Laparoscopic Nephrectomy for Wilms Tumor
I M Kagantsov*
Republican Children's Hospital, Syktyvkar, Russia
Submission: December 11, 2017; Published: January 18, 2018
*Corresponding author: I M kagantsov, Republican Children's Hospital, Syktyvkar, Russia, Email: ilkagan@rambler.ru
How to cite this article: I M Kagantsovl. Laparoscopic Nephrectomy for Wilms Tumor. JOJ uro & nephron. 2018; 4(5): 555646. DOI:10.19080/JOJUN.2018.04.555646
Abstract
Introduction: Minimally invasive approach in children's surgery has been widely spread for the last decades. However there are very few reports concerning laparoscopic surgery in children in infant with nephroblastoma (NB).
Study design: We retrospectively analyzed 15 children with unilateral II-IY stage NB who underwent radical nephrectomy. The volume of the tumor was calculated by CT scan just before the surgery. Radical nephrectomy via standard transperitoneal approach was performed in 7 and LN was used in 7 children. One patient who underwent tumor resection via lumbar approach was excluded from the study.
Results: All children who were treated by LN had a shorter duration of analgesia and less time standing at the intensive care unit as compared with patients in the open group. One patient died with the II stage of a NB (morphological option of high risk) who had been treated laparoscopicaly. The cause of death was multiple organ failure on the top of administered preoperative PHT.
Discussion: These favorable results are in accordance with previous literature emphasizing that LN for NB in children is feasible and safe.We have highlighted also all above mentioned advantages. Intraoperative blood loss did not exceed 50 ml; Mean duration of the postoperative analgesia was 2.4 days after LN, whereas after open operations the analgesia was continued for 4.5 days. An excellent cosmetic result was achieved in all cases.
Conclusion: Thus, we believe that LN nephroblastoma is feasible and can be recommended to infants with the tumor volume not exceeding 250 cm3. LN can be carried out in the clinics having sufficient equipment for carrying out such interventions with the assistance with experience of laparoscopic surgery.
Keywords: Wilms' tumor; Nephroblastoma; Children; Laparoscopic nephrectomy
Introduction
Minimally invasive approach in children’s surgery and urology has been widely spread for the last decades. Laparoscopy in pediatric oncology is mainly used for biopsy for diagnosis verification. Recently published reports recommend laparoscopic removal of Wilms tumor based on the favorable histological variant and absence of metastases. However, there are very few reports concerning surgery in children at the age of one. Recover success from Wilms’ tumor surpasses 90%; it gives surgeons the opportunity to focus on decrease of surgical injury rate and improvement of cosmetic result.
The aim of our research has become the evaluation of our experience of laparoscopic nephrectomy for Wilms’ tumor in order to prove the feasibility of its conducting in children at the very early age.
Patients and Methods
In the Republic children hospital of Syktyvkar, in the oncological and urology departments there were 15 children with unilateral nephroblastomy (NB) from 2010 to 2015.
Description of Surgical Treatment
The study comprised 15 children with Wilms' tumor; there were 12 (80.0%) boys and 3 (20.0%) girls. The mean age of patients was 21.9 months, 7 children (46.7%) were less than one year old at the time of surgical treatment. The tumor was located on the right in 7 patients (46.7%), on the left in 8 (53.3%). Clinical stage I was defined in one child (6.7%), II in 2 children (13.3%), IV in 4 (26.7%). All the children were treated according to the protocol of International Society of Pediatric Oncology, SIOP 2001). The preoperative polychemotherapy (PHT) was implemented in 7 (46.7%) and 8 (53.3%) patients did not receive PHT before operation. The fine needle biopsy was not carried out before surgery in connection with intended surgical treatment - radical excision of tumor and postoperative morphological verification.
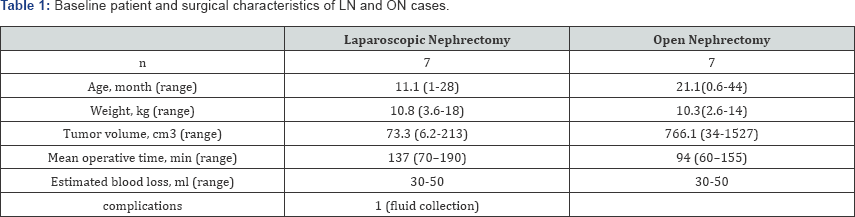
All the patients were done computerized tomography (CT scan) of abdominal and chest cavity. Neoadjuvant PHT was carried out according to SIOP protocol 2001. The volume of the tumor was calculated just before the surgery. The patients were split into two groups: the first one comprised 7 children who underwent surgery via laparoscopic approach. Five children in underwent radical nephrectomy via standard transperitoneal second group were less than one year old (Table 2). It was used approach (Table 1). The second group included 7 patients who CO2 pneumoperitoneum under pressure of 6-12mm.
