Assessment of Right Ventricular Mechanics Before and After Surgical Myectomy in Patients with Hypertrophic Obstructive Cardiomyopathy, using Two-Dimension Speckle Tracking Echocardiography
Mohamed Alassal1,4, Mohamed Ahmed Ezzat2, Magdy Hassenein7, Mohamed Elanany3, Ibrahim Eltaj4, Yosri Morsi4, Eman Aly Ahmady5 and Abdulaziz Aboshahba4,6
1 Department of cardiothoracic surgery, Benha University, Egypt
2Menoufyia university, Cardiology department, Egypt
3Department of Cardiothoracic surgery, Ain Shams University, Egypt
4 PAAMCC cardiac center, Arar, KSA
5Department of Clinical pathology, Menofia University, Egypt
6 Department of Cardiology, Alazhar university, Cairo, Egypt
7National Heart Institute, Cardiac Surg Department, Egypt
Submission: March 20, 2019; Published: April 12, 2019
*Corresponding author: Mohamed Abdelwahab Alassal, Faculty of medicine, Department of Cardiothoracic surgery, Benha University, Egypt
How to cite this article:Mohamed A, Mohamed AE, Magdy H, Mohamed E, Ibrahim E, Yosri M, Eman AA, Abdulaziz A. Assessment of Right Ventricular Mechanics Before and After Surgical Myectomy in Patients with Hypertrophic Obstructive Cardiomyopathy, using Two-Dimension Speckle Tracking Echocardiography. J Cardiol & Cardiovasc Ther. 2019; 13(4): 555868. DOI: 10.19080/JOCCT.2019.13.555868
Abstract
Objectives: The impairment of right ventricular (RV) myocardial mechanics is evident in hypertrophic cardiomyopathy (HCM). It is independently influenced by LV mechanics and correlated to the severity of LV phenotype. We investigated the changes in RV global and regional deformation following surgical septal myectomy using vector velocity imaging (VVI).
Methods: 25 HCM patients, 68% males with mean age (34.5±12years) were examined before and within two months after surgical myectomy using VVI. In addition to conventional echocardiographic parameters, peak systolic strain (εsys), strain rate (SR) and time to peak εsys (TTP) of regional RV free wall (RVFW) & septal walls were analyzed in longitudinal (long) directions from apical four chamber view and their (Δ) changes were calculated. Similar parameters were quantified in LV from apical 2&4 CH views. Intra-V-delay was defined as SD of TTP and inter-V dyssynchrony was estimated from TTP difference between the most delayed LV segment & RVFW.
Results:All study patients showed improvement of their functional class from NYHA class III to class I and reduction of LVOT gradient to below 20 mmHg except one patient who had 30 mmHg gradients at rest. There was significant reduction of septal thickness, left atrial diameter & volume, LVOT gradient, LVMI, severity of mitral regurgitation, tricuspid annular velocities (P<.0001), RV diameter (P<.02) and increase in LV internal dimensions (P<.001) post myectomy. However, there was significant reduction of RV and LV systolic mechanics; RV global εsys% (from -16.1±4.4 to -12.9±2.9, P<.0001) and LV global εsys%: from -11.6±2.8 to -9.4±2.2%, P<.0001) respectively. The magnitude of reduction of RV strain (Δ RV εsys%, Δ SRsys) was directly correlated LV maximal wall thickness (r=.46, P<.01) and ΔRV dyssynchrony (TTP-SD), (r=.4, P<.05) and negatively correlated to age (r=-.46, P<.02), pre-op RV SRsys (r=-.52, P<.01) and pre-op LV EF% (r=-.43, P<.03). Meanwhile the reduction in RV diastolic mechanics: Δ RV SRe&SRawere directly correlated to PAP and LVOT gradient before surgery (r=.62, P<.002).
Conclusion: Despite improvement of patient functional status and reduction LVOT gradient, RV mechanics shows further deterioration after surgical myectomy. The magnitude of reduction is modestly related to cardiac phenotype and pre-op mechanical function.
