Comparing Health Status and Access to Preventive Healthcare in Persons with Severe Intellectual and Developmental Disabilities by Age
Kayla Kostal1, Margherita Cameranesi1, Lindsay McCombe2, Maria Baranowski1, Jenna Heschuk2 and Shahin Shooshtari1,2*
1Rady Faculty of Health Sciences, University of Manitoba, Winnipeg, Canada
2St. Amant Research Centre, Winnipeg, Canada
Submission: June 24, 2022; Published: July 26, 2022
*Corresponding author: Dr. Shahin Shooshtari, Department of Community Health Sciences, Rady Faculty of Health Sciences University of Manitoba, Winnipeg, Canada
How to cite this article: Kostal., K., Cameranesi, M., McCombe, L., Baranowski, M., Heschuk, J., Shooshtari, S. Comparing Health Status and Access to Preventive Healthcare in Persons with Severe Intellectual and Developmental Disabilities by Age. OAJ Gerontol & Geriatric Med. 2022; 6(5): 555697. DOI: 10.19080/OAJGGM.2022.06.555697
Keywords: Intellectual disabilities; Developmental disabilities; Deinstitutionalization; Community transitions; Ageing; Health status; Older adults; Sociodemographic characteristics.
Introduction
Persons with intellectual and developmental disabilities (IDD) have higher rates of morbidity and premature mortality compared to those without IDD [1-4]. Persons with severe IDD experience complex aging and have a shorter lifespan compared to the general population [1]. As a group, persons with IDD encounter more challenges in receiving adequate healthcare [1], and therefore are more likely than the general population, or even those with other types of disabilities to report unmet healthcare and social service needs [5]. There has been limited research examining health status and access to preventive healthcare in persons aging with severe IDD. The objective of the present study was to describe health status and access to preventive healthcare for older adults with severe IDD (i.e., those aged 45 and over) compared to younger adults (i.e., younger than age 45) with severe IDD living in Manitoba, Canada.
Methods
A longitudinal, mixed-methods study was implemented in 2016 to examine the process and outcomes of deinstitutionalization for persons with severe IDD in the Canadian province of Manitoba. The examination of changes in health status and access to preventive healthcare in the study group was one component of this longitudinal study. pre-transition and post-transition health data were collected through medical chart review and a health assessment tool, the Comprehensive Health Assessment Program (CHAP), which is a standardized tool used to enhance access to primary healthcare for persons with IDD [6]. CHAP:
The CHAP includes two sections measuring the health status and access to healthcare of the person being assessed; section 1 is completed by a caregiver; section 2 by a primary care provider. A supplementary form was also completed by a nurse.
Data were collected for 52 persons with severe IDD while living in a complex care facility, St.Amant Health and Transition Services (Winnipeg, Manitoba), prior to their transition to community living. A previous paper [7] described the baseline (pre-transition) health status of this study cohort. For the purposes of this paper, we conducted secondary data analysis using SPSS version. Descriptive statistics were calculated to describe the sociodemographic characteristics of the study cohort and to compare their health status and access to healthcare by age .
Results
Of the 52 persons with severe IDD, 32 (61.5%) were younger than aged 45, while 20 (38.5%) were 45 years of age or older. The mean age of the sample was 40 years and 10 months; the group means was 34 years and 9 months for the younger adults, and 50 years and 9 months for those aged 45 and over. Less than half (23, 44.2%) of the study cohort were females. In the younger group of adults with IDD there were 15 females (46.9%), while 40% of those aged 45 and over were females (8). The cause of IDD was known for 73.1% of the study participants; 47.4% of the study sample had cerebral palsy and 15.8% had Down Syndrome. Table 1 summarizes physical health status of the two groups.
