Making Healthcare Waste Management A Priority: Thereality of Solid Waste Disposal at Mulago National Referral Hospital – Directorate of Medicine (Kiruddu)
Christine Katusiime*
Department of Prevention Care and Treatment, Uganda
Submission: November 19, 2018; Published: December 12, 2018
*Corresponding author: Christine Katusiime, Department of Prevention Care and Treatment, Uganda.
How to cite this article: Christine Katusiime. Making Healthcare Waste Management A Priority: Thereality of Solid Waste Disposal at Mulago National Referral Hospital – Directorate of Medicine (Kiruddu). Int J Environ Sci Nat Res. 2018; 15(5): 555921. DOI: 10.19080/IJESNR.2018.15.555921.
Abstract
Healthcare Waste Management in developing countries has become an issue of great concern. A cross-sectional qualitative study was carried out at the national referral facility- directorate of medicine (teaching hospital) in Uganda with the primary aim of assessing current procedures and practices of handling medical waste. The results showed that lack of systematic guidelines and management commitment and priorities were important factors contributing to suboptimal HCWM. Emphasis by the hospital authorities should be focused on institutional and operational guidelines, capacity building and adoption of environmentally and economically sound HCWM approaches.
Keywords: Healthcare Waste Management; Developing Countries; Hazardous Waste
Introduction
Generally, medical waste worldwide represents a small percentage of total generated waste. Up to 25% percent of this medical waste is hazardous/infectious and therefore is of concern because of the environmental hazards and public health risks that this waste carries [1, 2]. Over the past decade, Kampala district, like other districts in Uganda has seen an upsurge in the number of public and private healthcare establishments. In less than a decade, there has been a 15% increment in the number of healthcare facilities in Uganda from 4,450 facilities in 2010 to 5,117 facilities in 2016 [3]. This coupled with increased population growth and the adoption of disposable medical products has inevitably led to significant increases in healthcare waste (HCW) [4, 5].
There’s evidence that suggests that the incidence rises of HIV, Hepatitis B and C in the recent past are attributable to personnel who handle and transport waste, on account of 40% of this waste being hazardous [6,7]. In developing countries, medical waste has received insufficient attention and there is generally no major interest geared towards healthcare waste management (HCWM). HCWM in Uganda is the responsibility of the national environment protection and conservation agency, the National Environmental Management Authority (NEMA), which is governed by the National Environment Act 1995, Cap 153 and the national environment (Audit) Regulations, 2006 [8,9]. In spite of the existing legislative framework, there are still major challenges in the field of HCWM in Uganda. Improving and formulating institutional HCWM frameworks on the contrary, requires evaluation of current practices. The main objective of this study is to assess the current procedures and practices of handling medical waste at the Mulago National Referral Hospital- Directorate of Medicine, Kiruddu.
Material and Method
Study Site
Mulago National Referral Hospital- Directorate of Medicine, Kiruddu, is an urban, public hospital located approximately 13 kilometers south-east of the main Mulago National Referral Hospital and has been operational for a little over 28 months. The construction of this hospital is part of government efforts to improve health service delivery because of the rapid expansion of Kampala, the central cities, population [10]. Mulago National Referral Hospital- Directorate of Medicine, Kiruddu, serves on average 250 patients daily.
Study Design
A qualitative observational study at the National Referral Hospital-Directorate of Medicine was from August 2018 to October 2018. Data was collected in accordance with the Individualized Rapid Assessment Tool (I-RAT), a specified tool developed by the United Nations Development Program Global Environment Facility project that can be utilized to indicate levels of HCWM at healthcare facilities. It can also be used to reduce disease burden attributed to poor HCWM. This is the first study in Uganda to evaluate waste management practices in a public health institution. The findings from this study will be fundamental in devising effective HCWM practices and standards. This study will also seek to make the case for prioritizing HCWM interventions.
The measures suggested in this study will be adopted as the benchmark for HCWM in health centers and hospitals countrywide.
