Person-centered Planning for Pre-frail or Frail Adults with Intellectual and Developmental Disabilities
Shahin Shooshtari1,2*, Margherita Cameranesi1,2, Katherine Chimney2, Heather Church3, and Beverley Temple2
1University of Manitoba, Canada
2St.Amant Research Centre
3University of Western Ontario, Canada
Submission: August 18, 2021; Published: August 25, 2021
*Corresponding author: Shahin Shooshtari, Department of Community Health Sciences, Rady Faculty of Health Sciences, University of Manitoba, 219 Human Ecology Building, Canada.
How to cite this article: Shahin S, Margherita C, Katherine C, Heather C, Beverley T. Person-centered Planning for Pre-frail or Frail Adults with Intellectual and Developmental Disabilities. Glob J Intellect Dev Disabil, 2021; 8(5): 555750. DOI:10.19080/GJIDD.2021.08.555750
Abstract
In this paper, we described a review of the literature conducted to identify key elements of person-centered planning with persons with intellectual and developmental disabilities, who are pre-frail or frail. Additionally, we reported the results of an environmental scan performed to identify existing person-centered planning tools and guidelines that were developed to be used with adults with intellectual and developmental disabilities. Next, we classified and discussed the core elements of person-centered planning with persons with intellectual and developmental disabilities, who are pre-frail or frail, within an eight-dimension quality of life conceptual framework. This information will be of great use to practitioners and researchers in the field to work together to develop more valid and reliable tools for person-centered care planning with pre-frail and frail persons with intellectual and developmental disabilities.
Keywords: Aging; Frailty; Intellectual and Developmental Disabilities; Person-centered Planning
Introduction
As persons with intellectual and developmental disabilities age, they become increasingly frail due to the multitude and complex health problems that they experience [1]. Adults with intellectual and developmental disabilities are found to be at a higher risk for frailty than those without these conditions. For example, in 2017, McKenzie and colleagues used the Frailty Marker, a frailty assessment tool developed at John Hopkins University, to compare the prevalence of frailty amongst 51,138 adults with intellectual and developmental disabilities and 3,272,080 adults without intellectual and developmental disabilities. Approximately 9% of adults with intellectual and developmental disabilities were identified as frail, which was higher than the 3% of persons without intellectual and developmental disabilities that were identified as frail [2].
It is found that those providing care to older persons with intellectual and developmental disabilities who are pre-frail or frail tend to focus on the distinct health issues and difficulties that these persons are experiencing rather than focusing on them as a person as a whole, considering their wants and needs [3]. For the purpose of our study, frailty is understood as “a multi-dimensional state of vulnerability involving cognitive, social, psychological and biological deficits, as well as environmental aspects associated with ageing and adverse outcomes such as falls, hospitalization, institutionalization and mortality.” [4].
Given the importance of this issue, the authors of the International Consensus Statement on “How Best to Support Adults with Intellectual and Developmental Disabilities” recommended person-centered planning as one the main principles for supporting persons with intellectual and developmental disabilities [4]. In the Consensus Statements, Ouellette-Kuntz and colleagues [4] also suggested that any action addressing pre-frailty or frailty status must be person-centered and must both privilege and respect the autonomy of the person when making choices about their care. Additionally, the authors also recommended multidisciplinary assessment with direct involvement of the person’s caregivers, and documentation of the preferences and wishes of the person for their future as essential components of person-centered planning with persons with intellectual and developmental disabilities who are pre-frail or frail. There is extensive literature on person-centered planning for adults in general, and for adults with intellectual and developmental disabilities, in particular. A recent review provided a description of resources and approaches that are currently used for person-centered planning, as well as the best practice that should be used when working with older adults, or persons with physical or intellectual and developmental disabilities . A recent environmental scan also explored indicators that are currently used to assess person-centered principles in the aging and disability sectors (Human Services Research Institute, 2019). However, still little is known about the key elements that should be assessed and included in person-centered planning with adults with intellectual and developmental disabilities who are pre-frail or frail, and there is a lack of best practice guidelines in this regard.
To gain a better understanding of the key elements of person-centered planning with adults with intellectual and developmental disabilities who are pre-frail or frail, and facilitate the development of a guideline, we conducted a comprehensive review of the literature and an environmental scan to collect detailed information on the approaches currently being used,and the issues considered worldwide. This paper provides an overview of what we have learned from our literature review and environmental scan. The information presented in this paper will be of great use to policy makers, healthcare professionals, and other practitioners working with vulnerable populations, including persons with intellectual and developmental disabilities who are pre-frail or frail. It can be of great use to develop more valid and reliable tools for person-centered care planning with pre-frail and frail adults with intellectual and developmental disabilities..
Methods
The information presented in this paper has been gathered through two primary means of data collection: 1) by conducting a comprehensive review of the literature on person-centered planning with persons with intellectual and developmental disabilities, and 2) by conducting an environmental scan of existing person-centered planning tools that are currently being used worldwide with a variety of vulnerable populations, including persons with intellectual and developmental disabilities. Our research methods are described below.
