Developing An Early Supported Discharge for Delirium (ESDD) Program in An Australian Tertiary Hospital
Emily Jasper1*, Kien Chan2, Meegan Truarn3, Jacquie Bates4, Narelle Hawkins5, Kristie Harper6, Kelly McAuliffe7, Angela Jacques8 and Charles Inderjeeth9
1Geriatrics Senior Registrar, Geriatric and Rehabilitation Medicine, Sir Charles Gairdner Hospital, Perth, Australia
2Consultant geriatrician, Geriatric and Rehabilitation Medicine, Sir Charles Gairdner Hospital, Perth, Australia
3Senior Occupational Therapist, Osborne Park Hospital, Perth, Australia
4Acting Clinical Nurse Consultant Cognitive Impairment, Sir Charles Gairdner Hospital, Perth, Australia
5Clinical Nurse Specialist, Home Link, Sir Charles Gairdner Hospital, Perth, Australia
6Research Coordinator, Occupational Therapy Department, Sir Charles Gairdner Hospital, Curtin University, School of Allied Health, EnAble Institute, Curtin University, Perth, Australia
7Senior Occupational Therapist, Home Visiting Team, Sir Charles Gairdner Hospital, Perth, Australia
8Institute for Health Research, University of Notre Dame, Department of Research, Sir Charles Gairdner Hospital, Perth, Australia
9Consultant Physician, Geriatric and Rehabilitation Medicine, Sir Charles Gairdner and Osborne Park Hospital, Clinical Professor, School of Medicine, University of Western Australia, Clinical Dean, Curtin University
Submission: September 19, 2023; Published: October 10, 2023
*Corresponding author: Włodzisław Kuliński, Department of Rehabilitation, Military Institute of Medicine-National Research Institute, Warsaw, Poland
How to cite this article: Emily Jasper*, Kien Chan, Meegan Truarn, Jacquie Bates, Narelle Hawkins, Kristie Harper, Kelly McAuliffe, Angela Jacques and Charles Inderjeeth. Developing An Early Supported Discharge for Delirium (ESDD) Program in An Australian Tertiary Hospital. OAJ Gerontol & Geriatric Med. 2023; 7(4): 555718. DOI: 10.19080/OAJGGM.2023.07.555718
Abstract
Objective: Delirium in hospitalised older adults is common and associated with increased morbidity and mortality. This single-centre observational study aimed to assess the impact of an early supported discharge for delirium (ESDD) program on hospital length of stay, inpatient complications, readmission, and carer satisfaction.
Methods: All patients were recruited from the acute geriatric ward in a tertiary hospital in Western Australia. Patients recruited to the ESDD program, a supported discharge service allowing patients to be discharged earlier to their home with the support of a career, were compared with an age matched cohort of patients with delirium hospitalized the year prior (receiving current best practice delirium care). All patient data was collected from electronic and paper hospital records for both the retrospective and intervention group.
Results: The retrospective cohort included 100 patients, which was compared to 21 patients in the ESDD program. There were no significant differences between baseline characteristics of the two groups, including comorbidity status and frailty. Hospital length of stay was three days shorter in patients recruited to the ESDD intervention (ESDD median 9 days [6.4-11.6], retrospective 12 days [8.1-15.9], p≤0.001). There was no significant difference in inpatient falls, readmissions, or mortality. The ESDD program was well received by carers and cost-effective for the hospital.
Conclusion: The ESDD program appears to be an effective and feasible model of care for patients with delirium, resulting in a reduced hospital length of stay without any associated harm. This is promising for the future of delirium care, where further evaluation in larger studies is required.