Keywords: Hypertrophic obstructive cardiomyopathy; Right ventricle; Speckle tracking
Abbrevations: Δ: Delta Change; CH: Chamber; CMR: Cardiac Magnetic Resonance; LV: Left Ventricle; LVMI: Left Ventricular Mass Index; LVOT: Left Ventricular Outflow; MWT: Maximal Wall Thickness; NYHA: New York Heart Association; PAP: Pulmonary Artery Pressure; RVFW: Right Ventricular Free Wall; SD: Stander Deviation; SRa: Late diastolic strain rate; SRsys: Systolic strain rate; TAPSE: Tricuspid Annular Proximal Systolic Excursion; TDI: Tissue Doppler Imaging; TTP: Time to Peake Strain; VVI: Victor Velocity Imaging
Introduction
Hypertrophic cardiomyopathy is the most prevalent, monogenic heritable cardiovascular disease, affecting approximately1 in 500 people (0.2% of the population) and is the most common cause of sudden cardiac death in young people, including competitive athletes [1,2].
The mechanism of outflow obstruction involves basal septal hypertrophy and flow-mediated displacement of the mitral valve anteriorly into the LVOT [3].
Surgical septal myectomy is the primary treatment option for patients with severe drug-refractory heart failure symptoms and marked functional disability (equivalent to NYHA Class III and IV), associated with obstruction to LV outflow under basal conditions or with physiologic exercise (gradient, ≥50 mm Hg) [4-6].
With surgery, the LVOT is effectively widened, thereby abolishing the gradient and eliminating mitral regurgitation mediated by systolic anterior motion. In nonrandomized comparisons, patients who undergo septal myectomy have better survival than patients who receive nonsurgical management [7].
In patients with HCM and LVOT obstruction, increased LV loading conditions and diastolic dysfunction have an important affect in RV workload [8].
Patients and methods
Study population: A retrospective study included Twenty- Five patients with hypertrophic obstructive cardiomyopathy refractory to medical treatment whom referred to surgical myectomy according to the recommendation of American Heart Association. This study was carried out in a benha, Ainshams, Alazhar university hospitals and national heart institute, Egypt), from August 2011 to December 2018, after approval of Ethics Committee of University Hospitals was obtained.
Inclusion criteria: Patients with Hypertrophic obstructive cardiomyopathy (LVOT pressure gradient more than 50 mmHg at rest or after provocation.) and has Drug refractory symptoms: dyspnea, angina, or syncope (New York Heart Association (NYHA) functional class III–IV).
Exclusion criteria: We excluded Patients with poor echo window, patients with clinical or echo-cardio-graphic evidence of other cardiac diseases such as pericardial, infiltrative or congenital heart disease, or patients with NYHA functional class IV
Analysis of Myocardial Mechanics
a) Baseline (pre-procedural) and follow-up (post-myectomy) strain measurements were performed using 2D tissue- tracking software (Velocity Vector Imaging version 3.0.0; Esaotae Medical Solutions ITALY).
b) From archived 2D echocardiographic studies, Longitudinal wall strain and strain rate of RV were averaged from 6-segment measurements from the Focused RV view, while LV Longitudinal strain parameters were averaged from 12-segment measurements from the apical four-chamber, apical two chamber views.
The data (Pre and after myectomy) were compared to assess the effect of myectomy on the patient´s functional status and effect of myectomy on myocardial mechanics.
Results
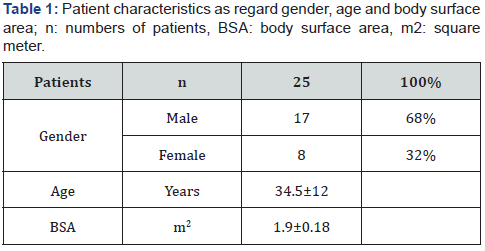
The study included 25 patients, 17 males (68%) and 8 females (32%), the age of them is ranged from 15 to 62 years (mean 34.5±12 years) with body surface area (BSA) ranged from 1.48 to 2.25m2 (mean 1.9±0.18) (Table 1).
