants with chronic pain and an average age of 65 who used the voice assistant for four weeks. Participants reported moderate scores for pain severity with a mean = 4.6 [SD = 2.3] and pain interference with a mean = 4 [SD = 2.6]). The PVA usability was above average (78 of 100). The median time to set up the Google Home Assistant profile was 5 minutes, with a median of asking for help two times. The participants perceived the pain self-management task reminders from the Google Home assistant as consistent, easy to set up, and helpful for accountability. The investigators concluded that voice assistant reminders might be an option for assisting a variety of pain self-management tasks in older adults.
Smith et al. conducted a RCT examining the effectiveness of employing smart speakers on speech and communication difficulties in individuals with intellectual disability (ID) [8]. Amazon Alexa and Google Home voice assistants can provide four important features for learning: spaced practice, reward immediacy, autonomy/intrinsic motivation, and reduced social barriers. They aimed to determine whether providing individuals with intellectual disabilities with smart speaker devices improved speech intelligibility ratings for
• Phrases related to device use and
• unrelated words.
They enrolled and randomized 21 older adults into the intervention group and 22 into the control group. The study participants were recorded saying smart speaker-related phrases and unrelated words before and after about 12 weeks. Naive participants then rated the intelligibility of the speech recordings. The intervention group participants who received smart speakers made significantly more significant intelligibility gains than the control group. Despite the modest effect size, they found the difference for both smart speaker-related phrases and unrelated words, which was in favor of the intervention. These initial findings suggest that voice-activated technology could be a novel and inclusive way to improve speech intelligibility in vulnerable populations. Amazon Alexa and Google Home voice assistants could improve speech intelligibility. The presence of PVA in the home had a demonstrable impact on speech intelligibility ratings. It could provide inclusive support for speech and communication improvement, cost-effective, improving the quality of life of vulnerable populations.
Discussion
This mini-review examined the use of voice-activated personal assistants (PVAs) by older adults. The findings suggest that PVAs have the potential to offer a variety of benefits to older adults, including convenience, social engagement, health management, and independence. However, older adults may face challenges when using PVAs, such as technical difficulties, privacy concerns, and lack of awareness. Results also show that participants had several challenges that evolved from the unfamiliarity with a voice assistant in their first interactions to coping with the functional errors due to limited speech technology as they got used to using it [17]. The learning curve associated with these technologies can significantly hinder their acceptance among older adults [19].
Therefore, implementing training modules or guidelines can facilitate ease of use and thus increase user satisfaction [20]. An intuitive design that minimizes cognitive load can greatly encourage usage among older adults [21]. The design includes large, legible fonts and simple navigation pathways. Research suggests that devices with less complex interfaces correlate with higher usage among older populations [22]. Real-time feedback mechanisms, like voice confirmations or visual cues, can bolster the user experience. Research indicates that such immediate feedback can enhance device confidence and reduce operation errors [22]. In addition, Family members and caregivers can facilitate the learning curve and motivate older adults to explore new technologies [23,24].
The use of voice assistants (PVAs) by older adults is a growing area of interest [25,26]. PVAs can potentially improve the quality of life for older adults by providing companionship, assisting with daily tasks, promoting physical activity and cognitive health, and managing chronic health conditions [27]. However, more research is needed to develop and implement PVAs specifically designed to meet older adults’ needs and address the challenges they face. The main limitations of these studies are small sample size, single-arm, and descriptive [9,14,15]. By addressing the challenges and needs of older adults, PVAs can be made more accessible and beneficial for this growing population.
Another critical factor is the management of chronic conditions. Technologies like Alexa have built-in functionalities that could assist with symptom tracking and alerting healthcare providers in real time [28]. The impact of voice assistants on mental well-being should not be overlooked. For many older adults, particularly those who live alone, voice assistants could serve as companionship, alleviating feelings of loneliness and improving mental health [29]. The evidence-based finding on this topic is scant, and rigorous studies evaluating the outcomes of such functionalities are yet to be conducted, underscoring the need for comprehensive research.
Some feasibility studies and pilot programs have explored voice assistants’ role in self-management, assisting with medication reminders, scheduling appointments, and symptom tracking [28,30]. A potential avenue for investigation relates to medication adherence. Older adults often have complex medication regimens, and voice assistants could offer timely reminders and information, potentially improving adherence rates [31,32]. However, most of these studies were small in scale and lacked the rigor of randomized controlled trials. The preliminary findings are promising but must be validated through more extensive research.
