Promoting Knowledge of Cognitive Dysfunction in Minority Older Communities, their Caregivers and Clinicians
Koshy Alexander¹* Ruth Manna¹, Natalie Gangai, Rosario Costas-Muñiz² and Beatriz Korc Grodzicki¹
1Geriatrics, Memorial Sloan Kettering Cancer Center, USA
2Psychiatry & Behavioral Sciences, Memorial Sloan Kettering Cancer Center, USA
Submission: November 14, 2019; Published: December 02, 2019
*Corresponding author: Koshy Alexander, Geriatrics, Memorial Sloan Kettering Cancer Center, New York, NY, USA
How to cite this article: Koshy Alexander, Ruth Manna, Natalie Gangai, BS, Rosario Costas-Muñiz, Beatriz Korc Grodzicki. Promoting Knowledge of Cognitive Dysfunction in Minority Older Communities, their Caregivers and Clinicians. OAJ Gerontol & Geriatric Med. 2019; 5(3): 555663. DOI : 10.19080/OAJGGM.2019.05.555663
Abstract
Objectives: Lack of knowledge about geriatric conditions is a barrier that prevents older minority populations from receiving optimal healthcare. We aim to develop an educational initiative to improve the knowledge gap on cognitive dysfunction in three target populations: older minority community members, their caregivers, and healthcare professionals (HCPs).
Methods: A nested mixed-methods with an interventional pre-post assessment approach was used for this community-based educational initiative. Educational sessions on memory loss were developed and conducted. 182 community members, 63 caregivers and 133 HCPs participated. Pre-posttest questionnaires and qualitative data were collected to measure the impact.
Results: The results showed significant improvements in knowledge in all three participant groups. The qualitative comments showed improved understanding and intentions to change.
Discussion: Development of an educational program on cognitive dysfunction targeting community members, caregivers and HCPs who take care of older patients is feasible in underserved community and clinical settings.
Keywords: Cognitive dysfunction Educational initiative Ethnogeriatrics Older minority populations
Abbrevations: MCI: Mild Cognitive Impairment; HCP: Health Care Providers; HRSA: Health Resources and Services Administration; MSK: Memorial Sloan Kettering Cancer Center; GRIP: Geriatric Resource Interprofessional Program; CBOs: Community-Based Organizations
Introduction
One important public health dilemma is the multi-layer challenge associated with the care of the older adult, specifically focused on cognitive health. The US population is getting older and growing more racially diverse. The number of racial/ethnic minority populations has increased from 46 million in 1980 to 83 million in 2000, with an estimated increase to 157 million by 2030 [1]. Minorities and older adults represent an intersection of populations that are particularly vulnerable to suboptimal care. The causes are complex and focus on racial and ethnic disparities in health resulting from socioeconomic status, unequal access to care, differences in behavioral, environmental and genetic risk factors, and social and cultural biases that influence the quality of care [2]. Moreover, ageism tends to reinforce social inequalities as it is more pronounced towards poor people or those with dementia [3]. An estimated 5.4 million Americans have Alzheimer’s disease, and by mid-century, this number is projected to grow to 13.8 million [4]. Today, someone in the US develops Alzheimer’s disease every 66 seconds. By 2050, one new case of Alzheimer’s is expected to develop every 33 seconds, resulting in nearly 1 million new cases per year [4]. Studies have shownthat more years of education is associated with a lower risk for dementia [5]. It is no surprise that dementia afflicts minority populations more than Caucasians; African Americans are twice as likely, and Hispanics are about one and one-half times as likely, to have Alzheimer’s or other dementias compared to Caucasians [6]. Several barriers to addressing cognitive dysfunction exist within both the older and minority populations. These barriers include poverty, lack of transportation, illiteracy, cultural taboos regarding dementia and poor communication [7-9]. For example, in New York City (NYC), 23% of the population is categorized as having low-English proficiency.