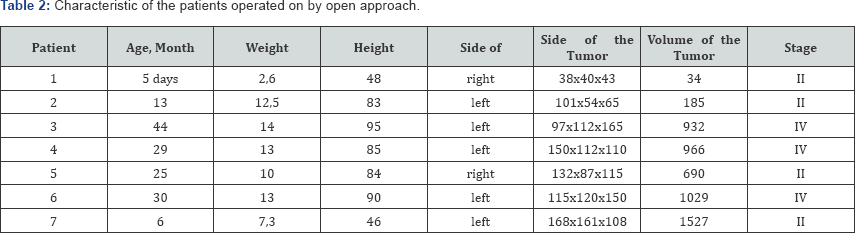
Three ports were used in all cases. The abdominal cavity was checked in order to identify metastases and concomitant pathology. After colon mobilization the renal vein and the artery were exposed with their subsequent clipping and transection. The ureter was exposed on extend down and also ligated and transected. The kidney and perinephric - perirenal fat were exposed en bloc. After full mobilization of the tumor it was placed into a plastic bag which was inserted into the abdominal cavity through the port and it was extracted through transversely expanded wound in the ileac area. One patent with tumor resection via lumbar approach was withdrawn from the study.
Results
In all children the diagnosis of nephroblastoma was confirmed by morphological study (Table 3 & 4). After open surgery children remained in the intensive care unit for an average of 2 days. Estimated blood loss was 30-50ml. The mean duration of operation was 94 (60-155) min. The mean time of analgesia was 4.5 days. PHT was started on average on the 10th day after surgery. All children who were treated laparoscopicaly had the early postoperative period easier; patients were transferred on the first day from the intensive care unit. Estimated blood loss was 30-50 ml. The mean duration of operation was 137 (70-190) min and the mean time of analgesia was 2.4 days. PHT started on average on the 7th day after LN.
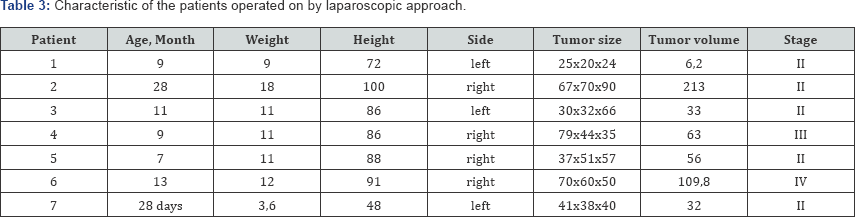
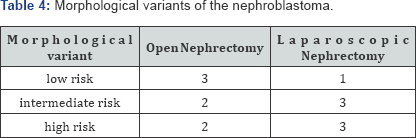
Fluid collection was defined in one patient after LN on the 8th day which required puncture drainage into the bed of a removed kidney for 22 days under ultrasonographic guidance with favorable outcome for a 4-year follow-up. One patient who had been treated laparoscopicaly with the II stage of a NB (morphological option of high risk) died four months later after operation. The cause of death was multiple organs failure on the top of administered preoperative PHT There are not any data about the continued growth of the tumor, implantation of tumor in a postoperative wound in patients of both groups. There were not recorded any remote complications in terms from 12 to 60 months in the course of following-up. The phenomena of renal failure in observed patients are not revealed. The general survival rate has been 92.9%.
Discussion
LN is a standard approach to the treatment of renal tumors in adult patients that is confirmed with the numerous publications in national and international literature. The reports about NB removal via laparoscopic surgery are very few. There are not a lot of studies in terms of this question; the main part has been published lately. Having analyzed available reports in Russian we have found one report about laparoscopic removal of renal tumor [1]. (Scientific research institute of a children's oncology and a hematology of RONTs named after N. N. Blokhina) reported 22 cases of LN: in 20 children with NB and in 2 with kidney cancer. Median age of the operated children was 34 months (of 3 weeks till 16 years). Median time of intervention-62min. Authors note one complication case during operation- inferior vena cava injury which required conversion and a hemotransfusion.
