Permissive Hypotension: What’s New in Fluid Resuscitation in the Management of Hemorrhagic Shock?
Ozgur Karcioglu*
Istanbul Research and Training Hospital, Department of Emergency Medicine, Turkey
Submission: May 29, 2018; Published: July 19, 2018
*Corresponding author: Ozgur Karcioglu, Emergency Physician, Istanbul Research and Training Hospital, Department of Emergency Medicine, Istanbul, Turkey.
How to cite this article: Ozgur Karcioglu. Permissive Hypotension: What’s New in Fluid Resuscitation in the Management of Hemorrhagic Shock?. J Anest & Inten Care Med. 2018; 7(2): 555708. DOI: 10.19080/JAICM.2018.07.555708
Abstract
This review addresses up-to-date recommendations on evaluation and management of the patient with hemorrhagic shock in the emergency setting. The endpoints recognized to monitor perfusion and oxygenation status of the victim are presented. Although it is traditionally recommended that patients should be `filled in` using crystalloid and even colloids, numerous complications secondary to such policy has led to a current trend towards permissive hypotension in trauma patients as opposed to over resuscitation. Day by day, the policy of judicious fluid administration to maintain the mean arterial pressure with lower-than-usual mean arterial pressures (around 65 mmHg) is set as the standard of care.
Keywords:Fluid resuscitation; Management; Hemorrhagic shock; Trauma; Permissive hypotension
Introduction
It is not a prophecy that there will be much more mass casualties affecting human being in this century. Additionally, hi-tech mass transportation using imported technologies are known to cause much more frequent incidents in developing countries, along with other man-made disasters. Therefore, it is not surprising to see that trauma resuscitation is a hot debate again nowadays. Primary care and emergency physicians should be well prepared to encounter a higher toll of victims with blood loss and Hemorrhagic Shock (HS) resulting from mass casualties as well as from individual accidents and suicides.
In brief, shock is a condition caused by inadequate blood flow to meet the metabolic demands of tissues to maintain basic processes for life. Shock is the final common pathway of many kinds of insults, classically including hypovolemic, septic, cardiac, or neurologic impairment. In the recent decades, the term `distributive` shock is used more commonly to comprise anaphylactic, septic and neurogenic subtypes, while `obstructive` shock is used to depict the low-perfusion state in conditions such as tension pneumothorax, cardiac tamponade, and massive pulmonary embolism. Among all, HS is one of the commonest causes of death in victims of trauma following Traumatic Brain Injury (TBI) [1,2]. Therefore, the key principle in the primary survey is to evaluate the oxygenation and ventilation, followed by the hemodynamic status and tissue perfusion of the victim. Another rule of thumb involves continuous monitoring for hemorrhage and efficacy of resuscitation [3].
Markers and endpoints of fluid resuscitation in HS
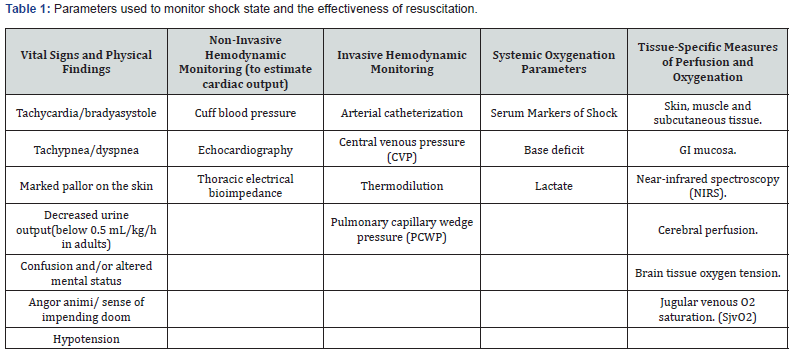
Roughly, monitoring adjuncts in shock management can be classified as hemodynamic vs. oxygenation parameters, and can also be divided as non-invasive and invasive tools as summarized in Table 1. Besides heart rate and Blood Pressure (BP), clinical assessment for blood loss should employ capillary refill, skin temperature and color, mental status, and urine output [4]. Unfortunately, these parameters are not sensitive or specific to identify early hemorrhage [3]. Among many tools proposed to evaluate severity of shock and resuscitation. efficacy so far (Table 1), few proved practical and routinely feasible in the Emergency Department (ED) setting. BP is known to be a poor predictor for tissue O2 delivery (DO2). A decrease in BP only occurs in Class III shock in the classification employed in ATLS that heralds impending multiorgan failure and consequently, a grave outcome. Thus, it is a rather late sign to screen for a proper trauma management strategy. Besides the `classical` vital signs, lactate and Base Deficit (BD) can be regarded practical and useful in the acute setting. Lactate and BD are the most commonly utilized indicators which yield accurate information on anaerobic glycolysis. Lactate is a measure of O2 debt, which is an important characteristic of shock states. BD is a rough measure of global tissue acidosis which is an indirect indicator of tissue perfusion. It was pointed out that BD could remain abnormal despite improvements in Mean Arterial Pressure (MAP), CO, mixed venous O2 saturation, and oxygen extraction in an animal model of HS [5].