Many people in the community with Mild Cognitive Impairment (MCI) and Alzheimer’s disease do not recognize cognitive, functional or behavioral impairment as abnormal [10]. This lack of understanding can have serious effects on health, and because they or their caregivers cannot recognize and acknowledge the deficits, they do not seek treatment. Daily functioning may be compromised because they lack adequate judgment of situations [11]. Enough education needs to be given to those affected and to the community at large to aid in preventive care and to improve understanding of early diagnosis and disease management
Caregivers play a crucial and physically, mentally and emotionally demanding role in the management of patients with serious chronic diseases. People with dementia typically require more supervision, are less likely to express gratitude for the help they receive and are more likely to be depressed. These factors have been linked to negative caregiver physical and psychosocial outcomes [12]. Family caregivers often feel unprepared to provide care, have inadequate knowledge to deliver proper care, and receive little guidance from the formal health care providers [13]. Family caregivers may not know when they need community resources, and then may not know how to access and best utilize available resources [14]. Without this support, caregivers often neglect their own health care needs to assist their family member, causing deterioration in the caregiver’s health and well-being [15].Despite the growth in the older population, there is an unmet need in healthcare workforce to take care of these patients’ needs. While the demand for physicians specialized in the medical care of older adults is increasing, the interest among medical students for a career in geriatrics is slow to follow [16]. Though the coverage of geriatric topics at medical schools is increasing, students still express significant reservations about their abilities to treat older patients. In one national survey, only 27 % of graduating familypractice residents and only 13% of graduating internal-medicine residents felt very prepared to care for nursing-home patients. Although a large majority of graduating psychiatry residents felt very prepared to diagnose and treat delirium (71%) and major depression (96%), only 56% felt very prepared to diagnose and treat dementia [17]. In this paper, we examine the role held by three specific groups of people in the care of cognitive health in underserved ethnically diverse populations: the older adult community members themselves, their caregivers, and the health care providers (HCP) taking care of them. Each role has significant opportunity in improving knowledge and in understanding the disease and its appropriate management. We focused our efforts on a large-scale educational program to address these gaps in knowledge, focusing on cognition in older adults, for all three groups.
Methods
Team development
The Health Resources and Services Administration (HRSA), an agency of the U.S. Department of Health and Human Services, is the primary federal agency for improving health care to people who are geographically isolated, and economically or medically vulnerable. Through the Geriatric Workforce Enhancement Program (GWEP), HRSA provides funds to improve the healthcare of older adults through education and training. With the GWEP award, the Geriatrics service at Memorial Sloan Kettering Cancer Center (MSK) established the Geriatric Resource Interprofessional Program (GRIP). The GRIP team serves as content experts and a teaching core that includes representation from occupational and physical therapy, pharmacy, nutrition, medicine, nursing, social work, psychiatry, immigrant health and members from the GRIP’scommunity and clinical partners that serve community-dwelling older adults in culturally diverse and medically underserved areas. The community-based organizations (CBOs) and clinical sites are experts in the populations they serve. Team members teach each other about their respective professions, context, and its unique relevance in the health management of the older adult during the process of developing appropriate community, caregiver and HCP educational material. Via GRIP, multiple professionals’ expertise and perspectives are infused into one educational program targeted for each audience.
Target population
We targeted three groups of learners: older community members, caregivers, and HCPs. All participants were selected by convenience sampling. Older adults were accessed through regular attendance to community programs in the NYC area, partnered with GRIP. The NYC boroughs of Queens and Brooklyn were targeted for their ethnic diversity to cater to the underserved. The borough of Queens in NYC is the most ethnically diverse urban area in the US with 74% of the population being Hispanic, African American or Asian and 48% being foreign born. The borough of Brooklyn is about 34% African American, 13% Asian and 19% Hispanic or Latino with about 36% of the population being foreign born [18]. The partner CBOs marketed for the educational programs through phone calls, digital and print advertising, and through in person reminders at other educational programs. Caregivers were approached through CBO staff who targeted invitations to this caregiver-client group. Digital and print marketing were also utilized for the caregiver audience. HCPs included residents and fellows in training, attendings, nursing staff including nurse practitioners, and social workers. Sessions for staff were conducted at scheduled educational settings, like monthly staff training and conferences at NYC area hospitals. Participation in the sessions and completion of related assessments were voluntary and explained as such by site staff with the help of interpreter(s) if needed.