Keywords: Delirium; Geriatrics; Home Care; Supported Discharge; Family Carer
Abbrevation: MAU: Medical Assessment Unit, ESDD: Early Supported Discharge for Delirium, CCI: Charlson Comorbidity Index, mFI: modified Frailty Index, ALoS: Average Length of Stay, nWAU: national Weighted Activity Unit, NEP: National Efficient Price
Introduction
Delirium is common amongst hospitalized older adults and associated with numerous adverse patient and hospital outcomes, including increased length of stay, readmission, morbidity, and mortality [1,2]. Despite ongoing medical advances, delirium associated mortality has remained unaltered over the last 30 years [3]. It is known that delirium prevention through the implementation of routine non-pharmacological measures is most effective, as beyond treating reversible precipitants, we lack definitive evidence for any direct treatment strategy [4]. The utility of family-led, home-based care has recently been demonstrated in delirium research as a proven non-pharmacological intervention with favorable outcomes, including reduced incidence of delirium and length of stay [5,6].
It is widely accepted that the hospital environment is an imperfect environment to deliver delirium care, due to patients being in unfamiliar “chaotic” surroundings, with frequent staff changes, bed moves and uncontrolled noise [7,8]. Previous studies have demonstrated that delivering care in the home environment is successful in preventing the onset of delirium, however providing care for patients with delirium in their home environment has not yet been widely studied [9,10]. There are only a select number of single-centre studies which have examined models of care to support early discharge of patients with delirium, with one Australian centre demonstrating promise with a reduced length of stay without any associated harm [11,12]. Two similar British programs demonstrated their programs were safe and well received, but not associated with reduced length of stay [13,14]. While the concept of early supported discharge for patients with delirium has begun to be explored, the small volume of research is currently insufficient to draw significant conclusions. The objective of this ESSD program was to assess whether a supported early return to the home environment with family support for patients with delirium was feasible, safe, accepted by families and effective in reducing hospital length of stay.
Methods
Study Design & Participants
This was a single-centre observational, feasibility study of patient outcomes before and after the implementation of an ESDD program within a metropolitan hospital. Eligible patients were admitted to the inpatient geriatric ward at a 600-bed tertiary hospital in Perth, Western Australia. Patients are admitted to the inpatient geriatric ward within 48 to 72 hours of their admission, with the majority of cases admitted directly from the Medical Assessment Unit (MAU). Inclusion criteria to the study for both the retrospective and intervention group were those aged ≥ 65 years old, from home, who had a family member able to stay with the patient (for up to 14 days) and had a medical diagnosis of delirium with an identifiable precipitant. Exclusion criteria included patients from residential care, medically unstable, without a suitable carer or unsafe mobility for discharge. This project was registered as Quality Activity 35048 (quality improvement project) and deemed by the hospital to not require ethics approval.
Pre-Intervention
Prior to the intervention (control group), routine care for patients with delirium on the acute geriatric ward involved a geriatrician-led multidisciplinary team screening for reversible causes and implementation of non-pharmacological and pharmacological measures. This model embodies current best practice delirium care, with patients being reviewed daily by a Geriatrician, occupational therapist and cared for by nurses trained in delirium management. Once patients’ delirium had improved, patients were discharged home, transferred for inpatient rehabilitation, or discharged to residential care.
Intervention
The ESDD model is a geriatrician-led subacute service which supports a patient with delirium to return to their own home early with the assistance of a live-in carer. Patients were referred to ESDD at the discretion of the treating Geriatrician. The occupational therapist discussed the program with the patient and their carer to obtain consent for program participation and provide delirium education. A 4AT was completed and if patients scored ≥4 they were referred to HomeLink, the hospital’s outpatient nursing service which provides ongoing acute and subacute care in the patient’s home environment [15]. All patients referred to ESDD were followed up with an occupational therapy home visit or phone call and a memory clinic appointment within eight weeks from discharge.
Once discharged, a HomeLink nurse visited the patient within one day post-discharge to assess progress of their delirium, treatment of the identified precipitant, assess carer stress and provide ongoing guidance on delirium management. During each home visit, the HomeLink nurse completed a 4AT and conducted a survey with the carer. Depending on clinical need, patients were then reviewed on a daily or second daily basis until the 4AT score fell below 4 on two consecutive visits, or visits continued until carers were comfortable in managing the patient. On completion of the ESDD program, a carer satisfaction survey was completed and a HomeLink discharge summary was sent to the GP. The ESDD pathway can be viewed in (Appendix 1).
