Pulmonary Metastasis Due to Superficial Transitional Cell Carcinoma of Urinary Bladder, A Rare Case Report and Literature Review
Ikram Ul Haq Chaudhry*, Irfan S Khan, Ahsan Cheema, Hadi Mutairi and Ibrahim Oraifi
Division of Chest Surgery, Urology and Pathology, King Fahad Specialist Hospital, Saud Arabia
Submission: September 28, 2018; Published: October 12, 2018
*Corresponding author: Ikram Ul Haq Chaudhry, Division of Chest Surgery, Urology and Pathology, King Fahad Specialist Hospital, Dammam, Saud Arabia.
How to cite this article: Ikram U H C, Irfan S K, Ahsan C, Hadi M, Ibrahim O. Pulmonary Metastasis Due to Superficial Transitional Cell Carcinoma of Urinary Bladder, A Rare Case Report and Literature Review. J Anest & Inten Care Med. 2018; 7(5): 555722. DOI: 10.19080/JAICM.2018.07.555722
Abstract
Urinary bladder Transitional Cell (TCC) carcinoma usually remains superficial. Only 5-20% cases can progress to muscle invasion and metastasis. Liver, lung, mediastinum and bone are the common sites for metastasis. Although long term survival of patients with metastasis is poor. We present a rare case of TCC with pulmonary nodule which treated with Video Assisted Thoracoscopic (VATS) lung resection. Histopathology report revealed transitional cell carcinoma of urinary bladder origin. Patient remained disease free to date as her CT scan of thorax and follow up cystoscopic examinations showed no recurrence.
Keywords: TCC; Urinary bladder; Metastasis; Lung; VATS; Surgery
Introduction
TCC is the most common malignant neoplasm of urinary tract. Overall incidence of urinary bladder cancer is 10.1 and 2.5 per 100,000 in male and female respectively [1]. American cancer society reported 68,810 new cases of TCC in 2008. Seventy percent of newly diagnosed TCC cases have superficial disease (stage Ta, T1, or carcinoma in situ) [2]. Due to recent advances in chemotherapy and early diagnosis survival rate has increased significantly in patients with urinary bladder cancer and this has led to increase in the number of patients developing a second primary cancer which is almost 16% according to NC I surveillance [3]. The stage and grade of TCC has great impact on survival and prognosis. We present two cases of urinary bladder cancer with pulmonary nodule. Pulmonary nodules were resected by Video Assisted Thoracoscopic Surgery (VATS) and histopathology report revealed metastatic TCC of urinary bladder origin.
Case
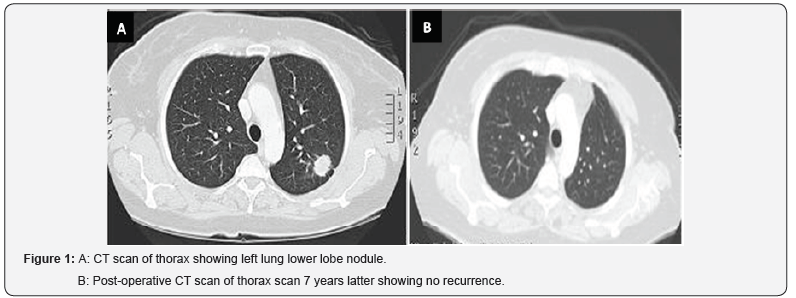
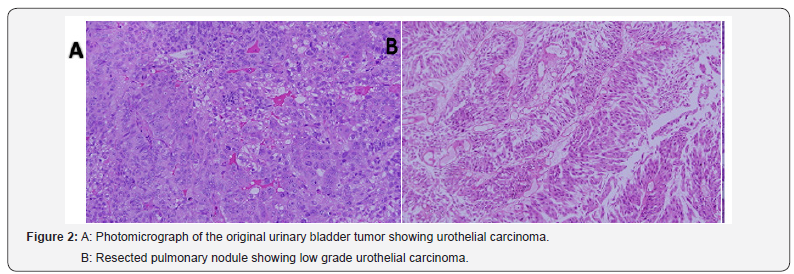
52 years old lady had nine years history of superficial urothelial carcinoma of the urinary bladder. She was treated with intravesical BCG therapy; follow up cystoscopic and biopsy showed no recurrence. In 2010, CT scan of the chest showed right upper lobe pulmonary lesion (Figure 1A). By VATS pulmonary nodule was resected. Her post-operative recovery was uneventful. Histopathology report showed metastatic TCC of urinary bladder origin (Figures 2A & 2B). Recent CT scan of chest showed no evidence of recurrence (Figures 1A & 1B).
Discussion
Urinary bladder cancer is more common in smokers and in those who are exposed to aromatic amines e.g. working in paint, iron and aluminum, printing, tar and gas industries [4]. Incidence of bladder cancer is related to duration and number of cigarette packs consumed. Two out of three urinary bladder cancer patients are smokers. In another study Livi & Germic reported smoking related risk of two primary cancers is 10-20 % [5,6].
Superficial bladder cancer by nature remains confined to superficial layers but local recurrence is more common. TCC commonly remains confined to urinary bladder; distal spread is usually via lymphatic. The most common sites of distant metastasis are distant lymph nodes, liver, lung, mediastinum, bone and adrenal gland. Pulmonary metastasis is most of the time well defined solitary and without any calcification or cavitation. Only 4 % of lung lesions progresses to cavitation due to necrosis. The important prognostic factors for survival are site of metastasis and response to advent chemotherapy [7,8].