Data collection
The data for this study was collected through the use of oral interviews and field visits from August 2018 to October 2018.
Results
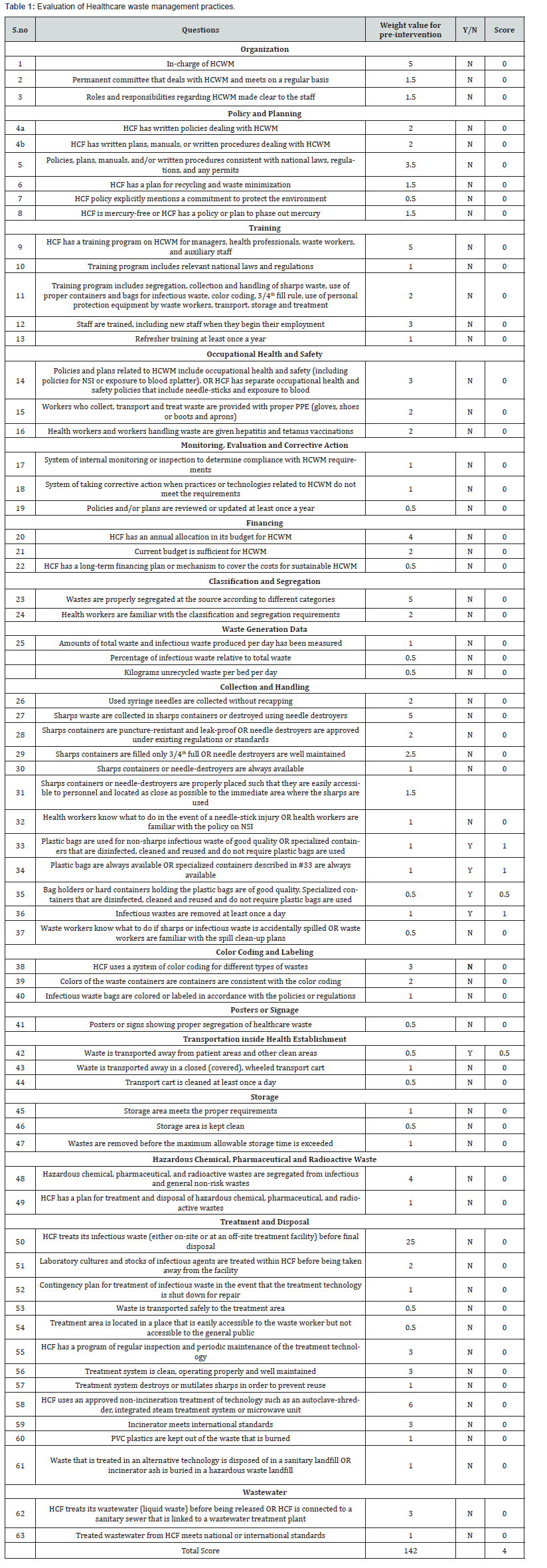
Regular visits were performed to monitor how HCWM was practiced. Data were collected regarding waste generation, collection, segregation, storage and transportation on-site. Assessment and scores were based on compliance with the Individualized Rapid Assessment Tool (IRAT) (Table 1).
Policies and guidelines
There is neither a HCWM department nor HCWM committee in place to monitor HCWM activities in the hospital. Although the hospital director is aware that there are government rules and regulations pertaining to waste management, the hospital has not developed institutional HCWM policies and standard operating procedures.
Training programs related to HCWM, standard operating procedures and legal provisions for waste management, segregation, collection, disposal, safety issues and safe injection practices for patients’ caregivers, physicians, nurses, waste handlers, were non-existent.
Medical Waste Generation
Medical waste inventories throughout the hospital are nonexistent hence quantitative data pertaining to the amount of medical waste generated was absent. Additional waste statistics indicating source, type and time were also lacking. Pictorial illustrations that would be critical in guiding patients, patients’ caregivers and visitors at waste generation points were nonexistent.