All carers had access to a 24-hour HomeLink number, allowing them to contact an on-call nurse if they were concerned. Governance over the ESDD program was provided by the On- Call Geriatrician accessible by the nurse 24 hours a day. The On- Call Geriatrician was contacted for medical advice on weaning or ceasing antipsychotic medications or if there were general concerns regarding the patient.
Outcomes
The primary outcome was to compare the inpatient length of stay of patients discharged home with the ESDD program, to patients in the retrospective cohort who would have met the eligibility criteria for the ESDD program. Secondary outcomes measures included inpatient falls, readmissions, mortality, antipsychotic use, and carer satisfaction.
Sample Selection
Patient files (paper records) and electronic records were reviewed to collate data on patient characteristics, demographics, and specified outcomes. An electronic database was set up to collect patient information on both patient cohorts. The study design set the desired number for the retrospective group at 100. The retrospective group was selected from hospital electronic records of patients admitted to the acute geriatric ward with a coded diagnosis of delirium over a nine-month period from July 1st, 2019, to March 21st, 2020. This list was then refined by identifying patients who would have met the inclusion criteria. Inpatient files were then reviewed in chronological segments, where patients who would have met the ESDD inclusion criteria were included in the retrospective group. 189 files were reviewed to achieve the desired 100 patients. The 89 patients were excluded for reasons including; conditions requiring ongoing inpatient management, requiring inpatient rehabilitation or no carer available.
The intervention group were patients discharged home with the ESDD service, from July 14th to November 22nd, 2020. Demographic and inpatient data was collected at the time of discharge from hospital and data regarding the intervention was collected after the patient had completed the ESDD program. Further data related to readmissions and mortality were collected at 30 days, 90 days, and 6 months post discharge respectively. Data was collected during each home visit by HomeLink nurses on paper records and entered electronically once discharged from ESDD.