Emergent management of shock in trauma
Known or suspected injuries, vital signs, extent of hemorrhage, available resources, and need for transfer guide the management in the ED and trauma bay. The search for the source of hemorrhage should occur simultaneously with the institution of volume infusion. A minimum of two 16-gauge intravenous catheters should be established in adults [4]. New and practical venous access options such as intraosseous devices supplanted the `traditional` venous cut-down. Resuscitation of patients with HS traditionally consisted of large volumes of fluids in order to restore tissue perfusion. Most respected protocols i.e. Advanced Trauma Life Support (ATLS) recommend to begin with infusing 2 L of crystalloid followed by packed Red Blood Cells (RBC) and plasma tailored for the patient’s general response and blood pressure (BP) [4]. However, there is virtually no scientific evidence proving the need for prompt Fluid Resuscitation (FR) in HS [6]. If the patient responds to the initial volume adequately and rapidly, one can say that the injury was not very severe and blood loss was relatively small. In these cases an infusion of a balanced saline solution can be sufficient treatment.
Which fluid to infuse?
If resuscitation of all critically ill patients is taken into account, researchers point out that the choice of fluid has a small or no effect on mortality [7,8]. In contrast, when only resuscitation of trauma patients is considered, the results are very similar and suggest that resuscitation with colloids carries an increased mortality. Crystalloids therefore should remain the fluid of choice for the resuscitation of trauma patients in HS. ATLS guidelines recommend administration of an aggressive FR with an initial 2-L bolus of crystalloids. Resuscitation continues with repeated boluses of Lactated Ringer’s (LR) solution, blood (if necessary), along with a thorough search of reversible sources of blood loss [4]. NS solution is also a reasonable choice for resuscitation of hypovolemic patients. Previous concerns about inducing hypernatremic, hyperchloremic metabolic acidosis with massive resuscitation volumes have not been borne out by further investigation with NS and the hypertonic saline solutions. Resuscitation with crystalloid solutions requires a volume administration ratio of 3 : 1 to 4 : 1 over volume lost [7].
Blood is the optimal agent to replace losses in victims of trauma with substantial hemorrhage. IV crystalloid resuscitation in HS boosts coagulopathy due to dilution of clotting factors and platelets, and hypothermia. Therefore, treatment with IV fluid should be avoided. In mandatory situations these fluids should be administered via small volumes, and should be halted when blood products can be infused. In the acute management of the victim in shock, blood products (i.e., red blood cells, plasma, and platelets) should be given in a ratio of 1:1:1. This approach will alleviate the untoward effects such as coagulopathy.
Small volume rsuscitation or “permissive hypotension”
Early or large-volume resuscitation in severe hemorrhage has not been supported by randomized controlled trials so far [9]. Increased hemorrhage volume and markedly higher mortality may ensue following ‘classical’ high-volume, normotensive resuscitation in case of major vascular injury [9,10]. In a study of uncontrolled hemorrhage, infusion of only enough fluid to maintain a MAP of 40 mm Hg improved survival rates and decreased hemorrhage [11] withholding of intravenous fluids in severe shock resuscitation still needs to be studied [12].
