Pre-Diabetes Predicts Longitudinal Change of Post Stroke Depressive Symptoms Following Acute Ischemic Stroke within One Year
Shuolin Wu1, Huicong Shen2, Zhengran Li2, Kang Du2 and Chunxue Wang1 and Bin Zhu3*
1Department of Neuropsychiatry and Behavioral Neurology and Clinical Psychology/Sleep Medicine Center, Beijing Tian Tan Hospital, Capital Medical University, China
2Department of Radiology, Beijing Tian Tan Hospital, Capital Medical University, China
3Department of Pharmacy, Beijing Tian Tan Hospital, Capital Medical University, China
Submission: October 26, 2020; Published: July 22, 2022
*Corresponding author:Bin Zhu, Department of Pharmacy, Beijing Tian Tan Hospital, Capital Medical University, Beijing, China
How to cite this article: Shuolin W, Huicong S, Zhengran L, Kang D, Chunxue W, et al. Pre-Diabetes Predicts Longitudinal Change of Post Stroke Depressive Symptoms Following Acute Ischemic Stroke within One Year. Glob J Intellect Dev Disabil, 2022; 10(3): 555787. DOI:10.19080/GJIDD.2022.10.555787
Abstract
The relationship of abnormal glycometaboism (AG) including diabetes mellitus (DM) and prediabetes, and post-stroke depression (PSD) and post-stroke depressive symptoms longitudinal change (PSDSLC) is not clear. we analyzed their relationship till one year after first-onset acute ischemic stroke (AIS). Two hundred and twenty-two AIS patients were consecutively recruited in Beijing Tiantan Hospital and were followed up for 1 year. The glycometabolism was diagnosed according to HbA1c criteria. Diagnosis of depression was performed by well-trained physicians according to the Diagnostic and Statistical Manual of Mental Disorders, fifth edition (DSM-Ⅴ). PSDSLC was defined as a ‘PHQ9 change’ ≤0, which indicated the depressive symptoms of the participate took a ‘definitely not better’ change. ‘PHQ9 change’ was calculated by ‘PHQ9 score on 14 days’ minus ‘PHQ9 score on the 3rd month or 1 year’. Multivariate logistic regression was used to analyze the associations between DM as well as prediabtes and PSD or PSDS. The prevalence of PSD was 21.2%, 15.6% and 12.8% on 14 day, 3.0%, 3.0% and 2.0% on 3 month and 9.7%, 8.7% and 7.7% on 1 year in DM, prediabetes and normoglycemia, respectively (P=0.035 for 14 day, 0.045 for 3 month and 0.033 for 1 year). AG independently predicted a longitudinal change of PSDS compared to normoglycaemia. OR with 95%CI were 4.09 (1.78-8.87) for DM (P=0.012) and 3.10 (1.25-7.36) for prediabetes (P=0.007) on 3 month, 3.25(1.21-7.58) for DM (P=0.025) and 2.68(1.17-6.76) for prediabetes (P=0.018) on 1 year. Prediabetes not only DM after acute ischemic stroke onset predict the worsening of PSDSLC within one year after AIS.
Keywords: Abnormal glycometabolism; Diabetes mellitus; Ischemic stroke; Post-stroke depression; Prediabetes
Abbreviations: AG: Abnormal Glycometaboism; DM: Diabetes Mellitus; PSD: Post-Stroke Depression; PSDSLC: Post-Stroke Depressive Symptoms Longitudinal Change; AIS: Ischemic Stroke; BMI: Body Mass Index; WHR: Waist to Hip Ratio; OCSP: Oxfordshire Community Stroke Project; FPG: Fasting Plasma Glucose
Introduction
The prevalence of PSD usually approximately one third is widely accepted [1,2]. It causes severe mortality, disability and other poor prognosis and huge social burden after acute cardiovascular disease onset [3]. Diabetes mellitus was widely accepted as a risk factor for stroke and its prognosis including death and poor functional outcome and recurrence [4]. DM was also found as a risk factor for major depression [5]. The most recent report demonstrated that almost 25% adults with DM experienced depression [6].