Statistical analysis
Descriptive summaries of patient characteristics and outcomes consisted of frequency distributions for categorical data and means and standard deviations or medians and interquartile ranges for continuous data, with group comparisons done using chi squared tests and t tests or Mann-Whitney U tests for categorical and continuous comparisons, respectively. Adjusted Cox regressions were used to examine length of stay (LOS) between groups, with results summarised as hazard ratios and 95% confidence intervals and LOS survival probabilities plotted using Kaplan-Meier survival curves. IBM SPSS version 27.0 (Armonk NY) was used for data analysis and significance levels were set at alpha=0.05.
Results
Baseline characteristics
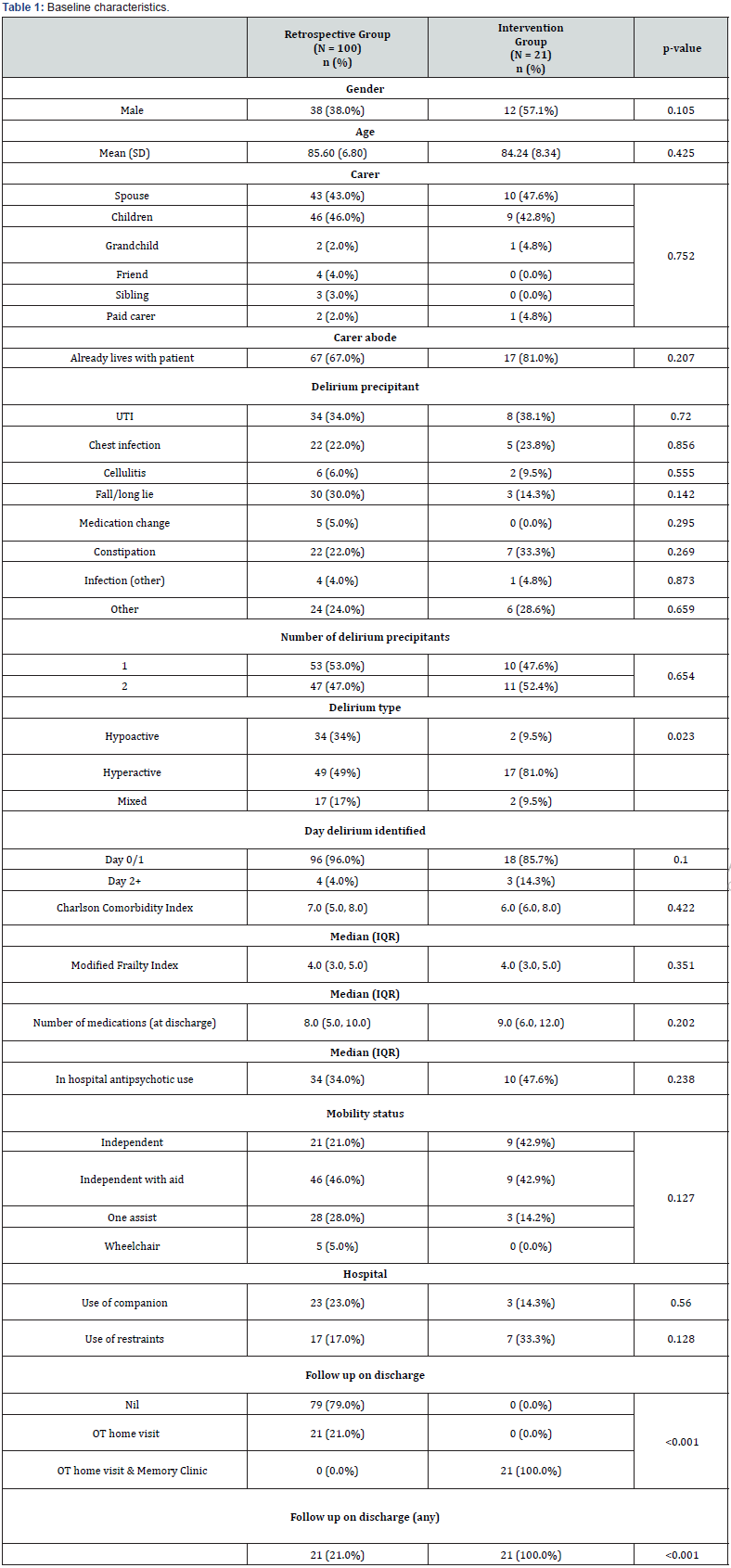
A total of 100 patients were included in the retrospective group and 21 patients in the intervention group. A total of 226 admitted patients were admitted with delirium during the intervention period (July 14th, 2020, to November 30th, 2020), of these 172 patients did not meet the inclusion criteria for ESDD. Of the 54 patients that were eligible for ESDD, 33 patients were not recruited either because family members declined or discharged out of the ESDD service recruitment hours. This gave a recruitment of 21 out of 54 eligible patients (39%). Baseline characteristics are described in (Table 1). The primary carer for patients across both groups was a spouse or their children, with the majority of these carers already living with the patient. The most commonly identified precipitant across both groups was a urinary tract infection. The two groups were comparable on the Charlson Comorbidity Index (CCI) and modified Frailty Index (mFI), demonstrating the comorbid, frail nature of this cohort [16,17]. The only significant differences between the two groups included the number of patients with hypoactive delirium (34% retrospective, 9.5% intervention) and the presence of scheduled follow up on discharge (21% retrospective, 100% intervention).