Literature review

To conduct a comprehensive literature review of personcentered planning with persons with intellectual and developmental disabilities who are pre-frail or frail, we searched the databases covered in the online portal EBSCOhost and Scopus with the help of an experienced academic librarian in the Summer of 2018. The terms that we used in our search covered three main concept areas: 1-intellectual and developmental disabilities (e.g., intellectual disabilit* OR developmental disabilit*), 2-person-centered planning (person-centred planning) (e.g., “personcentered plan*” OR “person-centered plan*”), and 3-pre-frailty and frailty (e.g., frail* OR pre-frail* OR aging OR geriat* OR elderly). We also searched the grey literature by conducting an online search on Google Scholar using similar concept areas. The original search led to the identification of 127 papers, whose title and abstracts were simultaneously and independently screened by two researchers working on this project (first level of screening). During level-two screening, the same two researchers simultaneously and independently screened the full-text of the 53 papers retained during level-one screening. At the end of the screening process, 31 papers were retained and included in our review. Figure 1 shows this screening process in a PRISMA diagram.
Environmental scan
Simultaneously to our literature search, we also performed an environmental scan of existing person-centered planning tools and guidelines that were developed and are currently being used with adults with intellectual and developmental disabilities. First, we performed a free Internet search of person-centered planning tools for care planning with adults with intellectual and developmental disabilities. We did not limit our search to any particular country, but rather searched available resources and tools in any jurisdiction worldwide. We compiled a list of resources and tools and contacted the developers to enquire about the tools and/or guidelines themselves and their use with persons with intellectual and developmental disabilities.
Second, as part of this environmental scan, given that healthcare is provincially governed in Canada, we examined the websites of all 10 Canadian provinces and three Canadian territories to search for available person-centered planning tools and guidelines used at the provincial or territorial level to perform person-centered planning with persons with intellectual and developmental disabilities, or other vulnerable populations such as persons with physical disabilities or older adults who are pre-frail or frail. To ensure validity of our efforts, we then sent an e-mail to the relevant authorities in each province and territory that summarized the findings of our search based on information posted on their website and asked them to confirm in writing if the listed tools/guidelines were the most current resources used in their jurisdiction. We also asked them that if the listed resources did not reflect the most current and up-to-date documents used in their province/territory to let us know and provide us with the correct documents, or direct us to where they could be found.
A list of elements that should be assessed and taken into account when conducting person-centered planning with persons with intellectual and developmental disabilities who are frail or pre-frail was developed based on our review of the literature. We also compiled a list of person-centered planning tools that are currently being used across the globe including those in Canada based on our environmental scan. Next, we put these findings together by assessing the core components of the person-centered planning tools we found against the person-centered planning elements we had previously identified. The most comprehensive tools currently available to perform person-centered planning with adults with intellectual and developmental disabilities who are pre-frail or frail were identified.
Findings
Literature review
Although person-centered planning is the recommended practice for provision of supports and services to pre-frail or frail adults with intellectual and developmental disabilities, our literature review revealed very limited research-based evidence on the core components of, or the effectiveness of person-centered planning in provision of care to this vulnerable population.
In 2015, Martin and colleagues conducted a study in the Canadian province of Ontario to examine the key elements of person-directed planning (PDP; [5]). PDP was defined as an approach that empowered the person, promoted and facilitated goal setting, and was based on what the person with intellectual and developmental disabilities wants for their life. They consulted with three planning teams from different community service agencies using participatory action research techniques. In discussing elements needed to be present for PDP to happen, the need for the right people, right attitudes and right actions were identified. All components related to the need for the right people, right attitudes and right actions were previously mentioned, but three new components related to right actions were reported. They were building community capacity, continuous evaluation of actions and progress, and responsiveness to changes in the person’s wants and needs.
For person-centered planning for frail adults with intellectual and developmental disabilities, it is vital to remember that the persons with intellectual and developmental disabilities and their caregivers age together. In a recent work, Coyle and colleagues [6] acknowledge that care is typically provided to adults with intellectual and developmental disabilities by aging families; in these families, primary care roles frequently transition from parents to siblings as aging parents become unable to continue care for their vulnerable children due to their own frailty or death. These authors conducted semi-structured interviews of siblings who had replaced parents in their role of primary caregivers of persons with intellectual and developmental disabilities to explore this transition from their perspective. Interview contents revealed that study participants expressed the need for long-term services and supports, such as educational resources, that could help and support them in acting as primary caregivers for their aging siblings with intellectual and developmental disabilities.
