A Study to Assess the Safety of Anticholinergic Drugs in the Indian Elderly Patients: A Retrospective Analysis
Pramil Tiwari* and Durgeshwari
Department of Pharmacy Practice, National Institute of Pharmaceutical Education and Research (NIPER), S.A.S. Nagar, Punjab, India
Submission: April 21, 2023; Published: May 01, 2023
*Corresponding author: Pramil Tiwari, Prof. & Head, Department of Pharmacy Practice, National Institute of Pharmaceutical Education and Research (NIPER), Punjab, India
How to cite this article: Pramil T, Durgeshwari. A Study to Assess the Safety of Anticholinergic Drugs in the Indian Elderly Patients: A Retrospective Analysis. OAJ Gerontol & Geriatric Med. 2023; 7(2): 555707. DOI: 10.19080/OAJGGM.2023.07.555707
Abstract
Background- It is estimated that by 2050, about 22% of the population will be over 60 years of age. And, across the geographies, the elderly population is the largest per capita medication consumers, especially the oldest old. Poorer physical performance falls, cognitive decline and death in the elderly are all related to a higher anticholinergic drug burden. Aim: To determine the anticholinergic burden in the elderly by using Drug Burden Index (DBI) Anticholinergic Risk Scale (ARS) and Anticholinergic Cognitive Burden (ACB) scale. Methodology:A retrospective observational study was carried out from the database in an inpatient setting of a public teaching hospital. The analysis of 411 elderly patients’ data, out of the pool of 564, forms the basis of this work. The parameters recorded were age, gender, comorbidities, and the total number of drugs prescribed. Analysis of the anticholinergic drugs prescribed was the backbone of the work. Results: Of the 411 patients, 170 were females and 241 (41.4% & 58.6%) were males. The mean (SD) age of patients was 70.46yrs (7.02) Patients were grouped into three classes viz. 60-69 yrs, 70-79 yrs, 80-89 yrs, and 90-99yrs. Almost half of the patients belonged to the 60-69yr group. Conclusion: The scores from the Drug Burden Index (DBI), Anticholinergic Risk Scale (ARS), and Anticholinergic Cognitive Burden (ACB) scales are closely linked to the health outcomes of elderly individuals, and they need to be used as a tool for deprescribing in the elderly. Prescribing to elderly also needs to focus on the patient specific factors.
Keywords: Elderly; DBI; ACB; ARS; Retrospective; Anticholinergic Burden; Sedative Drugs
Abbreviations: DBI: Drug Burden Index; ARS: Anticholinergic Risk Scale; ACB: Anticholinergic Cognitive Burden; SPSS: Statistical Package for the Social Sciences; SD: Mean
Introduction
Increase in the life expectancy in society implies that a larger proportion of population requires attention to address the including physiological, pathological, psychological, economic, and sociological problems. [1] According to an estimate, 14% of India’s population would be beyond the age of 60 by 2030. Moreover, the UN Population Fund predicts that this number will rise to 19.4% by 2050. [2] For the better quality of life of the patients, the appropriate use of the drug is an essential component. Ensuring the safe use of medications in elderly patients is indeed important due to the fact that multiple drugs are prescribed or often self-medicated.
Prescribing medications for older adults can be a challenging task as factors such as changes in body composition, physiology, altered pharmacokinetics, and altered pharmacodynamics must be considered [3,4]. These factors make it necessary to approach medication management in the elderly population with caution to prevent adverse reactions and ensure optimal therapeutic outcomes [5]. Older adults are at a higher risk of experiencing adverse effects from medications because of multiple illnesses.
Studies indicate that medications with anticholinergic properties can lead to negative outcomes such as cognitive impairment, delirium, falls, and difficulty in movement. Anticholinergic drugs are linked to impaired physical performance and functional status among the oldest subjects [6,7]. The aim of this study is to determine Anticholinergic burden using three different scales i.e., DBI (Drug Burden Index), ACB (Anticholinergic Cognitive Burden Scale), ARS (Anticholinergic Risk Scale) and to list down some drugs that are repetitively used and have high Anticholinergic Burden.
Method
The data retrieval was done from an existing database of 1000 case record forms. On screening, 564 were found to be elderly patients (over 60 years of age). 411 patients’ data out of this pool of 564 was analyzed for Drug Burden Index.
Study Design and Sample: A retrospective observational study was carried out from the database in an inpatient setting of a public teaching hospital. All patients with the age 60 years or above and who had at least one anticholinergic drug and sedative drug property in their prescription were included.