Based on the adverse effect of PSD as stated above, it is necessary to clarify the association between AG and PSD as well as the PSDSLC in AIS. HbA1c was recommended as a method for clinician to detect DM (≥6.5%) and prediabetes (5.7%-6.4%) [7]. Thus, HbA1c was used to diagnose AG in our study. Although it has been estimated prediabetes is related to PSD in one month after stroke [8], it is still unknown how long such an effect would exist for. The relationship will be analyzed till one year after AIS. It was postulated that prediabetes not only DM does harm to PSD and PSDSLC within one year after AIS.
Methods
Study participants and settings
All the participants were enrolled consecutively within 14 days after initial AIS in Beijing Tiantan Hospital. The inclusion criteria were as follows: Age ≥ 18 years; fulfilling the definition of stroke according to WHO criteria and confirmed by CT/MRI. Exclusion criteria were previous history of depression, dementia or other known neurological diseases that could affect cognitive functions; history of alcohol or drug abuse; and inability to communicate appropriately, including aphasia.
Demographic and clinical data
Patients’ demographic and clinical data were obtained within 24 hours after admission. Clinical data composed of tobacco use (current or quit smoking, defined as one who smoked at the time of stroke or had quit smoking within 1 year), alcohol intake (moderate or severe drinking, ≥2 standard alcoholic beverages consumed per day), medical histories, body mass index (BMI), waist to hip ratio (WHR), systolic and diastolic blood pressure, blood biochemical data, and stroke subtype according to the criteria described in the Oxfordshire Community Stroke Project (OCSP) [9] and the Trial of ORG 10172 in Acute Stroke Treatment (TOAST) [10]. Classification of stroke subtypes depends on clinical history, reliable clinical information, and radiological (computer tomography/magnetic resonance imaging scan) findings. Blood biochemical data consisted of HbA1c, fasting plasma glucose (FPG), fasting insulin, high density lipoprotein, low density lipoprotein, creatinine, uric acid, and homocysteine. Medications during hospitalization and 3-month and 1-year follow-up were recorded. HbA1c value was measured at admission using ‘high performance liquid chromatographic analysis (HPLC)’ by a Bio- Rad VariantⅡanalyzer (Bio-Rad Laboratories, Hercules, CA) with a reference value of 4.1-6.5%, which is standard in the Diabetes Control and Complications Trial (DCCT) and National Glycohemoglobin Standardization Program (NGSP) [11]. The intra-assay coefficient of variation (CV) was 2.5% and the interassay CV was <4.0%; both of them were within the limits of the NGSP [12].
Definition for AG according to HbA1c
HbA1c criteria for glycometabolism diagnosis were as follows: HbA1c ≥6.5% for DM, HbA1c5.7-6.4% for prediabetes, and HbA1c <5.7% for normoglycaemia [7].
Definition for PSD and PSDSLC
Patient health questionnaire (PHQ9) was used as the tool to detect depression after stroke [13]. Diagnosis of depression was performed by well-trained physicians according to the Diagnostic and Statistical Manual of Mental Disorders, fifth edition (DSM-V) [14] and with a score of PHQ9 over 4 [13]. PSDSLC was defined as a ‘PHQ9 change’ ≤0, which indicated the depressive symptoms of the participate took a ‘definitely not better’ change. ‘PHQ9 change’was calculated by ‘PHQ9 score on 14 days’ minus ‘PHQ9 score on 3 month or 1 year’.
