The Revelations of Malaria Associated Kidney Disease - A Menace in the Tropics
Kallol Bhattacharjee*, Abhishrut Jog, Chandra Prakash Thakur and Dwijen Das
Silchar Medical College, India
Submission: February 15, 2018; Published: March 07, 2018;
*Corresponding author: Kallol Bhattacharjee, Silchar Medical College, India, Email: kbsilchar64@gmail.com
How to cite this article: Kallol Bhattacharjee, Abhishrut Jog, Chandra Prakash Thakur, Dwijen Das. The Revelations of Malaria Associated Kidney Disease - A Menace in the Tropics. JOJ uro & nephron. 2018; 5(2): 555659. DOI: 10.19080/JOJUN.2018.05.555659
Keywords
Keywords: Malaria; Acute kidney injury; Clinical profile; Plasmodium; Falsiouram
Abbreviations : AKI: Acute Kidney Injury; RRT: Renal Replacement Therapy; MAKI: Malarial AKI; MODS: Multi Organ Dysfuction Syndrome; RDT: Rapid Diagnostic Test
Introduction
Malaria is an Italian word composed of "mala" and "aria" derived from malus (bad), and aeris (air). It was first used to describe a fever (miasma), which was wrongly attributed to exposure to poisonous air rising from marshes. Malaria is caused by protozoan parasites of the genus Plasmodium, namely, P falciparum, P. vivax, P. malariae, P. ovale, and P knowlesi. There are more than 3.3 billion people living in countries with ongoing malaria transmission at risk of infection [1]. According to the WHO 2015 report, an estimated 214 million cases of malaria and 438,000 deaths occurred in 2015 due to complications [2].
Acute kidney injury (AKI) is a fairly common and serious complication seen in acute falciparum malaria in adults and older children. Depending on the definitions used for AKI, intensity of malaria transmission, age affected, infecting species, and the cohort studied, incidence of AKI in malaria varies from 0.4% to 60% [2,3]. The pathogenesis of AKI in malaria is still not clearly understood. Blockage of renal microcirculation due to sequestration of infected erythrocytes, immune-mediated glomerular injury and volume depletion are some of the proposed hypotheses [4,5].
The availability of renal replacement therapy (RRT) and appropriate antimalarial chemotherapy has been shown to reduce case fatality rate as well as enhance the recovery of renal function [6,7].
Silchar Medical College and Hospital is the only referral hospital in the southern part of Assam, and serves neighbouring states including Mizoram, North Tripura, West Manipur and South Meghalaya. A study on this particular subject has not been conducted in these parts before.
Aims and Objectives
1) To study the clinical profile of malarial AKI (MAKI)
2) To classify MAKI in terms of its clinical presentation as - MAKI alone and MAKI with Multi Organ Dysfuction Syndrome (MODS)
Materials and Methods
Study setting
The present study was conducted in the Department of Medicine, Silchar Medical College and Hospital, Silchar, Assam.
Period of study
The present study was conducted from 1st August 2009 to 31st March 2017, for a period of 7 years and 8 months.
Sample size
A total of 668 patients admitted in the Department of Medicine during the study duration were included randomly for the study after fulfillment of the inclusion and exclusion criteria.
Study design
The study was a hospital based prospective observational study.
Methodology
All the patients diagnosed with malaria using either Rapid Diagnostic Test (RDT) or peripheral blood smear from freshly collected venous blood sample, were assessed. Lab investigations including Complete Blood Count, Sr. creatinine, Sr. electrolytes, Liver Function tests, Random blood glucose, Urine microscopy and dipstick examination, were performed in these patients.
Those patients having Acute Kidney Injury (AKI) were enrolled in the study. AKI was diagnosed using the KDIGO criteria:
a. Increase in Sr. Creatinine by 0.3mg/dl or more within 48 hours or
b. Increase in Sr. Creatinine to 1.5 times baseline or more within the last 7 days or
c. Urine output less than 0.5ml/kg/hour for 6 hours.
A written and informed consent was obtained from these patients. Multi-organ dysfunction syndrome (MODS) was defined using the Sequential Organ Failure Assessment score (SOFA score) of greater than 2 (Table 1).
