Physical and Cognitive Function in the Elderly in a Tertiary Hospital in Lagos: A Comparison between Diabetic and Non-Diabetic Older Patients
Ogbonna Adaobi Nneamaka1*, Akodu Babatunde Abdulmajeed2, Mohammed Ryhanat Bolanle2 and Agunbiade Hussein Taiwo2
1 Family Medicine Department, Lagos University Teaching Hospital, Idi-araba, Lagos
2 Lagos University Teaching Hospital, Idi-araba, Lagos
Submission: June 9, 2023; Published: June 19, 2023
*Corresponding author: Ogbonna Adaobi Nneamaka, Family Medicine Department, Lagos University Teaching Hospital, Idi-araba, Lagos
How to cite this article: Ogbonna Adaobi N, Akodu Babatunde A, Mohammed Ryhanat B, Agunbiade H T . Physical and Cognitive Function in the Elderly in a Tertiary Hospital in Lagos: A Comparison between Diabetic and Non-Diabetic Older Patients. OAJ Gerontol & Geriatric Med. 2023; 7(2): 555709. DOI: 10.19080/OAJGGM.2023.07.555709
Abstract
Background: The elderly, especially those with diabetes are known to have reduced health status which consist of impaired cognitive and physical function. This study compared the physical and cognitive function of elderly diabetic and non-diabetic patients receiving care at the Lagos University teaching hospital, Idi araba, Lagos.
Methods: A cross sectional comparative study involving 126 diabetic (subjects) and 126 age and sex-matched, non-diabetic (control) elderly patients. The sociodemographic characteristics and health status (Physical and cognitive function) was investigated using a semi-structured questionnaire. Physical activity meant engagement in activities beyond daily self-care routine function, active engagement in sports and social groups, while cognition was assessed using the 6-item cognitive impairment score (6-CIT). The proportion of participants involved in physical activities and with impaired cognitive function was estimated in the two study groups. The diabetic and non-diabetic groups were compared using the Chi-square test of proportion. The level of significance was set at p Value <0.05.
Results: Majority of the participants were female (64.3%) in both study groups. The mean age of participants was 65.5±5.7years, 65.3±5.9years and 65.6±5.4years in the total sample, diabetic and non-diabetic groups, respectively. With respect to physical activities 104 (82.5%) and 103 (81.7%) were physically active among the diabetic and non-diabetic elderly respectively, showing no significant difference (χ2 = 0.03; p - 0.869). However, the proportion of participants with normal cognitive function in the non-diabetic group (71.4%) was higher than in the diabetic group (67.4%), with a significant difference (χ2 = 8.56; p - 0.0.014).
Conclusion: Physical activities and normal cognitive function were prevalent among participants in hospital-based study. However, diabetes was significantly associated with impaired cognitive function. Routine assessment of cognitive function is recommended in the holistic management of diabetes, especially among the elderly.
Keywords: Diabetes Mellitus; Non-Diabetics; Cognitive Function; Cognitive Impairment; Physical Activities
Abbreviations: ADA: American Diabetes Association, IDF: International Diabetes Federation, LUTH: Lagos University Teaching Hospital, GOP: General Out-Patient, NHIS: National Health Insurance Scheme, BMI: Body Mass Index, LASUTH: Lagos State University Teaching Hospital, SPSS: Statistical Package for Social Sciences
Introduction
Diabetes mellitus is one of the most common lifelong chronic diseases globally. Its prevalence is on the rise and population aging is a significant driver of this epidemic [1,2]. It is associated with a high number of complications which significantly reduces the quality of life of affected individuals [3]. Diabetes Mellitus is defined by the American Diabetes Association (ADA) as a group of metabolic disorders characterized by hyperglycemia resulting from abnormalities in insulin secretion, insulin action or both [4]. The criteria for diagnosing diabetes by the World Health Organization include fasting plasma glucose ≥ 126 mg/dl (7.0mmol/l) on two consecutive occasions; 2-hour plasma glucose ≥ 200mg/dl (11.1mmol/l) and/or random plasma glucose ≥200 mg/dl (11.1mmol/l) in a patient with classic symptoms of hyperglycemia or hyperglycemic crisis [4,5].
The American Diabetes Association uses the same values as WHO for the diagnosis of diabetes but includes a glycosylated hemoglobin (HbA1c) of ≥ 6.5% [4]. Prevalence of Type 2 diabetes is higher among older adults [6]. This is due to changing lifestyle factors, economic growth in many countries favoring increased caloric consumption and increasing longevity of populations around the world [7,8]. The International Diabetes Federation (IDF), states that the highest prevalence of diabetes is in the older age group between 60 and 79 years [9]. The prevalence of diabetes among adults aged ≥ 65 years in the US varies from 22% to 33% depending on the diagnostic criteria used [1]. Diabetes mellitus is one of the costliest health conditions to manage because of its complications and associations with many geriatric syndromes in the elderly [1,10-12].
The health costs related exclusively to diabetes and its complications exceeded USD 376 billion in 2010 and will reach USD 490 billion in 2030 [13]. Greater than 75% of this estimate is expected to be spent on the healthcare of people aged between 50 and 80 years [14]. Sub-Saharan Africa is estimated to have about 20 million people with diabetes out of which 62.0% are undiagnosed and the number is expected to reach 41.4 million by 2035 [15,16]. In sub-Saharan Africa, Nigeria has the highest number of people with diabetes with an estimated 3.9 million people [15,16]. A study conducted by Balogun and Gureje in Ibadan Nigeria found the incidence of diabetes to be 8.9 per 1,000 person-years [9].
