A Case with Torsion Testis: Restore Testicular Viability after 18 Hours!
Peter T Fawzy*
Department of urology, Aswan University Hospital, Egypt
Submission: March 20, 2017; Published: April 19, 2017
*Correspondence Address: Peter T Fawzy, Department of urology, Aswan University Hospital, Egypt, Email: dr.peter444@gmail.com
How to cite this article: P T Fawzy. A Case with Torsion Testis: Restore Testicular Viability after 18 Hours!. JOJ uro & nephron. 2017; 2(4): 555594. DOI: 10.19080/JOJUN.2017.2.555594.
Abstract
Testicular torsion occurs when the spermatic cord twists, cutting off the testicle's blood supply leading to testicular ischemia. It is either intra vaginal or extra vaginal type. A 17 years old adolescent presented with neglected left testicular torsion more than 18 hours. He had history of severe left testicular pain about 17 hours ago presented by diffuse swelling at left scrotal compartment. Scrotal ultrasonography was carried out and confirmed absent vascularity of left testis. Surgical exploration, detorsion and warm fomentations were done. Little improvement in color was noticed and bilateral orchiopexy was done. Intact good vascularity of left testis was confirmed on scrotal ultrasonography two weeks postoperatively.
Keywords: Testicular torsion; Absent vascularity; Cord twist; Orchiopexy
Introduction
Testicular torsion is considered one of the important causes of acute scrotum condition. It is most common just after birth and during puberty. It occurs in about 1 in 4,000 to 1 per 25,000 males per year before 25 years of age [1]. Although its overall incidence not high, but remain the most common cause of testicular loss in these age groups. Yet, torsion may occasionally occur in men 40-50 years old. Torsion is subdivided into two types, intra vaginal & extra vaginal torsion [2]. Diagnosis of that condition based mainly on presenting symptoms and signs together with scrotal ultrasonography which is considered the single most useful appurtenance to the history and physical examination in the diagnosis of torsion [3]. Once diagnosis confirmed, immediate surgical exploration is mandatory for detorsion and either orchiopexy or orchiectomy depends upon viability of testis.
Case Presentation
A 17 years old adolescent with history of severe left testicular pain for one day (about 18 hours ago) presented by diffuse swelling at left scrotal compartment with diminished pain of left testes at time of presentation. There was associated nausea and vomiting 5 times. There is no previous history of trauma, fever or irritative voiding symptoms. Scrotal ultrasonography was carried out which revealed absent vascularity of left testis with comparable good vascularity of right testis (Figure 1).
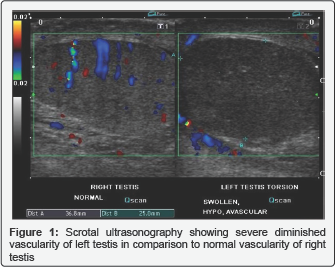
The patient was consented for operation with high possibility of left orchiectomy. Then, immediate scrotal exploration was carried out which revealed intra vaginal torsion (270°) of left testis with marked change in color of left testis (bluish) (Figure 2). Detorsion was done with frequent warm fomentations on left testis and left cord for about 45 minutes. Minute improvement of color was noticed. Decision was made to do left orchiopexy rather than orchiectomy as well as right orchiopexy also. After couple of weeks, postoperative scrotal ultrasonography was done showing intact good vascularity with left testis (Figure 3).