All study patients showed improvement of their functional class from NYHA class III to class I and reduction of LVOT gradient to below 20 mmHg except one patient who had 30 mmHg gradients at rest.
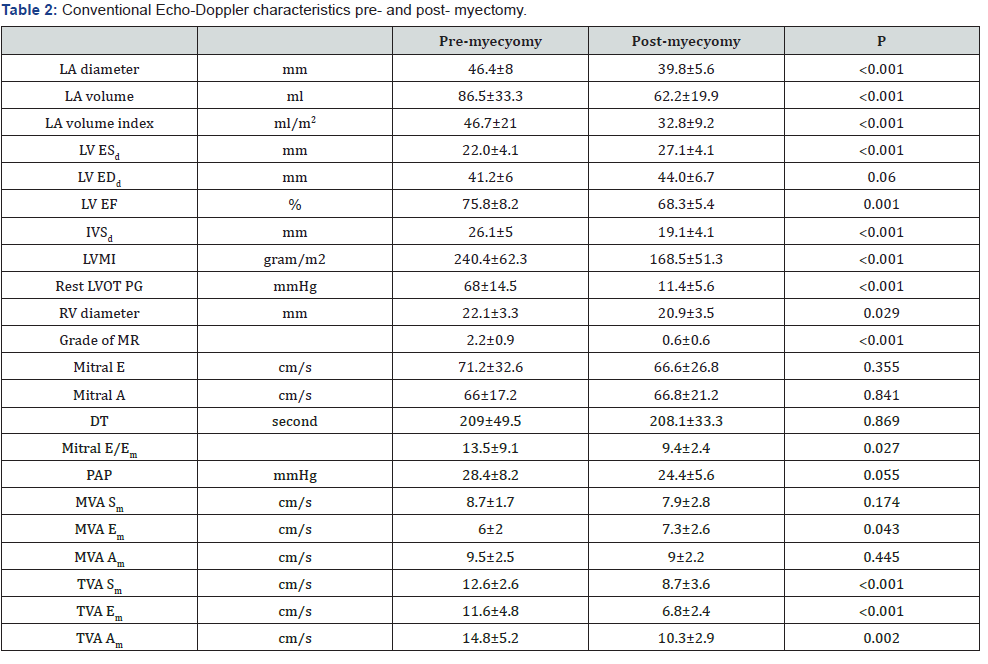
LA: left atrium, LV: left ventricle, ESd: end systolic diameter, EDd: end diastolic diameter, EF: Ejection fraction, IVSd: diastolic inter-ventricular septal diameter, LVMI: left ventricular mass index, LVOT PG: left ventricular outflow tract pressure gradient, RV: right ventricle, MR: mitral regurgitation, E: early diastolic velocity, A: late diastolic velocity, DT: deceleration time, Em: early diastolic tissue Doppler velocity, PAP: estimated pulmonary artery pressure, MVA: mitral valve annular, TVA: tricuspid valve annular, Sm: systolic tissue velocity, Am: late diastolic tissue velocity, mm: millimeter, ml: milliliter, m2: square meter, mmHg: millimeter mercury, cm/s: centimeter per second.
There was significant reduction of septal thickness (from 26.1±5 to 19.1±4; P<.0001), left atrial diameter (from 46.4±7.9 to 39.8±5.6; P<.0001) & volume (from 86.5±33.3 to 62.2±19.9; P<.0001), LVOT gradient (from 67.9±14.5 to 11.4±5.6; P<.0001), LVMI (from 240.4±62.3 to 165±51.3; P<.0001), severity of mitral regurgitation (from 2.2±0.9 to 0.6±0.6; P<.0001), tricuspid annular velocities (P<.0001), RV diameter (from 22.1±3.3 to 20.9±3.5; P<.03) and increase in LV internal dimensions (from 22.0±4.1 to 27.1±4.1; P<.001) post myectomy (Table 2). However, there was significant reduction of RV and LV systolic mechanics; RV global εsys % (from -16.1±4.4 to -12.9±2.9, P<.0001) (Figure 1) and LV global εsys %: (from -11.6±2.8 to -9.4±2.2%, P<.0001) respectively (Table 3).