It is well established that chronic hyperglycemia gives rise to the risk of microvascular (retinopathy, nephropathy, and neuropathy) and macrovascular (ischaemic heart disease, stroke, and peripheral vascular disease) damage [15]. Although most focus has been on diabetes causing the aforementioned complications, Diabetes mellitus, its complications, and its treatment can induce transient or permanent cognitive abnormalities [17]. Evidence from cross-sectional and longitudinal studies reveal that individuals with diabetes are at an increased risk for developing cognitive impairment and dementia [18,19].
Cognitive impairment is an emerging new complication of diabetes that requires further study [20]. Several studies, especially of international origin have shown that T2DM can be causally associated with cognitive impairment [20-23]. A European cross-sectional study by Albai et al. showed that 43.0% of people with diabetes had mild cognitive impairment [24]. A population-based South African study by Houle et al. showed that diabetes was associated with lower cognitive scores [25]. Eze et al. in Abakiliki Nigeria found the prevalence of cognitive impairment amongst T2DM patients to be 40.0% [26]. Similarly, a cross-sectional hospital-based study done by Odeigha et al. in North-central Nigeria found the prevalence of cognitive impairment amongst diabetic patients to be 27% with mild cognitive impairment being more prevalent than dementia [27].
Conversely, a systematic review by Sanna et al. showed that there was insufficient evidence to support the effect of T2DM on distinct cognitive ability due to the scarcity of comparable findings [22]. During the aging process, diabetes has also been related to reduced physical activity [12]. Some changes in body composition as individuals age are essential in the development of glucose intolerance and diabetes [12]. The loss of lean mass, its association with reduction of glucose uptake due to reduced insulin action, and increase in visceral fat mass, leading to inflammatory cytokines and hormones secretions that potentiate insulin resistance are physical changes associated with reduced physical activities [12,28].
These changes in body composition, although partly associated with the natural aging process, are augmented by the frequent reduction in physical activity, along with a history of poor eating habits, including a high intake of food with high glycaemic index, despite low calorie needs [12]. However, the ‘Physical Activity Guidelines for Americans’ of the United States Department of Health and Human Services recommends that people aged 65 years and above should engage in at least 150 minutes a week of aerobic physical activity with moderate intensity [29]. This should be spread over at least 3 days a week, not more than 2 days should be spent without exercising [29]. Despite the aforementioned findings, the associations between T2DM and cognitive function, physical activities have not been studied extensively in sub-Saharan Africa where socio-economic, environmental and modifiable risk factors may differ [30,31].
The specific mechanisms underlying cognitive impairment among T2DM patients, remains unknown although several hypothetical mechanisms have been proposed [20]. These include hyperglycemia, hypoglycemia and abnormal insulin action which has also been implicated as aetiology of physical inactivity in elderly diabetics [12,22]. This paucity of studies creates a dearth of knowledge in the physical and cognitive function of diabetic elderly adults in this locality. This study was thus conceived to investigate the relationship between diabetes mellitus and cognitive function, physical activities in the elderly in Lagos, Nigeria. The cognitive and physical function of elderly diabetic patients was compared to that of non-diabetic elderly patients to uncover existing association between cognitive and physical impairment and T2DM in this locality.
Methodology
Study Area: The study was carried out at Lagos University Teaching Hospital (LUTH) situated in Idi- araba in Lagos. Lagos is a metropolitan state located in South-West Nigeria with a population of about 21 million which makes it the largest city in Africa [32]. It is the commercial capital and was an administrative capital of Nigeria. It is a multi-ethnic and urban though the Yorubas constitute the major ethnic group [32]. The Lagos University Teaching Hospital was established in 1962 and has since been involved in the training of both undergraduate and postgraduate medical, dental, and paramedical students. It provides care in the major specialties of medicine to patients within and around Lagos as well as all over Nigeria.The Department of Family Medicine provides health care services to undifferentiated cases. It comprises of three clinics, namely the General out-patient (GOP) clinic, the National health insurance scheme (NHIS) clinic and the Staff clinic. The GOPC serves as a primary care clinic within a tertiary hospital setting and is run by consultant Family Physicians and resident Doctors in Family Medicine, various cadres of Medical Officers and House Officers. The Endocrinology clinic of the Department of Medicine, LUTH offers specialist care to adult diabetic patients.
Study Design: The study was a hospital based comparative cross-sectional study.
Study Population: The study population consisted of elderly diabetic and elderly non-diabetic patients aged 60 years and above attending GOPC and Endocrinology clinic LUTH within the period of study. The selection criteria included consenting elderly diabetic patients diagnosed with DM more than 6 months before the study. Age and sex- matched elderly non-diabetic patients constituted the comparison group. Exclusion criteria included acutely ill patients and any elderly with history suggestive of secondary cause of cognitive impairment (recent head injury, thyroid disease, HIV, ongoing depression, psychoactive substance use and stroke within the past six months), history suggestive of neuropsychiatric illness, delirium and hearing impairment [31,33,34]. Patients with fasting blood glucose of ≥126mg/dl who were not known as diabetic patients were also excluded.