Data Collection: Each record was serially checked for Anticholinergic drug burden using three different scales i.e., Drug Burden Index (DBI), Anticholinergic Cognitive Burden Scale (ACB), Anticholinergic Risk scale (ARS). The DBI, ACB, and ARS were calculated for each drug individually; and, these parameters were checked on the individual drug as well for whole 411 patients. Some other details like demographic details, total no. of drugs (polypharmacy), and comorbidities were also collected from these case record forms.
Data Analysis: The results were represented as average supported by standard deviation, percentages, as considered appropriate. Statistical significance was determined at 95% level of confidence. The parameters recorded were age, total number of drugs, gender, comorbidities, and anticholinergic drug prescribed. The data was analyzed using statistical package for the social sciences (SPSS), Version 20. The scores for calculating Anticholinergic Burden were DBI, ACB and ARS. DBI is a validated risk assessment scale that is used to estimate cumulative exposure to anticholinergic and sedative drugs. DBI helps with the dose-related measurement of each drug. The calculation was carried out by the web portal software program “Anticholinergic Burden Calculator” (www.anticholinergicscales. es/) [8]. The Anticholinergic Cognitive Burden (ACB) scale is used for determining the severity of anticholinergic drugs on cognition caused by prescribed medications. It gives a score of 0, 1, 2 & 3 which reflects the cumulative anticholinergic cognitive burden caused by the medication elderly patients take [9]. The Anticholinergic Risk Score (ARS) is an essential tool for determining the degree to which a certain patient may be at risk of an adverse anticholinergic impact that can cause cognitive dysfunction and delirium. It uses scores that range from 0-3 [10].
Results
This study has analyzed records of 411 patients, out of the pool of 564 who were 60 years of age or more. The baseline characteristics of the sample are shown in (Table 1). Of the total sample studied, 170 were females and 241 were males (41.4% & 58.6%), respectively. The mean age of patients was 70.46±7.02years. Patients were grouped into three classes viz. 60-69yrs, 70-79yrs, 80-89yrs, and 90-99yrs. Almost half of the patients belonged to the 60-69yr group. Further, the patients were categorized on the basis of the number of co-morbidities. 372 patients had at least 3 comorbidities and only 39 patients had more than 3 comorbidities.

The average number of drugs prescribed was found to be 5.20±2.50. Patients were also classified based upon the number of drugs prescribed. The patients who were prescribed 5 drugs or less were 257(62.5%); 141(34.3%) with 6-10 drugs prescribed and 13(3.16%) had more than 10 drugs prescribed. And, 35% of the prescribed drugs (749 in number) had anticholinergics & sedative properties. The top five drugs prescribed were Tramadol (76 times), Rantidine (66 times), Pregabalin (41 times), Alprazolam (29 times) and Levetriacetam (76 times).
DBI Score: In this study, the total DBI score of 749 drugs in 411 patients was found to be 117.5; and, the mean was 0.15±0.23. With respect to drug exposure, 35% of drugs had anticholinergic activity (including sedative effects as well). After computing the Drug Burden Index, the results were classified into four groups based upon the DBI score as follows:
0-1, where 0 (reference group with 209 patients),
Low: 0 to less than 0.20 (n=1 patient),
Moderate: 0.20 to less than 0.50 (n=80 patients),
High: 0.50 to less than 1.0 (n=97 patients), and
Very High: 1.0 or more (n=24 patients).
An attempt was also made to correlate gender and comorbidity with the DBI. It was found that females had a higher DBI compared to male patients. Further, as the number of comorbidities increased, DBI also increased. The relationship was statistically insignificant, though.
ACB Score: The total ACB score of 749 drugs in 411 patients was found to be 273 with a mean of 0.66±0.79. The drugs with Anticholinergic Cognitive Burden (ACB) Scale with a score of 0 (n = 200 patients), a score of 1 (n = 167 patients), a score of 2 (n = 30 patients), and a score of 3 (n = 14 patients). After performing multiple linear regression analysis, female patients in this study were found to have a higher impact on cognition than males; and, the Anticholinergic Burden Scale score is higher in females. Comorbidity and ACB are associated with each other statistically and the relationship are statistically insignificant. As comorbidity increased, the ACB score also increased leading to an impact on cognition in patients.