Content development and implementation
Across all content development, the GRIP team used the Patient Education Materials Assessment Tool -A/V (PEMAT) [19] to rate the content’s understandability and actionability. GRIP team members, including CBO representatives, provided feedback to the presenter about content organization, language, and engagement. Cultural responsiveness was discussed to ensure attendees would be able to connect and identify with the material and that the material was communicated in a culturally appropriate way, accounting for traditions and norms around aging and health.
To understand the educational gaps of older community members, regular attendants of our partner CBO educational programs at senior centers, religious institutions, public libraries and CBO headquarters completed an informal needs assessment. Older community members were asked to rank the followingtopics on their interest level, on a scale from 1 to 4 (1 being their first choice and 4 their last) on four listed topics: nutrition, falls, memory loss and cancer. Thirty-five older adults responded to this survey and 71% indicated memory loss as most interesting to them. From this, the GRIP team focused initial efforts to develop the memory loss and dementia program. In the Fall 2015, the primary presenter, a geriatrician, developed the audiovisual module Memory Loss & Dementia, for the community older adult population. The material incorporated imagery that the target audience could relate to, such as Yoga, ethnic foods and landscapes for sessions developed for the South Asian communities. The geriatrician presented the material to the GRIP team. Using the PEMAT, GRIP team members rated the material and the scores for understandability and actionability were 59% and 78% respectively. The material was revised based on the feedback, improving these scores to 83% and 90%. Five of the 8 lectures were interpreted, 4 to the predominant South Asian language (Hindi or Bengali) and 1 to Spanish. The remaining 3 lectures were delivered to English speaking audiences.
To identify the educational needs and the interests of caregivers, the GRIP conducted a 90-minute focus group. The subject of memory loss was identified as a topic of interest. A module called Caregiver Education: Cognitive Impairment was developed. Per GRIP’s content development process, it underwent a PEMAT review (83% understandability and 80% actionability), with the presenter adjusting after the feedback regarding organization, language and cultural responsiveness. Since most caregivers identified as South Asian, 4 of the 7 sessions were provided in English with simultaneous interpretation to the predominantly understood language of the group, Hindi. Though the majority caregivers were native Gujarati speakers, the most commonly understood language in the group was Hindi. The remaining 3 sessions did not need interpretation or translation as it was to English-speaking audiences.
Given the well-documented shortage of appropriately trained HCPs in the care of the older adults, the subject of memory loss/ dementia/delirium, was well-suited for our HCP target population. Four modules were created to meet the needs of each types and level of HCP audience: Delirium in Older Hospital Patients (Post Graduate Year -PGY- 1-3), Assessment and Management of Cognitive Impairment in the Older Adult (Interprofessional), Cognitive Impairment in the Older Adult (Nursing), and Dementia & Delirium (PGY1). In this large educational initiative across three learner groups, between November 2015 and January 2019, the following sessions were implemented: Memory Loss & Dementia (older community members) was conducted 8 times at 7 different centers. Caregiver Education: Cognitive Impairment was offered 7 times at 3 different centers (one being a video live-stream program) for caregivers. The 10 sessions for HCPs comprised one of the four modules described and were conducted in 5 different sites.
Measures
This study was conducted as a nested mixed-methods pre-post intervention design to incorporate quantitative pre and post data and qualitative data after the intervention to assess its effectiveness (20). Questionnaires were developed to assess knowledge uptake after participation. They contained five to six multiple choice questions and were translated to multiple languages. They were administered prior to and immediately after participation in the educational program. Pre- and post-questionnaires were matched using an identification case number. In August 2018, the pre-post questions for community members were modified to increase the difficulty of one question due to ceiling effect (question was too easy on baseline). As seen in (Table 2), we are presenting the aggregate results for the sessions prior to and after this change in measure for the Memory Loss & Dementia sessions. Completion of the questionnaires was voluntary and anonymous, and the publication of these data was approved by the MSK Institutional Review Board.