Sample Size Determination: Sample size was calculated using the formula for comparing two proportions shown below: [35]
where n is the minimum sample size in each group, Zα/2 is the standard normal deviate at 95% confidence interval which corresponds to 1.96. Zβ is the power of the test at 80% given as 0.84 and P1 is the proportion of elderly diabetic patients estimated to have cognitive impairment reported as 51.6% in a study by Eze et al in Ebonyi state, south-east Nigeria [26]. P2 is the proportion of elderly non-diabetic patients estimated to have cognitive impairment which was 33.3% in a study conducted in 2019 by Tianyi et al in Cameroun [36]. P1 - P2 is the difference in proportion of events in two groups and P is the pooled prevalence given by (P1+P2)/2. Substitution yielded a minimum sample size of 114 participants per group, which was adjusted for non-response using a non-response rate of 10%. Adjusted sample size was 126 per group. Giving a total of 252 participants in the study.
Sampling Technique: The diabetic and non-diabetic participants were recruited from Endocrinology and General out-patient clinics of LUTH, respectively by systematic random sampling using the daily attendance list to the clinic as the sample frame. The recruitment of diabetic participants was over 3-months. Non-diabetic participants were recruited over 2 months following the period of recruitment of diabetic patients. This was done to ensure that the study groups were appropriately matched for age and sex. Data collection was conducted over a period of five months from October 2020 to February 2021.
Study Instruments: Data was collected using a 5-sectioned, adapted, interviewer-administered questionnaire. The 5 sections of the data collection tool were Section A which assessed socio-demographic characteristic of participants, Section B investigated drug and family history while Section C explored lifestyle characteristics (social and physical activities and tobacco use) of participants. The 6-item CIT was contained in Section D of the questionnaire. Section E captured clinical and laboratory measurements like weight, height, body mass index (BMI), and blood pressure readings. The 6-item cognitive impairment test is a simple 2 - 3 minutes test deployed in the examination of cognition in the elderly. It is made up of 6 items testing concentration and memory [37]. It was scored from 0 - 28. Normal cognition is depicted by scores 0 - 7; mild cognitive impairment is indicated by 8 - 9 points and 10 - 28 suggests severe cognitive impairment [38]. The adapted questionnaire was pretested among 25 patients aged ≥60 years at the General out-patient department of Lagos State University Teaching Hospital (LASUTH) a health facility in Ikeja, capital of Lagos, offering specialized medical services. The pretest helped assess applicability in a tertiary centre, appropriateness, and wording of items on the questionnaire. It also helped to confirm the clarity of the questionnaire.
Data Collection: Before commencement of data collection, 2 research assistants were recruited and trained. They were fresh medical graduates who just completed one mandatory period of internship. Their background medical knowledge, their venepuncture skills and expertise in English and Yoruba language were the basis for the selection. The training lasted 6 hours in two consecutive days (3 hours/day) and covered tips on the objectives, benefits, recruitment, and procedure of the study. Research assistants were trained on politeness, initiating, and establishing a rapport, assuring confidentiality, obtaining an informed consent, ensuring a comfortable and private environment, and administering the questionnaire while ensuring that principles of medical research ethics are not breached. At the commencement of data collection, all clinical staff in the outpatient clinics of LUTH were informed about the study to ensure their cooperation. As patients arrived at the clinics, selection by systematic random sampling was activated after considering each patient for eligibility in the study. Eligible patients were approached, and the study was introduced by explaining the objectives, benefits, and procedure of the study. Patients who consented to participate after asking questions and receiving satisfactory answers on any issue of concerns were recruited into the study.
An informed consent was obtained from each participant, thereafter the questionnaire was administered, and participants’ weight, height, and blood pressure were measured. Seca® weighing scale and stadiometer were used for weight and height measurement respectively. Both were measured to the nearest one decimal place abiding by strict protocols for weight and height measurement [39] Accoson® mercury sphygmomanometer was deployed for blood pressure measurement. Sufficient time of five to ten minutes was allowed for rest. Blood pressure was measured using an appropriately sized cuff in the sitting position with participant’s back supported, feet on the floor, right arm supported, and cubital fossa at heart level. The first (K1) and fifth (K5) phases of Korotkoff sounds were taken as indicative of the systolic and diastolic blood pressures respectively according to WHO specifications and readings were recorded to the nearest 2mmHg. Fasting blood glucose of the diabetic and non-diabetic participants was measured after an overnight fast of 8-10 hours using capillary blood obtained by fingertip pin prick onto a glucometer strip after cleaning with alcohol-soaked swab and pricking with a lancet. This was loaded on an Accu-check Active® glucometer which estimates the blood glucose using the hexokinase method. This served as a screening test for patients assumed to be non-diabetic. A fasting blood sugar of ≥126mg/dl was indicative of DM, and this excluded such participants from the non-diabetic arm of the study [5].
Data Analysis: Data were entered and analyzed on Statistical Package for Social Sciences (SPSS) version 26 after verifying that questionnaires from the data collection exercise were completely and accurately filled out. Questionnaire verification was done by the principal researcher at the end of every data collection exercise. Univariate analysis was done by summarizing categorical variables (socio-demographic characteristics, physical and social activities, and tobacco use) as frequencies and percentages; and continuous variables (age, weight, height, blood pressure etc.) using means and standard deviation. Participants were classified as poor and non-poor using the national poverty line in Nigeria put at 11,456 per capita per month [40]. Participants with a monthly income above the line were classified as non-poor, while those below were seen as poor [40]. Dividing weight in kilogram by square of height in metre squared, body mass index was calculated for all participants. Body mass index < 18.5kg/m2; 18.5 - 24.9kg/m2, 25.0 - 29.9kg/m2 and ≥30.0kg/m2 were categorized as underweight; normal weight, overweight and obese, respectively. Level of cognition was categorized into 3 as normal (0 - 7), mild (8 - 9) and severe cognitive impairment (10 - 28) [37,38]. Bivariate analyses were done using Chi square test of proportion. Fischer exact test was used where one or more cells had an expected frequency less than 5. Categorical variables in the study were compared between the diabetic and non-diabetic group by the Chi-square test. The level of statistical significance was set at pValue <0.05.