Older adults need cognitive support in their daily lives. Voice assistants could offer various cognitive support functionalities, such as aiding memory recall or providing cognitive behavioral therapy-based interventions for mental health [27]. These applications could be particularly useful for older adults with mild cognitive impairment. However, further research is needed to establish efficacy and long-term effects [33,34]. Future research should focus on developing PVAs that are more user-friendly and accessible for older adults. Although voice-activated personal assistants have permeated various domains of daily living, their role in geriatric care remains undefined. Studies demonstrated that common usage patterns among older adults included setting reminders and weather information, but few studies directly assessed the effectiveness of these devices through well-designed pragmatic trials in disease management for this population. Most studies were qualitative, feasibility, and pilot tests. The data supporting this hypothesis is currently lacking, emphasizing the need for targeted studies.
With the increased telemedicine adoption, there is growing interest in integrating voice assistants as a patient-clinician interface [35]. Making telemedicine for geriatric services more acceptable for people with limited health and computer literacy may affect the ability of older adults with chronic health conditions to use home-based telemedicine systems effectively. Recent studies explored using Amazon Alexa to deliver various skill sets to individuals with minimal computer literacy. Alexa assistant can potentially help older adults who do not feel comfortable using computers or computer-like devices to overcome computer literacy barriers by allowing natural voice–driven interactions with the telerehabilitation system. However, substantial barriers such as data security, interoperability, and clinician adoption must be overcome for effective implementation [36]. Additionally, research should explore the long-term effects of PVA use on older adults and conduct a trial-based study. In practice, healthcare providers and other professionals who work with older adults should educate them about the potential benefits and challenges of PVA use, help them to identify the best PVA for their needs, and teach them how to use it safely and effectively.
Implications for Geriatric Care
The findings of this mini review have several implications for geriatric care. First, PVAs have the potential to offer a variety of benefits for older adults, including supporting medication management, chronic disease management, fall prevention, and dementia care. Second, healthcare providers can play a role in helping older adults to use PVAs safely and effectively by educating them about the potential benefits and challenges of PVA use, helping them to choose the right PVA for their needs, teaching them how to use PVAs safely and securely, and providing support and troubleshooting assistance. Third, PVAs can collect data on older adults’ health and well-being. This data can be used to screen and monitor the early decline of cognitive function, improve the quality of geriatric care, and develop new interventions to support older adults. Overall, PVAs have the potential to play an important role in geriatric care by supporting older adults to manage their health and well-being.
Potential Risks in Using PVA for Geriatric Patients
Voice-activated personal assistants carry potential benefits and risks that need to be carefully evaluated, mainly when used by older adults. Data privacy and security, user error, overdependence, and safety are concerns. As these devices often require access to personal data to function effectively, data privacy and security remain a significant concern [37,38]. Voice assistants often store voice commands in cloud servers, which, if not adequately protected, can cause unauthorized access and misuse of personal information. Cybersecurity remains a lingering concern when using digital technology in healthcare settings [39]. The risk of breach is higher for older adults who may not be tech-savvy as they might be unable to implement additional security measures. A balance between utility and privacy should be meticulously considered during the system’s design and implementation phases [35]. Trust in technology is essential, particularly for older adults who may be wary of potential risks like identity theft [40]. Robust security measures, such as twofactor authentication and data encryption, can alleviate these concerns and increase willingness to adopt new technology.
User error is caused by cognitive and physical aging-related impairment that might cause unintentional misuse of voice assistant technology. Simple commands may be mispronounced or forgotten, leading to incorrect health advice or delays in emergency responses, which could exacerbate health conditions. The technology’s potential for misuse could lead to unintended consequences, such as accidental emergency calls or accessing misleading or harmful information online. Despite Natural Language Processing (NLP) advancements, voice recognition technology is not flawless. Many older adults are not fully educated on the safe use of digital technologies, including voice assistants [41]. Therefore, education on safety for using PVA is necessary for older adults. Over-dependence on using PVA could be a risk of reducing human-to-human contact. Older adults may find the convenience of voice assistants enticing, which can result in social isolation and a decline in physical activity.
Conclusion
The studies included in this mini-review provide valuable insights into using PVAs by older adults. PVAs have the potential to offer a variety of benefits to older adults. However, addressing the challenges they may face when using PVAs to maximize their benefits is crucial. Future research should focus on developing more user-friendly and accessible PVAs for older adults and develop intervention-based randomized controlled trials to assess the effectiveness and cost-effectiveness of these technologies. Additionally, research should explore the long-term effects of PVA use on older adults. In practice, healthcare providers and other professionals who work with older adults should educate them about the potential benefits and challenges of PVA use, help them to identify the best PVA for their needs, and teach them how to use it safely and effectively.
