Singing Enhanced Swallowing Protocol for a Patient with Intellectual Disability: A Case Report
Myung Sun Yeo*
Senior Researcher & Clinical Supervisor, Ewha Music Rehabilitation Center/ Republic of Korea
Submission: August 25, 2021; Published: August 30, 2021
*Corresponding author: Myung Sun Yeo, Senior Researcher & Clinical Supervisor, Ewha Music Rehabilitation Center 52 Ewhayeodae-gil, Seodaemun-gu, Seoul 03760, Republic of Korea
How to cite this article: Myung Sun Yeo. Singing Enhanced Swallowing Protocol for a Patient with Intellectual Disability: A Case Report. Glob J Intellect Dev Disabil, 2021; 9(1): 555751. DOI:10.19080/GJIDD.2021.09.555751
Abstract
This study aimed to describe the case of intervention for a neurologic patient with a developmental disorder. The 50-year-old woman patient had ID and was diagnosed with Parkinsonism six years ago. She participated in individual 20-minute singing enhanced swallowing protocol sessions two times per week for four weeks. Her voice data were measured to evaluate laryngeal movement changes related to vocal, speech, and swallowing function before and after sessions. After eight sessions, there was a partial improvement in her vocal function. Also, her speech and swallowing function has improved either. The case and the results showed that the additional difficulties of adults with ID following an acquired brain injury are easy to be overlooked. Therefore, they should be considered through a differentiated therapeutic strategy in the medical setting.
Keywords: Intellectual disability; Swallowing disorders; Music; Cognitive; Parkinsonism; Vocal function; Neurologic impairment
Introduction
As complications are prevalent, swallowing disorders represent key predictors of increased morbidity and mortality in adults with intellectual disability (ID) [1]. They might result from disorders developed during infancy that persist into adulthood [2,3]. Adult-onset medical disorders and physiological changes resulting from the aging process may significantly impact swallowing skills or exacerbate pre-existing difficulties.
A neurologic patient with ID has a more significant challenge due to increased loss of function following brain damage. Little information is pertinent regarding supporting and rehabilitating patients with ID issues as societies increasingly move toward community integration [4]. Recent research indicates that adults with IDs are more likely to incur an injury requiring medical attention [5,6]. While swallowing with ID has focused on intervention or outcomes following pre-existing symptoms, neurologic impairment has been excluded. Therefore, we know that acquired brain injury can cause a decline in cognitive functioning [7].
Neurorehabilitation refers to the restoration of developed initial functions. The treatment goal is to return to the pre-onset functional level. In this regard, the therapeutic approach to the target group of developmental disorders with nerve damage needs to proceed differently from the general approach.
Accordingly, this study attempted to describe the outcomes and considerations regarding intervention for a neurologic patient with ID. The results of this study present baseline data and clinical implications for applying more diversified singing-based swallowing interventions for the target group of developmental disorders with nerve damage. Given that many of these problems are already a feature of ID, it is probable that a brain injury event will exacerbate any existing symptoms. Moreover, any issues with neurologic impairment are likely to be dismissed as pre-existing for a patient with developmental disorders.
Case Report
The patient in this study is a 50-year-old woman with ID diagnosed with dysphagia due to Parkinsonism about six years ago. In the interview before the intervention, the caregiver reported that the patient had previously been diagnosed with ID in her childhood. All procedures in this study were reviewed and approved by the Institution Review Board of the Hospital (IRB No. 4-2012-0483). Before the participation, she completed the informed consent form. The patient participated in individual 20-minute singing enhanced swallowing protocol sessions two times per week for 4 weeks. Pretest measures were administered during the week before the patient’s first intervention session, and posttest measures were taken within one week after completion of the protocol.
Patients’ voice data were recorded to assess laryngeal movement, including speech and swallowing function. The recorded voice data were analyzed using the Praat program. As a voice measured, maximum phonation time (MPT) was recorded. The patient was asked to make the /ah/ sound and maintain it as long as possible. Three trials of phonation were administered, and the most extended sound was included for analysis. Then, to evaluate the range and speed of vocal fold movement, the patient was asked to cut off the vowel /ah/ as quickly as possible. The rate of laryngeal diadochokinesis (L-DDK) was measured [8-11]. L-DDK data is used as an index of laryngeal function in research, which is measured by asking the patient to repeat the glottal syllable /ah/ sound.
