Laparoscopic Approach for a Mucinous Mullerian Retroperitoneal Cystadenoma
Cabello Benavente R*, Alcoba Garcia, Quicios Dorado C, Gomis Goti C, Rodriguez Castro, Martinez Mateo, Garcia Fernandez E and Gonzalez Enguita C
Department of Urology, Fundacion Jimenez Diaz university Hospital, Spain
Submission: January 17, 2017; Published: February 09, 2017
*Corresponding author: Alcoba Garcia, Department of Urology, Fundacion Jimenez Diaz university Hospital, Spain,Tel: 91-550 48 00; Email: pilar.alcoba@fjd.es
How to cite this article: Cabello B R, Alcoba G, Quicios D C, Gomis G C, Rodriguez C,et al. Laparoscopic Approach for a Mucinous Mullerian Retroperitoneal Cystadenoma.JOJ uro & nephron. 2017; 1(4): 555569. DOI: 10.19080/JOJUN.2017.01.555569
Abstract
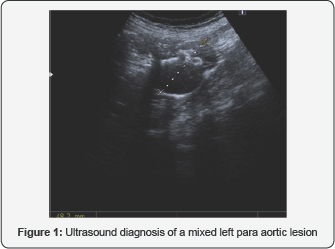
Based on a clinical case, we shall go through the literature concerning a rare tumor, the retroperitoneal mucinous cystadenoma. We present the case of a woman aged 41, with abdominal pain and an ultrasound diagnosis of a mixed left para aortic lesion of 44x34mm (Figure 1), with multiple calcifications. Radical resection is performed by laparoscopic approach. The anatomical pathology result was a mullerian mucinous cystadenoma. Retroperitoneal tumours are uncommon and have a controversial management. The treatment of choice is in-bloc resection; laparoscopic surgery remains a viable technique, with similar results to open surgery, with the advantages of minimally invasive surgery.
Keywords: Cystadenoma; Laparoscopy; Mucinous; Mullerian ducts; Retroperitoneal space
Abbreviations: FNA: Fine-Needle Aspiration; PAS-d: Periodic Acid Schiff Diastase; AB: Alcian Blue; EMA: Epithelial Membrane Antigen
Introduction
Retroperitoneal mucinous cystadenomas are rare neoplasms, and given the scarcity of cases, its pathogenesis and management is still poorly understood. Although classically the excision was done with open surgery, there has been a gradual evolution towards the laparoscopic approach due to the development of this trans-peritoneal technique, as well as a retro-peritoneoscopic one. Lahey & Handfield [1], first classified retroperitoneal cystic lesions in 1924 and Roth, et al [2] in 1977, first described a case of retroperitoneal mucinous cystadenoma.
Case Report
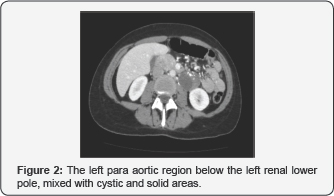
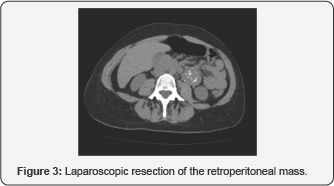
41 years old woman with vague abdominal discomfort and an ovoid lesion of about 48mm found with ultrasound, adjacent to the left renal lower pole, predominantly hypo echoic with arciform hyper echoic areas, that do not depend from the kidney. TAC showed the 44x34mm lesion found at the left para aortic region below the left renal lower pole, mixed with cystic and solid areas, multiple calcifications and low enhancement, in contact with inferior mesenteric artery (Figure 2). Without infiltration of adjacent structures tumor markers, catecholamines, metanephrines in urine and PET, were normal. Laparoscopic resection of the retroperitoneal mass was done, using 4 trocars, carefully dissecting the mass and its thick feeder vessels. No irregularities during surgery or post-operatory, with the exception of febricula, relation with lymphorrhoea, that resolves itself with antibiotic treatment (Figure 3). The anatomopathologic diagnosis concludes that it was a mucinous cystadenoma of endocervical pattern consistent with injury derived from mullerian remnants, with no signs of malignancy.
Discussion
Retroperitoneal mucinous tumours are rare. The largest series of cases of this kind of tumours, are those described by Bifulco G, et al [3], with 48 cases in the international literature [3]. The majority of the cases occur in women, with an average age of 43. Cases in men are rather infrequent, with only 4 cases reported [4], with an average age of 70 [5]. The published cases show tumor size between 5 and 35 cm [3,5], without finding any relation between the size of the cysts and the age of the patient [6]. They are classified into 3 groups according to their behaviour, the degree of cell proliferation, nuclear atypia, and the presence or absence of stromal invasion: Benign, limits or low malignant potential and malignant. Most of them are considered benign tumours, without recurrence after complete surgical removal. Malignant or cystadenocarcinomas, have the characteristic of relapsing and meta-stating [7]. They can become large, causing abdominal symptoms due to compression: pain, distention, nonspecific discomfort and palpable mass. Positive for oestrogen receptors in stromal cells in these types of tumours have been described, which may explain their main incidence in women and their greater frequency in women taking hormone therapy. Their origin is still uncertain. Three theories have been suggested: an origin from teratoma, from heterotopic ovarian tissue or metaplasia of the mesothelial cell lining [8]. In most cases, no ovarian tissue residue is identified and so therefore the most correct histogenetic hypothesis seems to be metaplasia, and more concretely in our case, in which a mullerian differentiation of the tumor is described from remains of the mullerian ducts. In women, Muller ducts develop the fallopian tubes, uterus, cervix and upper 2/3 of the vagina. They degenerate in men and are adjacent Wolfian ducts that give rise to the male reproductive organs. These tumours have been recorded at various locations: the ovaries, pancreas, appendix, bile duct, retro peritoneum and the epididymis.