References
- Ki CW, Cho E, Lee JE (2020) Can an intelligent personal assistant (IPA) be your friend? Para-friendship development mechanism between IPAs and their users. Computers in Human Behavior 111: 106412.
- US Census Bureau (2020) 65 and Older Population Grows Rapidly as Baby Boomers Age, USA.
- Vollmer Dahlke D, Ory MG (2017) Emerging Opportunities and Challenges in Optimal Aging with Virtual Personal Assistants. Public Policy & Aging Report 27(2): 68-73.
- Zwakman DS, Pal D, Arpnikanondt C (2021) Usability Evaluation of Artificial Intelligence-Based Voice Assistants: The Case of Amazon Alexa. SN Computer Science 2(1): 28.
- Bérubé C, Kovacs ZF, Fleisch E, Kowatsch T (2021) Reliability of Commercial Voice Assistants' Responses to Health-Related Questions in Noncommunicable Disease Management: Factorial Experiment Assessing Response Rate and Source of Information. Journal of Medical Internet Research 23(12): e32161.
- Islam MU, Chaudhry BM (2023) A Framework to Enhance User Experience of Older Adults with Speech-Based Intelligent Personal Assistants. Ieee Access 11: 16683-16699.
- Arnold A, Kolody S, Comeau A, Miguel Cruz A (2022) What does the literature say about the use of personal voice assistants in older adults? A scoping review. Disabil Rehabil Assist Technol 22: 1-12.
- Smith E, Sumner P, Hedge C, Powell G (2021) Smart speaker devices can improve speech intelligibility in adults with intellectual disability. International Journal of Language & Communication Disorders 56(3): 583-593.
- Corbett CF, Bowers DC, Combs EM, Parmer M, Jones K, et al. (2023) Using Virtual Home Assistants to Address Vulnerable Adults' Complex Care Needs: An Exploratory Feasibility Study. Journal of Gerontological Nursing 49(6): 33-40.
- Corbett CF, Combs EM, Wright PJ, Owens OL, Stringfellow I, et al. (2021) Virtual Home Assistant Use and Perceptions of Usefulness by Older Adults and Support Person Dyads. International Journal of Environmental Research and Public Health 18(3): 1113.
- Jansons P, Fyfe J, Dalla Via J, Daly RM, Gvozdenko E, et al. (2022) Barriers and enablers for older adults participating in a home-based pragmatic exercise program delivered and monitored by Amazon Alexa: a qualitative study. Bmc Geriatrics 22(1): 248.
- Kim S, Choudhury A (2021) Exploring older adults' perception and use of smart speaker-based voice assistants: A longitudinal study. Computers in Human Behavior 124: 106914.
- Liang XH, Batsis JA, Zhu YX, Driesse TM, Roth RM, et al. (2022) Evaluating voice-assistant commands for dementia detection. Computer Speech and Language 72: 101297.
- O'Brien K, Light SW, Bradley S, Lindquist L (2022) Optimizing voice-controlled intelligent personal assistants for use by home-bound older adults. Journal of the American Geriatrics Society 70(5): 1504-1509.
- Pradhan A, Lazar A, Findlater L (2020) Use of Intelligent Voice Assistants by Older Adults with Low Technology Use. Acm Transactions on Computer-Human Interaction 27(4): 31.
- Shade MY, Rector K, Soumana R, Kupzyk K (2020) Voice Assistant Reminders for Pain Self-Management Tasks in Aging Adults. Journal of Gerontological Nursing 46(10): 27-33.
- Orlofsky S, Wozniak K (2022) Older adults' experiences using Alexa. Geriatric Nursing 48: 240-250.
- Jansons P, Fyfe JJ, Dalla Via J, Daly RM, Scott D (2023) Barriers and enablers associated with participation in a home-based pragmatic exercise snacking program in older adults delivered and monitored by Amazon Alexa: a qualitative study. Aging Clinical and Experimental Research 35(3): 561-569.
- Harrington CN, Garg R, Woodward A, Williams D (2022) "It's Kind of Like Code-Switching": Black Older Adults' Experiences with a Voice Assistant for Health Information Seeking. Proc SIGCHI Conf Hum Factor Comput Syst 2022: 604.
- Ermolina A, Tiberius V (2021) Voice-Controlled Intelligent Personal Assistants in Health Care: International Delphi Study. Journal of Medical Internet Research 23(4): e25312.
- Boot WR, Moxley JH, Roque NA, Andringa R, Charness N, et al. (2018) Exploring Older Adults' Video Game Use in the PRISM Computer System. Innov Aging 2(1): igy009.