A detailed clinical history was taken and a complete physical examination was done in all cases. Wherever necessary additional investigations such as Chest Radiographs, Ultrasound of Abdomen, CT scan Brain, cANCA, pANCA were performed.
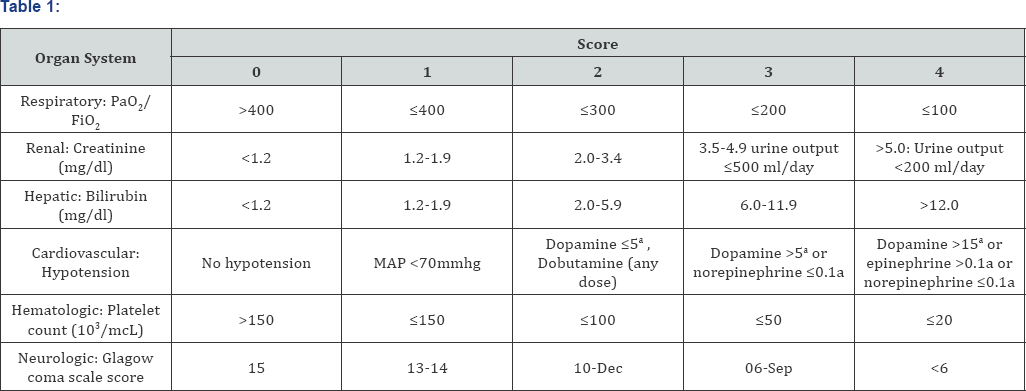
Adrenergic agents administered for at least 1h (does given are in |ig/kg/min). FiO2= Fractional inspired oxygen; MAP= Mean arterial pressure; PaO2= Arterial oxygen tension; SOFA= Sequential organ failure assessment
The data of such patients fulfilling the inclusion and exclusion criteria were collected on a structured proforma.
Inclusion criteria
1) Malaria patients with AKI (as per the KDIGO criteria mentioned above)
2) Age > 13 years.
Exclusion criteria
1) Pre-existing Kidney diseases.
2) Concomitant febrile illnesses (dengue, viral hepatitis, HIV infection, leptospirosis, filariasis, typhoid fever, tuberculosis, any urinary tract infection.
3) Any concomitant cause leading to AKI (Nephrolithiasis, ureteric calculi, Bladder outlet obstruction, hepato-renal syndrome, vasculitis)
4) Unwilling patients.
Statistical analysis
The data collected, were compiled, tabulated and analysed in terms of descriptive statistics using SPSS version 17.0 software. Continuous variables were presented as mean ± SD and categorical variables were expressed as frequencies and percentages. Categorical data between the groups were compared using Chi square test. A p value <0.05 was considered as statistically significant.
Results and Observations
A total of 725 patients with malaria were hospitalized between August 2009 and March 2017. 57 (7.86%) cases were excluded due to pre-specified criteria.
Out of 668 patients eligible for the study, AKI was diagnosed in 124 (18.6%) patients. 544 (81.43%) patients had no evidence of AKI (Table 2) (Figure 1).


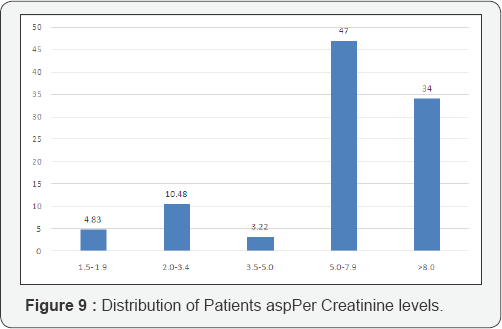
The distribution of MAKI in various follows (Table 2-6) (Figure 2-5). age groups was as
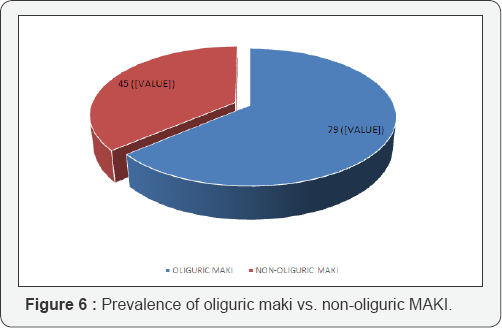
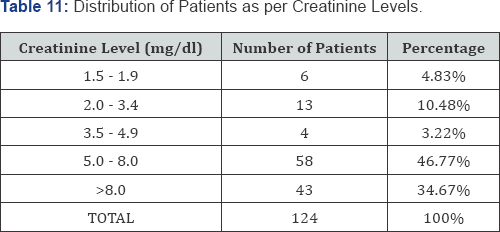
Out of total MAKI cases, oliguric AKI was found in 79 (63.7%) cases and non-oliguric AKI was found in 45 (36.3%) cases (Table 7) (Figure 6).

