Parsonage - Turner Syndrome, A Cause of Underdiagnosed Painful Shoulder: Case Report
Simon Uribe Castaño1, Miguel Jose Ortiz1, Felipe Garcia Jaramillo1 and Santiago Vasquez Builes2*
1CES University, Medellín, Antioquia, Colombia
2Emergency Department, Instituto Neurológico de Colombia, Medellín, Antioquia, Colombia
Submission: July 02, 2021; Published: July 12, 2021
*Corresponding author: Santiago Vasquez Builes, Emergency Department, Instituto Neurológico de Colombia, Medellín, Antioquia, Colombia.
How to cite this article: Simon U C, Miguel J O, Felipe Garcia J, Santiago V B. Parsonage - Turner Syndrome, A Cause of Underdiagnosed Painful Shoulder: Case Report. Glob J Intellect Dev Disabil, 2021; 8(5): 555746. DOI:10.19080/GJIDD.2021.08.555746
Abstract
The Painful shoulder condition is a frequent reason for consultation in medical practice. One of the non-traumatic causes of painful shoulder is the brachial nerve neuritis, or Parsonage-Turner syndrome. This syndrome has been underdiagnosed because of the little knowledge of disease. Its external exact cause is unknown up to now, although it has been associated to infectious processes, autoimmune diseases, strenuous physical activity, among others.
We report a case of 31-year-old patient who presented acute non-traumatic shoulder pain with distribution in C5 and C6 dermatomes, associated with functional limitation, who was diagnosed with brachial nerve neuritis through imaging and electromyography studies. Acutely, the patient was treated with steroids and nonsteroidal anti-inflammatory drugs. After discharging, pregabalin was started with improvement of the symptoms. In the outpatient follow-up, the immunological profile was ordered, the results of which were negative. Also, cervical MRI is performed without pathologic findings.
The purpose of this article is to present neuritis of the brachial nerve as a cause of acute painful shoulder and diagnosis that leads to suspect autoimmune, infectious diseases or cervical pathology.
Key words: Brachial neuritis; Parsonage turner syndrome; Neuralgic amyotrophy
Abbreviations: PTS: Parsonage Turner Syndrome; MRI: Magnetic Resonance Imaging
Introduction
Non-traumatic painful shoulder is a common reason for consultation in primary medical care resulting in the third reason for consultation in medical practice [1]. Multiple causes of non-traumatic painful shoulder have been described, including glenohumeral pathology, rotator cuff syndrome, Parsonage Turner Syndrome (PTS), among others. PTS was initially described with the name of serratus major paralysis, shoulder neurosis or acute brachial radiculitis [2,3]. It was until 1948 when doctors Parsonage and Turner found out this pathology in a population pathology, and later they named it shoulder neuralgic amyotrophy. Its cardinal clinical symptom is an acute pain that may be associated with the limb weakness and atrophy of muscles that make up the shoulder structure. Its incidence has not been estimated, since it is an underdiagnosed pathology [4-6].
Below there is a case report of a PTS patient, which is a diagnostic challenge pathology for the medical practice.
Case Report
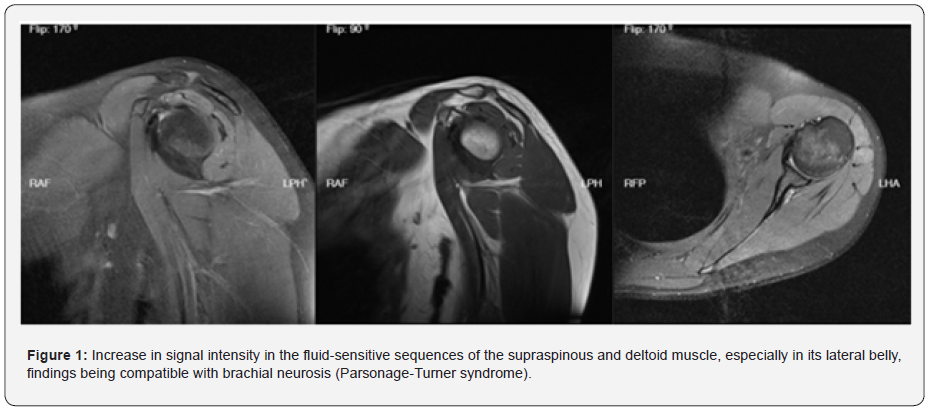
31-year-old female patient, with a history of hypothyroidism in treatment with levothyroxine 75 mg per day, who consults for 8 days of disabling pain in her left shoulder of dorsal predominance, with irradiation to the triceps region, limiting the shoulder abduction and elbow extension, and no other symptoms. At the admission, her vital signs are interpreted as normal, and it is evident that the pain has a distribution in dermatome C5 and C6, reflex alteration in the involved limb not documented and also no loss of muscular force. Shoulder ultrasound is performed reporting free liquid in periarticular region, so simple magnetic resonance imaging in her left shoulder is carried out resulting in an increase in the signal intensity in the fluid-sensitive sequences of the supraspinous muscle and deltoids, especially in her lateral belly, findings compatible with brachial neuritis (Parsonage-Turner syndrome) (Figure 1). Subsequently, an electromyography is performed reporting triceps denervation with C7 radiculopathy with normal distal motor and sensitive latencies. Acutely the patient was treated with an intravenous dose of Dexametasone along with Diclofenac, then the outpatient treatment for neuropathic pain was pregabalin per day for 8 weeks. At 4 weeks, antinuclear antibodies, extractable nuclear antigens, antiphospholipid antibodies and anticardiolipine were ordered, whose results were negative. Outpatient cervical magnetic resonance imaging is performed without any pathological findings. The outcome of the patient was favorable, because there wasn't any finding that supported any lower motor neuron syndrome, this case was only presented with acute and subacute pain, therefore no other interventions were needed.