As the patients with lung and soft tissue metastasis has better survival as compared to those who have liver and bone metastasis. Prognosis is poor if Karnosfsky performance status is less than 80 which includes weight loss, elevated serum alkaline phosphatase or LDH levels and non TCC histopathology [9,10]. Metastatic site can reveal adenocarcinoma or squamous cell carcinoma this can be reflection of stem cell function of TCC or the second primary [11]. Pulmonary nodule in the presence of TCC should be differentiated from second primary lung carcinoma. Some urological surgical procedures such as ureterosigmoidostomy may induce second primary neoplasm [12]. Superficial bladder cancer rarely progresses to invasive or metastasis stage. Sometimes superficial bladder cancer patient can have second primary lung cancer Finnish cancer registry data showed 1300 second primary cancer patients in 77548 lung cancer patients including 140 cases of urinary bladder cancer [13].
Diagnosis of urinary bladder cancer is based on several factors including symptoms, imaging investigations including IVU, USS and CT will clinch the diagnosis. Urine cytology may be positive for malignant cells in high grade tumors and in cases of CIS. Preoperative work up and correct diagnosis and staging using proper diagnostic modalities are essential for treatment and future prognosis. Superficial urinary bladder cancer rarely progresses to invasive or metastasis stage though it is more common cancer in urogenital system, only a few cases of superficial urinary bladder cancer with pulmonary metastasis have been reported in literature [14-16].
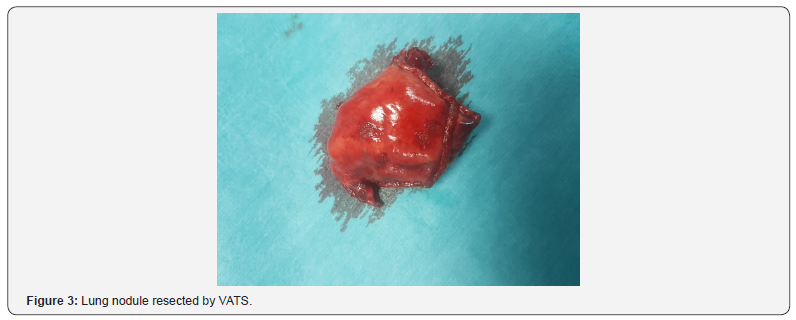
In conclusion we report a rare case of lung metastasis from TCC of urinary bladder. This was resected by VATS, after seven years patient CT scan thorax showed no recurrence (Figure 3). Mainstay of treatment for superficial TCC is bladder sparing surgery followed by intravesical chemotherapy. Although lung metastasis is rare after TCC of urinary bladder still surgical resection is mandatory and can provide excellent long-term survival.
References
- David W Dougherty, Victoria K Gonsorcik, Lewis E Harpster, J C Trussell, Joseph J Drabick (2009) Superficial bladder cancer metastasis to the lungs: two case reports and review of the literature. Urology 73(1): 210.
- American cancer society: cancer facts and figures (2008) Atlanta, American cancer society.
- Khanal A, Budhathoki N, Sing VP, Shah BK (2017) Second primary malignancy in bladder carcinoma. A population-based study. Anticancer Res 37(4): 2033-2036.
- J Lorenzo Bermejo J Sundquist and K Hemminki (2009) Bladder cancer in cancer patients: population-based estimates from a large Swedish study. British Journal of Cancer 101(7): 1091-1099.
- Berenn P, Pogillot O, Cordier S, Greiser E, Schill W, et al. (2000) Cigarette smoking and bladder cancer in men, pooled analysis of 11 case - control study. Int J Cancer 86(2): 289-294.
- Yun YH, Jung KW, Bae JM, Lee JS, Shin SA, et al. (2005) Cigarette smoking and Cancer incidence in adult men: national health insurance corporation study. Cancer Detect Prev 29(1): 15-24.
- Alexandra PW, Sanders C, Nah H (1990) Cavitary pulmonary metastasis in transitional cell carcinoma of urinary bladder. AJR 154(3): 493-494.
- Anil Kurian, Jason lee, Abraham Born (2011) Urothelial blabber cancer with cavitatory lung lesion. Can Resir J 18(3): e46-e47.
- Geller Nl, Sternberg CN, Peneberg D, Scher H, Yagoda A et al. (1991) Prognostic factors for survival of patients with advanced urothelial tumors treated with methotrexate, vinblastine, doxorubicin and cisplatin chemotherapy. Cancer 67(6): 1525-1531.
- Raghavan D, Shiplley WU, Garnick MB, Russell PJ, Richie JP, et al. (1990) Biology and management of bladder cancer. New Eng J Med 7: 706- 709.
- Dapeeka Parimoo, Derek Raghavan (2000) Progress in the management of metastatic bladder cancer. Cancer Control (2000): 7(4): 347-356.
- Ray P, Sharifi R, Ortolano V, Guin P (1938) Involvement of genitourinary system in multiple malignant primary neoplasm’s review. J Clin Oncol 1(9): 574-581.
- Teppo L, Salminen E, Pukkala E (2001) Risk of new primary cancer among patients with lung cancer of different histological type. Eur J Cancer 37(5): 613-619.
- Tanis PJ, Zondervan PA, Van de Wiel BA (2005) Surgery for isolated lung metastasis in two patients with bladder cancer. Urology 66: 881
- Koh KB, Rogawski K, Smith PH (1994) Cavitating pulmonary metastasis from superficial transitional cell carcinoma of urinary bladder. Scand J Urol Nephrol 28: 201-202.
- David W Dogherty, Victoria K, Gonosorcik Lewis E, Harpester JC, Trussel Joseph J, et al. (2009) Superficial bladder cancer metastatic to the lungs: two case reports and review of literature. Urology 73(1): 210.






