Ethical Consideration: The LUTH Health Research and Ethical Committee approved the conduct of the study after due consideration of the objectives and procedure of the study. Each participant at the point of recruitment gave a written informed consent. Participants were assured of confidentiality in all information obtained from them and the questionnaires were safely and securely stored for research purposes only. The completed questionnaires were serially coded with numbers without any links to identifying the participants.
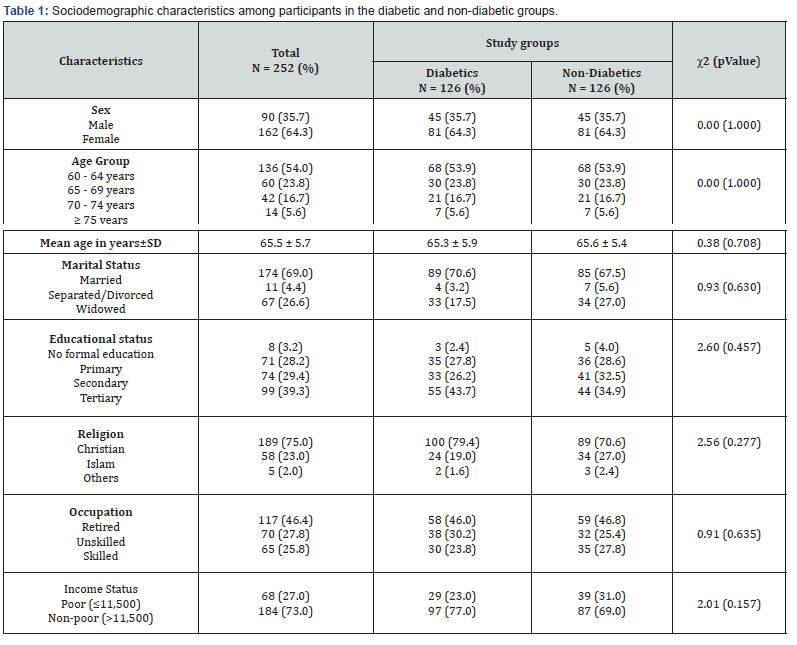
Results: Sociodemographic Characteristics of participants in the diabetics and non-diabetics elderly. (Table 1) shows that gender distribution was 90 male (35.7%) and 162 female participants (64.3%) with a male to female ratio of 1:1.8. The age range of the respondents in both groups was between 60 to 86 years with a mean age of 65.3 ± 5.9years and 65.6 ± 5.4years for the diabetic and non-diabetic participants respectively. In both groups, more than half (53.9%) of the participants were aged 60 - 64years while 30 (23.8%), 21 (16.7%) and 7 (5.6%) were in the age bracket of 65 - 69years, 70 - 74 years and ≥75 years respectively. The diabetic and non-diabetic groups were matched for age and sex, hence there was no difference between the two groups (ꭓ2 = 0.00; p - 1.000). (Table 1) shows that majority of the respondents were married (69.0%), had tertiary education (39.3%) retired (46.6%) and belonged to the Christian faith (75.0%). About three quarters (73.0%) were classified as non-poor using the national poverty line. There was no significant difference in the distribution of participants in the two study groups with respect to educational status (ꭓ2 = 2.60; p - 0.457), marital status (ꭓ2 = 0.93; p - 0.630), occupation (ꭓ2 = 0.91; p - 0.635) and income status (ꭓ2 = 2.01; p - 0.157).
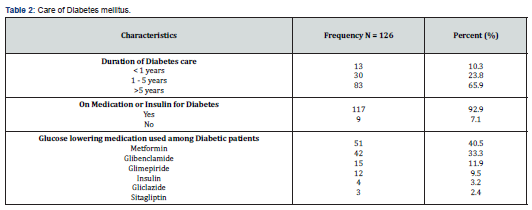
Care of Diabetes mellitus: As presented in (Table 2), More than half (65.9%) of the diabetic participants were diagnosed with diabetes greater than 5 years preceding the study while 30 participants (23.8%) and 13 participants (10.3%) had diabetes for 1 - 5 years and less than one year respectively. Nine out of 10 diabetic participants (92.9%) were on medication for diabetics. Metformin (40.5%), Glibenclamide (33.3%) and Glimepiride (11.9%) were the leading medication used in the management of diabetes mellitus. Slightly less than a tenth (9.5%) were on insulin to achieve good glycaemic control (Table 2) (Figure 1).