Segregation and Collection
Although waste was generally discarded in large waste bins and sharps in separate sharps containers, the concept of waste segregation was non-existent. Insufficient segregation at waste disposal points resulted in domestic waste being mixed with HCW. This will inevitably increase both waste disposal costs and health risks to health workers, waste disposal workers and the public. There was a visible absence of appropriate color coded and labeled waste bins and as a result, the hospital did not follow the recommended WHO basic three-bin system [11] for simple and safe waste segregation system at the points of waste generation. Posters aimed at reinforcing good waste management practices, indicating the type of waste for instance hazardous vs. non-hazardous waste to be disposed in waste receptacles, placed at appropriate waste generation points for instance on the walls adjacent to these waste receptacles were absent. Furthermore, absence of appropriate labeling, reinforcement and color coding makes identification of the type and source of medical waste difficult for both health workers and the public.
Waste Handling
Transportation of waste is done with wheelbarrows. The transport staff was observed to adorn only one form of personal protective equipment (PPE) - gloves. They did not wear the satisfactory PPE – in particular overalls, eye protection, masks, aprons and closed shoes as is recommended by WHO [11].
Because of inadequate color coding and segregation, hazardous and non-hazardous waste is transported as mixed waste.
Storage and Transportation
The hospital neither has a dug-out waste pit nor a medical waste incinerator. There is an on-site temporary waste storage area that was cordoned off under the directive of the hospital director. Although this temporary waste storage area is isolated from the general public, it is an open air storage area, making it completely exposed to the elements particularly rain and heat. Additionally, it is situated on an uphill slope.
In the likelihood of rain, the rainwater that falls on the waste, washes through the waste producing a toxic leachate, that flows downhill by gravity to the gate and then outside the hospital premises. In the likelihood of high temperatures during the hot season, offensive odors are generated from this waste area which could increase exposure risk to waste workers.
Disposal
Final disposal to an off-site area is done by outsourced disposal company trucks which come to the hospital once weekly and in all cases infectious waste is transported together with noninfectious waste.
The disposal workers typically do not wear sufficient protective gear for instance, overalls, eye protection and masks hence increasing the potential of health risks.
Safety
Mitigation against infectious diseases for physicians, nurses and handlers of medical waste was virtually non-existent. Serological screening for HIV sero-conversion and vaccination against infectious diseases in particular Hepatitis B and tetanus as well as post-exposure prophylaxis (PEP) against HIV in the event of needle-stick injuries were absent.
Discussion
This is the first study of its kind in Uganda, documenting that WHO and United Nations Development Program Global Environment Facility guidelines on HCWM are not being followed by Mulago National Referral Hospital, Directorate of Medicine, Kiruddu, a public sector healthcare hospital. With increasing urbanization, most developing countries are facing the growing challenges of solid waste management. In Uganda, the infrastructure for operationalizing, institutionalizing and sustaining best practices for HCWM are weak and deficient. HCWM is an essential element of how efficient a hospital and consequently a country’s health system is. The findings from this study reiterate the inefficiency of medical waste management at the Directorate of Medicine, Kiruddu. The study findings demonstrated that HCWM is not a priority in this hospital as evidenced by the lack of allocated budget funding towards waste management and the lack of economical waste management facilities for instance an incinerator.
HCWM protocols and regulations in developing countries have generally not been implemented in comparison to developed countries. This effectually shows how inefficient the health systems of developing countries are. Because HCWM is not considered as priority, hardly any funding is allocated and as a result, HCWM policies, protocols, regulations, guidelines and implementation plans in most developing countries are nonexistent and ineffective and are still an unmet goal in developing countries. The pre-intervention evaluation showed poor waste management practices at the directorate of medicine, Kiruddu, which is similar to studies in other countries that demonstrate that compliance with HCWM regulations and guidelines in many healthcare facilities remains a challenge. It is critical to note that one of the common barriers to effective HCWM in health facilities is lack of proper waste management practices among patients and patient caregivers as evidenced in this study by the observed lack of waste segregation at waste generation points [12]. As is seen by the findings in this study, solid waste is not sorted which in turn makes handling hazardous. Secondly, the danger to the health workers, local community and environment highlighted in this paper, is the toxic leachate from the open temporary waste storage area which not only poses serious environmental risks but is also a source of disease.