Analysis
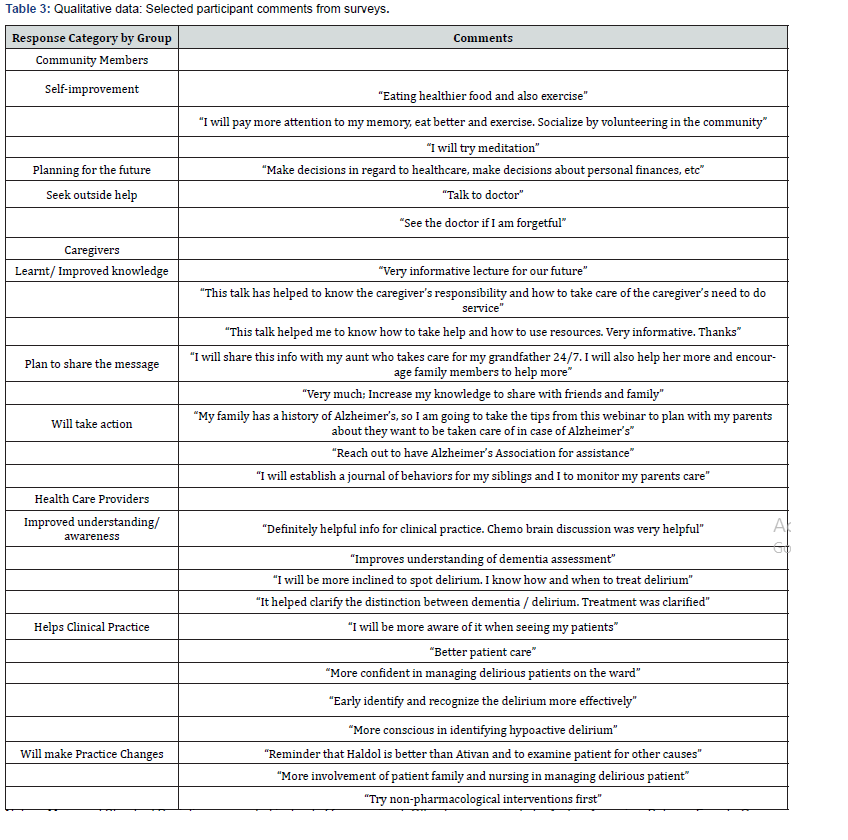
Analyses were conducted using the statistical program SPSS 21 (IBM Corp. Released 2017. IBM SPSS Statistics for Windows, Version 25.0. Armonk, NY: IBM Corp). Demographic characteristics, including age, gender, language preference and birthplace, were analyzed using descriptive statistics (mean, frequencies and standard deviations). Paired samples t-tests were used to evaluate change in knowledge on the programs on preand post-assessments. A p-value less than .05 was considered statistically significant. Qualitative analyses were conducted using thematic content analysis, the most frequent themes are presented on (Table 3).