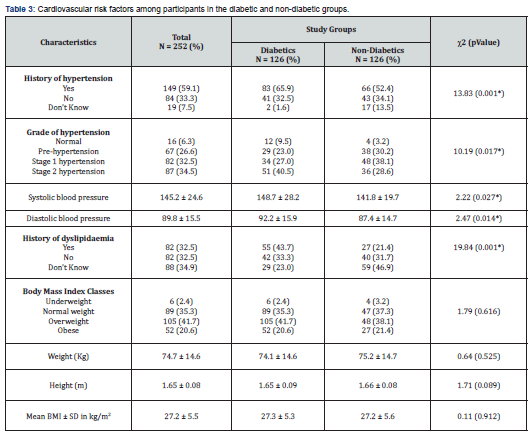
Cardiovascular risk factors among participants in the diabetic and non-diabetic groups: (Table 3) shows that more than half (59.1%) of the participants were known to be hypertensive. While 84 participants (33.3%) did not have history of hypertension, 19 participants (7.5%) were ignorant of their hypertensive status. However, after assessing participants’ blood pressure, about 83 participants (32.9%) had normal blood pressure readings, but 67 (26.6%) were in the pre-hypertension range. Stage 1 and 2 hypertension was found in 32.5% and 34.5% respectively (Table 3). As regards dyslipidemia, 32.5% of the participants had a history of dyslipidemia while 32 (20.6%) and 105 participants (41.7%) were obese and overweight respectively (Table 3). Between the diabetic and non-diabetic groups, the proportion of diabetics with history of hypertension (65.9%) was significantly higher (ꭓ2 = 2.01; p - 0.157) than it was among non-diabetic group (52.4%). Stage 2 hypertension (40.5% Vs 28.5%) was more among the diabetics, while stage 1 hypertension (27.0% Vs 38.1%) was higher in the non-diabetic group, showing statistically significant difference in the distribution of hypertension among the two study groups (Table 3). Furthermore, Table 3 shows that systolic (148.7 ± 28.2mmHg Vs 141.8 ± 19.7mmHg) and diastolic blood pressures (92.2 ± 15.9mmHg Vs 87.4 ± 14.7mmHg) were significantly higher (p < 0.05) in the diabetic group than the non-diabetic group. The mean body mass index of the participants was similar (t-test = 0.11; p - 0.912) in both groups (27.3 ± 5.3kg/m2 Vs 27.2 ± 5.6kg/m2). Other anthropometric parameters were not significantly (p > 0.05) different in the two study groups (Table 3).
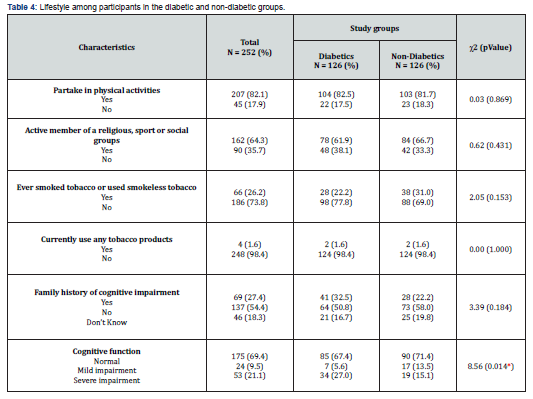
Physical and Cognitive function of Participants in the diabetic and non-diabetic groups: As presented in (Table 4), about four fifths (82.1%) of the participants engaged in physical activity outside daily self-care routine and more than half (64.3%) of the participants were actively involved in religious, sports or social activities. As regards smoking, 66 (26.6%) of the participants had smoked tobacco products while 186 participants (73.4%) had never smoked. Only 4 (1.6%) of the participants were currently smoking (Table 4). Sixty-nine participants (27.4%) reported a family history of cognitive impairment while 30.6% were already experiencing mild (9.5%) to severe (21.1%) cognitive impairment (Table 4). Furthermore, (Table 4) shows that with respects to cognitive function, there was a significant difference (ꭓ2 = 8.56; p - 0.014) between the two groups. The proportion of participants with normal cognitive function (67.4% Vs 71.4%) was higher in the non-diabetic group (71.4%) than the diabetic group (67.4%). Other lifestyle characteristics like partaking in physical activities (ꭓ2 = 0.03; p - 0.869), membership of religious, sports or social groups (ꭓ2 = 0.62; p - 0.431) etc. were similar between the 2 groups (Table 4).
Discussion
This study compared the health status of diabetic and non-diabetic elderly patients accessing care at outpatient clinics in LUTH with respect to cardiovascular risk, physical and social activities, and cognitive function. The participants were matched according to age and gender to limit the effect of these characteristics on the health status of diabetes and non-diabetes elderly patients. Participants’ engagement in physical (82.1%) and social activities (64.3%) was high in this study. There was also no significant difference between the elderly diabetic and the non-diabetic participants in this regard.
The proportion of participants that engaged in physical activities was reportedly lower in studies by Al-Hamdan in Saudi Arabia (46.1%), and Sibai et al in Lebanon (10.0 - 23.4%) [41,42]. The Saudi Arabian and Lebanon studies showed additional difference from the index study as they both reported a significantly lower physical activity among diabetic participants [41,42]. However, Ahmad et al reported similar proportion of participants’ engagement in physical activities among diabetic and non-diabetic patients, though more vigorous exercises were reported among non-diabetic participants [43]. These varying findings may not be unrelated to the different study settings of these studies, while the index study is a hospital-based study, the Arabian, Lebanon, and Japan studies were community-based studies [41-43].
One of the cardinal strategies in managing elderly patients is to emphasis lifestyle modification that encourage physical activities, this may have accounted for the very high prevalence of physical activities among participants in the index study which is a hospital-based study. There is a growing recognition that physical activities form the foundation for lifestyle modification aimed at averting and managing T2DM and its related complications [44]. Regular physical activities improve the health status of the elderly diabetics and non-diabetics alike [45]. and significantly lessen the risk of cardiovascular diseases [46,47]. Among the elderly, those with diabetes in particular, physical activities have been shown to improve glycaemic control through increased insulin sensitivity and glucose tolerance [1].