Advanced care planning (ACP), or future planning, is also reported as an important component of person-centered planning for pre-frail or frail adults with intellectual and developmental disabilities (Church et al., unpublished work). ACP is the process of developing a plan for care in preparation for when one is no longer able to inform care and treatment decisions for him/ herself or for one’s care recipients [7,8]. Several themes emerged from a recent environmental scan of ACP tools and guidelines for planning care with persons with intellectual and developmental disabilities who are pre-frail, or frail. They included identity of ACP team, decisional capacity, end of life decisions, values and priorities, conflict resolution and training (Church et al., unpublished). Decisional capacity determinations must include consideration of age-related cognitive declines. This may require assessment of understanding and implicit reasoning necessary to make important decisions. Issues that must be understood by the person with intellectual and developmental disabilities and/ or informal care providers include: information about service options, including palliative and hospice care and ensuring that ACP and end of life directives are documented appropriately [9]. The team involved in ACP must be comprised of members who are aware of and competent to implement resources and innovations to support age-related declines as needed and develop a process for managing and resolving conflict.
In 2012, Taggart and colleagues [10] conducted a study using structured questionnaires and semi-structured interviews to explore the future planning preferences of aging primary caregivers of a family member with intellectual and developmental disabilities. The authors also investigated the support systems that are required to develop future care plans. Study findings revealed that the primary caregivers of persons with intellectual and developmental disabilities included in this study expressed a strong preference for continuing to support their family members in the family home environment, either alone or with the support of paid staff. Only a minority of these primary caregivers expressed favoring other options. Additionally, the study identified four main themes around future care planning including: i) apprehension regarding future care, ii) the extent of future planning performed, iii) obstacles to planning, and iv) enabling factors that would provide solutions to planning. These primary caregivers of family members with intellectual and developmental disabilities reported that thinking about future care planning resulted in feelings of emotional upset that were aggravated by the obstacles they identified in future care planning, such as a lack of guidance and appropriate residential facilities. The authors concluded that the provision of accessible information, one-on-one guidance, and early future care planning were important to helping families of persons with intellectual or developmental disabilities with future care planning.
Brennan and colleagues [11] conducted a qualitative study nested within the larger longitudinal study of Intellectual Disability Supplement to the Irish Longitudinal Database on Ageing [12]. This qualitative component of the study involved focus groups and semi-structured interviews with primary caregivers of adult family members with intellectual and developmental disabilities [11]. Content analysis of the focus groups and interviews revealed three main themes in caregivers’ accounts, including i) the extent and type of future care planning their family members would need, ii) their diminishing ability to care for their family members with intellectual and developmental disabilities, and iii) the increasing need for supports such as residential care. Study findings also revealed that the majority of family caregivers shared an apprehension about the future with frequent worry concerning the varying options possible for future care plans should they no longer be able to support their family members with intellectual and developmental disabilities. Despite these concerns about future care planning and caregivers’ desires to continue caring for their aging family members with intellectual and developmental disabilities, definitive action planning was rarely undertaken. Most family caregivers included in the study questioned the sustainability of their ability to provide care into the future, with both parent and sibling caregivers acknowledging that this would be dependent upon the availability of resources. Many family members expressed that, as family caregiving capacity diminished, the most likely outcome would be a need for placement with residential services, despite their desire to personally care for their family members with intellectual and developmental disabilities in the home environment for as long as they could. Primary caregivers recognized residential services as the only feasible option due to the increasing age and associated physical health problems experienced by their family members with intellectual and developmental disabilities, which are core component of frailty status. These caregivers anticipated not being able to provide adequate care to their family members with intellectual and developmental disabilities who were becoming pre-frail or frail. Drawing on their findings, the authors concluded that to provide quality care supports to aging adults with intellectual and developmental disabilities, there is a need to establish proactive initiatives that facilitate the early development of long-term care plans for both people aging with intellectual and developmental disabilities and their families. Thus, advanced care planning must be considered as a key component of person-centered planning with persons with intellectual and developmental disabilities.
Ongoing frailty assessment for person-centered planning with adults with intellectual and developmental disabilities is also recommended [4]. However, a recent review identified only three research teams who have developed frailty measures for persons with intellectual and developmental disabilities [13]. In Austria, where the care provider varies between provinces to include a mix of non-governmental, governmental, and private organizations, the Vienna Frailty Questionnaire for Persons with Intellectual Disability (VFQ-ID) was developed and has since been revised (VFQ-ID-R) [14,15]. In the Netherlands, where care is organized and provided by region, and no one organization has a widespread directive to caring for aging adults with intellectual and developmental disabilities, Schoufour and colleagues [16] developed a frailty index for persons with intellectual and developmental disabilities over 50 years of age as part of their Healthy Aging and Intellectual Disability study. In Canada, where there are no national policies and guidelines, and the provision of disability services and disability supports varies across provinces and territories, McKenzie and colleagues [17] created a frailty index for adults with intellectual and developmental disabilities who use home care services.