Brown et al. [13] cited that infusions of more than 500 mL of crystalloid in the prehospital setting led to worse outcomes in trauma victims without hypotension [13]. This finding indicated that resuscitation should be goal directed based on the blood pressure and hemodynamics. Infusion of crystalloids are to be replaced by blood as soon as possible in the hypotensive trauma cases. Crystalloid infusion (ie, ratio of crystalloid to PRBCs >1.5:1) was shown to result in worse outcomes in patients with ongoing hemorrhage [14,15]. Aggressive fluid infusion was blamed as potentially harmful in many reports [6,14,16,17] [7,9,21,22]. The algorithm known as permissive hypotension adopts a strategy of fluid infusion only to maintan the systolic BP at a minimum of 70 mmHg.
In the study by Bickell et al. [18], patients who did not receive the `usual` amounts of fluids reached to the ED with BP readings equivalent to those received the expected doses [18]. One of the major advantages of SVR is believed to be its allowance to homeostatic mechanisms to play their roles freely with resultant diminution of hemorrhage [19,20]. Accordingly, withholding FR has been shown to cause a significant decrease (62.5%) in ARDS and renal failure [18]. Aggressive volume replacement in the shocky patient is known to cause pulmonary edema, exacerbation of hemorrhage and increased intracranial pressure [21]. In a, RCT by Dutton et al. [20] patients with HS were assigned to either a protocol with target systolic BP>100 or 70 mmHg and gauged the FR as needed for these endpoints. The study failed to show any detrimental effect of a low systolic BP endpoint on mortality.
In another study, SVR with HHS (7.5% NaCl plus 6% of dextran-70) substantially improved systemic and splanchnic hemodynamic and oxygen transport, without an increase in pulmonary artery pressure [22]. In a clinical study of 230 patients after penetrating torso injuries, Wade et al. [23] demonstrated that HSD could result in favorable prognosis, especially if surgery is contemplated [23]. PH encompasses the strategy of maintenance of BP infranormal levels in order to sustain optimal or acceptable perfusion of vital organs without exacerbating bleeding due to injury. In well, designed animal studies of uncontrolled hemorrhage, it was shown that the survival rate of the animals left hypotensive and of the animals receiving fluid resuscitation was similar [24]. Most trauma surgeons advocate a policy of judicious fluid administration to maintain the MAP between 60 and 80 mmHg. Permissive hypotension is not proposed as a definitive therapy; in fact it can only be a temporizing measure before definitive control of blood loss is accomplished [25]. Initial fluid resuscitation for shock should comprise 500 cc boluses of NS via the largest and shortest gauge as possible peripheral IV route. Infusion of NS will cease with commencement of blood products or a normalized systolic blood pressure of 90 mmHg is noted with improvement of clinical status.
Conclusion
Hypovolemia resulting from hemorrhage is the leading etiology of shock in victims of multiple trauma. Although crystalloid solutions are chosen as the initial treatment to expand the volume and prevent cellular hypoxia, hemodynamically, unstable patients deserve treatment with blood products. Although aggressive FR is the mainstay therapy in trauma management, permissive hypotension should also be considered as a temporizing measure before definitive control of blood loss is accomplished. “A little goes a long way” in severely injured patients, that is, crystalloid administration is to be minimized while being cautious of significant hypotension. Limited volume resuscitation or PH is recommended to maintain minimally adequate organ perfusion to increase survival rates after trauma.
References
- Siegel JH (1995) The effect of associated injuries, blood loss, and oxygen debt on death and disability in blunt traumatic brain injury: the need for early physiologic predictors of severity. J Neurotrauma 12(4): 579-590.
- (1997) American College of Surgeons Advanced Trauma Life Support (Student Manual). American College of Surgeons.
- Wilson M, Davis DP, Coimbra R (2003) Diagnosis and Monitoring of Hemorrhagic Shock During the initial Resuscitatıon of Multiple Trauma Patients: a review. J Emerg Med 24(4): 413-422.
- American College of Surgeons. ATLS
- Davis JW, Shackford SR, Holbrook TL (1991) Base deficit as a sensitive indicator of compensated shock and tissue oxygen utilization. Surg Gynecol Obstet 173(6): 473-476.