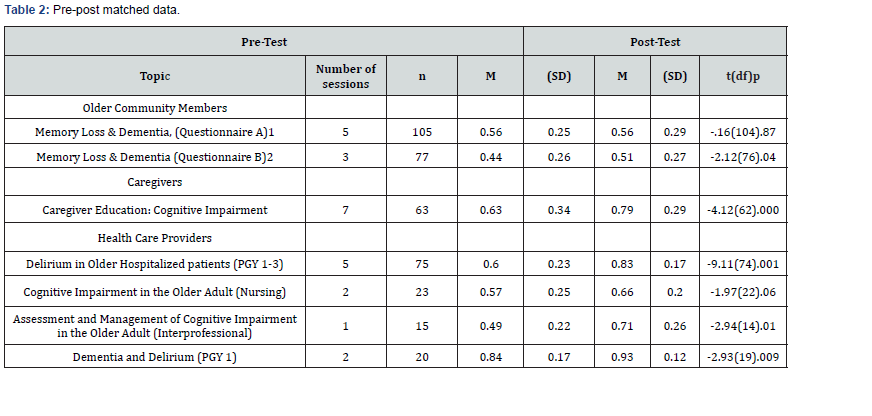
df: Degrees of Freedom
Sessions conducted before August 2018
Sessions conducted after August 2018: Questionnaire B includes increased difficulty in listed questions
Results
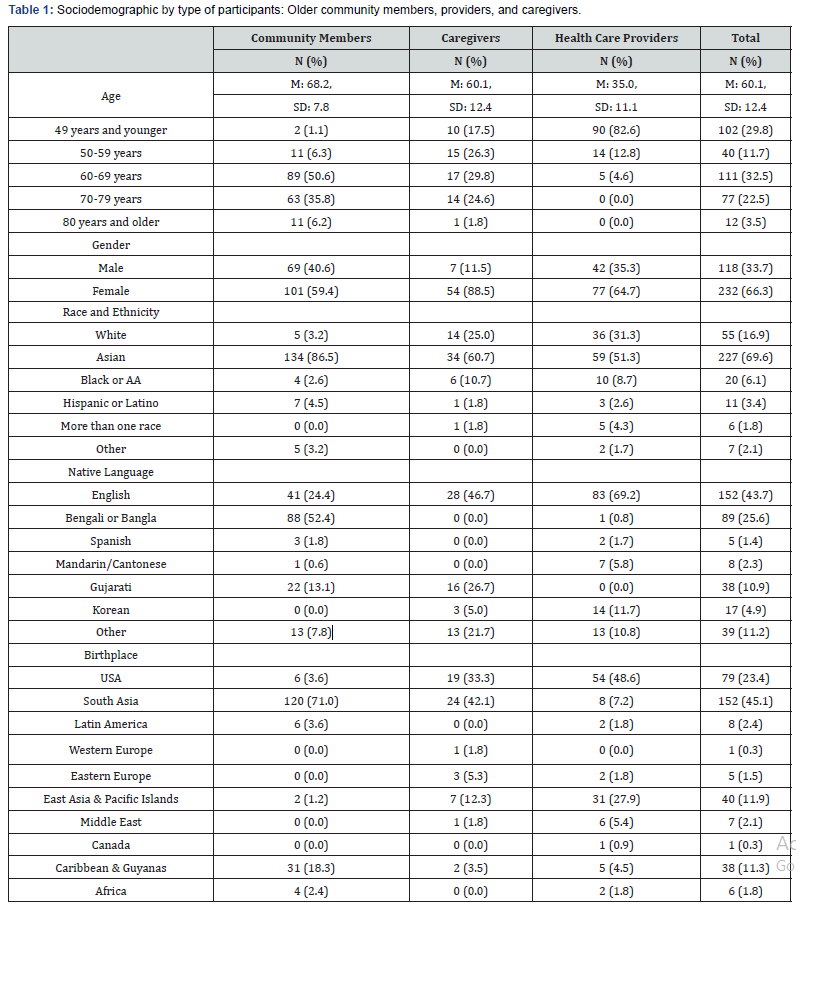
The total sample consisted of 378 participants:182 community members, 63 caregivers, and 133 HCPs. Sociodemographic data is presented in (Table 1). Of the older community members who reported demographic information, the mean age was 68 (SD=7.8) and three out of five were female (59%). The majority were Asian (87%), half reported their native language to be Bengali (52%), and 71% were born in a South Asian country (India, Pakistan, Bangladesh and Nepal). Caregivers had a mean age of 60 (SD=12.4). The majority were females (89%) and almost two thirds were Asian (61%). The primary language of 47% of the caregivers was English, followed by Gujarati (27%). One third were born in USA (33%) and 42% were born in South Asia.