Follow-up
Telephone interviews were taken at 3 month and 1 year. All interviewers were trained together according to the followup protocol. Data on medications including anti-thrombotic agents, anti-hypertension agents, lipid-lowering agents and antidepressive medications were recorded during hospitalization and at 3-month and 1-year intervals. If an individual received the medication during hospitalization, we recorded ‘yes’. Persistence was calculated as the cumulative duration of taking drugs (antithrombotic, antihypertensive or lipid-lowering therapy) divided by the length of the follow-up period. If the patient had PSD, persistence would be calculated as the cumulative duration of taking drugs divided by the length of the follow-up period before PSD occurrence. Medication persistence of ≥ 75% was defined as high and < 75% was defined as low.
Statistical analysis
Patient baseline characteristics were compared between the three glycometabolism statuses. Continuous variables were expressed as means ± standard deviations; One-way ANOVA test was used for comparison between groups. Categorical variables were expressed as frequencies and ratios; χ2 test or Fisher’s exact test was used for comparison between groups. All these above variables were included in the univariate analysis. The candidate variables that were entered into the multivariate analysis were those with biologically plausible link to PSD on the basis of prior publication and those associated with PSD in univariate analysis (P <0.10). In the multivariate analysis for PSD occurrence, age, BMI, WHR, gender, education status, housewife, tobacco use, alcohol intake, Stroke severity (NIHSS ≥9), mRS >2, TOAST and OCSP subtypes, medications and previous medical history of hypertension, coronary heart disease, stroke and DM were entered as confounding factors. In the multivariate analysis for PSDSLC, the same variables as above were entered. Statistical analyses were performed with the SPSS 17.0 software (SPSS Inc., Chicago, IL). A P <0.05 was considered statistically significant.