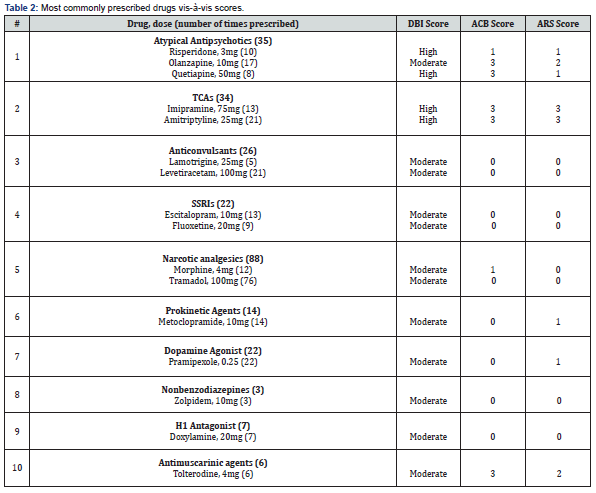
ARS Score: The total ARS score of 749 drugs in 411 patients was found to be 116 with a mean of 0.28±0.60. The patients with an ARS score 0 (n = 318), score 1 (n = 79), score 2 (n = 6), and score 3 (n = 8). After multiple linear regression analysis, ARS and gender were not associated that much with each other. Comorbidity and ARS were found to be associated with each other in a statistically significant way as comorbidity increases the ARS score is also increasing. Higher ARS scores are related to a statistically higher risk of peripheral and central adverse effects from anticholinergics drugs. The DBI, ACB and ARS score of 257 different drugs prescribed in this study (classified in 10 categories) is given in (Table 2).
Kimia and co-workers have reported that among the 1532 elderly people with an average age of 69.21 years, 29% had DBI>0 [11]. In contrast, in this study almost half of the patients had a DBI score of more than zero. Possibly, this can be improved when the results are fed back to the prescribers. Atypical antipsychotics, TCAs and antimuscarinics have the highest ACB score in our study and Lisa and co-workers in one of the studies stated that antipsychotics, antidepressants, opioid analgesics, and other drugs acting on the central nervous system can cause sedation, delirium, and impaired functional and cognitive status [12]. Rudolph and coworkers report that a single medication with an ARS score of 3 would likely cause 2 or more anticholinergic adverse effects in more than 70% of the patients.
However, in this study, only 8 patients had an ARS score of 3 [10]. It implies that the patients in this study were less likely to face anticholinergic side effects. These findings are pilot in terms of understanding the likely anticholinergic side effects in the elderly inpatients. It is equally likely that the response of the drugs in focus of this study could elicit atypical responses in the elderly. Hence, the patient specific factors also need to be considered before generalizing/ applying these results in clinical settings.
References
- Andres TM, McGrane T, McEvoy MD, Allen BFS (2019) Geriatric Pharmacology: An Update. Anesthesiol Clin 37(3): 475-492.
- (2023) Policy Watch- National Policy for Senior Citizens - Insightsias.
- Cardwell K, Kerse N, Ryan C, Teh R, Moyes SA, et al. (2020) The Association Between Drug Burden Index (DBI) and Health-Related Outcomes: A Longitudinal Study of the 'Oldest Old' (LiLACS NZ). Drugs Aging 37(3): 205-213.
- Kashyap M, D'Cruz S, Sachdev A, Tiwari P (2015) Evidence-based information leads to reduction in inappropriate drug prescribing: Results from Indian older inpatients. Int J Risk Saf Med 27(4): 209-217.
- Dauphinot V, Faure R, Omrani S, Goutelle S, Bourguignon L, et al. (2014) Exposure to anticholinergic and sedative drugs, risk of falls, and mortality: an elderly inpatient, multicenter cohort. J Clin Psychopharmacol 34(5): 565-570.
- Jaffuel M, Gervais F, Vernaudon J, Cerfon MA, Krolak-Salmon P, et al. (2023) Potentially inappropriate medications and anticholinergic and sedative burden in older community-dwelling patients with advanced chronic kidney disease. Nephrol Ther 19(1): 1-10.
- Care AB (2012) Anticholinergic cognitive burden Scale-2012 update.
- Villalba-Moreno Á, Alfaro-Lara ER, Sánchez-Fidalgo S, Nieto-Martín MD, Santos-Ramos B (2017) Development of the anticholinergic burden calculator web tool. Farmacia Hospitalaria 41(5): 647-648.
- Boustani M, Campbell N, Munger S, Maidment I, Fox C (2008) Impact of anticholinergics on the aging brain: a review and practical application.
- Rudolph JL, Salow MJ, Angelini MC, McGlinchey RE (2008) The anticholinergic risk scale and anticholinergic adverse effects in older persons. Arch Intern Med 168(5): 508-513.
- Raei K, Rahimi A, Hosseini SR, Moghadamnia AA, Bijani A (2021) Anticholinergic drug use in elderly people: A population- based study in Iran. Caspian J Intern Med 12(4): 593-599.
- Kouladjian L, Gnjidic D, Chen TF, Mangoni AA, Hilmer SN (2014) Drug Burden Index in older adults: theoretical and practical issues. Clin Interv Aging 9: 1503-1515.






