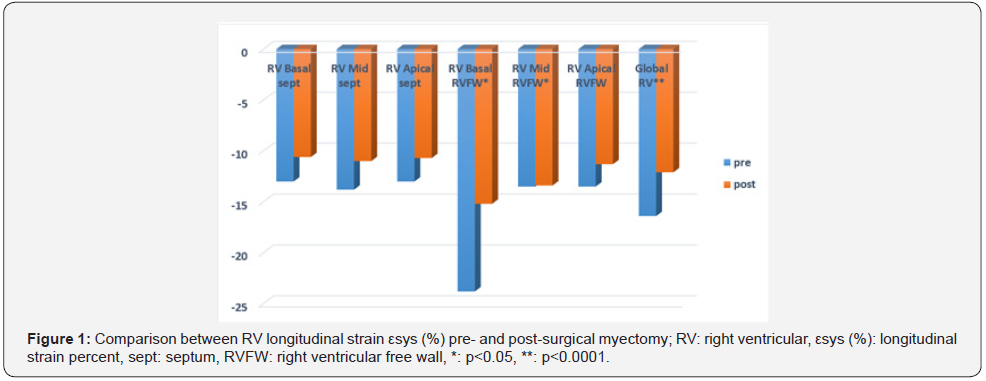
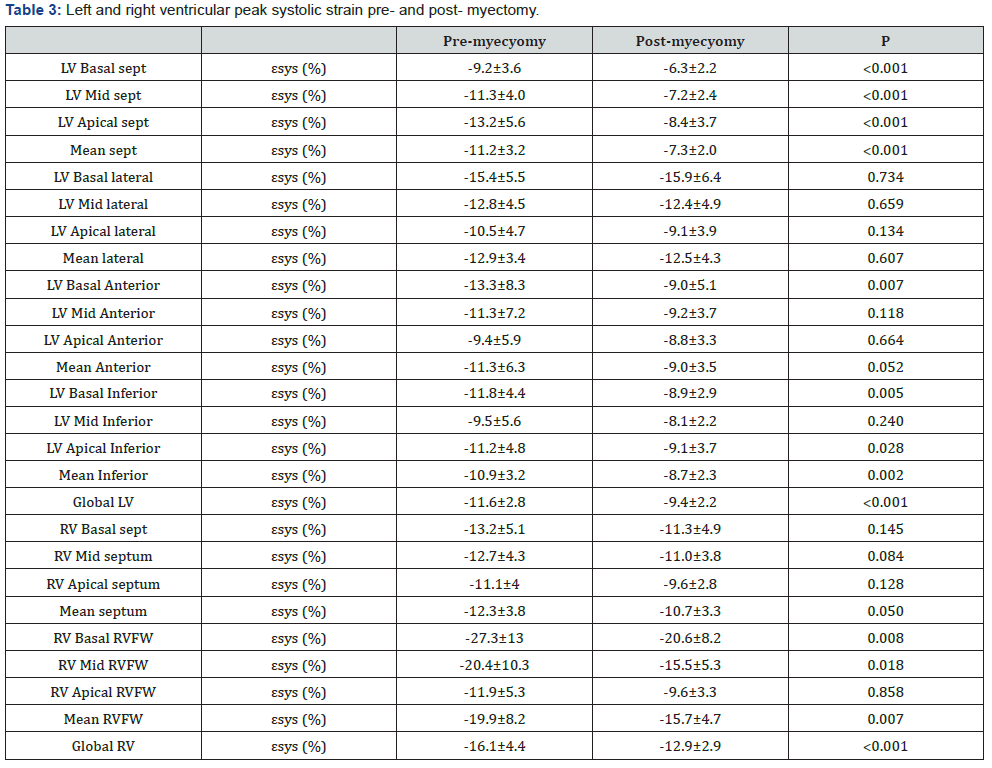
LV: left ventricular, εsys (%): longitudinal strain percent, sept: septum, RVFW: right ventricular free wall.