Results
Clinical characteristics at 14-day, 3 month and 1 year
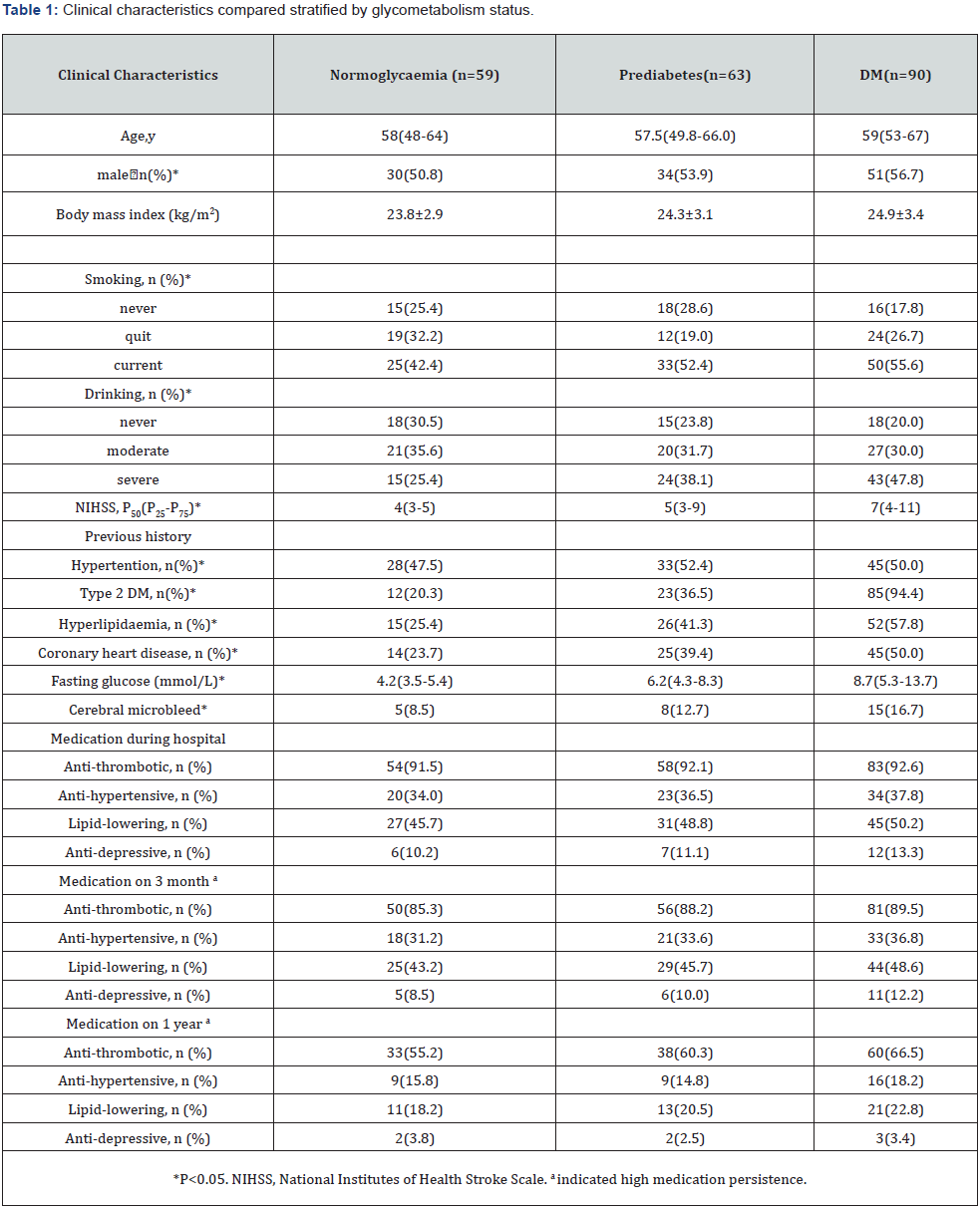
The mean age was 58.5 including 115 males and 97 females. The number of patients lost to follow-up on 3 months was 14(6.6%) and the cumulative number of that on one year were 17(8.0%). The fasting glucose level in DM is highest than other two kinds of glycometabolism. Most of DM were male and tended to have cerebral microbleed, current smoking and moderate to severe drinking. The rate of never smoking is lowest in DM than the other two. Also, the rate of previous DM, hyperlipidemia and coronary heart disease is highest. The rate of hypertension is lower than that in prediabetes but much higher than that in normoglycaemia. Medicine persistence were all getting worse after discharge (P=0.018). There was no significant difference on the use of antidepressive medicine between in hospitalization and in 3 months after discharge, even stratified by glycometabolism status (all P values were >0.05) (Table 1).
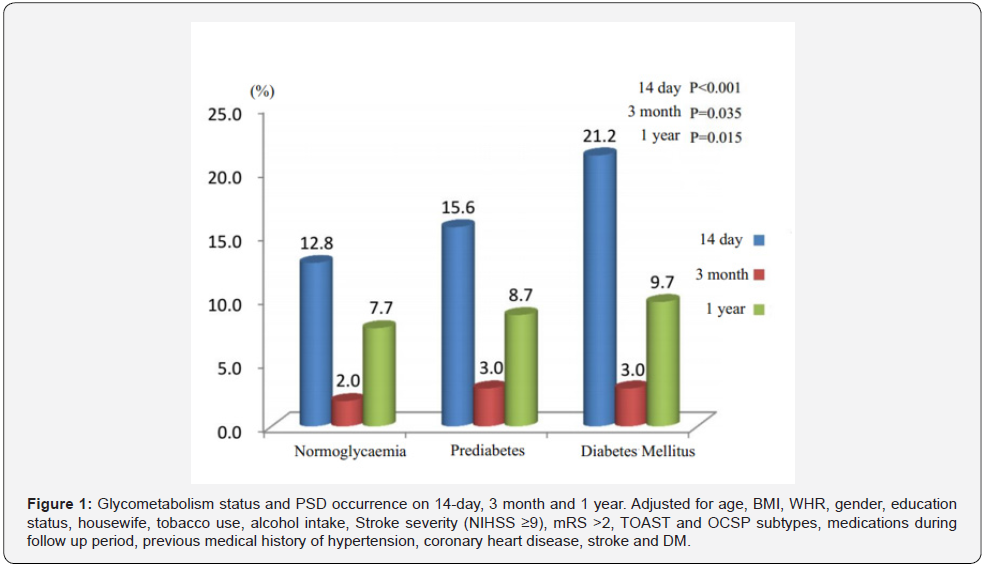
PSD occurrence and PSDS longitudinal change within 1 year following stroke stratified by glycometabolism status
The PSD patients were 105 (49.5%), 16 (8.1%) and 51 (26.2%) on 14 days, 3 month and 1year respectively. The prevalence of PSDs for 14 days was 21.2%, 15.6% and 12.8% in diabetes mellitus, prediabetes and normoglycaemia, respectively (P=0.035). The prevalences were 3.0%, 3.0% and 2.0% on 3 month and 9.7%, 8.7% and 7.7% on 1 year in the above sequence of glycometabolism status, respectively (P=0.045 for 3 month and 0.033 for 1 year) (Figure 1).