Note: a Mean and Standard Deviations presented instead of frequencies; b Other languages include: Arabic, Armenian, Bahasa, French, German, Guyanese, Hebrew, Hindi, Kannada, Korean, Nepali, Persian, Poshto, Punjabi, Romanian, Russian, Tagalog, Tamil, Telugu, Turkish, Urdu, Vietnamese; c Other Countries by region include: 1) in South Asia, Bangladesh, India, Pakistan, Nepal, 2) in Latin America, Brazil, Colombia, Puerto Rico, Dominican Republic, Paraguay, El Salvador, 3) in Western Europe, England, Germany, Ireland, 4) in Eastern Europe, Poland, Romania, Russia, Botswana, Greece, 5) in East Asia & Pacific Islands, China, Philippines, Korea, Taiwan, Vietnam, 6) in Middle East, Israel, Syria, Turkey, Bahrain, Iran, Saudi Arabia, Lebanon, Iraq, Cyprus, in 7) Caribbean (non-Hispanic) & Guyanas, Jamaica, Trinidad, Haiti, and 8) in Africa, Cameroon.
Providers had a mean age of 35 years (SD=11.1), two thirds were females (65%), almost half (51%) were Asian, the native language of two thirds (69%) was English followed by Korean (12%). Most of the providers were born in USA (49%), followed by East Asian countries (28%). Almost half of the medical professionals were residents (49%), followed by nurses (24%), medical students (19%), physicians (5%), patient care technicians (2%), and social workers (2%).
The t-tests for paired samples are presented in (Table 2). The results indicate a statistically significant difference for the sessions, Memory Loss & Dementia [t (76) = -2.12, p< .04], conducted with older community members after the measure assessment was updated in August 2018. The pre-post evaluations for the sessions on Memory Loss & Dementia prior to upscaling of difficulty in the measure conducted between April 2017 to May 2018 did not yield significant results [t (104) = -0.16 p = .87]. The sessions conducted with caregivers: Caregiver Education: Cognitive Impairment showed highly significant increase in knowledge [t (62) = -4.12, p < .001]. Among the HCP sessions Delirium in Older Hospitalized Patients (PGY1-3) [t(74) = -9.11, p < .001]; Cognitive Impairment in the Older Adult (Nursing) [t(14) = -2.94, p = .01]; and Dementia and Delirium (PGY 1) [t(20) = -2.93, p = .009] showed improvement in knowledge. There were no significant improvements in knowledge for the Assessment and Management of Cognitive Impairment in the Older Adult (Interprofessional) group. All participants were given the opportunity to provide feedback after completion of the sessions and asked how this information would change their daily behavior or practice. These responses were categorized into common broad themes which reflect improved understanding and plans to make behavioral changes. Selected themes and comments are presented in (Table 3). Overall, older adults described specific behavior changes they would make, as well as resources they would seek out to clarify doubts and obtain care. Caregivers commented on knowledge gained as well as future planning for those older family members who might need dementia care. HCPs reported increased knowledge and detailed clinical practice changes they planned to make in the care of older adults with cognitive impairment.
Discussion
Our results demonstrate the successful development and application of an educational program to improve the understanding of cognitive syndromes in older minority communities. We see consistent, significant improvements in knowledge among older adults, caregivers and HCPs, and qualitative data that describe improved understanding and planned changes in behavior after the sessions. We identified educational needs of older community dwelling ethnic minority members and their caregivers to provide culturally responsive educational sessions, in their language in a familiar and comfortable environment. This specific educational and cultural tailoring made sessions interactive and open for community members and caregivers to approach it with a sense of familiarity. There is a well described national shortage of geriatricians in the US [21, 22]. Few medical residents choose the extra year of training required to become a geriatrician, and those going into other specialties typically get little exposure to the health needs of older adults during their training. Internists, family medicine doctors and other HCPs such as nurse practitioners and physician assistants provide most care for older adults and they should be trained [21-23] Educational programs like ours help to correct the deficits in geriatric medicine knowledge in non-geriatrician HCPs. This is one way of improving the quality of healthcare received by older patients.