Outcomes
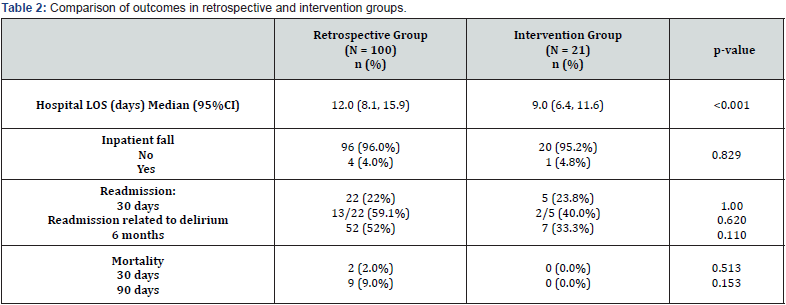
The comparison of outcomes between the retrospective and the intervention group are summarized in (Table 2). The median length of stay (LOS) in the retrospective group was 12 days [8.1,15.9] versus nine days (6.4,11.6) in the intervention group, which was a statistically significant reduction (p≤0.001); hazard ratio 0.46(95% CI: 0.27-0.76, p=0.002) for the intervention group compared to retrospective group, after adjusting for CCI and mFI. The number of inpatient falls between the two groups was low; 4% and 4.8% in the retrospective and intervention group respectively (p=0.829). Readmission rates at 30 days were 22.4% versus 23.8% (p=1.00) and at six months were 52.5% versus 33.3% (p=0.110) for the retrospective and intervention group respectively. The proportion of readmissions related to delirium at 30 days in the retrospective group was 59% and 40% in the intervention group, however this difference was not statistically significant (p=0.620). There were no deaths in the intervention group, compared with nine deaths by 90 days (9%) in the retrospective group (p=0.153).
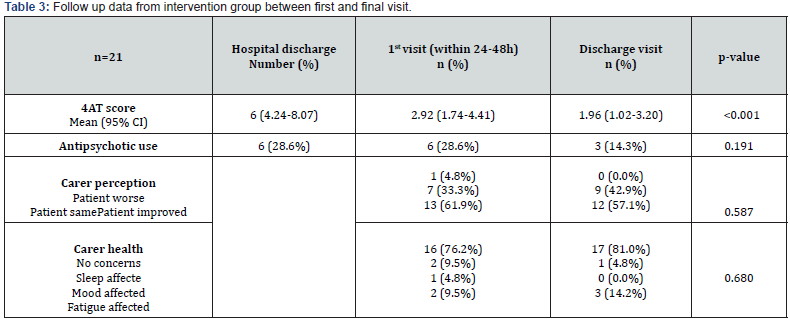
A summary of key outcomes from the intervention group is listed in (Table 3). The mean 4AT score on discharge from hospital was six with a mean period of two days to achieve a 4AT score <4. The mean duration of the ESDD program was 12 days. There was a non-statistically significant reduction in antipsychotic use throughout the ESDD program and no falls were recorded once patients were home. At both the initial and final visit, around 60% of carers felt that the patient was improving in the home environment. Only 5% of carers at the initial visit reported any deterioration in the patient’s behaviour and nil carers reported ongoing deterioration by the final visit. Over 75% of carers at both the initial and final visit did not report any carer stress.
Carer Feedback
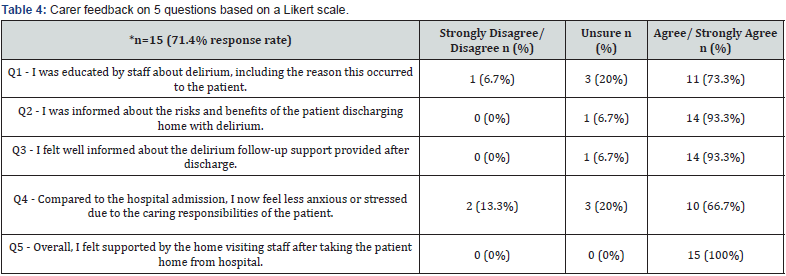
All carers were encouraged to complete the feedback survey at the final visit and 71% responded. The survey responses are summarised in (Table 4). Survey responses were positive overall, with carers reporting they felt educated on delirium and the risks and benefits of an early supported discharge and felt well equipped to look after their family member with delirium.