Our review of the literature did not identify any practice application of these frailty measures to person-centered care planning with persons with intellectual and developmental disabilities. A qualitative study conducted by McKenzie and colleagues [18] can help us to better understand the factors affecting the implementation of frailty measures in populations of adults with intellectual and developmental disabilities. In this study, key informants from two research teams from the Netherlands and Austria were interviewed about their knowledge translation experiences. The study findings revealed that, to be implemented in practice, a frailty measure must be brief and relevant, and it must inform care decisions. In practice, brief and relevant frailty measures could be implemented to better care for persons aging with intellectual and developmental disabilities, and to inform person-centered care plans. The qualitative interviews conducted in the context of this study also revealed that it should be ensured that frailty measures are both valid and have a clear purpose, as well as that appropriate knowledge users are included as collaborators, prior to knowledge translation. Connections between frailty researchers, practitioners, and policy makers were also identified as key elements to successful implementation of frailty measures.
We found only two studies that were conducted by the same research team in the UK and assessed the effectiveness of personcentered planning in provision of care to persons with intellectual and developmental disabilities [19,20].
In 2005, Robertson and colleagues released a report describing a longitudinal study that examined the efficacy and costs of introducing person-centered planning for 93 persons with intellectual and developmental disabilities over 2 years. After the introduction of person-centered planning, for those who had a plan developed, positive changes were found in areas such as social networking, contact with family and friends, communitybased activities, scheduled day activities, and personal choice [19]. Further, it was found that the implementation of personcentered planning did not lead to a significant change in the costof- service delivery [19].
In their subsequent study, Robertson and colleagues [20] addressed what factors were associated with the likelihood of receiving a person-centered plan, as well as what factors were associated with the positive impact of person-centered planning that had previously been reported in their 2005 study. This more recent study revealed that factors related to participant characteristics, situational context, and the process of personcentered planning influenced both access to and efficacy of person-centered planning. Characteristics related to persons with intellectual and developmental disabilities included sex, as well as concurrent mental illness, behavioural issues, and physical health problems. Some of the contextual factors that were found to be associated with the success of person-centered planning in the study population included the presence of a care coordinator and the place of residence of persons with intellectual and developmental disability. Factors related to the person-centered planning process included facilitator commitment and the level of involvement of persons with intellectual and developmental disabilities. As these studies showed, these are important indicators to consider when developing a person-centered plan with persons who have intellectual and developmental disabilities.
Environmental scan
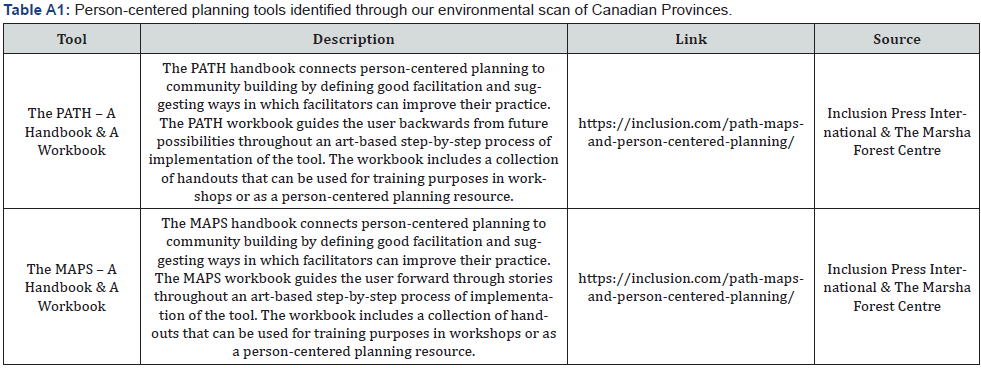
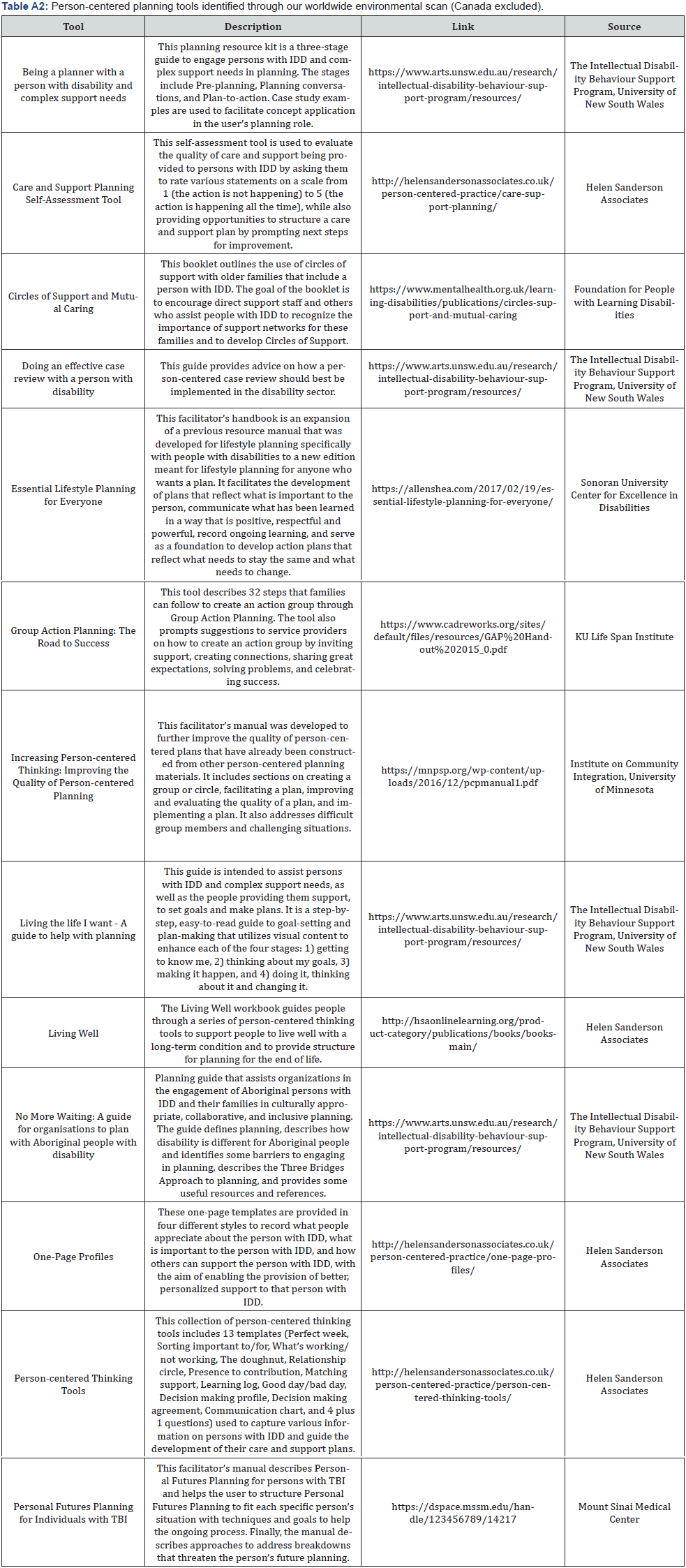