The implementation of this educational approach came with its own set of challenges. Community health education in underserved populations is complex: One major barrier we faced was the wide range in literacy levels of the community member participants. It ranged from a few people who were illiterate and could not write their name in their primary language to people with post-secondary and professional degrees. In many cases, community organizers and members of the GRIP team had to sit one-on-one with participants to fill the questionnaires. Tailoring a pre-post questionnaire to assess knowledge change in such an audience proved challenging Additionally, we had to adjust educational materials to ensure understandability. Some audiences wanted more detailed information and others didnot, so adjustments would often have to be made during the presentation. These adjustments might have limited the ability to accurately capture knowledge gain. After analyzing the difficulty level of the questions based on initial sessions with a wide range of audiences, we noted consistent high achievement on one item. We modified that item to increase the difficulty of a question and subsequent results showed statistical significance in knowledge improvement. The community members’ qualitative comments showed a positive impact. In the case of the HCPs, with higher and more homogeneous educational attainment, the quantitative analysis showed a significant improvement in knowledge uptake and it paralleled the qualitative comments.
Another barrier we faced was adapting to the multiple cultures and primary languages of the community and caregiver participants. The sessions were interpreted to the most understood predominant primary language of the audience and the questionnaires and take-home resources were translated into the same language. However, it is still probable that the sessions were not fully understood by all members who attended because some participants spoke different variations of the primary language or a different primary language entirely. We conformed to cultural practices by learning the cultural norms of the community prior to conducting in each session. The sessions conducted at a mosque for example had physical partitions between seating areas for the male and female participants, and our own staff members respected these boundaries and conformed to the dress codes and interactions. Transportation and access to the community centers by participants varied. Even in NYC, where public transportation is available, it is a challenge for some older community members and the attendance also depended on the weather. We tried to schedule sessions according to the best times of day for the caregiver groups and utilized existing protected meeting times for HCPs to maintain attendance.
Future directions
We will need ongoing educational efforts and future studies to assess the long-term benefits of these interventions in increasing awareness and promoting a more proactive approach to care from the community members and their caregivers. Patient reported outcomes could be measured in community clinics after educational interventions. Behavioral intention measures after the sessions are also worth exploring. Caregiver related measures such as stress, satisfaction with medical care, knowledge retention and change in behavior should be evaluated long-term. Continued retention of knowledge and the implementation of geriatric principles by HCPs in their daily practices could also be studied. Strategies to address challenges around health literacy and surveys will continue to be addressed and cultural responsiveness will continue to be integrated into the data collection procedures.
Conclusions
We have successfully developed and applied a critical educational program about memory loss for older communitymembers, their caregivers and HCPs in diverse underserved areas of NYC. The education was very well received and prompted the attendees to propose behavior changes that could potentially improve the care of individuals with cognitive disfunction. We demonstrated significant short-term knowledge uptake on memory loss and cognitive health among the three audiences. The long-term effect of the knowledge gain and behavior change needs to be better determined on future studies.
Acknowledgements
This publication was made possible by Grant Number #U1QHP28705 from the Health Resources and Services Administration (HRSA), an operating division of the U.S. Department of Health and Human Services. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the Health Resources and Services Administration or the U.S. Department of Health and Human Services. This research was funded in part through the NIH/NCI Cancer Center Support Grant P30 CA008748.
Conflict of Interest
The authors declare no conflicts of interest and have nothing to disclose.
References
- Smith BD, Smith GL, Hurria A, Hortobagyi GN, Buchholz TA (2009) Future of Cancer Incidence in the United States: Burdens Upon an Aging, Changing Nation. J Clin Oncol 27(17): 2758-2765.
- Williams DR, Priest N, Anderson N (2016) Understanding Associations between Race, Socioeconomic Status and Health: Patterns and Prospects. Health Psychol 35(4): 407-411.