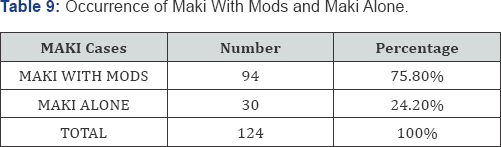
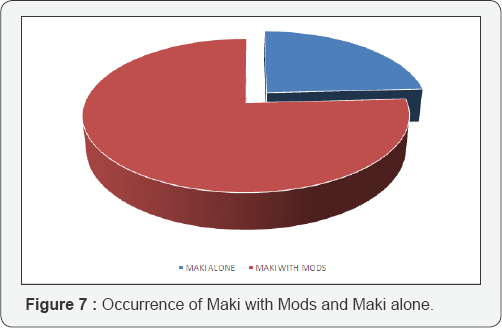
Out of the 124 MAKI cases, MAKI with MODS was seen in 94 (75.8%) patients whereas occurrence of MAKI alone was seen in 30 (24.2%) cases (Table 8-13) (Figure 7-12).

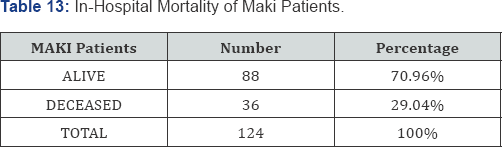


Discussion
Incidence of MAKI
Incidence of MAKI in the present study was 18.6%.
Mehta et al. [9] in their study on this subject noted an incidence of 22.4%. Philips et al. [10] noted an incidence of 17.2% in their study. These findings corroborate with our study. Koopmans et al. [11] in their study on 485 patients, found a low incidence of 8%, whereas Thanachartwet et al. [12] found a high incidence of 44.7%. Variability in the incidence of MAKI is the result of the locality, age group studied and the immunity.
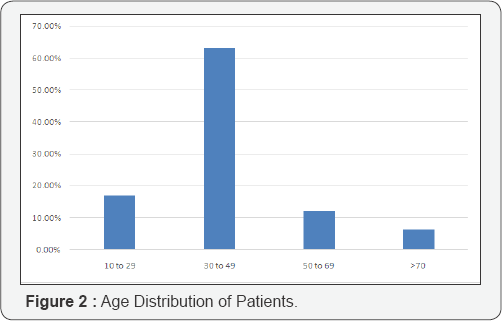
Age
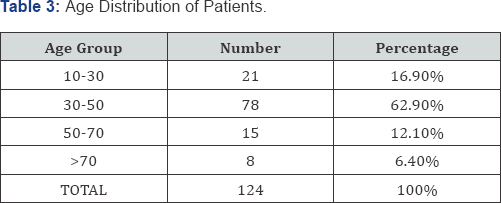
In the present study the age group with most cases of MAKI was 30 to 50 (62.9%), followed by the age group, 10-30 (16.9%), 50-70 (12.1%) and >70 (6.4%).
In the study conducted by Mehta et al. [9] 75% of the cases were in the age group of 20 to 40. In the study conducted by Gupta et al. [13] the mean age of MAKI patients was 38.3 years. In the 3 year study conducted by Prakash et al. [14] the mean age was found to be 36.3 years. Thanachartwet et al. [12], in their study noted a majority of patients were in the age group of 22- 40 with a mean age of 31 years. These studies show similar findings to present study [12]. MAKI is considered a disease of older children and young adults; this is re-affirmed by the present study.