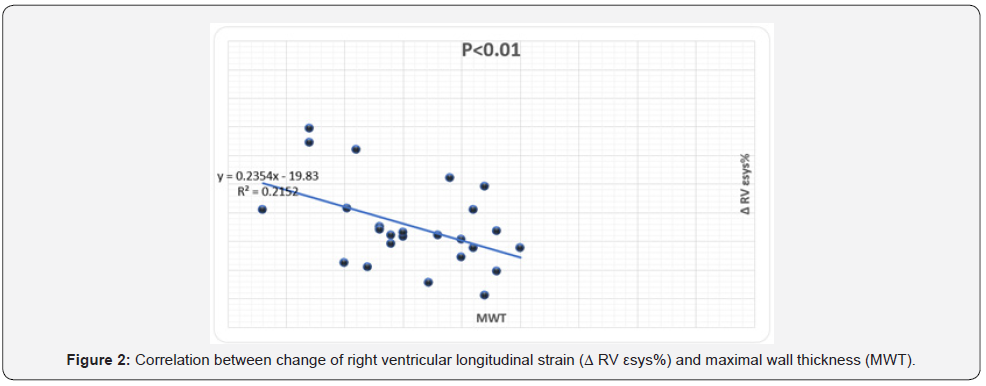
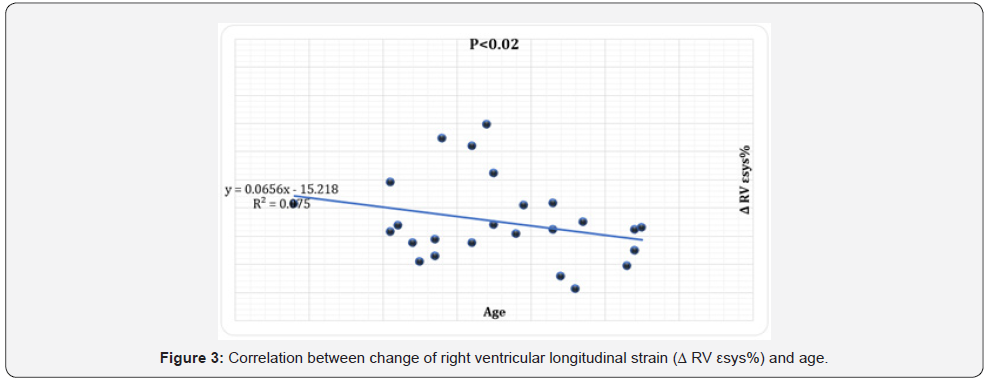
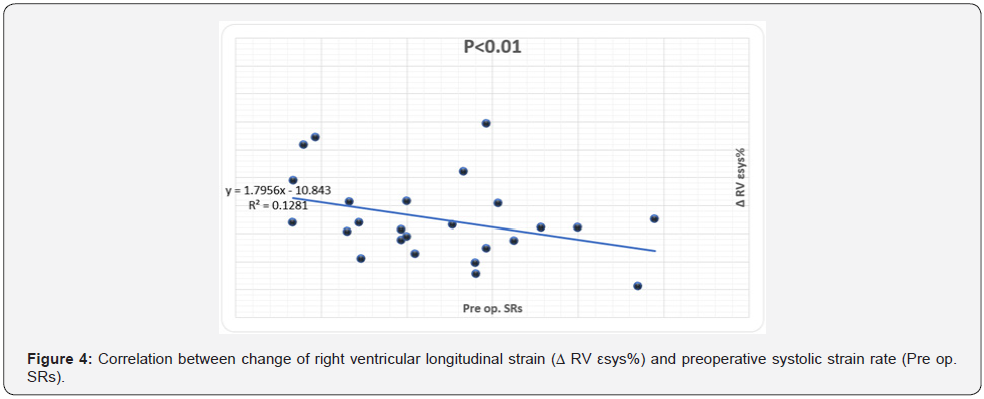
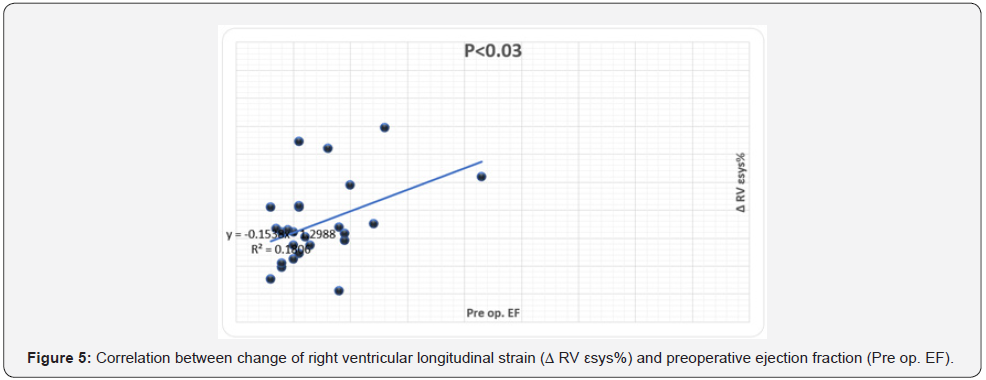
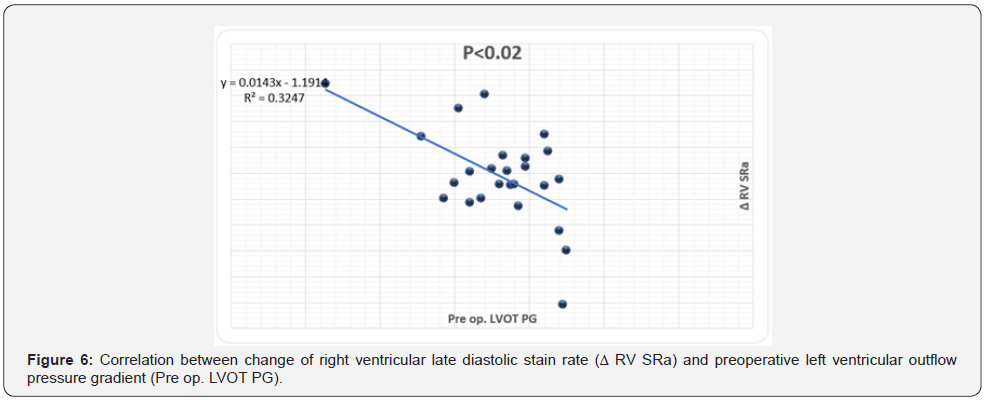
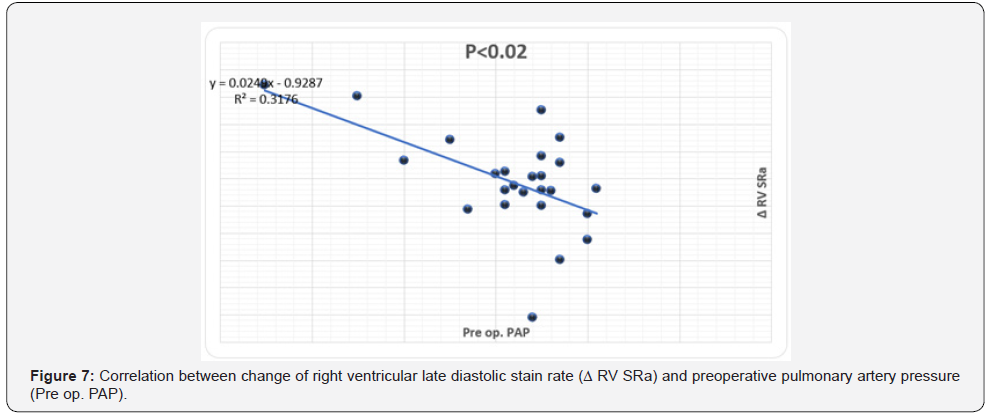
The magnitude of reduction of RV strain (Δ RV εsys%, Δ SRsys) was directly correlated LV maximal wall thickness (r=.46, P<.01) (Figure 2) and negatively correlated to age (r=-.46, P<.02), preop RV SRsys (r=-.52, P<.01) and pre-op LV EF% (r=-.43, P<.03), (Figures 3-5). Meanwhile the reduction in RV diastolic mechanics: Δ RV SRa were directly correlated to PAP and LVOT gradient before surgery (r=.62, P<.002), (Figures 6 & 7).
Discussion
The importance of the right ventricle as a determinant of the prognostic value of right ventricular (RV) function in cardiac surgery outcome, have been largely proved. Speckle-tracking echocardiography is a new technology that allows quantification of myocardial regional deformation. The main advantage compared with tissue Doppler imaging is its angle independency [9]. In this study we found significant reduction in RV global strain after surgical myectomy despite improvement of NYHA functional