The biggest experience of laparoscopic removal of NB in children for the last eleven years was published by Duarte R et al. [2-4]. On the 26th European congress of children's urologists, in 2015 scientists reported about 23 patients with NB who had been removed Wilms tumor laparoscopically. According to Duarte R, the median operative time in 10 children with I-IY stage of a disease was 170.71±26.07min, the positive surgical edge was in 1 case (4.3%). Recurrence of a tumor is noted in 2 (8.7%) patients: at 1-a local (positive edge) and at 1-metastasis in lungs. Event-free survival for the 10-year period was 91.3% [5]. On the same congress of Leclair MD et al [6] published data of multicenter research from 5 centers of France for 9 years. Authors reported that 34 out of 79 (43%) patients with NB had been selected for minimally invasive surgery, 12 (15.2%) of them had been performed LN.
Romao RL et al. [7] from Toronto reported about 13 LN for kidney tumor, 7 children of them with NB. Authors consider LN an attractive alternative to the open operation in carefully selected cases in children with kidney tumor.
In 2014 Varlet F et al. [8] published the multicenter report from 6 centers of France about LN for kidney tumor in 17 children. Fifteen children had no oncological complications after radical LN with median follow up of 42 months (range of 12 and 77 months). One patient had a local recurrence without intraoperative damage of a tumor. One child with kidney and cellular cancer died 4 years after LN because of pulmonary and cerebral metastases without local recurrence. Cabezali BD et al. [9] have reported 4 patients with NB operated with laparoscopic access whose mean age at the time of intervention was 3 years 7 months (from 23 months to 6 years), two of them were with the stage I, and two with IV stage. All patients have survived more than 3 years of the follow-up.
Liu JB et al. [10] have published data on 7 patients with NB who were managed by laparoscopic approach in two centers of China. Mean age of children at the time of intervention was 1.9±1.5 years (from 3 months to 2 years 9 months). There are also publications with the description of single patients who underwent LN for NB [11]. In published papers of results all authors note that LN for NB in children is feasible and has advantages and disadvantages, minimally invasive operations. On the plus side it is noticed less intraoperative blood loss, less expressed pain syndrome in the postoperative period, shorter hospital stay, and greater cosmetic benefit.
We have highlighted also all above mentioned advantages. Intraoperative blood loss didn’t exceed 50ml in patients, none of the cases required hemotransfusion. Anesthesia was carried out only on the first day after operation for all children, whereas after open operations the analgesia was continued for on average 2.1 days. An excellent cosmetic result was achieved in all cases. We did not find the growth of tumor in the wound after port insertion in our patients, and none of the authors mention the same fact after performing LH with NB in children in the available publications.
Thus, the problem about feasibility of performing LN for NB is resolved nowadays, in spite of few reports. Basically, in all publication papers all the authors pinpoint that the issue which has not been handled yet, is indications for LN. So, having calculated coefficient between height of the child and the largest size of a tumor on CT before surgery, Duarte R et al consider that the operation can be performed in case the value is less than 0.1 [4]. If the tumor size is 10% more than the patient's height, laparoscopy is contraindicated as so there are no clinical data with the coefficient exceeding 0.1. If this dimension is applied to group of our patients treated by laparoscopic surgery, then it also corresponded to 0.1 values. In case of open procedures one of the tumor sizes always exceeded 10cm, at the same time we know that Wilms tumor occurs in children in the first 5 years of life more often, and at this age, height of the child cannot be more than 100cm. Respectively, the coefficient will always be more than 0.1, if tumor size exceeds 10cm. Thus, it turns out that there is no need for coefficient calculation, and it is just a simple statement of fact that the tumor with the size less than 10cm can be removed laparascopicaly.
Almost all authors note that LN can be performed if the tumor does not cross edge of vertebras, according to CT, and does not exceed 8cm in the diameter [4, 6-8, 10].
According to the SIOP 2001 protocol, tumor volume measurement is used according to the mathematical formula in order to evaluate PHT efficiency: V = 4/3π x a/2 x b/2 x c/2 = a x b x c x 0.52.