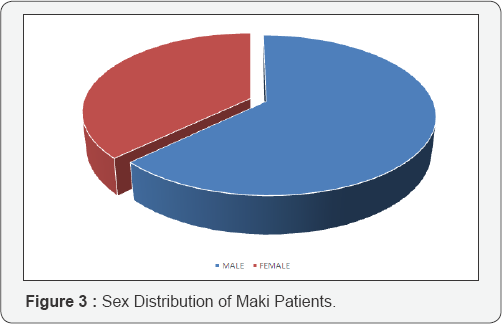
Sex
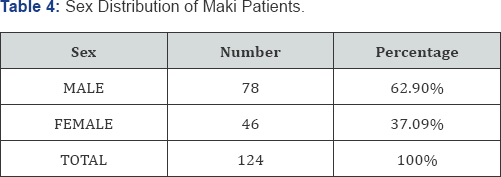
In the present study, there was a higher incidence of MAKI in male population (62.9%) whereas females were affected in 37.09% cases.
In the study conducted by Prakash et al. [14] a similar predominance of male cases was noted (Males- 69.14% and Females- 30.85%). Thanachartwet et al. [12] also noted a majority of male cases (74.3%) as opposed to female cases (25.7%). In the study conducted by Gupta et al. [13] male to female ratio was found to be 4:1.
These findings corroborate with the present study.
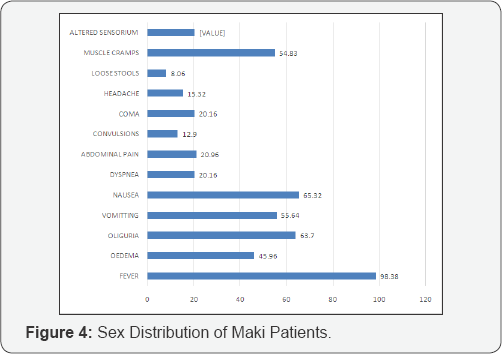
Clinical features
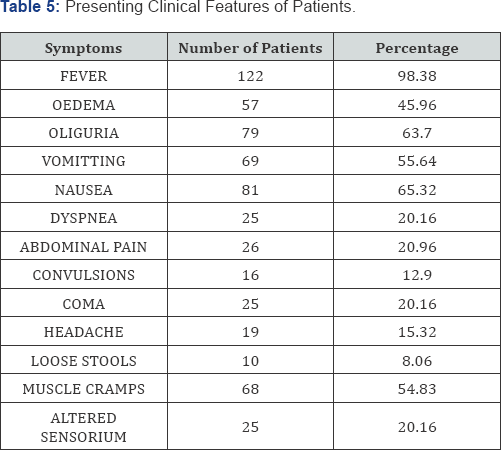
In the present study the commonest presenting features were, fever (98.38%), oliguria (63.7%), nausea (65.32%) and vomiting (55.64%).
In the study by Mehta et al. [9] the commonest features were fever, oliguria, vomiting.
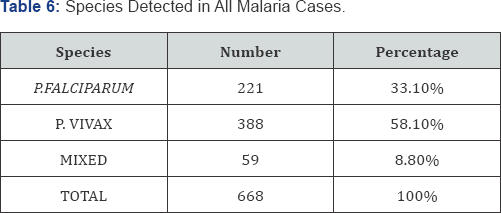
Causative species
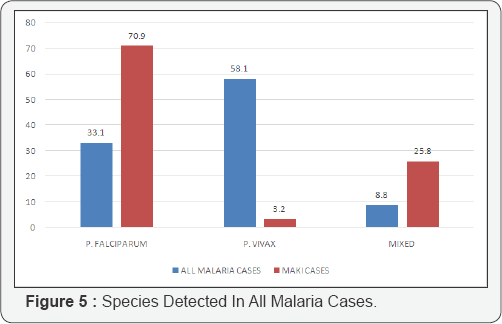
In our study the plasmodium species showing highest causation of MAKI was P. falciparum (70.9%). This was followed by mixed falciparum and vivax infections (25.8%), followed by P vivax infections (3.4%).
The study of Mehta et al. [9] shows similar findings, where commonest cause of MAKI was P. falciparum (66.6%), followed by mixed infections (20.8%) followed by P. vivax (12.5%). In the study by Maheshwari et al. [15]. P falciparum was the causative species in 97.53% cases and P vivax was the responsible species in 2.47% cases. In the study by Naqvi et al. [7]. P. falciparum was the causative species in 97.5% cases and P. vivax was the causative agent in 2.5% cases. Thus P. falciparum is the most common species associated with MAKI.