class from NYHA class III to class I and significant reduction of LVOT gradient at rest, significant reduction of septal thickness, left atrial diameter& volume, LVMI and severity of mitral regurgitation.
Assessment of right ventricular function post cardiac surgery has been investigated in several studies.
Nguyen T, et al. [10] showed significant reduction in RV longitudinal function when assessed by TAPSE (23 ± 3 Vs 15 ± 4; P < 0.001) [10].
Schuuring MJ, et al. [11] demonstrated found a significant decline in RVF using TAPSE and TDI (S’), after cardiac surgery in all adult congenital heart disease patients. With no differences between patients who underwent surgery on right, left or both sides of the heart. (TAPSE 22 ± 5 Vs 13 ± 3 mm; P<0.01) & (RV S’ 11 ± 4 Vs 8 ± 2 cm/s; P<0.01) [11].
Steffen HJ, et al. [12] demonstrated found a significant decline in RVF using TAPSE and TDI (S’),3, 6 and 12 months after cardiac surgery, TAPSE (15.5+3, 16.5+3, and 18.5+4 mm at 3, 6, and 12 months, respectively) and S’ (11.9+2, 12+2, and 12.8+3 cm/s at 3, 6, and 12 months, respectively) (P<0.01). This declining was not observed when assessment of RVEF was done using 3D echo [12].
Orde Sam, et al. [13] showed significant reduction of right ventricular longitudinal strain from -25.3% to -15.5% (P<0.001), RV longitudinal strain rate from -1.5 to -0.94 (P<0.001) and RV diastolic function assessed by speckle tracking was similarly reduced: RV longitudinal strain rate early relaxation from 1.4 to 0.92 (P<0.001) when assessed 48h post cardiac surgery [13].
Raina A, et al. [14] demonstrated reduction of longitudinal function post cardiac surgery when assessed by TAPSE while RV FAC was lower but still in normal range [14].
Exact explanation of deterioration of RV longitudinal function is not well known but in our patients it seems that RV systolic function is correlated to phenotype of HCM, age and preoperative mechanics.
Limitation
The main limitations of our study is the relatively small number of patients examined and this is due to relatively rare cases in a single referral tertiary center, short period of follow up and absence of a gold standard method for detection of the extend of myocardial fibrosis and disarray (CMR) to compare between the extent of myocardial involvement in each segment and its actual response after surgical myectomy.