Furthermore, alternating/sequential motion rates (AMR/ SMR) were measured to evaluate patients’ oral motor articulatory function. For the AMR measure, participants were asked to repeat /puh/, /tuh/, and /kuh/ as fast and accurately as possible for five seconds. For SMR, the participants were asked to repeat /puh-tuhkuh/ in a sequence for over five seconds. The number of repeated target sounds during five seconds was calculated.
The singing enhanced swallowing protocol consisted of four parts: respiratory muscle relaxation, vocal folds relaxation, laryngeal elevation, and modified singing focused on oral motor movement and respiration. The protocol was a modified version of the music-based swallowing enhancement protocol [12]. The protocol process is described in Table 1.
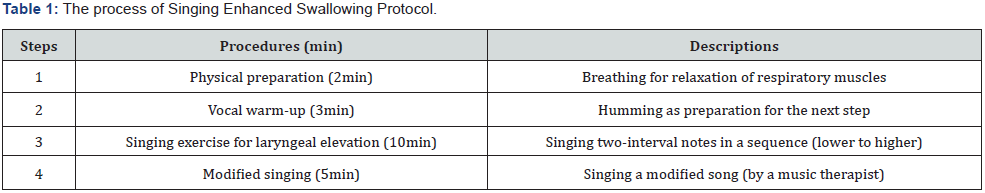
The first step was upper body movements such as turning the neck right and left, lifting and lowering the shoulders, and stretching by extending the arms upward for respiratory muscle relaxation. The second step involved humming a sound for vocal fold relaxation. Since humming can relax a tensed larynx and cause the vocal folds to be gradually introverted within a narrow range, it is appropriate as a preparatory process for vocalization [13]. The third step of this protocol was the primary component of the laryngeal elevation protocol. This activity initially induced laryngeal elevation by executing sequential vocalization of two vowels, /ooh/ and /i:/, following two different pitches. In this session, the patient was instructed to vocalize the back vowel / oh/ at a low pitch instead of /ooh/, the front vowel /i:/ at a high pitch, and both sounds with different musical pitches. The therapist asked the patient to connect two sounds to form a single word, /oh-i:/(which means “cucumber” in Korean) because it was expected that tasks using meaningful words would be easier for patients to understand. Finally, modified singing included two interval notes in a sequence on regular beats in a song. While the patient’s preferred pieces were used, the original song’s lyrics,melody, or rhythm were modified. The rationale of the protocol was described in previous studies [12-14]. In all steps, considering the patient’s cognitive function, the therapist demonstrated the movement or vocalization to the patient and imitated it with a live keyboard playing as an accompaniment. The tempo and dynamics of the music were adjusted to match the movement executed by the patient and provide cueing for each target activity. She was more likely to imitate the therapist’s singing demonstrations than their verbal instructions. Her favorite song is the Korean folk song ‘Doraji’ (‘ballon flower’), enjoyed by people much older than her. Since the melody of ‘Doraji’ repeats the same musical notes, the therapist modified the melody by varying the range of the musical notes. Also, it made the rhythm structure simple and consistent to prevent the patient from recognizing it as a new song.
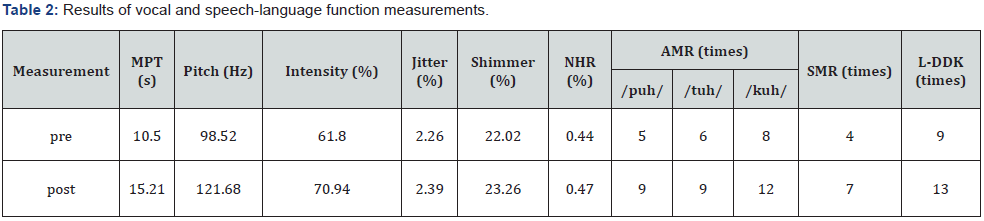
After the sessions, the patient’s voice data increased in MPT, pitch, and intensity. In contrast, other voice quality data, such as jitter, shimmer, and NHR, hardly changed. AMR and SMR, which indicate the oral motor movement rate, increased. L-DDK also increased after the intervention (Table 2).
Discussion
This study aimed to draw attention to neurologic music therapy strategies in a patient with ID. It can be discussed by two points through the case presented in the study.