CT scans are the tests of choice for diagnosis of retroperitoneal pathology, MRI and ultrasound play a secondary role. It is difficult to make an accurate diagnosis of this disease by imaging techniques. Fine-needle aspiration (FNA) may be used to confirm the presence of mucin, but not to determine malignancy or benignity, and usually the utility is low, and therefore is not routinely used in diagnosis.
Radiological findings, together with certain clinical data may help with the diagnosis. Dal Mo Yang, et al. [9], list radiological and clinical features of various retroperitoneal masses, helping the differential diagnosis. In this way, the presence of a unilocular or multilocular lesion in a CT, in an obese woman taking hormone therapy, guides us to the presence of a mullerian cyst. Tumor markers are negative in most cases, although there are recorded cases of high levels of CA 19.9, CA 125, and AFP [3,4]. Therefore, they not very useful in diagnosis and monitoring.
The retroperitoneal mucinous cystadenoma enters the differential diagnosis with cystic masses and retroperitoneal masses, as ovarian and pancreatic mucinous cystic tumours, mesothelial cyst, teratoma cyst, lymphangioma, enteric duplication cyst, bronchogenic cyst, neurogenic tumours and paragangliomas, retroperitoneal pseudomyxoma, perianal mucionous carcinoma, non pancreatic pseudocysts, lymphocele, urinoma and hematomas [4,5,9]. They are usually large, unilobular cysts, sometimes compartmentalized, with thin and smooth surface. They contain a colorless mucinous substance. The microscopic description shows a monolayer of columnar epithelial cells or flattened cells lining on the cyst wall. The columnar cells contain mucin tested positive for “Periodic Acid Schiff Diastase" (PAS-d) and “alcian blue" (AB) at pH 2.5. Immunohistochemistry of the columnar cells show positive for epithelial membrane antigen (EMA) and flattened cells are positive for a mesothelial marker, calretinin. Oestrogen receptors are identified on the stromal cells and similar components to those of ovarian stroma (ovarian stromal-like). They share histologic features with ovarian mucinous cystadenomas but can be found anywhere in the retro peritoneum [6]. The treatment of choice is surgical, with excision of the mass. This prevents infection, recurrence and malignant degeneration [8]. Classically, laparotomy was performed, but currently there are already several reported cases of laparoscopic surgery, being safe and successful approach [10], with less aggression against the immune system, a lower analgesic requirement, less alteration of respiratory dynamics, earlier discharge from hospital and an earlier return to daily life. Although some authors propose carrying out hysterectomy and bilateral salpingo-oophorectomy, there is insufficient evidence, therefore it is not recommended [3]. The value of chemotherapy and radiotherapy is still being studied; some authors recommend the use of chemotherapy in case of cyst rupture or invasion of adjacent organs [4,5].
Conclusion
The retroperitoneal mucinous cystadenoma is a rare tumor and usually benign. Accurate diagnosis is given by an anatomo pathological examination. A full excision of the mass must be carried out, being laparoscopic approach a valid technique and increasingly used. It is not possible to determine a monitoring algorithm, adjuvant treatment or a prognosis estimation, given the shortage of reported cases of this disease.
References
- Handfield Jones R (1924) Retro peritoneal cysts: their pathology diagnosis, and treatment. Br J Surg 12(45): 119-134.
- Roth LM, Ehrlich CE (1997) Mucinous cystadeno carcinoma of the retro peritoneum. Obstet Gynecol 49(4): 486-488.
- Bifulco G, Mandato VD, Giampaolino P, Nappi C, De Cecio R, et al. (2008) Huge primary retroperitoneal mucinous cystadenoma of borderline malignancy mimicking an ovarian mass: Case Report and Review. Anticancer Research 28(4C): 2309-2316.
- Rivera Domínguez A, Cueto Alvarez L, García de Oliva A, Ruiz Garcia T (2011) Cistoadenocarcinoma mucinoso retro peritoneal ocurrido a los 7 años de apendicetomía y hemicolectomía derecha. Radiología 56(3): 268-271.
- Meizoso T, Navas R, Alijo R, Mestre MJ, Raquel Sánchez-Simón, et al. (2009) Cistoadenocarcinoma mucinoso retro peritoneal: Presentación de un caso. Rev Esp Patol 42(4): 305-308.
- Isse K, Harada K, Suzuki Y, Ishiquro K, Sasaki M, et al. (2004) Retro peritoneal mucinous cystadenoma: Report of two cases and review of the literature. Pathology International 54(2): 132-138.
- Min BW, Kim JM, Um JW, Lee ES, Son GS, et al. (2004) The first case of primary retro peritoneal mucinous cystadenoma in Korea: A case report. Korean J Intern Med 19(4): 282-284.
- Yan SL, Lin H, Kuo CL, Wu HS, Huang MH, et al. (2008) Primary retro peritoneal mucinous cystadenoma: Report of a case and review of the literature. World J Gastroenterol 14(37): 5769-5772.
- Yang DM, Jung DH, Kim H, Kang JH, Kim SH, et al. (2004) Retro peritoneal Cystic Masses: CT, Clinical and Pathologic Finding and Literature Review. RadioGraphics 24(5): 1353-1365.
- 10.Ishikawa K, Hirashita T, Araki K, Kitano M, Matsuo S, et al. (2008) A case of retro peritoneal mucinous cystadenoma treated successfully by laparoscopic excision. Surg Laparosc Endosc Percutan Tech 18(5): 516-519.






