The environmental scan of person-centered planning tools available to be used with adults with intellectual and developmental disabilities led to the identification of a number of resources currently in use in Canada and abroad by professionals in person-centered thinking, planning, and practice. All the tools that were identified through this environmental scan are listed in Appendix A. Specifically, in the Appendix Table A1 presents the person-centered planning resources currently in use in some Canadian Provinces, while Table A2 presents several international resources.
In Canada, the Provinces of British Columbia, Ontario, Saskatchewan, and Manitoba are currently using some resources to perform person-centered planning with vulnerable persons, including those with intellectual and developmental disabilities, and their families (see Table A1 in Appendix A). These resources are currently being used by Canadian professionals who work with persons with disabilities as guiding frameworks and tools when conducting person-centered planning. A common theme to all the Canadian resources identified through the environmental scan is the inclusion of the persons at the center of a planning process that takes into account their individualities and that is therefore designed to enhance their well-being and quality of life. We found that in some jurisdictions in Canada, for example, in Prince Edward Island (PEI), Yukon and Northwest Territories, person-centered planning is not a common practice with persons with disabilities in general and with those with intellectual and developmental disabilities in particular. This is unfortunate given that, in planning that is not person-centered, there is a risk of overlooking the identities of the people whose lives are going to be most impacted by the planning being implemented. This is especially true for persons with intellectual and developmental disabilities who, given the intellectual and verbal challenges they experience, are less able to clearly and directly express their preferences and wishes to others.
As shown in Table A2 (Appendix A), the environmental scan also revealed 15 person-centered tools developed by a number of professional teams in the United States (US), United Kingdom UK), and Australia. These tools are currently being used in countries around the world by professionals in person-centered thinking, planning, and practice. The tool “Essential Lifestyle Planning for Everyone” [21] was developed by a team in the US and represents the most comprehensive resource identified through the environmental scan. This facilitator’s handbook or resource manual was created to help all professionals who perform essential lifestyle plans, particularly those working with persons with disabilities, to develop plans that help persons who use disability services to obtain the lives they truly want.
Accordingly, the handbook aids professionals in the development of plans that reflect what is important to the person, communicate what has been learned in a way that is positive, respectful and powerful, record ongoing learning, and serve as a foundation to develop action plans that reflect what needs to stay the same and what needs to change in the plan. Some key elements of the person-center planning outlined in the handbook include the respect of the person’s rights, the inclusion of the person’s support network in the planning, the ongoing assessment of the person’s physical and emotional needs, the consideration of social inclusion and community engagement, and setting daily activity goals organized into a larger and longer term personal action plan. Additionally, the handbook highlights how person-centered planning for persons with disabilities should take into account the physical environment where the person lives and should include the development of intentional personal safeguards. Planning for the future or advanced care planning is also an element of personcentered planning highlighted in the handbook, together with the assessment of the training needs of caregivers as well as the evaluation of the needs of aging caregivers. Specific action plans should be developed following these assessments.