Because mis-segregated HCW, subsequently, leads to elevation of HCWM costs, implementation of HCW segregation and minimization are therefore crucial to decreasing costs attributed to HCWM. During observations, it was obvious that transportation of hazardous and non-hazardous waste was also not segregated. Inability to separate medical waste from ordinary garbage potentially puts health workers, disposal workers and scavengers at serious risk of contracting HIV/AIDS, tetanus, Hepatitis B and C. There’s compelling evidence that confirms that the prevalence of Hepatitis B and C infections are much higher in healthcare workers and waste-exposed populations in comparison to the general population, thus making them high risk groups [13-16]. Infectious waste increases transmissibility of major bacterial infections particularly salmonella typhi, pseudomonas aeruginosa, Escherichia coli and staphylococcus aureus [17- 20]. These pathogens can lead to the contamination of groundwater and air particularly, E coli.
It therefore is essential for health institutions to promote vigorous HCWM practices. To counteract the unnecessary health risks of HCWM it ought to be mandatory for health institutions to adopt full PPE for waste disposal workers and health workers as well as availability of annual blood testing, appropriate PEP and mandatory vaccination programs for all waste disposal workers and health workers against hepatitis A and B and tetanus. It is critical that every hospital and health center have internal waste disposal inventories. A central online manifest system that monitors medical waste transportation is essential to ensure firstly, that infectious medical waste is tracked and secondly that protocols and regulations regarding safe disposal of infectious medical waste are adhered to. Effective capacity building and training programs incorporating public and private health institutions, waste collection and disposal companies, municipal governments, partners and stakeholders are vital to scaling up implementation of HCWM policies. There’s need for effective visual training aids, health talks, announcements and counseling sessions that equip patient caregivers with proper waste management techniques.
This study has limitations. Most studies on HCWM have a quantitative aspect to it. There was no quantitative data because of non-existent health care waste management policies. The other limitation is that this study was restricted to one hospital hence the findings may not be generalizable. Adequate budgetary allocations, adoption of robust HCWM plans and HCWM training at health centers and hospitals should also be prioritized as key to the health policy agenda.
Conclusion and Recommendations
The general observation is that HCWM at Mulago National Referral Hospital, Directorate of Medicine, Kiruddu, is poorly coordinated, under-financed and under-prioritized achieving a score of 2.8% (Table 1). Due to poor leadership and weak HCWM implementation practices, the institutional framework for HCWM that encompasses policies, surveillance and interventions is virtually non-existent. Compliance of the Directorate of Medicine, Kiruddu with WHO recommendations of immunization and use of PPE for waste handlers and all healthcare workers is important in reducing risks of exposure to infectious diseases. The ramifications of poor HCWM as seen in this study are far-reaching affecting health workers, waste handlers, waste disposal workers, scavengers, the local community and the environment.
It is crucial from the institutional point of view, for health institutions, to establish occupational medical departments that are dedicated to effectively managing medical waste generated from these institutions. It is critical to note that training and capacity building are the cornerstones to effective HCWM. Adoption of environmentally and economically sound HCWM approaches for instance installation of an incinerator and autoclaves will go a long way in counteracting the effect of hazardous waste and toxic leachate at the Directorate of Medicine, Kiruddu. The author provides the following recommendations as a way forward towards effective and sustainable HCWM:
a) Formulation of an appropriate institutional HCWM plan and HCW SOPs.
b) Creation of an occupational health and safety department that will monitor HCWM activities and provide appropriate vaccination for tetanus, Hepatitis B and PEP for HIV.
c) Budgetary allocation for HCWM.
d) Prioritizing HCWM activities and research.
e) Regular staff training and capacity building.
f) Information, Education and Communication (IEC) of HCWM practices to hospital staff, waste handlers, waste disposal workers, patients and patients’ caretakers.
g) Prioritizing HCWM strategies for instance use of multichamber incinerators and adoption of alternative modern technologies to treat HCW for instance autoclaves and shredders.