Oliguria in MAKI
In the present study oliguric AKI was found in 63.7% cases whereas non-oliguric AKI was seen in 36.3% cases.
In the study conducted by Misra et al. [16] the incidence of oliguric AKI (70.2%) was greater than non-oliguric AKI (29.8%) [16]. Prakash et al. [14] noted an incidence of oliguric AKI as 69% and an incidence of non-oliguric AKI as 31%.
These findings tally with the present study. However, in the study conducted by Mehta et al. [9] the incidence of non-oliguric renal failure (58%) was found to be higher than oliguric renal failure (42%).
Associated complications
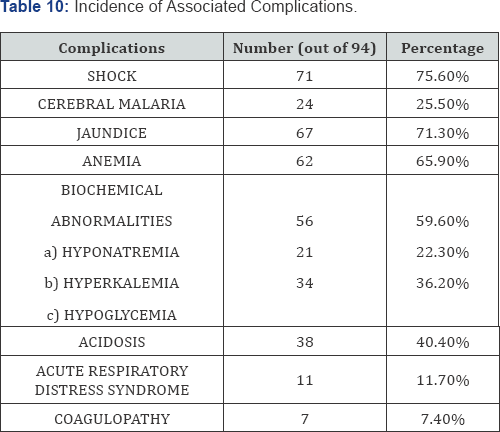
Common complications associated with MAKI were shock (75.6%), cerebral malaria (25.5%), jaundice (71.3%), and anemia (65.9%).
In the study conducted by RE Philips et al. [10] in Thailand, the incidence of co-existence of cerebral malaria and MAKI was recorded as being 30%. In the study conducted by SK Misra et al. [16] in Rourkela, India the incidence of co-existence of cerebral malaria and MAKI was found to be 29%. These findings tally with the current study.
However, a higher incidence of cerebral malaria was noted in the study of Krishnan et al. [17] (40.19%) and Prakash et al. [14] (57.44%).
Misra et al. [16] reported an incidence of 60% with regards to anemia. Wilairtana et al. reported jaundice in more than half their cases. These findings corroborate with our study.
Requirement for dialysis
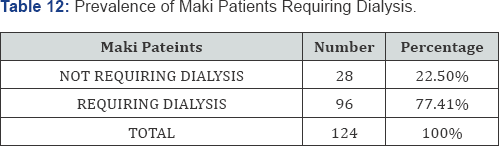
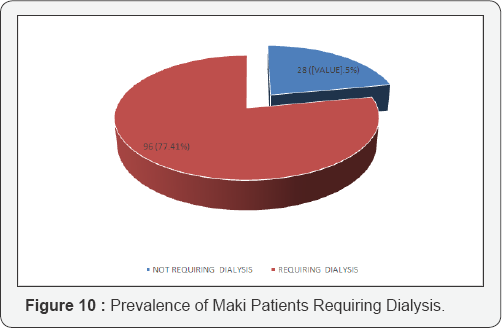
In present study, dialysis was needed by 77.41% patients.
In the study of Gupta et al. [13] 70% of MAKI patients required dialysis. Prakash et al. [14] reported a need for dialysis in 76.6% cases. Mehta et al. [9] noted that in their study, 92% patients required dialysis.
Thus, a high requirement for dialysis was seen in these studies and tallies with the current study.
However, a slightly lower dialysis requirement was seen in the studies conducted by Thanachartwet et al. [13] (45.2%) and Krishnan et al. [17] (36.26%).
MODS in MAKI
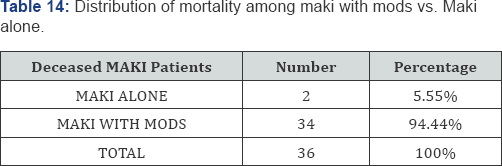
In the current study, a majority of patients showed evidence of Multi-organ dysfunction as defined by the SOFA score (75.8%). Statistically significant mortality was found in those patients that presented with MODS (94.44% of total deceased cases- p value= 0.001937).