Three additional resources identified through the environmental scan that are quite comprehensive, as they include most of the elements described above, are: i) Being a planner with a person with disability and complex support needs; ii) Doing an effective case review with a person with disability; and iii) Living the life I want (see Table A2 in Appendix A). These three resources were developed by a research team in the Intellectual Disability Behaviour Support Program at the University of New South Wales in Australia, and they represent tools created for use in different circumstances and by different professionals when conducting person-center planning with persons with intellectual disabilities.
It is important to note that none of the resources identified thought the environmental scan included the assessment of frailty status as a key element to include in person-centered planning with persons with disabilities. Given the early significant decline in health status that this population experiences when becoming pre-frail or frail, we recommend the inclusion of ongoing assessment of frailty status as one key component of personcentered planning with these persons.
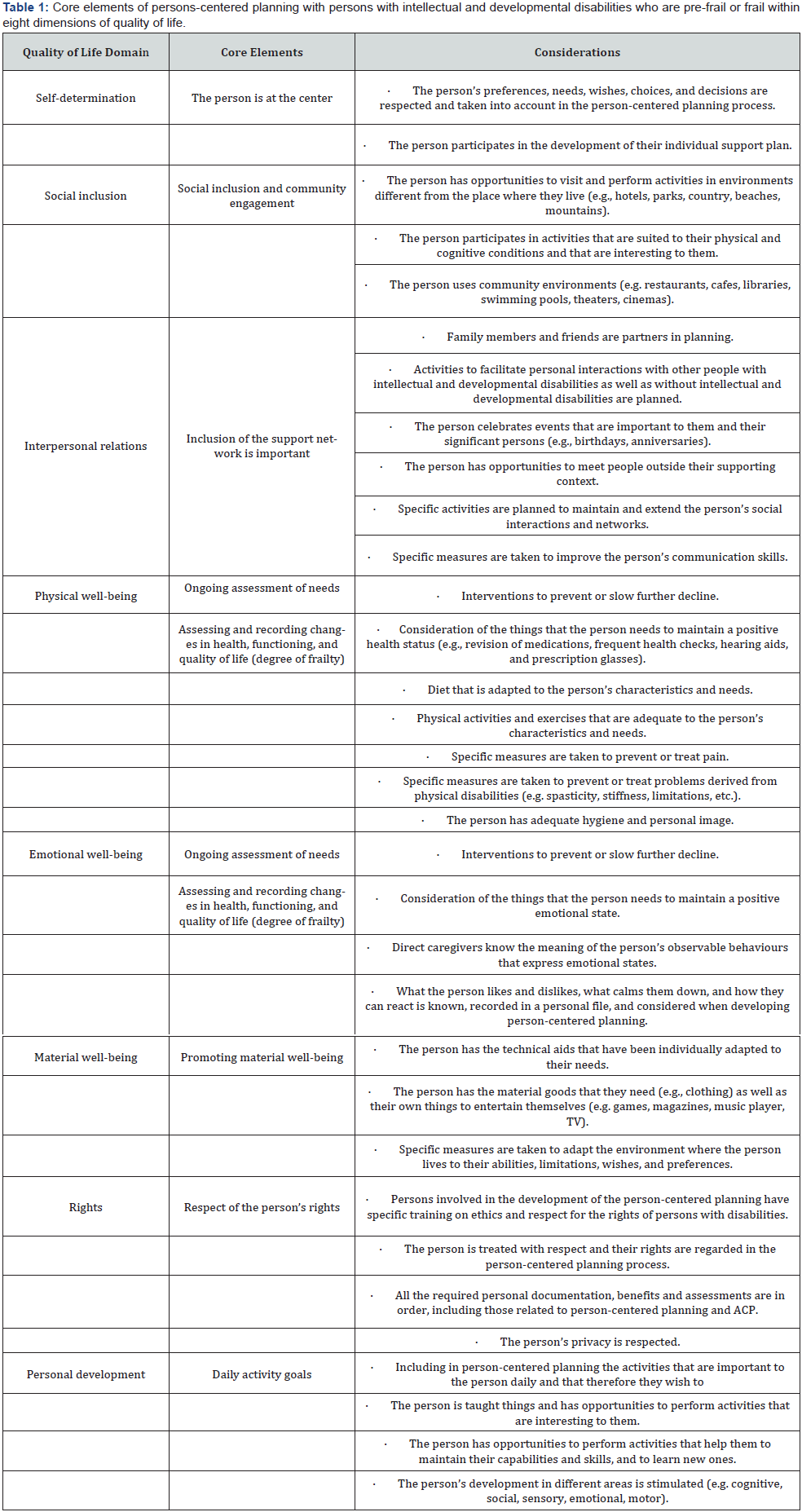
Based on a synthesis of the literature review and environmental scan presented, we developed some recommendations regarding a number of core elements that should be considered for personcentered planning with pre-frail or frail persons with intellectual and developmental disabilities. These core elements are listed in Table 1, organized within the eight dimensions of the qualityof- life conceptual framework proposed by Verdugo & Shalock [22]. We decided to present the recommended core elements of person-centered planning within a quality-of-life framework to stress that person-centered planning is planning conducted to maintain or enhance persons’ quality of life by respecting their individualities.