Cost analysis
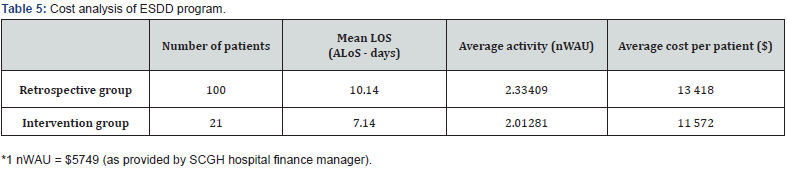
Cost analysis was performed based off the average length of stay (ALoS) for the two groups and the average national weighted activity unit (nWAU) per patient episode. The nWAU is a method of measuring health service activity, to generate a common unit against which the national efficient price (NEP) is paid [18]. The nWAU is weighted for clinical complexity and provides a standardized measure to compare public hospital activity across Australia [18]. The ALoS and nWAU of the retrospective and intervention group are summarized in (Table 5), calculated specifically from the patients included in each group. If 100 patients went through the ESDD program, as compared to the traditional model of care (retrospective group), this would generate an extra $486 000 in revenue (calculation demonstrated in Appendix 2).
Discussion
This is the first study to outline the benefits of an ESDD program over current best practice delirium care, including reduced length of stay without associated harm, high carer acceptability and favorable cost benefits. The three-day reduction in length of stay demonstrates the confidence of the multidisciplinary team in the ESDD service, acknowledging that inpatient care for delirium is likely inferior to the individualized support the ESDD service could provide. While secondary end points were not met, there was notably no increase in readmissions or adverse events such as falls or mortality within the ESDD cohort. Within the ESDD group, the short time to delirium resolution highlights the likely benefits of patients being at home surrounded by family. Importantly, the feasibility of ESDD was dependent on carer acceptance and availability, where our positive carer response has ensured the sustainability of the ESDD program within our hospital.
There is increasing demand for hospital beds across Australian health networks, therefore any innovation which can improve bed flow is worthy of review. Our ESDD study is the first to demonstrate improved bed flow through allowing an almost 50% increase in patients with delirium that could be managed within the same number of hospital bed days on a geriatric ward if discharged with ESDD. The resultant financial benefit for the hospital, with the ability to generate increased nWAU through a greater number of patient episodes, was an important metric in ensuring ESDD’s feasibility and sustainability.
Within the limited literature that currently exists in this area, a unique aspect of our study is the inclusion of the retrospective control group, allowing our ESDD intervention to be compared with current best practice delirium care (e.g., geriatrician-led multidisciplinary team). This therefore gives credibility to the positive results of the ESDD intervention, highlighting the potential influence ESDD programs could have in changing delirium care practices internationally.
A limitation of our study is the small sample size, having recruited only 21 patients to the intervention group. Our project start was delayed due to COVID-19 (March 2020) and recruitment was terminated early due to our acute geriatric ward being closed for extensive renovations. Our intervention numbers however are not dissimilar to the previous Australian study in this area, highlighting the recruitment challenges that come in running such a service amongst older, comorbid patients. A second limitation in our study design is the lack of randomization, introducing the possibility of selection bias. Clinicians and carers made a decision with regard to patient suitability which may result in a highly selected population i.e., exclusion of those less likely to do well. We were also unable to control the bias of a single clinician making a clinical decision off medical notes regarding whether the retrospective cohort would have been eligible for the ESDD program (i.e., observer bias), requiring some assumptions to be made whether the documented carer would have agreed to take on this responsibility. The only way to overcome such bias would be through a randomized control trial, which due to logistical difficulties has not yet been performed in this area internationally. We were reassured however by the extent to which both groups were matched across baseline characteristics, except for an insignificant gender imbalance between groups.
Our study demonstrated that ESDD was effective in significantly reducing length of stay, at the same time as being safe and well received by carers. This has resulted in the hospital continuing to fund and expand the service hospital-wide, where the ESDD program is now available as standard care for all older patients within delirium at Sir Charles Gairdner Hospital.