The rate of longitudinal change of PSDS “definetely not better” were 81.9% (n=72), 77.1% (n=47) and 55.1% (n=27) for 3 month and 90.7% (n=81), 85.0% (n=50) and 59.2% (n=29) for 1 year in DM, prediabetes and normoglycemia, respectively. Both of the PHQ9 score change in 3 months and 1 year significantly differed in DM, prediabetes and normoglycaemia (P=0.003 for 3 month and < 0.001 for 1-year univariate analysis) (Table 2).

Multivariate analyses for PSD and PSDS longitudinal change
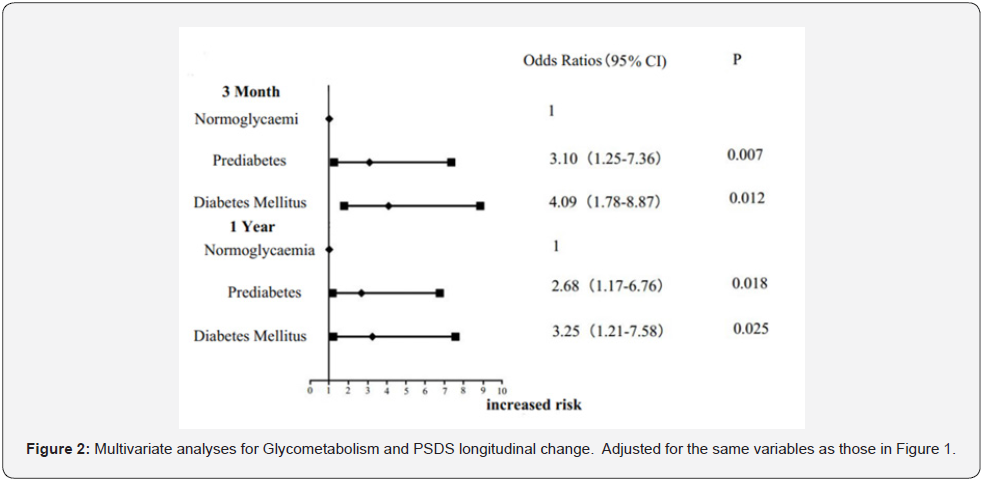
In multivariate analysis for PSDS longitudinal change, not only DM but also prediabetes independently predicted such a longitudinal change of PSDs compared with normoglycaemia. OR with 95%CI were 4.09 (1.78-8.87) for DM (P=0.012) and 3.10 (1.25-7.36) for prediabetes (P=0.007) on 3 month, 3.25(1.21- 7.58) for DM (P=0.025) and 2.68(1.17-6.76) for prediabetes (P=0.018) on 1 year (Figure 2).