- Ayalon L, Tesch-Römer C (2017) Taking a closer look at ageism: self- and other-directed ageist attitudes and discrimination. Eur J Ageing 14(1): 1-4.
- 2016 Alzheimer's disease facts and figures. Alzheimer's & dementia: the journal of the Alzheimer's Association 12: 459-509.
- Langa KM, Larson EB, Crimmins EM, Faul JD, Levine DA, et al. (2017) A Comparison of the Prevalence of Dementia in the United States in 2000 and 2012. JAMA Intern Med 177(1): 51-58.
- (2018) Alzheimer's Disease Facts and Figures. Alzheimer’s Association.
- Kenning C, Daker-White G, Blakemore A, Panagioti M, Waheed W (2017) Barriers and facilitators in accessing dementia care by ethnic minority groups: a meta-synthesis of qualitative studies. BMC psychiatry 17: 316-316.
- Giebel CM, Zubair M, Jolley D, Bhui KS, Purandare N, et al. (2015) South Asian older adults with memory impairment: improving assessment and access to dementia care. Int J Geriatr Psychiatry 30(4): 345-356.
- Syed ST, Gerber BS, Sharp LK (2013) Traveling towards disease: transportation barriers to health care access. J Community Health 38(5): 976-993.
- Zamboni G, Wilcock G (2011) Lack of awareness of symptoms in people with dementia: the structural and functional basis. Int J Geriatr Psychiatry 26(8): 783-792.
- Aalten P, van Valen E, Clare L, Kenny G, Verhey F (2005) Awareness in dementia: a review of clinical correlates. Aging Ment Health 9(5): 414-422.
- Ory MG, Hoffman RR, Yee JL, Tennstedt S, Schulz R (1999) Prevalence and impact of caregiving: a detailed comparison between dementia and nondementia caregivers. Gerontologist 39(2): 177-185.
- Scherbring M (2002) Effect of caregiver perception of preparedness on burden in an oncology population. Oncol Nurs Forum 29: E70-76.
- Given BA, Given CW, Stommel M, Lin CS (1994) Predictors of use of secondary carers used by the elderly following hospital discharge. J Aging Health 6(3): 353-376.
- Schulz R, Beach SR (1999) Caregiving as a risk factor for mortality: the Caregiver Health Effects Study. JAMA : the journal of the American Medical Association 282(23): 2215-2219.
- Meiboom AA, de Vries H, Hertogh CMPM, Scheele F (2015) Why medical students do not choose a career in geriatrics: a systematic review. BMC Med Educ 15: 101.
- Institute of Medicine (US) Committee on the Future Health Care Workforce for Older Americans. Retooling for an Aging America: Building the Health Care Workforce. Washington (DC), National Academies Press, USA.
- US Census Bureau QuickFacts: Kings County (Brooklyn Borough), New York; Queens County (Queens Borough), New York.
- Shoemaker SJ, Wolf MS, Brach C (2014) Development of the Patient Education Materials Assessment Tool (PEMAT): A new measure of understandability and actionability for print and audiovisual patient information. Patient Educ Couns 96(3): 395-403.
- (2018) NIH Office of Behavioral and Social Sciences. Best practices for mixed methods research in the health sciences. (2nd ), Bethesda: National Institutes of Health.
- Warshaw GA, Bragg EJ (2014) Preparing the health care workforce to care for adults with Alzheimer's disease and related dementias. Health affairs (Project Hope) 33(4): 633-641.
- Bragg EJ, Warshaw GA, Meganathan K, Brewer DE (2012) The development of academic geriatric medicine in the United States 2005 to 2010: an essential resource for improving the medical care of older adults. J Am Geriatr Soc 60: 1540-1545.
- Peterson LE, Bazemore A, Bragg EJ, Xierali I, Warshaw GA (2011) Rural-urban distribution of the U.S. Geriatrics physician workforce. J Am Geriatr Soc 59(4): 699-703.






