There are two main types of exercise, the resistance training and aerobic exercises, both contribute to the health-related components of physical fitness by modifying body composition, improving cardiorespiratory resistance, muscular strength and resistance [12,14,48]. Physical activities outside daily self-care routine should be engaged cautiously and under expert guidance to maximize its benefits among the elderly, especially older adults with T2DM because they are prone to falls resulting from lower limb dysfunction, impaired balance and the effect of polypharmacy [44]. Therefore, exercises tailored to suit each patient’s peculiarities should be encouraged whenever possible [12,44]. Also, physical activity programs despite the benefits of glycaemic control should be viewed as a good means of promoting functional independence among the elderly [12,44].
The prevalence of cognitive impairment in the diabetic elderly participants was 32.6% where 5.6% had MCI and 27.0% had SCI. The prevalence of cognitive impairment in the non-diabetic participants was 28.6% with 13.5% and 15.1% participants having MCI and SCI respectively. Impaired cognitive function was significantly higher among elderly diabetics than elderly non-diabetics. This adds to the growing evidence from previous studies that diabetes mellitus is significantly associated with cognitive impairment [21,26,31,49,50]. Yusuf et al and Yarube et al. in different comparative studies among diabetic and non-diabetic patients in northern Nigeria found a significant association between DM and cognitive impairment [31,51].
In an Ethiopian study by Baye et al, cognitive impairment was also significantly higher among T2DM patients compared to the non-diabetic study participants [52]. Studies in other parts of the world which showed similar findings include prospective studies by Rawlings et al., Wessel et al., Marseglia et al. and Formiga et al. where diabetes was found to be independently associated with accelerated cognitive decline [23,53-55]. A systematic review by Sanna et al. also found a significant decline in cognition among older adults who had T2DM similar to our study [22]. The mechanism leading to cognitive decline in the T2DM patients have been identified to include hyperinsulinaemia, advanced glycosylated end products, Lipoprotein related proteins, the effect of brain infarct and white matter disease [56].
These mechanisms are purportedly responsible for a twofold increase in the likelihood of cognitive decline in T2DM patients over their non-diabetic counterparts. Diabetes mellitus has also been linked with accumulation of beta amyloid caused by increased deposition and reduced clearance [12]. Additionally, impaired glycemic control with recurrent episodes of hypo- or hyperglycemia contributes to microangiopathy, neuronal loss, and ultimately cognitive impairment [12,52,54]. Some studies however did not find a significant association between cognitive function and Diabetes. Tiwari et al. in an Indian study reported a non-significant association between diabetes and cognitive function and therefore concluded that there was a weak relationship between diabetes and cognitive impairment amongst urban older adults [50].
The disparity between the index study and that by Tiwari et al. could be due to the difference in geographical locations of both studies. The hospital-based design of this study as opposed to the population-based design by Tiwari et al. could also be another reason for this disparity [50]. Other cross-sectional studies conducted in Malaysia by Momtaz et al and in China by Li et al amongst elderly adults (60 years or older) found that diabetes was not statistically associated with cognitive function [57,58]. These studies were also population-based studies like the Indian study by Tiwari et al [50,57,58].
Population studies gives access to variety of cases and the proportion of diabetic patients with complications might not be as high as researchers would find in a hospital-based study like ours, hence the relationship between impaired cognitive function and diabetes may not be obvious. Li et al therefore opined that diabetes might be an adjunctive risk factor for MCI [58]. In managing elderly diabetic patients, cognitive function should be assessed regularly to facilitate early detection of a decline and institution of preventive measures. The study was not without its limitations.
The hospital-based design may have affected the rating of the health status of elderly in this locality. Patients receiving care in facilities like ours, especially those on long term follow-up, may be more informed and knowledgeable about healthy lifestyle tips and thus their health status as reported in our study may not be a true reflection of health status of elderly in our communities. Notwithstanding, this study was able to demonstrate the effect of diabetes on physical activities and cognitive function in the elderly because of its comparative design and matching of participants for age and sex. Secondly, being a cross sectional study limited the conclusion of a causal relationship between diabetes mellitus and cognitive function in the elderly.
In conclusion, despite its limitations, the study showed that impaired cognitive function was high among the elderly in this locality, and significantly higher among diabetic elderly patients than their non-diabetic counterparts. Physical activity was also found to be prevalent among the elderly patients in the study, however, there was no significant difference between the diabetic and non-diabetic groups. Attention should be paid to the assessment of cognitive function in the care of the elderly, especially among elderly diabetic patients for early detection and prevention of decline in cognitive function.
- Kirkman MS, Briscoe VJ, Clark N, Florez H, Haas LB, et al. (2012) Diabetes in older adults. Diabetes Care 35(12): 2650-2664.
- Yakaryılmaz FD, Öztürk ZA (2017) Treatment of type 2 diabetes mellitus in the elderly. World J Diabetes 8(6): 278-285.
- Saedi E, Gheini MR, Faiz F, Arami MA (2016) Diabetes mellitus and cognitive impairments. World J Diabetes 7(17): 412-422.
- (2012) Diagnosis and Classification of Diabetes Mellitus. Diabetes Care.
- (2019) World Health Organization: Definition and Diagnosis of Diabetes Mellitus and Intermediate Hyperglycemia.