First, since singing is a noninvasive therapeutic tool in medical settings, it can be used for various purposes and populations. To be used therapeutically, it has a more detailed specification of which singing activities best support specific problems, and diagnoses are needed. Also, singing’s objective and the contents of the intervention’s activities were selected based on a patient’s specific problems. From this viewpoint, for the patient with developmental disabilities with neurologic impairment, the approach must be differentiated from the initial neurorehabilitation; this is because it must be considered that the knowledge level acquired or stored in the developmental process before the illness’s onset or the brain processing pathway is different from that of a typical brain injury patient. In this study, the therapist modified the verbal direction or task in the protocol to make it easier for the patient to understand. Also, the therapist modified the patient’s preferred song and used it for the therapeutic goal. The therapist’s clinical and musical expertise is essential to modify and use music according to the patient’s function.
Second, this case is particularly relevant as the intellectual disability was mild, whereas the subsequent Parkinsonism was undisputedly severe. If the caregiver hadn’t said it, the therapist wouldn’t have known about it until the end. There is no doubt that a person with ID will experience problems with cognition and social interactions. However, these problems should not cause the additional difficulties that adults with ID face following an acquired brain injury to be overlooked as they were in the case presented in this study. There were several limitations to the research methods used for this study. For example, the information related to ID presented here relied substantially on the accuracy of retrospective recall from the caregiver. Despite these limitations, a longitudinal perspective provides an opportunity to evaluate the case across the entirety of the patient’s formative years. It is hoped that future research will propose more efficient compositions for music interventions and more specific application methods for treating patients with swallowing disorders due to diverse causes, including a pre-existing intellectual disability in a neurorehabilitation setting.
References
- Manduchi B, Fainman GM, Walshe M (2020) Interventions for feeding and swallowing disorders in adults with intellectual disability: A systematic review of the evidence. Dysphagia 35(2): 207-219.
- Riquelme LF, Benjamin RD, Tahhan HJ, Sandoval GK, Alomari N, et al. (2016) Feeding/swallowing disorders: Maintaining quality of life in persons with intellectual disability. Journal of Intellectual Disability-Diagnosis and Treatment 4(2): 81-93.
- Robertson J, Chadwick D, Baines S, Emerson E, Hatton C (2017) Prevalence of dysphagia in people with intellectual disability: a systematic review. Intellectual and developmental disabilities 55(6): 377-391.
- McKinlay A, McLellan T, Daffue C (2012) The invisible brain injury: The importance of identifying deficits following brain injury in children with intellectual disability. NeuroRehabilitation 30(3): 183-187.
- Patel DR, Apple R, Kanungo S, Akkal A (2018) Intellectual disability: Definitions, evaluation and principles of treatment. Pediatr Med 1(11).
- Sappok T, Diefenbacher A, Winterholler M (2019) The medical care of people with intellectual disability. Deutsches Ärzteblatt International 116(48): 809-816.
- Kleynen M, Beurskens A, Olijve H, Kamphuis J, Braun S (2018) Application of motor learning in neurorehabilitation: a framework for health-care professionals. Physiotherapy theory and practice 36(1): 1-20.
- Han TR, Paik NJ, Park JW, Kwon BS (2008) The prediction of persistent dysphagia beyond six months after stroke. Dysphagia 23: 59-64.
- Lombard L, Solomon NP (2020) Laryngeal diadochokinesis across the adult lifespan J Voice 34: 651-656.
- Louzada T, Beraldinelle R, Berretin-Felix G, Brasolotto AG (2011) Oral and vocal fold diadochokinesis in dysphonic women. J Appl Oral Sci 19L 567-572.
- Ollivere B, Duce K, Rowlands G, Harrison P, O Reilly BJ (2006) Swallowing dysfunction in patients with unilateral vocal fold paralysis: Aetiology and outcomes. J Laryngol Otol 120: 38-41.
- Kim SJ (2010) Music therapy protocol development to enhance swallowing training for stroke patients with dysphagia. J Music Ther 47(2): 102-119.
- Yiu EM, Ho EY (2002) Short-term effect of humming on vocal quality. Asia Pac J Speech Lang Hear 7(3): 123-137.
- Yeo MS, Kim SJ (2018) Therapeutic singing-based music therapy for patients with dysphagia: Case studies. J Rehabil Res 22: 169-194.






