These findings corroborate with the study of Gupta et al. [13] where 100% mortality was found in those patients who had MODS with 3, 4 or 5 organ system failures.
Mortality
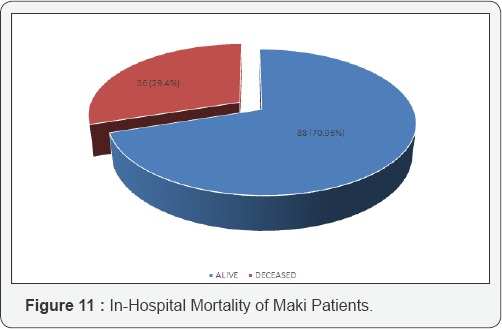
In the present study the in-hospital mortality was found to be 29.04%.
In the study by Thanachartwet et al. [12] the in-hospital mortality was found to be 31.9%. In the study by Mehta et al. [9] the mortality was found to be 29%. The study by Gupta et al. [13] showed a mortality of 30%. These studies corroborate with the present study. Prakash et al. [14] found a mortality rate of 20%.
These studies show findings similar to the current study. References
References
- World Health Organization (2015) Management of severe malaria: A practical handbook. Italy: World Health Organization Press. p: 89.
- Sheehy TW, Reba RC (1967) Complications of falciparum malaria and their treatment. Ann Intern Med 66(4): 807-809.
- Sitprija V (1988) Nephropathy in falciparum malaria. Kidney Int 34(6): 867-877.
- Nguansangiam S, Day NP, Hien TT, Mai NT, Chaisri U, et al. (2007) A quantitative ultrastructural study of renal pathology in fatal Plasmodium falciparum malaria. Trop Med Int Health 12(9): 10371050.
- Mishra SK, Das BS (2008) Malaria and acute kidney injury. Semin Nephrol 28(4): 395-408.
- Trang TT, Phu NH, Vinh H, Hien TT, Cuong BM, et al. (1982) Acute renal failure in patients with severe falciparum malaria. Clinical Infectious Diseases 15(5): 874-880.
- Naqvi R, Ahmad E, Akhtar F, Naqvi A, Rizvi A, et al. (2003) Outcome in severe acute renal failure associated with malaria. Nephrology Dialysis Transplantation 18(9): 1820-1823.
- WHO (2006) Guidelines for the Treatment of Malaria (1st edn). WHO, Geneva, Switzerland.
- Mehta KS, Halankar AR, Makwana PD, Torane PP, Satija PS, et al. (2001) Severe acute renal failure in malaria. J Postgrad Med 47(1): 24-26.
- Philips RE, White NJ, Looareesuwan S (1984) XI International Congress for Tropical Medicine and Malaria, Calgary, Canada.
- Koopmans LC, van Wolfswinkel ME, Hesselink DA, Hoorn EJ, Koelewijn R, et al. (2015) Acute kidney injury in imported Plasmodium falciparum malaria. Malaria Journal 14: 523.
- Thanachartwet V, Desakorn V, Sahassananda D, Win YK, Supaporn T (2013) Acute Renal Failure in Patients with Severe Falciparum Malaria: Using the WHO 2006 and RIFLE Criteria. International Journal of Nephrology.
- Gupta PB, Vadgama P, Bhatt KN, Bhavsar MV, Desai H, et al. (2014) Clinical Profile of Acute Renal Failure in Cases of P Falciparum Malaria in South Gujarat, Int J Res 3(4); 117-123.
- Prakash J, Singh AK, Gujrati S, Maheshwari A (2002) Acute renal failure in Malaria. Changing trends. Indian J Nephrol 12: 113-117
- Maheshwari A, Singh AK, Sinha DK, Tripathi K, Prakash J (2004) Spectrum of renal disease in malaria. J Indian Med Assoc 102(3): 143, 146, 148 passim
- Misra S, Das BS (2008) Malaria and Acute Kidney Injury. Seminars in Nephrology 28 (4): 395-408.
- Krishnan A, Karnad DR (2003) Severe falciparum malaria. an important cause of multiple organ failure in Indian intensive care unit patients. Crit Care Med 31(9): 2278-84.






