- Tate DF, Lytle L, Polzien K, Diamond M, Leonard KR, et al. (2019) Deconstructing Weight Management Interventions for Young Adults: Looking Inside the Black Box of the EARLY Consortium Trials. Obesity (Silver Spring) 27(7): 1085-1098.
- Czaja SJ (2016) Long-term care services and support systems for older adults: The role of technology. Am Psychol 71(4): 294-301.
- Sharit J, Czaja SJ (2020) Overcoming Older Adult Barriers to Learning Through an Understanding of Perspectives on Human Information Processing. J Appl Gerontol 39(3): 233-241.
- Balki E, Hayes N, Holland C (2022) Effectiveness of Technology Interventions in Addressing Social Isolation, Connectedness, and Loneliness in Older Adults: Systematic Umbrella Review. JMIR Aging 5(4): e40125.
- Helal S, Bull CN (2019) From Smart Homes to Smart-Ready Homes and Communities. Dement Geriatr Cogn Disord 47(3): 157-163.
- Herold F, Theobald P, Gronwald T, Kaushal N, Zou L, et al. (2023) Alexa, let's train now! - A systematic review and classification approach to digital and home-based physical training interventions aiming to support healthy cognitive aging. J Sport Health Sci.
- Hoy MB (2018) Alexa, Siri, Cortana, and More: An Introduction to Voice Assistants. Medical Reference Services Quarterly 37(1): 81-88.
- Williams CYK, Townson AT, Kapur M, Ferreira AF, Nunn R, et al. (2021) Interventions to reduce social isolation and loneliness during COVID-19 physical distancing measures: A rapid systematic review. PLoS One 16(2): e0247139.
- Bérubé C, Schachner T, Keller R, Fleisch EFVW, Barata F, et al. (2021) Voice-Based Conversational Agents for the Prevention and Management of Chronic and Mental Health Conditions: Systematic Literature Review. J Med Internet Res 23(3): e25933.
- Conde-Caballero D, Rivero-Jiménez B, Cipriano-Crespo C, Jesus-Azabal M, Garcia-Alonso J, et al. (2021) Treatment Adherence in Chronic Conditions during Ageing: Uses, Functionalities, and Cultural Adaptation of the Assistant on Care and Health Offline (ACHO) in Rural Areas. J Pers Med 11(3): 173.
- Corbett CF, Combs EM, Chandarana PS, Stringfellow I, Worthy K, et al. (2021) Medication Adherence Reminder System for Virtual Home Assistants: Mixed Methods Evaluation Study. JMIR Form Res 5(7): e27327.
- Oliveira JD, Engelmann DC, Kniest D, Vieira R, Bordini RH (2022) Multi-Agent Interaction to Assist Visually Impaired and Elderly People. Int J Environ Res Public Health 19(15): 8945.
- Talbot CV, Briggs P (2022) The use of digital technologies by people with mild-to-moderate dementia during the COVID-19 pandemic: A positive technology perspective. Dementia (London) 21(4): 1363-1380.
- Sinha Gregory N, Shukla AP, Noel JJ, Alonso LC, Moxley J, et al. (2023) The feasibility, acceptability, and usability of telehealth visits. Front Med (Lausanne) 10: 1198096.
- Milne-Ives M, de Cock C, Lim E, Shehadeh MH, de Pennington N, et al. (2020) The Effectiveness of Artificial Intelligence Conversational Agents in Health Care: Systematic Review. J Med Internet Res 22(10): e20346.
- Sprengholz P, Betsch C (2022) Ok Google: Using virtual assistants for data collection in psychological and behavioral research. Behav Res Methods 54(3): 1227-1239.
- Wilder JL, Nadar D, Gujral N, Ortiz B, Stevens R, et al. (2019) Pediatrician Attitudes toward Digital Voice Assistant Technology Use in Clinical Practice. Appl Clin Inform 10(2): 286-294.
- Maier E, Doerk M, Reimer U, Baldauf M (2023) Digital natives aren't concerned much about privacy, are they? I Com (Berl) 22(1): 83-98.
- Kim S (2021) Exploring How Older Adults Use a Smart Speaker-Based Voice Assistant in Their First Interactions: Qualitative Study. JMIR Mhealth Uhealth 9(1): e20427.
- Alagha EC, Helbing RR (2019) Evaluating the quality of voice assistants' responses to consumer health questions about vaccines: an exploratory comparison of Alexa, Google Assistant and Siri. BMJ Health Care Inform 26(1).






