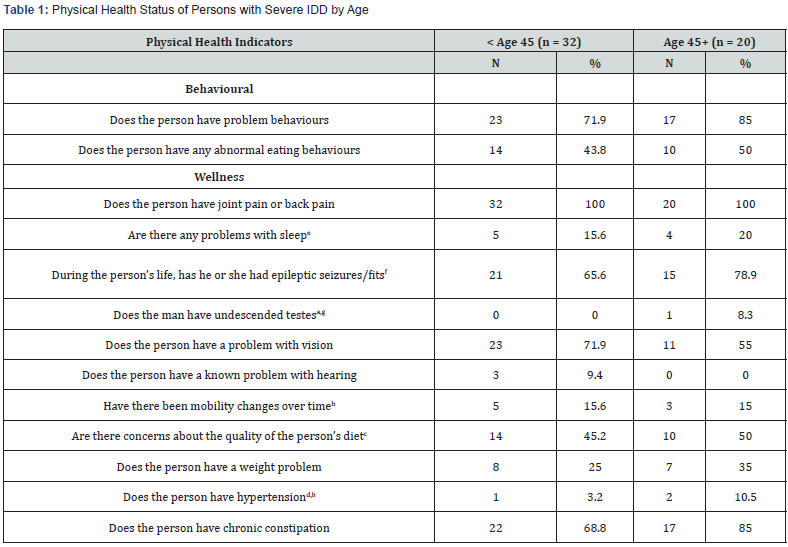
Note: All variables were measure on a dichotomous scale (Yes/No), and this table presents the frequencies of the “yes” responses. aMissing data for 15 (46.9%) study participants in the younger age group, because this is a sex-related variable. bThis change was a decline for both age groups. cMissing data for 1 (3.1%) person < age 45. dMissing data for 1 (3.1%) person < age 45. eUnknown data for 1 (5.0%) person age 45+. fMissing data for 1 (5.0%) person age 45+. gMissing data for 8 (40.0%) of the study participants in the older age group, because this is a sex-related variable for person age 45+. hMissing data for 1 (5.0%) person age 45+.
Behavioural-related indicators showed an increased proportion of both problem and abnormal eating behaviours in those above 45 years of age, compared to those under 45 years of age. Within the wellness component, similarities (less than 5% difference) were seen between age groups regarding joint pain or back pain, sleep problems, and mobility changes over time. There was a higher proportion of epileptic seizures/fits, concerns about the quality of diet, undescended testes, weight problems, hypertension, and chronic constipation for study participants aged 45+ compared to those who were under 45 years of age. There was a smaller proportion of persons with vision problems and hearing problems among those aged 45 years or older ,compared to those under 45 years of age.
Table 2 summarize mental health status for the two age groups. There was a higher proportion of psychiatric illness and evidence of an underlying psychiatric disorder in study participants aged 45+, compared to those under 45 years of age. Table 3 summarizes access to preventive healthcare status for the two age groups.
Within screening, similarities (less than 5% difference) were seen between age groups regarding diabetes testing and osteoporosis assessments. All woman above 45 years of age had breast cancer screening which is at a slightly higher rate than those under 45 years of age. Study participants aged 45+ had a higher frequency of bowel cancer tests, compared to those under 45 years of age. Within immunization, those aged 45 and older had higher rates of tetanus, diphtheria and pertussis, and influenza vaccinations; however, rates were similar in the two age groups with a less than 5% difference. Those younger than age 45 had higher rate of hepatitis B vaccinations. Within health-related behaviours, those younger than age 45 had a higher proportion of dental examinations, and both age groups had the same proportion of medication reviews.
Discussion and Conclusion
Overall, this analysis identified some similarities as well as some important differences between the two groups of adults with IDD compared. Within physical health indicators, there were more problem and abnormal eating behaviours in the age group 45+. Similarities were seen in the two age groups in terms of joint pain or back pain, sleep problems, and mobility changes over time. Vision and hearing problems were more common among those under the age of 45 years. The remaining physical health indicators, namely epileptic seizures/fits, quality of diet concerns, undescended testes, weight problems, hypertension, and chronic constipation were more common among those 45 years of age and over. Psychiatric illness and evidence of an underlying psychiatric disorder were more common in those above 45 years of age. Within preventive healthcare access, similarities between the two age groups were seen regarding diabetes testing, osteoporosis assessments, and breasts cancer screening (<10% difference). Bowel cancer testing was much more common in the 45+ age group. Similarities were seen between the two age groups regarding tetanus diphtheria and pertussis, and influenza vaccinations. Hepatitis B vaccinations were more common in those younger than age 45. There was a large difference in dental examination, which was more common in those under the age of 45. The rates of medication review... were the same for the two age groups. A greater understanding of the impact of aging in individuals with IDD may inform better organization and coordination of healthcare and social services, and the development of interventions, and policies that aim to improve their overall health and quality of this vulnerable group life throughout the lifespan.
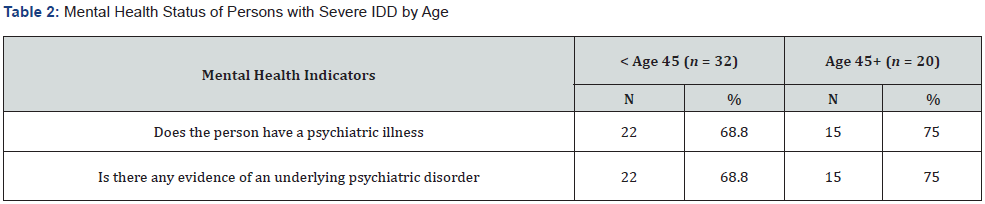
Note: All variables were measure on a dichotomous scale (Yes/No), and this table presents the frequencies of the “yes” responses.