- Mayeda ER, Haan MN, Kanaya AM, Yaffe K, Neuhaus J (2013) Type 2 Diabetes and 10-Year Risk of Dementia and Cognitive Impairment Among Older Mexican Americans. Diabetes Care 36(9): 2600-2606.
- Ley SH, Hamdy O, Mohan V, Hu FB (2014) Prevention and management of type 2 diabetes: dietary components and nutritional strategies. The Lancet 383(9933): 1999-2007.
- Biessels GJ, Despa F (2018) Cognitive decline and dementia in diabetes mellitus: mechanisms and clinical implications. Nat Rev Endocrinol 14(10): 591-604.
- Balogun WO, Gureje O (2013) Self-Reported Incident Type 2 Diabetes in the Ibadan Study of Ageing: Relationship with Urban Residence and Socioeconomic Status. Gerontology 59(1): 3-7.
- Mollentze WF (2010) Management of diabetes in the elderly. The care of diabetes in the elderly may be different from that in younger patients 28: 480-483.
- Lipscombe LL, Hux JE (2007) Trends in diabetes prevalence, incidence, and mortality in Ontario, Canada 1995–2005: a population-based study. Lancet 369: 750-756.
- Ferriolli E, Pessanha FP, Marchesi JC (2014) Diabetes and exercise in the elderly. Diabetes and physical activity 60: 122-129.
- Zhang P, Zhang X, Brown J, Vistisen D, Sicree R, et al. (2010) Global healthcare expenditure on diabetes for 2010 and 2030. Diabetes Res Clin Pract 87(3): 293-301.
- Hodge AM, Flicker L, O’dea K, English DR, Giles GG (2013) Diabetes and ageing in the Melbourne Collaborative Cohort Study (MCCS). Diabetes Res Clin Pract 100(3): 398-403.
- Chinenye S, Young E (2011) Care of diabetes in Nigeria. A Review. Niger Heal J 11(4): 101-106.
- Dahiru T, Aliyu A, Shehu A (2016) A review of population-based studies on diabetes mellitus in Nigeria. Sub-Saharan African J Med 3(2): 59-64.
- McCrimmon RJ, Ryan CM, Frier BM (2012) Diabetes and cognitive dysfunction. Lancet 379(9833): 2291-2299.
- Baumgart M, Snyder HM, Carrillo MC, Fazio S, Kim H, et al. (2015) Summary of the evidence on modifiable risk factors for cognitive decline and dementia: A population-based perspective. Alzheimer’s Dement 11(6): 718-726.
- Rizzi L, Rosset I, Roriz-Cruz M (2014) Global Epidemiology of Dementia: Alzheimer’s and Vascular Types. Biomed Res Int. 2014: 1-8.
- Umegaki H (2014) Type 2 diabetes as a risk factor for cognitive impairment: current insights. Clin Interv Aging 9: 1011-1019.
- Cheng G, Huang C, Deng H, Wang H (2012) Diabetes as a risk factor for dementia and mild cognitive impairment: a meta-analysis of longitudinal studies. Intern Med J 42(5): 484-491.
- Papunen S, Mustakallio-Könönen A, Auvinen J, Timonen M, Keinänen-Kiukaanniemi S, et al. (2020) The association between diabetes and cognitive changes during aging. Scand J Prim Health Care 38(3): 281-290.
- Wessels AM, Lane KA, Gao S, Hall KS, Unverzagt FW, et al. (2011) Diabetes and cognitive decline in elderly African Americans: A 15-year follow-up study. Alzheimer’s Dement 7(4): 418-424.
- Albai O, Frandes M, Timar R, Roman D, Timar B (2019) Risk factors for developing dementia in type 2 diabetes mellitus patients with mild cognitive impairment. Neuropsychiatr Dis Treat 15: 167-175.
- Houle B, Gaziano T, Farrell M, Gómez-Olivé FX, Kobayashi LC, et al. (2019) Cognitive function and cardiometabolic disease risk factors in rural South Africa: Baseline evidence from the HAALSI study. BMC Public Health 19(1): 1-11.
- Eze CO, Ezeokpo BC, Kalu UA, Onwuekwe IO (2015) The Prevalence of Cognitive Impairment amongst Type 2 Diabetes Mellitus Patients at Abakaliki South-East Nigeria. J Metab Syndr 04(01): 1-3.
- Lo O, Su R, Oligbu P, Okeke K (2020) Cognitive Impairment in Patients with Type 2 Diabetes Mellitus in a Primary Care Setting of a Tertiary Hospital in North Central 1(3): 1-6.
- Hawthorne G (2011) Diabetes, the glycaemic index and older people. Age and ageing 40(6): 655-656.
- (2008) US Department of Health and Human Services. Physical activity guidelines for Americans: be active, healthy, and happy!
- Guerchet M, Mouanga AM, M’belesso P, Tabo A, Bandzouzi B, et al. (2012) Factors Associated with Dementia Among Elderly People Living in Two Cities in Central Africa: The EDAC Multicenter Study. J Alzheimer’s Dis 29(1): 15-24.
- Yusuf AJ, Baiyewu O, Bakari AG, Garko SB, Jibril ME-B, et al. (2018) Low education and lack of spousal relationship are associated with dementia in older adults with diabetes mellitus in Nigeria. Psychogeriatrics 18(3): 216-223.
- (2020) Lagos Population 2020 (Demographics, Maps, Graphs). World Population Review.
- Sakusic A, O’Horo JC, Dziadzko M, Volha D, Ali R, et al. (2018) Potentially Modifiable Risk Factors for Long-Term Cognitive Impairment After Critical Illness: A Systematic Review. Mayo Clin Proc 93(1): 68-82.