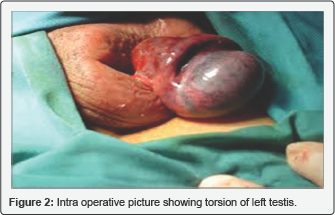
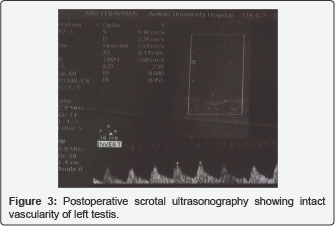
Discussion
Testicular torsion was firstly described by Hunter in 1810 when he noticed an 18 years old man with no previous pain or injury who was “seized with pain” after a few hours of ice- skating followed by testicular atrophy [4].There are two types of testicular torsion; extra vaginal & intra vaginal type. Both types of testicular torsion result from twisting of the spermatic cord leading to testicular ischemia. However, extra vaginal torsion results from twisting of the tunica vaginalis and testicle before complete descent into the scrotum and fusion of the tunica vaginalis to the scrotal wall (more in neonates). On contrary, intra vaginal torsion is the result of inadequate fixation to the testicular gubernaculum during descent of the testis, thus allowing the testis to rotate freely within the tunica vaginalis (more frequent in adolescents). This accounts for the “bell clapper” deformity noted in many cases of testicular torsion [2].The importance of torsion is the resultant testicular ischemia & testicular atrophy later on if not treated. The degree of ischemia is affected by the degree of torsion together with the duration of the event. In animal studies 90 degree twists have been shown to cause no necrosis even after 7 days, whereas 360 degree rotation resulted in necrosis after 12 to 24 hours and 1440 degree rotation resulted in necrosis in only 2 hours [5].
Canine studies have demonstrated destruction of all spermatogenic and Sertoli cells by 6 hours of testicular ischemia and the loss of Leydig cells by 10 hours of ischemia. Clinically, it has been observed that beyond 10 hours of torsion most patients will have significant atrophy unless spontaneous reduction has occurred or the torsion is limited to 180 to 360 degrees of rotation. Complete or severe testicular atrophy is expected in all cases of testicular torsion of greater than 360 degrees lasting for more than 24 hours [6].
Patient with testicular torsion is often present with acute scrotum condition. Acute non-traumatic scrotal discomfort may be related to pathology of the scrotal contents including the testicle, epididymis and cord structures but may also be caused by pathology directly or indirectly related to abdominal or retroperitoneal structures. Testicular tumors with acute hemorrhage with or without a history of apparently minor trauma may be acutely painful. Inflammation of the testicular adnexa (epididymitis) may also cause severe scrotal pain. Torsion of testicular appendages (appendix epididymis or appendix testis) or epididymo-orchitis may also have similar presentations. Incarcerated inguinal hernia may cause symptoms mimicking testicular torsion. Ureteral calculi may present with acute referred testicular pain without associated physical findings [7].
Once the diagnosis is confirmed, immediate surgical exploration. Regardless of whether the testis can be manually detorsed, scrotal exploration and bilateral testicular fixation should still be performed as residual torsion poses a risk to testicular viability. Otherwise, testicular atrophy will subsequently occur.
Conclusion
There is no strict timeout for torsion testis to be removed. Even after 6 hours torsion, you should give chance provided that there is some improvements in color even its minute.
References
- Sharp VJ, Kieran K, Arlen AM (2013) Testicular torsion: diagnosis, evaluation, and management. Am Fam Physician 88(12): 835-840.
- Barthold JS (2012) Abnormalities of the Testis and Scrotum and their Surgical Management. McDougal WS, Kavoussi LR, et al. (Eds.) Campbell-Walsh Urology. (10th edn), WB Saunders, Philadelphia, USA, pp. 642-645.
- AUA (2017) Acute Scrotum. American Urological Association 36: 2017.
- Noske HD, Kraus SW, Altinkilic BM, Weidner W (1998) Historical milestones regarding torsion of the scrotal organs. J Urol 159(1): 1316.
- Marcozzi D, Suner S (2001) The non traumatic, acute scrotum. Emerg Med Clin North Am 19(3): 547-568.
- Thomas WE, Cooper MJ, Crane GA, Lee G, Williamson RC (1984) Testicular exocrine malfunction after torsion. Lancet 2(8416): 13571360.
- Wein AJ, Kavoussi LR, Novick AC (2007) Campbell-Walsh Urology. (9th edn), Elsevier Saunders, Philadelphia, USA.






