- Roberts I, Evans P, Bunn F, Kwan I, Crowhurst E (2001) Is the normalisation of blood pressure in bleeding trauma patients harmful?. Lancet 357(9253): 385-387.
- Myburgh JA, Mythen MG (2013) Resuscitation Fluids. N Engl J Med 369: 1243-1251.
- Rizoli SB (2003) Crystalloids and Colloids in Trauma Resuscitation: A Brief Overview of the Current Debate, J Trauma 54: S82-S88.
- Dutton RP (2012) Haemostatic resuscitation. Br J Anaesth 109(S1): i39–i46.
- Salgado DR, Favory R, Backer DD (2010) Microcirculatory assessment in daily clinical practice - not yet ready but not too far! Einstein (São Paulo) 8(1): 107-116.
- Kowalenko T, Stern S, Dronen S (1992) Improved outcome with hypotensive resuscitation of uncontrolled hemorrhagic shock in a swine model. J Trauma 33(3): 349–353.
- D av i s J W Patient Care Phase: Shock. In: Greenfield, Lazar J, Mulholland, Michael W, Oldham, Keith T, Zelenock, et al. (2001) Surgery: Scientific Principles & Practice ( 3rd edn), Lippincott Williams & Wilkins pp. 288-294.
- Brown JB, Cohen MJ, Minei JP, Maier RV, West MA et al. (2013) Goaldirected resuscitation in the prehospital setting: a propensity-adjusted analysis. J Trauma Acute Care Surg 74(5): 1207-1212.
- Neal MD, Hoffman MK, Cuschieri J, Minei JP, Maier RV et al. (2012) Crystalloid to packed red blood cell transfusion ratio in the massively transfused patient: when a little goes a long way. J Trauma Acute Care Surg 72(4): 892-898.
- Duchesne JC, Heaney J, Guidry C, McSwain N Jr, Meade P et al. (2013) Diluting the benefits of hemostatic resuscitation: a multi-institutional analysis. J Trauma Acute Care Surg 75(1): 76-82.
- Ley EJ, Clond MA, Srour MK, Barnajian M, Mirocha J, et al. (2011) Emergency department crystalloid resuscitation of 1.5 L or more is associated with increased mortality in elderly and nonelderly trauma patients. J Trauma 70(2): 398-400.
- Veech RL (1995) Immediate versus delayed fluid resuscitation in patients with trauma. N Engl J Med 332(10): 681-682.
- Bickell WH, Wall MJ Jr, Pepe PE, Martin RR, Ginger VF, et al. (1994) Immediate versus delayed fluid resuscitation for hypotensive patients with penetrating torso injuries. N Engl J Med 331(17): 1105-1109.
- Stern SA, Dronen SC, Birrer P, Wang X (1993) Effect of blood pressure on hemorrhage volume and survival in a near-fatal hemorrhage model incorporating a vascular injury. Ann Emerg Med 22(2): 155-163.
- Dutton RP, Mackenzie CF, Scalea TM (2002) Hypotensive resuscitation during active hemorrhage: impact on in-hospital mortality. J Trauma 52(6): 1141-1146.
- Cabañas JG; Manning JE; Cairns CB (2011) Fluid and Blood Resuscitation. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7e, McGraw-Hill Companies, Inc.
- Chiara O, Pelosi P, Brazzi L, Bottino N, Taccone P et al. (2003) Resuscitation from hemorrhagic shock: Experimental model comparing normal saline, dextran, and hypertonic saline solutions. Crit Care Med 31(7): 1915-1922.
- Wade CE, Grady J J, Kramer GC (2003) Efficacy of Hypertonic Saline Dextran Fluid Resuscitation for Patients with Hypotension from Penetrating Trauma. J Trauma 54: S144-S148.
- Silbergleit R, Satz W, McNamara RM, Lee DC, Schoffstall JM (1996) Effect of permissive hypotension in continuous uncontrolled intraabdominal hemorrhage. Acad Emerg Med 3(10): 922-926.
- https://www.ncbi.nlm.nih.gov/pubmed/8891037






