As shown in Table 1, most of the elements we recommend including in person-centered planning with persons with intellectual and developmental disabilities who are pre-frail or frail can be found in person-centered planning with all individuals. First, persons with intellectual and developmental disabilities who are pre-frail or frail should, to the extent possible, be involved in the planning process, together with their caregivers and support network, and the developing plan should respect their preferences, wishes, desires, choices, and decisions as much as possible. Additionally, throughout the planning process, the persons’ rights should be protected and respected; the persons should be treated with respect and their rights should be regarded in the person-centered planning process (e.g., privacy). Persons’ physical, emotional, and material well-being should be taken into account in the planning process by performing an ongoing assessment of their needs and by assessing and recording changes in health, functioning, and quality of life (i.e., degree of frailty). Finally, person-center planning with these persons should pay attention to and enhance their interpersonal relations, social inclusion and community engagement, and personal developmen
Discussion
A person-centered approach to planning focused on the person as a whole and is based on what is important and meaningful to the individual [23]. Given that people with intellectual and developmental disabilities are at a greater risk for frailty and at an earlier age, person-centered planning must be done as soon as possible.
Since frailty is a multidimensional concept, person-centered planning tools should include items not only based on biology/ physiology, but also based on other dimensions including social health and cognition. Using the eight-dimension quality of life conceptual framework proposed by Verdugo & Schalock [22], we identified a number of core elements and items to be considered within a tool for person-centered planning for pre-frail or frail people with intellectual and developmental disabilities.
Based on our review and synthesis of the literature, we also recommend a number of additional considerations that should be included in person-centered planning with persons with intellectual and developmental disabilities who are prefrail or frail. To monitor the health and quality of life of persons with intellectual and developmental disabilities as they age, person-centered planning should be a dynamic process that pays attention to the changing needs of persons with intellectual and developmental disabilities in their environment as they age, and that considers the aging of the caregivers themselves and their changing needs [24].
Ongoing frailty assessment is key, due to the early onset of frailty in adults with intellectual and developmental disabilities. Frailty assessment should be performed on an ongoing basis in this population (e.g., more often than just yearly) and should inform the development of person-centered plans. During frailty assessment, direct support staff, other professionals assisting persons with intellectual and developmental disabilities, and caregivers (e.g., family members) should pay attention to not only assessing but also recording the changes in all domains of health and quality of life that these persons experience at an earlier age than the general population. Specific training in these areas of assessment and in relevant health-related issues may be needed in certain circumstances, and therefore training of direct support staff, other professionals assisting persons with intellectual and developmental disabilities and caregivers (e.g., family members) must be implemented as needed to ensure a consistent frailty assessment.
A reflection on and discussion about the age-related declines and the associated deteriorating health status, changing care needs, and decreasing caregiving capacity of aging caregivers should also be included in person-centered planning with persons with intellectual and developmental disabilities who are becoming pre-frail or frail. Assessment of the needs of aging caregivers (e.g., family members) is pivotal to develop a plan that supports them and their aging family members (persons with intellectual and developmental disabilities). At some point, when the capacity for care and support within the family diminishes considerably, there is an inevitable need to support the person with intellectual and developmental disabilities who is aging by involving resources external to the family system (e.g., moving the person from the family home to a residential care facility).
Conclusion
Persons with intellectual and developmental disabilities who are pre-frail or frail, regardless of their age, should have a personal action plan of individual support that all of their support network members including family members and paid caregivers must know and implement. Personal action plans should be person-centered, which means they should be developed based on the wishes and preferences of the person with intellectual and developmental disabilities, for the present and for the future, and developed in collaboration with the meaningful people in their lives (e.g., family members). The plans should also be revised on an ongoing basis in accordance with the changing needs of the aging persons with intellectual and developmental disabilities, and their support network (e.g., aging parents). Ongoing frailty assessment using simple and practical tools is recommended to record persons’ unique vulnerabilities and build intentional personal safeguards in the plan to reduce them. These plans must be comprehensive address issues related to self-determination, social inclusion, interpersonal relations, physical wellbeing, emotional wellbeing, material wellbeing, rights, and personal development. They must be developed at an earlier age, applying a future planning lens.
Appendix A: Person-Centered Planning Resources Identified through the Environmental Scan
References
- Stax TE, Luciano L, Dunn AM, Quevedo JP (2010) Aging and developmental disability. Physical Medicine & Rehabilitation Clinics of North America 21(2): 419-427.
- McKenzie K, Ouellette‐Kuntz H, Martin L (2017) Applying a General Measure of Frailty to Assess the Aging Related Needs of Adults with Intellectual and Developmental Disabilities. Journal of Policy and Practice in Intellectual Disabilities 14(2): 124-128.