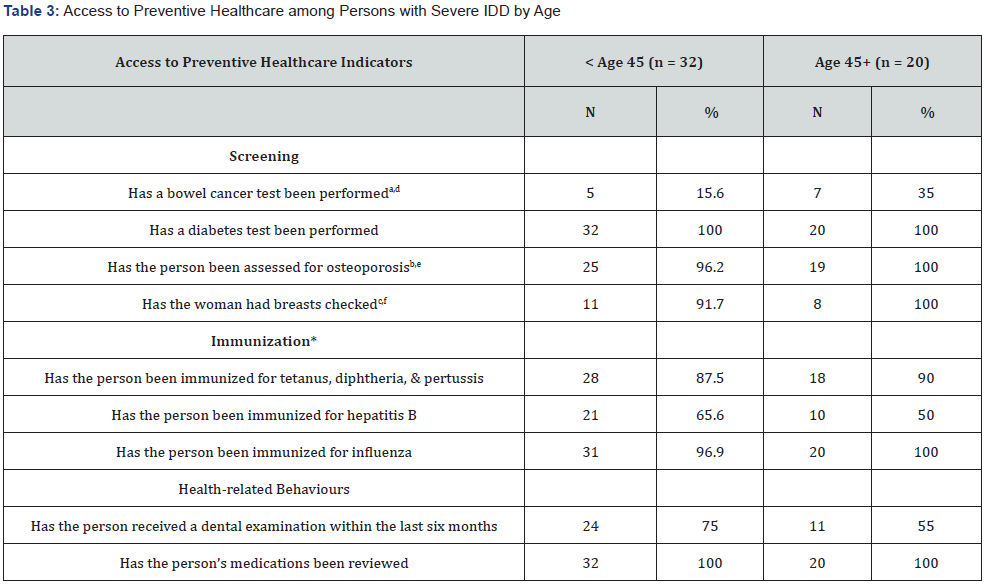
Note: All variables were measure on a dichotomous scale (Yes/No), and this table presents the frequencies of the “yes” responses. Missing data were excluded. aNo/unknown data for 27 (84.4%) persons under 45 years of age. bMissing data for 6 (18.8%) persons under 45 years of age. cMissing data for 20 (62.5%) of the study participants in the younger age group, because this is a sex-related variable. *All immunization status variables were coded as yes or no/unknown. dNo/unknown data for 13 (65.0%) study participants aged 45+. eMissing data for 1 (5.0%) persons age 45+. fMissing data for 12 (60.0%) study participants in the older age group, because this is a sex-related variable.
References
- Pimlott N (2019) Aging with intellectual and developmental disabilities: Family physicians can make a difference. C Fam Physician 65(Suppl 1): S3.
- Shooshtari S, Ouellette-Kuntz H, Balogh R, McIsaac M, Stankiewicz E, et al. (2020) Patterns of mortality among adults with intellectual and developmental disabilities in Manitoba. Journal of Policy and Practice in Intellectual and Developmental Disabilities, 17(3): 185-278.
- Shooshtari S, Martens PJ, Burchill C, Dik N, Naghipur S (2011) Prevalence of Depression and Dementia among Adults with Developmental Disabilities in Manitoba (Canada). Int J Family Med 2011: 319574.
- Stankiewicz E, Ouellette-Kuntz H, McIsaac M, Shooshtari S, Balogh R (2018) Patterns of mortality among adults with intellectual and developmental disabilities in Ontario. Can J Public Health 109(5-6): 866-872.
- Shooshtari S, Naghipur S, Zhang J (2012) Unmet health care and social services needs of older adults living with a developmental disability in Canada. Journal of Policy and Practice in Intellectual Disabilities 9(2): 81-91.
- Lennox N, Bain C, Rey-Conde T, Purdie D, Bush R, et al. (2007) Effects of a comprehensive health assessment programme for Australian adults with intellectual disability: A cluster randomized trial. Int J Epidemiol. 36(1): 139-146.
- Chimney K, Kian S, Cameranesi M, McCombe L, Shooshtari S (2020) Health of persons with intellectual and developmental disabilities transitioning into community homes from a complex care residence in Canada. Journal on Developmental Disabilities 25(2).






