Acknowledgement
I accord double honor to the chief custodian of this project, Prophet Elvis Mbonye to whom I am entirely indebted. I would like to thank the Director of Mulago National Referral Hospital, Directorate of Medicine, Kiruddu for his invaluable cooperation in this study.
References
- World Health Organization (2017) Safe management of wastes from health care activities: a summary. Geneva.
- Rushbrook P, Zghondi R (2005) Better health care waste management: an integral component of health investment. World Health Organization.
- (2017) Uganda Bureau of Statistics. Statistical Abstract.
- Arab M, Baghbani RA, Tajvar M, Pourreza A, Omrani G, et al. (2008) Report The assessment of hospital waste management: a case study in Tehran. Waste Manag Res 26(3): 304-308.
- Taghipour H, Mosaferi M (2009) The challenge of medical waste management a case study in northwest Iran Tabriz. Waste Manag Res 27(4): 328-335.
- Almuneef M, Memish ZA (2003) Effective medical waste management: it can be done. Am J Infect Control 31(3): 188-92.
- AIDSTAR-One FACT SHEET. Health Care Waste Management in Uganda.
- (1995) Uganda Legal Information Institute. National Environment Act 1995.
- (2006) Uganda Legal Information Institute. National Environment (Audit) Regulations.
- Namuli Z (2013) Government to construct more referral hospitals. National Broadcasting Service (NBS).
- (2017) World Health Organization. Safe management of wastes from health care activities: a summary.
- Oroei M, Momeni M, Palenik CJ, Danaei M, Askarian M (2014) A qualitative study of the causes of improper segregation of infectious waste at Nemazee Hospital Shiraz Iran. J Infect Public Health 7(3): 192- 198.
- Ream PS, Tipple AF, Barros DX, Souza AC, Pereira MS (2016) Biological risk among hospital housekeepers. Arch Environ Occup Health 71(2): 59-65./a>
- Rachiotis G, Papagiannis D, Markas D, Thanasias E, Dounias G, et al. (2012) Hepatitis B virus infection and waste collection: prevalence, risk factors, and infection pathway. Am J Ind Med 55(7):6 50-655.
- Sharma A, Sharma V, Sharma S, Singh P (2013) Awareness of biomedical waste management among health care personnel in Jaipur, India. Oral Health Dent Manag 12(1): 32-40.
- Qaiser S (2012) Survey of sharp waste disposal system in clinics of New Karachi. J Pak Med Assoc 62(2): 163-164.
- Soares SR, Finotti AR, Da Silva VP, Alvarenga RA (2013) Applications of life cycle assessment and cost analysis in health care waste management. Waste Manag 33(1): 175-183.
- Abah SO, Ohimain El (2011) Healthcare waste management in Nigeria: a case study. J Public Health Epidemiol 3(3): 99-110.
- Shiferaw Y, Abebe T, Mihret A (2011) Hepatitis B virus infection among medical waste handlers in Addis Ababa, Ethiopia. BMC Res Notes 4: 479.
- Yenesew MA, Moges HG, Woldeyohannes SM (2012) A cross sectional study on factors associated with risk perception of healthcare workers toward healthcare waste management in health care facilities of Gondar town, northwest Ethiopia. Int J Infect Control 8(3): 1-9.






