- Claes C, Van Hove G, Vandervelde S, van Loon J, Schalock R (2010) Person-Centered Planning: Analysis of Research and Effectiveness. Intellectual and Developmental Disabilities 48(6): 432-453.
- Ouellette-Kuntz H, Martin L, Burke E, Philip Mc, Mary Mc, et al. (2018) How best to support individuals with intellectual and developmental disabilities as they become frail: A Consensus Statement. Journal of Applied Research in Intellectual Disabilities 32(1): 1-8.
- Martin L, Grandia P, Ouellette-Kuntz H, Cobigo V (2016) From Framework to Practice: Person-Directed Planning in the Real World. Journal of Applied Research in Intellectual Disabilities 29: 552-565.
- Coyle CE, Kramer J, Mutchler JE (2014) Aging Together: Sibling Carers of Adults with Intellectual and Developmental Disabilities. Journal of Policy and Practice in Intellectual Disabilities 11(4): 302-312.
- Perkins E, van Heumen L (2018) When the journey ends: Parental caregiving and later life planning. In: Goff N, Piland N (Eds.), Intellectual and developmental disabilities: A roadmap for families and professionals. New York, NY: Routledge, Taylor and Francis Group, pp. 216-228.
- The Arc Center for Future Planning (2016a) Future Planning 101: What is Future Planning.
- Stein G (2007) Advance Directives and Advance Care Planning for People with Intellectual and Physical Disabilities. U.S. Department of Health and Human Services Assistant Secretary: 25.
- Taggart L, Truesdale-Kennedy M, Ryan A, Roy Mc (2012) Examining the support needs of ageing family caregivers in developing future plans for a relative with an intellectual disability. Journal of Intellectual Disabilities 16(3): 217-234.
- Brennan D, Murphy R, McCallion P, Mary Mc (2018) “What’s going to happen when we’re gone?” Family caregiving capacity for older people with an intellectual disability in Ireland. Journal of Applied Research in Intellectual Disabilities 31(2): 226-235.
- McCarron M, Swinburne J, Burke E, et al. (2011) Growing older with an intellectual disability in Ireland 2011: Results from the intellectual disability supplement of the Irish longitudinal study on ageing. Dublin: School of Nursing and Midwifery, Trinity College Dublin.
- McKenzie K, Martin L, Ouellette-Kuntz H (2016a) Frailty and Intellectual and Developmental Disabilities: a Scoping Review. Canadian Geriatrics Journal 19(3): 103-112.
- Brehmer B, Weber G (2010) Frailty versus disability distinctions in people with intellectual disabilities. Journal of Policy and Practice in Intellectual Disabilities 7(1): 49-58.
- Brehmer-Rinderer B, Zeilinger EL, Radaljevic A, Germain W (2013) The Vienna Frailty Questionnaire for persons with intellectual disabilities-Revised. Research in Developmental Disabilities: A Multidisciplinary Journal 34(6): 1958-1965.
- Schoufour JD, Mitnitski A, Rockwood K, Haleen M, Micheal AE (2013) Development of a Frailty Index for Older People with Intellectual Disabilities: Results from the HA-ID study. Research in Developmental Disabilities: A Multidisciplinary Journal 34(5): 1541-1555.
- McKenzie K, Ouellette-Kuntz H, Martin L (2015) Using an accumulation of deficits approach to measure frailty in a population of home care users with intellectual and developmental disabilities: an analytical descriptive study. BMC Geriatrics 15: 170.
- McKenzie K, Martin L, Ouellette-Kuntz H (2016b) Understanding Implementation of Frailty Measures Among Adults with Intellectual and Developmental Disabilities. Journal on Developmental Disabilities 22(2): 91-100.
- Robertson J, Emerson E, Hatton C, et al. (2005) The Impact of Person Centred Planning. Institute for Health Research, Lancaster University. UK.
- Robertson J, Emerson E, Hatton C, Elliott J, McIntosh B, et al. (2007) Person-centered Planning: Factors Associated with Successful Outcomes for People with Intellectual Disabilities. Journal of Intellectual Disability Research 51(3): 232-243.
- Smull MW, Sanderson H, Sweeney C, Skelhorn L, George A, et al. (2009) Essential lifestyle planning for everyone (2nd), Annapolis (MD), USA: The Learning Community - Essential Lifestyle Planning.
- Verdugo MA, Schalock RL (2009 Quality of life: from concept to future applications in the field of intellectual disabilities. Journal of Policy and Practice in Intellectual Disabilities 6: 62-64.
- Sanderson H (2000) Person-centered planning: key features and approaches.
- Baumbusch J, Mayer S, Phinney A, Sarah B (2017) Aging together: Caring relations in families of adults with intellectual disabilities. Journals of Gerontology Series B: Psychological Sciences and Social Sciences 57(2): 341-347.






