Discussion
The PTS has an incidence of 1.64 cases per 100,000 people; however, the true incidence may be higher since it is an underreported entity [7]. Its distribution mainly occurs between the third and fifth decade of life and there appears to be a higher incidence in men than in women [3,4]. No exact cause for this pathology is known up to date, although it has been associated with bacterial infections (Borrelia), viral infections (cytomegalovirus), flue, HIV), autoimmune diseases, (polyarteritis nodosa, systemic erythematosus lupus, among others) or external factors such as postsurgical stress, traumatisms or strenuous physical exercise [2,4,7].
PTS usually appears for the first time with severe pain in the involved limb, associated with symptoms of lower motor neuron syndrome such as paresis and hyporeflexia. It commonly affects the proximal muscles of the upper limb. Deltoid is the most compromised muscle followed by supraspinous, infraspinatus, serratus major, biceps, triceps and carpus and fingers extensor muscles [6,8]. A correct anamnesis and physical exploration, in accordance with an electromyographic examination of the involved upper limb provide a diagnosis [4,5].
The electromyography plays an important role during the muscular denervation period, since it is there where the muscular alteration specific pattern is documented. Moreover, it indicates the localization of the neurologic injury. The speeds of conduction or medium distal motor and sensitive latencies in upper limbs, are usually normal or do not report any alteration [9].
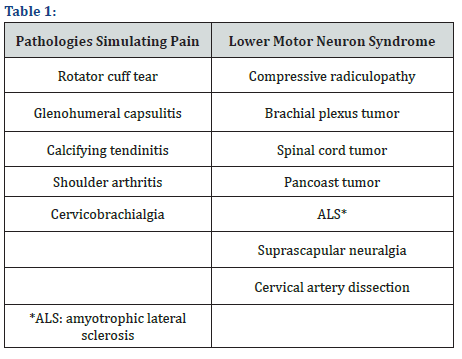
The shoulder magnetic resonance (MRI) does not show any specific changes of the PTS; however, during the acute phase, it may show muscular edema caused by both the muscle denervation and the increase of blood supply to the denervated muscles. This edema is not clearly different from the one that may cause a traumatic injury, so, it is not a specific finding. In the late phases atrophy can be seen in denervated muscles. The examiner should take into account the differential diagnosis (Table 1) [10,11].
Conclusion
The PTS is a little frequent cause in the approach of a patient with non-traumatic shoulder acute pain; however, it must be taken into account as a possible cause thereof. Its cardinal symptom is the acute pain at shoulder level. Its diagnosis may become a challenge for the doctor, since the symptoms are nonspecific to be diagnosed by the physical exploration and may be present in its differential diagnosis. In the reported clinical case, the painful shoulder approach was made based on both the clinical history and the patient’s physical exploration. Due to the semiological findings, it was decided to complement the studies with diagnostic aids such as electromyography and nuclear magnetic resonance which are critical to make the PTS diagnosis and finally to discard any autoimmune diseases.
Authors’ Contribution
Bibliographic search and writing of the initial manuscript: S.U.C., F.G.J. and M.J.O Review and complement of both the manuscript and the initial bibliography: S.V.B. Following corrections, complements and final review: S.U.C., F.G.J., M.J.O. and S.V.B.
References
- Seror P (2017) Neuralgic amyotrophy. An update. Joint Bone Spine 84(2): 153-158.
- Kim TU, Chang MC (2021) Neuralgic amyotrophy: an underrecognized entity. J Int Med Res 49(4): 3000605211006542.
- Gstoettner C, Mayer JA, Rassam S, Hruby LA, Salminger S, et al. (2020) Neuralgic amyotrophy: a paradigm shift in diagnosis and treatment. J Neurol Neurosurg Psychiatry 91(8): 879-888.
- Sneag Darryl B, Schneider K Rancy, Scott W Wolfe, Susan C Lee, Vivek Kalia, et al. (2018) Brachial Plexitis or Neuritis MRI Features of Lesion Distribution in Parsonage-Turner Syndrome: Brachial Plexitis or Neuritis? Muscle & Nerve 58(3): 359-366.
- Shaukat MFS, Ogunwale B, Arpan BK (2019) MRI Appearances of Parsonage-Turner Syndrome. J Coll Physicians Surg Pak 29(11): 1127-1128.
- Sneag DB, Rancy SK, Wolfe SW, Lee SC, Kalia V, et al. (2018) Brachial plexitis or neuritis? MRI features of lesion distribution in Parsonage-Turner syndrome. Muscle Nerve 58(3): 359-366.
- Mitry MA, Collins LK, Kazam JJ, Kaicker S, Kovanlikaya A (2021) Parsonage-turner syndrome associated with SARS-CoV2 (COVID-19) infection. Clinical Imaging 72: 8-10.
- Devon I Rubin (2020) Brachial and Lumbosacral Plexopathies: A Review, Clinical Neurophysiology Practice 5: 173-193.
- Feinberg JH, Nguyen ET, Boachie-Adjei K, Gribbin C, Lee SK, et al. (2017) The Electrodiagnostic Natural History of Parsonage-Turner Syndrome. Muscle Nerve 56(4): 737-743.
- Upadhyaya V, Upadhyaya DN, Bansal R, Pandey T, Pandey AK (2019) MR neurography in Parsonage-Turner syndrome. Indian J Radiol Imaging 29(3): 264-270.
- Shaukat MFS, Ogunwale B, Arpan BK (2019) MRI Appearances of Parsonage-Turner Syndrome. J Coll Physicians Surg Pak 29(11): 1127-1128.






