Using this formula we have obtained the average tumor volume of patients who were selected for LN, equal 73.3cm3 (from 6.2 to 213). In the group of patients who underwent open surgery, there were two children whose tumor volume did not exceed 250cm3; therefore they were retrospectively evaluated by us as candidates for carrying out LN. The tumor volume of the rest of the group exceeded 650cm3. Taking into consideration the fact that according to the SIOP 2001 protocol, all children should be determined the tumor volume; we think that it is more convenient to be guided by this dimension for patient's selection for possible LN. We believe that children with the volume of kidney tumor of less than 250cm3 should be considered as potential patients on carrying out radical nephrectomy by laparoscopic surgery.
In the research we note that duration of LN is higher, than of standard nephrectomy. At the same time, as we are gaining more experience, the operation time of LN tends to reduce. Five out of seven children, who were treated by laparoscopic surgery, were younger than 12 months. It is considered that performing laparoscopic interventions in babies is most difficult. It is bound to limited small «working space», in the abdominal cavity.
Also there are special aspects of carrying out anesthesia in babies in the conditions of the elevated pressure within the abdominal cavity. We use 3mm trocars and a pneumoperitoneum of CO2 under pressure of 6-8mm hg for patients of the first year of life. In our series of interventions we did not note additional difficulties when carrying out LN depending on age of the patient. In our opinion, it is bound to the previously gathered experience of performance of laparoscopic operations in infants (pyeloplasty, ureteropyeloanastomosis, nephrectomy for multicystosis and terminal hydronephrosis).
Conclusion
Thus, we believe that LN nefroblastoma is feasible and can be recommended to children at any age with the tumor volume, not exceeding 250cm3. The decision on carrying out LN for NB has to be made by doctors-oncologists. LN can be carried out in the clinics having sufficient equipment for carrying out such interventions with the assistance of experts with experience of performance of urological reconstructive operations by laparoscopic access.
References
- Volobuyev AV, Rubanskyi MA, Rubanskay MV, Kazancev AP, Kerimov PA, et al. (2011) Laparoscopic surgery for kidney tumors in children. Proceedings of the 2nd Congress for Pediatric Urologists, Moscow, Russia.
- Duarte RJ, Denes FT, Cristofani LM, Odone Filho V, Srougi M, et al. (2004) Laparoscopic nephrectomy for Wilms tumor after chemotherapy: initial experience. J Urol 172(4 pt 1): 1438-1440.
- Duarte RJ, Denes FT, Cristofani LM, Odone Filho V, Srougi M (2006) Further experience with laparoscopic nephrectomy for Wilms tumor after chemotherapy. BJU Int 98(1): 15-19.
- Duarte RJ, Denes FT, Cristofani LM, Srougi M (2009) Laparoscopic nephrectomy for Wilms tumor. Expert Rev Anticancer Ther 9(6): 753761.
- Duarte RJ, Cristofani LM, Denes FT, Srougi M (2015) Eleven year pioneer experience on laparoscopic nephrectomy for treatment of Wilms tumor: Brazilian pioneer experience in a single institution. Proceedings of the 26th ESPU Congress, Prague, Czech Republic, Europe.
- Leclair MD, Floret A, Pellier I, Renaudin Autain K, Lefrancois T, et al. (2015) How many Wilms tumors are amenable to safe laparoscopic total nephrectomy? Proceedings of the 26th ESPU Congress, Prague, Czech Republic, Europe.
- Romao RL, Weber B, Gerstle JT, Grant R, Pippi Salle JL, et al. (2014) Comparison between laparoscopic and open radical nephrectomy for the treatment of primary renal tumors in children: single-center experience over a 5-year period. J Pediatr Urol 10(3): 488-494.
- Varlet F, Petit T, Leclair MD, Lardy H, Geiss S, et al. (2013) Laparoscopic treatment of renal cancer in children: a multicentric study and review of oncologic and surgical complications. J Pediatr Urol 10(3): 500-505.
- Cabezalf BD, Guerrero RF, Lopez VF, Aransay BA, Gomez FA (2014) Laparoscopic approach for Wilms tumor. Surg Laparosc Endosc Percutan Tech 24(1): 22-25.
- Liu JB, Lu ZB, Xiao XM (2015) Laparoscopic Radical Nephrectomy of Wilms Tumor and Renal Cancer in Children: Preliminary Experience from a Two-Center Study in China. J Laparoendosc Adv Surg Tech A 25(6): 516-521.
- Javida PJ, Lendvayb TS, Aciernoa S, Gowa KW (2011) Laparoscopic nephroureterectomy for Wilms tumor: Oncologic considerations. J Pediatr Surg 46(5): 978-982.






