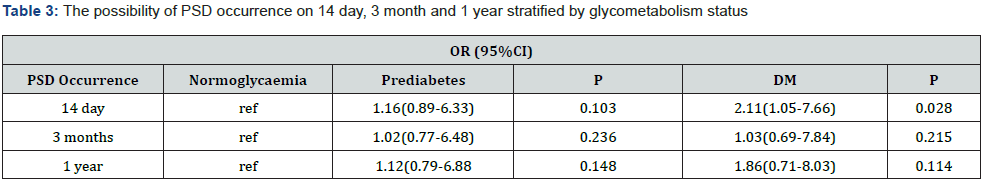
In multivariate analysis for PSD, DM independently predicts 14day-PSDs but prediabetes not (OR with 95%CI DM 2.11 (1.05- 7.66), P= 0.028, prediabetes 1.16(0.89-6.33), P =0.103). Neither DM nor prediabetes was statistically associated with 3-month and 1-year PSD occurrence (Table 3).
Conclusion
Prediabetes not only DM after acute ischemic stroke onset predict the worsening of PSDSLC within one year following AIS.
These findings might draw clinicians’ attention to blood glucose management before a true PSD formed in prediabetes when handle with AIS.
Ethics Approval and Consent to Participate
The study was approved by the Ethics Committees at all participating hospitals. Disclosure statement.
Funding
The study was supported by the Clinical Toxicology Project of Chinese Society of Toxicology(Number: CST2020CT109).
Acknowledgements
We thank all the participants in the study.
References
- Hackett ML, Pickles K (2014) Part I: frequency of depression after stroke: an updated systematic review and meta-analysis of observational studies. Int J Stroke 9(8): 1017-1025.
- Robinson RG, Jorge RE (2016) Post-Stroke Depression: A Review. Am J Psychiatry 173(3): 221-231.
- Lichtman JH, Froelicher ES, Blumenthal JA, Carney RM, Doering LV, et al. (2014) Depression as a risk factor for poor prognosis among patients with acute coronary syndrome: systematic review and recommendations: a scientific statement from the American Heart Association. Circulation 129(12): 1350-1369.
- Wu S, Wang C, Jia Q, Liu G, Hoff K, et al. (2014) HbA1c is associated with increased all-cause mortality in the first year after acute ischemic stroke. Neurol Res 36(5): 444-452.
- Renn BN, Feliciano L, Segal DL (2011) The bidirectional relationship of depression and diabetes: a systematic review. Clin Psychol Rev 31(8): 1239-1246.
- Khaledi M, Haghighatdoost F, Feizi A, Aminorroaya A (2019) The prevalence of comorbid depression in patients with type 2 diabetes: an updated systematic review and meta-analysis on huge number of observational studies. Acta Diabetologica 56(6): 631-650.
- American Diabetes Association (2012) Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 35(Suppl 1): S64-S71.
- Xiao M, Wang Q, Ren W, Zhang Z, Wu X, et al. (2018) Impact of prediabetes on poststroke depression in Chinese patients with acute ischemic stroke. Int J Geriatr Psychiatry 33(7): 956-963.
- Bamford J, Sandercock P, Dennis M, Burn J, Warlow C (1991) Classification and natural history of clinically identifiable subtypes of cerebral infarction. Lancet 337(8756): 1521-1526.
- Adams HP, Bendixen BH, Kappelle LJ, Biller J, Love BB, et al. (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24(1): 35-41.
- National Glycohemoglobin Standardization Program (NGSP). List of NGSP certified methods.
- Schwartz KL, Monsur JC, Bartoces MG, West PA, Neale AV (2005) Correlation of same-visit HbA1c test with laboratory-based measurements: a MetroNet study. BMC Fam Pract 6: 28.
- Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16(9): 606-613.
- American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders. (5th edn), Arlington, VA: American Psychiatric Publishing.
- Lewin-Richter A, Volz M, Jöbges M, Werheid K (2015) Predictivity of Early Depressive Symptoms for Post-Stroke Depression. J Nutr Health Aging 19(7): 754-758.






