Conclusion
Despite improvement of patient functional status and reduction LVOT gradient, RV mechanics shows further deterioration after surgical myectomy. The magnitude of reduction is modestly related to cardiac phenotype and pre-op mechanical function.
References
- Maron BJ, McKenna WJ, Danielson GK, Kappenberger LJ, Kuhn HJ, et al. (2003) American College of Cardiology/European Society of Cardiology clinical expert consensus document on hypertrophic cardiomyopathy. A report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents and the European Society of Cardiology Committee for Practice Guidelines. J Am Coll Cardiol 42(9): 1687-1713.
- Spirito P, Seidman CE, McKenna WJ, Maron BJ (1997) The management of hypertrophic cardiomyopathy. N Engl J Med 336(11): 775-785.
- Ommen SR (2013) Hypertrophic cardiomyopathy”, Joseph G. Murphy& Margaret A.Lioyd , Myo clinic cardiology - concise textbook 4th edition 900-100.
- Woo A, Williams WG, Choi R, Wigle ED, Rozenblyum E, et al. (2005) Clinical and echocardiographic determinants of long-term survival following surgical myectomy in obstructive hypertrophic cardiomyopathy. Circulation 111(16): 2033-2041.
- Ommen SR, Maron BJ, Olivotto I, Maron MS, Cecchi F, et al. (2005) Longterm effects of surgical septal myectomy on survival in patients with obstructive hypertrophic cardiomyopathy. J Am Coll Cardiol 46(3): 470-476.
- Maron BJ, Dearani JA, Ommen SR, Maron MS, Schaff HV, et al. (2004) The case for surgery in obstructive hypertrophic cardiomyopathy. J Am Coll Cardiol 44(10): 2044-2053.
- Ommen SR (2013),” Hypertrophic cardiomyopathy”, Joseph G. Murphy & Margaret A Lioyd, Myo clinic cardiology - concise textbook 4th edition 905-100.
- Timmer SA, Knaapen P, Germans T, Lubberink M, Dijkmans PA, et al. (2011) Right ventricular energetics in patients with hypertrophic cardiomyopathy and the effect of alcohol septal ablation. J Card Fail 17(10): 827-831.
- Jurcut R, Giusca S, La Gerche A, Vasile S, Ginghina C, et al. (2010) The echocardiographic assessment of the right ventricle: What to do in 2010? Eur J Echocardiogr 11(2): 81-96.
- Nguyen T, Cao L, Movahed A (2014) Altered Right Ventricular Contractile Pattern after Cardiac Surgery: Monitoring of Septal Function Is Essential. Echocardiography 31(9): 1159-1165.
- Schuuring MJ, Bolmers PP, Mulder BJ, de Bruin-Bon RA, Koolbergen DR, et al. (2011) Right Ventricular Function Declines after Cardiac Surgery in Adult Patients with Congenital Heart Disease. Int J Cardiovasc Imaging 28(4): 755-762.
- Steffen HJ, Kalverkamp S, Zayat R, Autschbach R, Spillner JW, et al. (2018) Is Systolic Right Ventricular Function Reduced after Thoracic Non-Cardiac Surgery? A Propensity Matched Echocardiographic Analysis. Ann Thorac Cardiovasc Surg 24(5): 238-246.
- Orde Sam, Oh J, Stulak J, Suri R, Pulido J, et al. (2013) Effect of Cardiac Surgery on Right Ventricular Function, A Speckle Tracking Echocardiography Study. Critical Care Medicine 41(12).
- Raina A, Vaidya A, Gertz ZM, Susan Chambers, Forfia PR (2013) Marked Changes in Right Ventricular Contractile Pattern after Cardiothoracic Surgery: Implications for Post-Surgical Assessment of Right Ventricular Function. J Heart Lung Transplant 32(8): 777-783.






