Conclusion
1. The ESDD program appears to have improved the quality of care delivered to older patients with delirium in an innovative way. Our results are consistent with the limited literature that exists in this field, demonstrating promise for this new model of care. The ESDD program allows patients with delirium to recover in their home environment, simultaneously lessening the burden on an already strained hospital system translating to a favorable cost analysis. The impact of an ESDD program on other delirium outcomes including time to delirium resolution and delirium severity should be further investigated in larger, ideally randomized studies. At this stage however, the novel ESDD model of care offers hope for improving outcomes for patients with delirium, where alternative treatment options remain limited.
References
- Inouye S, Westendorp R, Saczynski J (2014) Delirium in elderly people. Lancet 383(9920): 911-922.
- Marcantonio ER (2017) Delirium in Hospitalized Older Adults. New England Journal of Medicine 377(15): 1456-1466.
- Thein M, Pereira J, Nitchinham A, Caplan G (2020) A call to action for delirium research: Meta-analysis and regression of delirium associated mortality. BMC Geriatrics 20(4): 325.
- Inouye S, Bogardus S, Charpentier P, Leo-Summers L, Holford T, et al. (1999) A Multicomponent Intervention to Prevent Delirium in Hospitalized Older Patients. New England Journal of Medicine 340: 669-676.
- Wang Y, Yue J, Xie D (2019) Effect of the Tailored, Family-Involved Hospital Elder Life Program on Postoperative Delirium and Function in Older Adults: A Randomized Clinical Trial. JAMA Internal Medicine 180(1): 17-25.
- Rosenbloom-Brunton D, Henneman E, Inouye S (2010) Feasibility of Family Participation in a Delirium Prevention Program for Hospitalized Older Adults. Journal of Gerontological Nursing 36(9): 22-33.
- Goldberg A, Straus S, Hamid J, Wong C (2015) Room transfers and the risk of delirium incidence amongst hospitazed elderly medical patients: a case-control study. BMC Geriatrics 15(69).
- McCusker J, Cole M, Abahamowicz M, Han L, Podoba J, et al. (2001) Environmental risk factors for delirium in hospitalized older peopl. J Am Geriat Soc 49(10): 1327-1334.
- Caplan G, Coconis J, Board N, Sayers A, Woods J (2006) Does home treatment affect delirium? A randomised controlled trial of rehabilitation of elderly and care at home or usual treatment (The REACH-OUT trial). Age and Ageing 35(1): 53-60.
- Isaia G, Astengo M, Tibaldi V, Zanocchi M, Benedetta Bardelli, et al. (2009) Delirium in elderly home-treated patients: a prospective study with 6-month follow-up. Age (Dordr) 31(2): 109-117.
- Eeles E, Whiting E, Tattam K, Hay K, Pandy S, et al. (2016) Hospitals in the home for patients with delirium: No place like home. Australasian Medical Journal 9(11): 428-435.
- Chia J, Eeles E, Tattam K, Yerkovich S (2020) Outcomes for patients with delirium receiving hospital-in-the-home treatment: An Australian perspective. Australasian Journal of Ageing 39(2): e215-e219.
- Alrawi Y (2020) Delirium pathway: a North Hampshire experience. Progress in Neurology and Psychiatry 24(3): 26-29.
- Glanville E, Shakespeare K, Laverack S. North Derbyshire Delirium Pathway: Early Supported Discharge and Recovery Programme.
- Bellelli G, Morandi A, Davis D (2014) Validation of the 4AT, a new instrument for rapid delirium screening: a study in 234 hosiptalised older people. Age and Ageing 43(4): 496-502.
- Subramaniam S, Jeffrey A, Soriano R, Divino C (2018) New 5-Factor Modified Frailty Index Using American College of Surgeons NSQIP Data. Journal of American College of Surgery 226(2): 173-181.
- Charlson M, Szatrowski T, Peterson J, Gold J (1994) Validation of a combined comorbidity index. Journal of Clinical Epidemiology 47(11): 1245-1251.
- (2021) Cost weight calculators and episodes of care [Internet]. Melbourne: Victorian Department of Health.






