- (2019) World Health Organization. Risk reduction of cognitive decline and dementia: WHO guidelines.
- Adebiyi AO, Ogunniyi A, Adediran BA, Olakehinde OO, Siwoku AA (2015) Cognitive Impairment Among the Aging Population in a Community in Southwest Nigeria. Heal Educ Behav 43(1): 93S-99.
- Corriere M, Rooparinesingh N, Kalyani RR (2013) Epidemiology of Diabetes and Diabetes Complications in the Elderly: An Emerging Public Health Burden. Curr Diab Rep 13(6): 805-813.
- Ogunrin AO (2014) Effect of Vinpocetine (CognitolTM) on Cognitive Performances of a Nigerian Population. Ann Med Health Sci Res 4(4): 654-661.
- (2019) Six Item Cognitive Impairment Test (6CIT).
- (2020) Nutrition Screening as as A guide to completing the Mini Nutritional Assessment (MNA ®).
- (2018) Nigerian Bureau of Statistics. NBS 2019 Poverty and Inequality in Nigeria: Executive Summary. Natl Bur Stat.
- Al-Hamdan N, Bahnassy A, Saeed A, Abbas M, Abuzaid L, et al. (2010) Comparison of physical activity patterns among diabetic and non-diabetic adults in Saudi Arabia. Journal of High Institute of Public Health 40(3): 424-435.
- Sibai AM, Costanian C, Tohme R, Assaad S, Hwalla N (2013) Physical activity in adults with and without diabetes: from the ‘high-risk’approach to the ‘population-based’approach of prevention. BMC public health 13(1): 1-8.
- Ahmad I, Aung MN, Ueno S, Khin ET, Latt TS, et al. (2021) Physical activity of type 2 diabetes mellitus patients and non-diabetes participants in yangon, myanmar: A case-control study applying the international physical activity questionnaires (IPAQ-S). Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy 14: 1729-1739.
- Sinclair AJ, Conroy SP, Bayer AJ (2008) Impact of diabetes on physical function in older people. Diabetes care 31(2): 233-235.
- Luke A, Dugas LR, Durazo-Arvizu RA, Cao G, Cooper RS (2011) Assessing physical activity and its relationship to cardiovascular risk factors: NHANES 2003-2006. BMC Public Health 11(1): 1-1.
- Kohl HW, Craig CL, Lambert EV, Shigeru Inoue, Jasem Ramadan Alkandari, et al. (2012) The pandemic of physical inactivity: global action for public health. Lancet 380(9838): 294-305.
- Xu Y, Wang L, He J, Yufang Bi, Mian Li, et al. (2013) Prevalence and control of diabetes in Chinese adults. JAMA 310(9): 948-959.
- Otterman NM, Van Schie CH, Van Der Schaaf M, Van Bon AC, Busch-West broek TE, et al. (2011) An exercise pro gramme for patients with diabetic com plications: a study on feasibility and preliminary effectiveness. Diabet Med 28(2): 212-217.
- Jia L, Du Y, Chu L, Zhang Z, Li F, et al. (2020) Prevalence, risk factors, and management of dementia and mild cognitive impairment in adults aged 60 years or older in China: a cross-sectional study. Lancet Public Heal 5(12): 661-671.
- Tiwari SC, Tripathi RK, Farooqi SA, Kumar R, Srivastava G, et al. (2012) Diabetes mellitus: A risk factor for cognitive impairment amongst urban older adults. Industrial Psychiatry Journal 21(1): 44-48.
- Yarube IU, Mukhtar IG (2018) Impaired cognition and normal cardiometabolic parameters in patients with type 2 diabetes in Kano, Nigeria. Sub-Saharan Afr J Med 5(2): 37-44.
- Baye D, Amare DW, Andualem M (2017) Cognitive impairment among type 2 diabetes mellitus patients at Jimma University Specialized Hospital, Southwest Ethiopia. J Public Heal Epidemiol 9(11): 300-308.
- Rawlings AM, Sharrett AR, Albert MS, Coresh J, Windham BG, et al. (2019) The association of late-life diabetes status and hyperglycemia with incident mild cognitive impairment and dementia: The ARIC study. Diabetes Care 42(7): 1248-1264.
- Marseglia A, Fratiglioni L, Kalpouzos G, Wang R, Bäckman L, et al. (2019) Prediabetes and diabetes accelerate cognitive decline and predict microvascular lesions: A population-based cohort study. Alzheimer’s Dement 15(1): 25-33.
- Formiga F, Ferrer A, Padrós G, Corbella X, Cos L, et al. (2014) Diabetes Mellitus as a Risk Factor for Functional and Cognitive Decline in Very Old People: The Octabaix Study. J Am Med Dir Assoc.
- Luchsinger JA (2012) Type 2 diabetes and cognitive impairment: linking mechanisms. Journal of Alzheimer's Disease 30(s2): S185-S198.
- Momtaz YA, Hamid TA, Bagat MF, Hazrati M (2019) The Association Between Diabetes and Cognitive Function in Later Life. Curr Aging Sci 12(1): 62-66.
- Li W, Sun L, Li G, Xiao S (2019) Prevalence, influence factors and cognitive characteristics of mild cognitive impairment in type 2 diabetes mellitus. Frontiers in aging neuroscience 11: 180.






























